Abstract
Background
The efficacy of ablative surgery for head and neck squamous cell carcinoma (HNSCC) depends critically on obtaining negative margins. Although intraoperative “frozen section” analysis of margins is a valuable adjunct, it is expensive, time-consuming, and highly dependent on pathologist expertise. Optical imaging has potential to improve the accuracy of margins by identifying cancerous tissue in real time. Our goal was to determine the accuracy and inter-rater reliability of head and neck cancer specialists using high-resolution microendoscopic (HRME) images to discriminate between cancerous and benign mucosa.
Methods
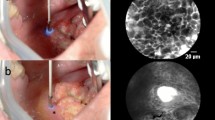
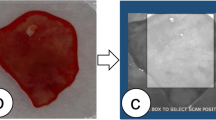
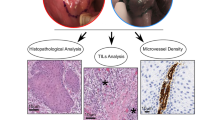
Thirty-eight patients diagnosed with head and neck squamous cell carcinoma (HNSCC) were enrolled in this single-center study. HRME was used to image each specimen after application of proflavine, with concurrent standard histopathologic analysis. Images were evaluated for quality control, and a training set containing representative images of benign and neoplastic tissue was assembled. After viewing training images, seven head and neck cancer specialists with no previous HRME experience reviewed 36 test images and were asked to classify each.
Results
The mean accuracy of all reviewers in correctly diagnosing neoplastic mucosa was 97 % (95 % confidence interval (CI), 94–99 %). The mean sensitivity and specificity were 98 % (97–100 %) and 92 % (87–98 %), respectively. The Fleiss kappa statistic for inter-rater reliability was 0.84 (0.77–0.91).
Conclusions
Medical professionals can be quickly trained to use HRME to discriminate between benign and neoplastic mucosa in the head and neck. With further development, the HRME shows promise as a method of real-time margin determination at the point of care.




Similar content being viewed by others
References
Silverman S, Sugerman PB. Oral premalignancies and squamous cell carcinoma. Clin Dermatol. 2000;18:563–8.
Binahmed A, Nason RW, Abdoh AA. The clinical significance of the positive surgical margin in oral cancer. Oral Oncol. 2007;43:780–4.
Meier JD, Oliver DA, Varvares MA. Surgical margin determination in head and neck oncology: current clinical practice. The results of an International American Head and Neck Society member survey. Head Neck. 2005;27:952–8.
Gandour-Edwards RF, Donald PJ, Wiese DA. Accuracy of intraoperative frozen section diagnosis in head and neck surgery: experience at a university medical center. Head Neck. 1993;15:33–8.
Schwarz RA, Gao W, Daye D, Williams MD, Richards-Kortum R, Gillenwater AM. Autofluorescence and diffuse reflectance spectroscopy of oral epithelial tissue using a depth-sensitive fiber-optic probe. Appl Optics. 2008;47:825–34.
Ramanujam N, Mitchell MF, Mahadevan A, et al. In vivo diagnosis of cervical intraepithelial neoplasia using 337-nm-excited laser-induced fluorescence. Proc Natl Acad Sci USA. 1994;91:10193–7.
Muldoon TJ, Anandasabapathy S, Maru D, Richards-Kortum R. High-resolution imaging in Barrett’s esophagus: a novel, low-cost endoscopic microscope. Gastrointest Endosc. 2008;68:737–44.
Muldoon TJ, Roblyer D, Williams MD, Stepanek VMT, Richards-Kortum R, Gillenwater AM. Noninvasive imaging of oral neoplasia with a high-resolution fiber-optic microendoscope. Head Neck. 2012;34(3):305–12.
Girousi ST, Alexiadou DK, Ioannou AK. An electroanalytical study of the drug proflavine. Microchim Acta. 2008;160:435–39.
Polglase AL, McLaren WJ, Skinner SA, Kiesslich R, Neurath MF, Delaney PM. A fluorescence confocal endomicroscope for in vivo microscopy of the upper- and the lower-GI tract. Gastrointest Endosc. 2005;62:686–95.
Kiesslich R, Burg J, Vieth M, et al. Confocal laser endoscopy for diagnosing intraepithelial neoplasias and colorectal cancer in vivo. Gastroenterology. 2004;127:706–13.
Pitten FA, Kramer A. Antimicrobial efficacy of antiseptic mouthrinse solutions. Eur J Clin Pharmacol. 1999;55:95–100.
Mathe G. The failure of HARRT to cure the HIV-1/AIDS complex. Suggestions to add integrase inhibitors as complementary virostatics, and to replace their continuous long combination applications by short sequences differing by drug rotations. Biomed Pharmacother. 2001;55:295–300.
Ke S, Wen XX, Gurfinkel M, et al. Near-infrared optical imaging of epidermal growth factor receptor in breast cancer xenografts. Cancer Res. 2003;63:7870–75.
Soukos NS, Hamblin MR, Keel S, Fabian RL, Deutsch TF, Hasan T. Epidermal growth factor receptor-targeted immunophotodiagnosis and photoimmunotherapy of oral precancer in vivo. Cancer Res. 2001;61:4490–6.
Acknowledgments
The authors thank Dr. Vishal Gupta, Dr. Michelle Kim, Dr. Marshall Posner, Dr. Krys Misiukiwicz, Dr. Kenneth Altman, and Dr. Benjamin Malkin of the Mount Sinai School of Medicine for participating in the grading of HRME data. We also thank Dr. Richard Schwarz of Rice University for the helpful comments and critiques during the preparation of this manuscript. This project was funded in part by the National Cancer Institute (NCI) Bioengineering Research Partnerships (BRP) Grant 2R01CA103830-06A1, a competitive research grant from Intuitive Surgical, Inc., and by the Doris Duke Charitable Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vila, P.M., Park, C.W., Pierce, M.C. et al. Discrimination of Benign and Neoplastic Mucosa with a High-Resolution Microendoscope (HRME) in Head and Neck Cancer. Ann Surg Oncol 19, 3534–3539 (2012). https://doi.org/10.1245/s10434-012-2351-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-012-2351-1