Abstract
Background
Sentinel lymph node biopsy (SLNB) has recently been used to detect occult lymph node metastases. The aim of this study was to assess the feasibility and clinical efficacy of SLNB in the treatment of clinically node-negative papillary thyroid carcinoma.
Methods
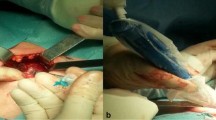
A total of 114 consecutive patients with clinically node-negative papillary thyroid carcinoma were enrolled and underwent SLNB. After injection of 1% methylene blue around the tumors, blue-stained sentinel lymph nodes (SLN) were collected from the central compartments. All the patients underwent total thyroidectomy with bilateral central compartment neck dissection after SLNB.
Results
SLN were identified in 84 (73.7%) of the 114 patients. Of these 84 patients, 24 (28.6%) had metastases in the SLN. Among the 60 patients who had no metastases in their SLN in frozen biopsy samples, seven had metastatic foci in their SLN in the permanent biopsy samples and six had metastases in their non-SLN samples. Central compartment lymph node metastases were detected in 11 of the 30 patients in whom SLN were not identified. Thus, the sensitivity, specificity, and positive and negative predictive values of SLNB were 64.9, 100, 100, and 78.3%, respectively. The false-positive and false-negative rates were 0 and 35.1%, respectively. The detection of SLN led to no major complications.
Conclusions
SLNB using methylene blue in papillary thyroid carcinoma is a safe and technically feasible procedure. However, it is of limited use in the management of clinically node-negative papillary thyroid carcinoma because of low sensitivity and a high false-negative rate.


Similar content being viewed by others
References
Hay ID, Bergstralh EJ, Goellner JR, Ebersold JR, Grant CS. Predicting outcome in papillary thyroid carcinoma: development of a reliable prognostic scoring system in a cohort of 1779 patients surgically treated at one institution during 1940 through 1989. Surgery. 1999;114:1050–8.
Shaha AR. Thyroid cancer: extent of thyroidectomy. Cancer Control. 2000;7:240–5.
Henry JF, Gramatica L, Denizot A, Kvachenyuk A, Puccini M, Defechereux T. Morbidity of prophylactic lymph node dissection in the central neck area in patients with papillary thyroid carcinoma. Langenbecks Arch Surg. 1998;383:167–9.
Cady B. Lymph node metastases. Indicators, but not governors of survival. Arch Surg. 1984;119:1067–72.
Shah JP, Loree TR, Dharker D, Strong EW, Begg C, Vlamis V. Prognostic factors in differentiated carcinoma of the thyroid gland. Am J Surg. 1992;164:658–61.
Zaydfudim V, Feurer ID, Griffin MR, Phay JE. The impact of lymph node involvement on survival in patients with papillary and follicular thyroid carcinoma. Surgery. 2008;144:1070–7; discussion 1077–8.
Mazzaferri EL, Doherty GM, Steward DL. The pros and cons of prophylactic central compartment lymph node dissection for papillary thyroid carcinoma. Thyroid. 2009;19:683–9.
Lundgren CI, Hall P, Dickman PW, Zedenius J. Clinically significant prognostic factors for differentiated thyroid carcinoma: a population-based, nested case-control study. Cancer. 2006;106:524–31.
Podnos YD, Smith D, Wagman LD, Ellenhorn JD. The implication of lymph node metastasis on survival in patients with well-differentiated thyroid cancer. Am Surg. 2005;71:731–4.
Cooper DS, Doherty GM, Haugen BR, et al. Revised American thyroid association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009;19:1167–214.
Cheah WK, Arici C, Ituarte PH, Siperstein AE, Duh QY, Clark OH. Complications of neck dissection for thyroid cancer. World J Surg. 2002;26:1013–6.
Cavicchi O, Piccin O, Caliceti U, De Cataldis A, Pasquali R, Ceroni AR. Transient hypoparathyroidism following thyroidectomy: a prospective study and multivariate analysis of 604 consecutive patients. Otolaryngol Head Neck Surg. 2007;137:654–8.
Kim E, Park JS, Son KR, Kim JH, Jeon SJ, Na DG. Preoperative diagnosis of cervical metastatic lymph nodes in papillary thyroid carcinoma: comparison of ultrasound, computed tomography, and combined ultrasound with computed tomography. Thyroid. 2008;18:411–8.
Krag DN, Weaver DL, Alex JC, Fairbank JT. Surgical resection and radiolocalization of the sentinel lymph node in breast cancer using a gamma probe. Surg Oncol. 1993;2:335–9.
Van Der Veen H, Hoekstra OS, Paul MA, Cuesta MA, Meijer S. Gamma probe-guided sentinel node biopsy to select patients with melanoma for lymphadectomy. Br J Surg. 1994;81:1769–70.
Pelizzo MR, Merante Boschin I, Toniato A, et al. Sentinel node mapping and biopsy in thyroid cancer: a surgical perspective. Biomed Pharmacother. 2006;60:405–8.
Raijmakers PG, Paul MA, Lips P. Sentinel node detection in patients with thyroid carcinoma: a meta-analysis. World J Surg. 2008;32:1961–7.
Balasubramanian SP, Harrison BJ. Systematic review and meta-analysis of sentinel node biopsy in thyroid cancer. Br J Surg. 2011;98:334–344.
Anand SM, Gologan O, Rochon L, et al. The role of sentinel lymph node biopsy in differentiated thyroid carcinoma. Arch Otolaryngol Head Neck Surg. 2009;135:1199–204.
Fukui Y, Yamakawa T, Taniki T, Numoto S, Miki H, Monden Y. Sentinel lymph node biopsy in patients with papillary thyroid carcinoma. Cancer. 2001;92:2868–74.
Dzodic R, Markovic I, Inic M, et al. Sentinel lymph node biopsy may be used to support the decision to perform modified radical neck dissection in differentiated thyroid carcinoma. World J Surg. 2006;30:841–6.
Cunningham DK, Yao KA, Turner RR, Singer FR, Van Herle AR, Giuliano AE. Sentinel lymph node biopsy for papillary thyroid cancer: 12 years of experience at a single institution. Ann Surg Oncol. 2010;17:2970–5.
Chow TL, Lim BH, Kwok SP. Sentinel lymph node dissection in papillary thyroid carcinoma. ANZ J Surg. 2004;74:10–2.
Carcoforo P, Feggi L, Trasforini G, et al. Use of preoperative lymphoscintigraphy and intraoperative gamma-probe detection for identification of the sentinel lymph node in patients with papillary thyroid carcinoma. Eur J Surg Oncol. 2007;33:1075–80.
Carty SE, Cooper DS, Doherty GM, et al. Consensus statement on the terminology and classification of central neck dissection for thyroid cancer. Thyroid. 2009;19:1153–8.
Ramin S, Azar FP, Malihe H. Methylene blue as the safest blue dye for sentinel node mapping: Emphasis on anaphylaxis reaction. Acta Oncol. 2011;50:729–31.
Noguchi M, Kumaki T, Taniya T, Miyazaki I. Bilateral cervical lymph node metastases in well-differentiated thyroid cancer. Arch Surg. 1990;125:804–6.
Gourin CG, Johnson JT. Postoperative complications. In: Randolph GW, editor. Surgery of the thyroid and parathyroid glands. Philadelphia: Saunders; 2003. p. 433–43.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ji, Y.B., Lee, K.J., Park, Y.S. et al. Clinical Efficacy of Sentinel Lymph Node Biopsy Using Methylene Blue Dye in Clinically Node-Negative Papillary Thyroid Carcinoma. Ann Surg Oncol 19, 1868–1873 (2012). https://doi.org/10.1245/s10434-011-2109-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-011-2109-1