Abstract
Background
This study was designed to identify pathological predictors of para-aortic nodal invasion in advanced gastric cancer.
Methods
Between 1990 and 2007, 294 patients with advanced gastric cancer underwent gastrectomy with D2 lymphadenectomy + para-aortic nodal dissection in Siena and Verona, Italy.
Results
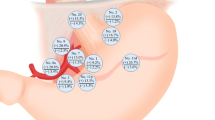
Forty-seven (16%) patients had para-aortic node metastases. Of these, 91%, 88%, and 74%, respectively, also had metastases at stations No. 3, No. 1, and No. 7. Para-aortic node metastases were never observed when stations No. 1 and No. 3 were both negative. Patients were divided into three groups, according to the risk of para-aortic node invasion: (1) high-risk group (n = 24, 8.2%), presenting a 42% risk and comprising T3/T4 cancers with mixed/nonintestinal histology, arising from the upper third; (2) low-risk group (n = 138, 46.9%), presenting a 0–10% risk and including middle-lower third tumors—either T2 irrespective of histology, or T3/T4 with intestinal histology; (3) intermediate-risk group, comprising all other patients (n = 132, 44.9%). Their risk ranged between 16% and 30%, but increased up to 21–37.5% after excluding 33 patients with negative No. 1 and No. 3 stations.
Conclusions
The combination of tumor site, histology, and T stage with perigastric nodal status allowed identification of patients at higher risk of para-aortic nodal invasion who could benefit from para-aortic nodal dissection.


Similar content being viewed by others
References
Sobin LH, Wittekind C, editors. TNM classification of malignant tumors, 6th ed. New York: Wiley-Liss; 2002.
Di Leo A, Marrelli D, Roviello F, et al. Lymph node involvement in gastric cancer for different tumor site and T stage. Italian Research Group for Gastric Cancer (IRGGC) experience. J Gastrointest Surg. 2007;11:1146–53.
Kunisaki C, Shimada H, Yamaoka H, et al. Significance of para-aortic lymph node dissection in advanced gastric cancer. Hepatogastroenterology. 1999;46:2635–42.
Maeta M, Yamashiro H, Saito H, et al. A prospective pilot study of extended (D3) and superextended para-aortic lymphadenectomy (D4) in patients with T3 or T4 gastric cancer managed by total gastrectomy. Surgery. 1999;125:325–31.
Kunisaki C, Shimada H, Yamaoka H, et al. Indications for paraortic lymph node dissection in gastric cancer patients with paraortic lymph node involvement. Hepatogastroenterology. 2000;47:586–9.
Gunji Y, Suzuki T, Kobayashi S, et al. Evaluation of D3/D4 lymph node dissection for patients with grossly N2 positive advanced gastric cancer. Hepatogastroenterology. 2003;50:1178–82.
de Manzoni G, Verlato G, Guglielmi A, Laterza E, Genna M, Cordiano C. Prognostic significance of lymph node dissection in gastric cancer. Br J Surg. 1996;83:1064–7.
Marrelli D, Pedrazzani C, Neri A, Corso G, De Stefano A, Pinto E, Roviello F. Complications after extended (D2) and superextended (D3) lymphadenectomy for gastric cancer: analysis of potential risk factors. Ann Surg Oncol. 2007;14:25–33.
Günther K, Horbach T, Merkel S, Meyer M, Schnell U, Klein P, Hohenberger W. D3 lymph node dissection in gastric cancer: evaluation of postoperative mortality and complications. Surg Today. 2000;30:700–5.
Bostanci EB, Kayaalp C, Ozogul Y, Aydin C, Atalay F, Akoglu M. Comparison of complications after D2 and D3 dissection for gastric cancer. Eur J Surg Oncol. 2004;30:20–5.
Kulig J, Popiela T, Kolodziejczyk P, Sierzega M, Szczepanik A. Standard D2 versus extended D2 (D+) lymphadenectomy for gastric cancer: an interim safety analysis of a multicenter, randomized, clinical trial. Am J Surg. 2007;193:10–5.
Roviello F, Pedrazzani C, Marrelli D, et al. Super-extended (D3) lymphadenectomy in advanced gastric cancer. Eur J Surg Oncol. 2010;36:439–46.
Kodera Y. Para-aortic lymph node dissection revisited: have we been neglecting a promising treatment option for gastric carcinoma? (letter). Eur J Surg Oncol. 2010;36:447–8.
Sasako M, Sano T, Yamamoto S, et al. D2 lymphadenectomy alone or with para-aortic nodal dissection for gastric cancer. N Engl J Med. 2008;359:453–62.
Yonemura Y, Wu CC, Fukushima N, et al. Operative morbidity and mortality after D2 and D4 extended dissection for advanced gastric cancer: a prospective randomized trial conducted by Asian surgeons. Hepatogastroenterology. 2006;53:389–94.
Verlato G, Roviello F, Marchet A, Giacopuzzi S, Marrelli D, Nitti D, de Manzoni G. Indexes of surgical quality in gastric cancer surgery: experience of an Italian network. Ann Surg Oncol. 2009;16:594–602.
Japanese Gastric Cancer Association. Japanese classification of gastric carcinoma, 2th English edition. Gastric Cancer. 1998;1:10–24.
Yonemura Y, Wu CC, Fukushima N, et al. Metastasis in para-aortic lymph nodes in patients with advanced gastric cancer, treated with extended lymphadenectomy. Hepatogastroenterology. 2007;54:634–8.
Nomura E, Sasako M, Yamamoto S, et al. Risk factors for para-aortic lymph node metastasis of gastric cancer from a randomized controlled trial of JCOG9501. Jpn J Clin Oncol. 2007;37:429–33.
Zhou Y, Zhang Z, Zhang Z, et al. A rising trend of gastric cardia cancer in Gansu Province of China. Cancer Letters. 2008;269:18–25.
Hansen S, Wiig JN, Giercksky KE, Tretli S. Esophageal and gastric carcinoma in Norway 1958-1992: incidence time trend variability according to morphological subtypes and organ subsites. Int J Cancer. 1997;71:340–4.
Marrelli D, Pedrazzani C, Morgagni P, et al. (2009) Changing clinical and pathological features of gastric cancer in the period 1991–2005. A statistical evaluation of the Italian Research Group for Gastric Cancer (IRGGC) database on 2843 patients [abstract]. Eighth International Gastric Cancer Congress. Krakow, Poland, p. 25.
Conflicts of Interest
All of the authors declare that they have no potential commercial conflicts of interest relevant to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Manzoni, G., Di Leo, A., Roviello, F. et al. Tumor Site and Perigastric Nodal Status are the Most Important Predictors of Para-Aortic Nodal Involvement in Advanced Gastric Cancer. Ann Surg Oncol 18, 2273–2280 (2011). https://doi.org/10.1245/s10434-010-1547-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1547-5