Abstract
Background
A larger number of dissected lymph nodes (LN) during pelvic lymphadenectomy in patients with muscle-invasive transitional-cell carcinoma of the bladder treated by radical cystectomy (RC) is crucial for exact tumor staging and is associated with a positive oncological outcome.
Methods
Clinical and pathological records of 1291 patients undergoing RC due to LN-negative transitional-cell carcinoma of the bladder were summarized and evaluated in a multi-institutional database. The number of removed LNs and the presence or absence of lymphovascular invasion were assessed. On the basis of multivariate Cox regression analyses, a threshold number of removed LNs was defined that exerted an independent influence on cancer-specific survival (CSS).
Results
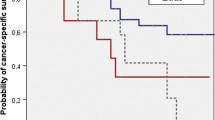
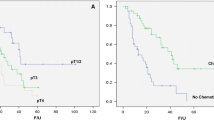
In multivariate Cox regression models for different numbers of removed LNs, a statistically significant enhancement of CSS could be demonstrated for a LN count of 16. Furthermore, the integration of the dichotomized LN count of 16 resulted in a statistically significantly enhanced predictive ability of the model for CSS. Patients with <16 and ≥16 removed LNs showed CSS rates after 5 years of 72% and 83%, respectively (P = 0.01). In addition, age, sex, pT stage, and lymphovascular invasion had independent influences on CSS in every Cox regression model.
Conclusions
In patients undergoing RC, removal of a higher LN count is associated with an improved oncological outcome. The information resulting from an assessment of lymphovascular invasion and an extended lymphadenectomy is critical for stratification of risk groups and identification of patients who might benefit from adjuvant treatment.


Similar content being viewed by others
References
Stein JP, Lieskovsky G, Cote R, et al. Radical cystectomy in the treatment of invasive bladder cancer: long-term results in 1,054 patients. J Clin Oncol. 2001;19:666–75.
Gore JL, Litwin MS, Lai J, et al. Use of radical cystectomy for patients with invasive bladder cancer. J Natl Cancer Inst. 2010;102:802–11.
Skinner DG. Management of invasive bladder cancer: a meticulous pelvic node dissection can make a difference. J Urol. 1982;128:34–6.
Poulsen AL, Horn T, Steven K. Radical cystectomy: extending the limits of pelvic lymph node dissection improves survival for patients with bladder cancer confined to the bladder wall. J Urol. 1998;160(6 Pt 1):2015–9.
Leissner J, Hohenfellner R, Thüroff JW, Wolf HK. Lymphadenectomy in patients with transitional cell carcinoma of the urinary bladder; significance for staging and prognosis. BJU Int. 2000;85:817–23.
Herr HW, Bochner BH, Dalbagni G, et al. Impact of the number of lymph nodes retrieved on outcome in patients with muscle invasive bladder cancer. J Urol. 2002;167:1295–8.
Konety BR, Joslyn SA, O’Donnell MA. Extent of pelvic lymphadenectomy and its impact on outcome in patients diagnosed with bladder cancer: analysis of data from the Surveillance, Epidemiology and End Results Program data base. J Urol. 2003;169:946–50.
Fleischmann A, Thalmann GN, Markwalder R, Studer UE. Prognostic implications of extracapsular extension of pelvic lymph node metastases in urothelial carcinoma of the bladder. Am J Surg Pathol. 2005;29:89–95.
Koppie TM, Vickers AJ, Vora K, Dalbagni G, Bochner BH. Standardization of pelvic lymphadenectomy performed at radical cystectomy: can we establish a minimum number of lymph nodes that should be removed? Cancer. 2006;107:2368–74.
Dhar NB, Klein EA, Reuther AM, Thalmann GN, Madersbacher S, Studer UE. Outcome after radical cystectomy with limited or extended pelvic lymph node dissection. J Urol. 2008;179:873–8.
Herr HW. Superiority of ratio based lymph node staging for bladder cancer. J Urol. 2003;169:943–5.
Stein JP, Cai J, Groshen S, Skinner DG. Risk factors for patients with pelvic lymph node metastases following radical cystectomy with en bloc pelvic lymphadenectomy: concept of lymph node density. J Urol. 2003;170:35–41.
Wright JL, Lin DW, Porter MP. The association between extent of lymphadenectomy and survival among patients with lymph node metastases undergoing radical cystectomy. Cancer. 2008;112:2401–8.
Sharir S, Fleshner NE. Lymph node assessment and lymphadenectomy in bladder cancer. J Surg Oncol. 2009;99:225–31.
Buscarini M, Josephson DY, Stein JP. Lymphadenectomy in bladder cancer: a review. Urol Int. 2007;79:191–9.
Herr HW. Extent of surgery and pathology evaluation has an impact on bladder cancer outcomes after radical cystectomy. Urology. 2003;61:105–8.
Wittekind C, Tischoff I. Tumor classifications. Pathologe. 2004;25:481–90.
Epstein JI, Amin MB, Reuter VR, Mostofi FK. The World Health Organization/International Society of Urological Pathology consensus classification of urothelial (transitional cell) neoplasms of the urinary bladder. Bladder Consensus Conference Committee. Am J Surg Pathol. 1998;22:1435–48.
Smith DD, Schwarz RR, Schwarz RE. Impact of total lymph node count on staging and survival after gastrectomy for gastric cancer: data from a large US-population database. J Clin Oncol. 2005;23:7114–24.
Chang GJ, Rodriguez-Bigas MA, Skibber JM, Moyer VA. Lymph node evaluation and survival after curative resection of colon cancer: systematic review. J Natl Cancer Inst. 2007;99:433–41.
Roscigno M, Shariat SF, Margulis V, et al. The extent of lymphadenectomy seems to be associated with better survival in patients with nonmetastatic upper-tract urothelial carcinoma: how many lymph nodes should be removed? Eur Urol. 2009;56:512–8.
Karl A, Carroll PR, Gschwend JE, et al. The impact of lymphadenectomy and lymph node metastasis on the outcomes of radical cystectomy for bladder cancer. Eur Urol. 2009;55:826–35.
Kurtz GA, McKinney JL, Lay CH. Toward quality measures in bladder cancer surgery: a population-based assessment of radical cystectomy in Ontario. J Urol. 2008;179(4 Suppl):581.
Herr H, Lee C, Chang S, Lerner S; Bladder Cancer Collaborative Group. Standardization of radical cystectomy and pelvic lymph node dissection for bladder cancer: a collaborative group report. J Urol. 2004;171:1823–8.
Weingärtner K, Ramaswamy A, Bittinger A, Gerharz EW, Vöge D, Riedmiller H. Anatomical basis for pelvic lymphadenectomy in prostate cancer: results of an autopsy study and implications for the clinic. J Urol. 1996;156:1969–71.
Leissner J, Ghoneim MA, Abol-Enein H, et al. Extended radical lymphadenectomy in patients with urothelial bladder cancer: results of a prospective multicenter study. J Urol. 2004;171:139–44.
Stenzl A, Cowan NC, De Santis M, et al. The updated EAU guidelines on muscle-invasive and metastatic bladder cancer. Eur Urol. 2009;55:815–25.
Heck MM, Gschwend JE, Retz M. Update on chemotherapy for bladder cancer. Update 2010. Urologe A. 2010;49:1294–300.
Capitanio U, Suardi N, Shariat SF, et al. Assessing the minimum number of lymph nodes needed at radical cystectomy in patients with bladder cancer. BJU Int. 2009;103:1359–62.
Author information
Authors and Affiliations
Corresponding author
Additional information
Matthias May and Edwin Herrmann contributed equally to this work.
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
May, M., Herrmann, E., Bolenz, C. et al. Association Between the Number of Dissected Lymph Nodes During Pelvic Lymphadenectomy and Cancer-Specific Survival in Patients with Lymph Node–Negative Urothelial Carcinoma of the Bladder Undergoing Radical Cystectomy. Ann Surg Oncol 18, 2018–2025 (2011). https://doi.org/10.1245/s10434-010-1538-6
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1538-6