Abstract
Background
The objective of this study was to assess the value of metastatic lymph node ratio in predicting prognosis of patients with stage III colorectal cancer.
Methods
From 2000 to 2005 inclusively, a total of 626 patients featuring stage III colorectal cancer underwent curative resection. These patients were stratified into LNR groups: 1 (0 < LNR ≤ 0.1); 2 (0.1 < LNR ≤ 0.25); 3 (0.25 < LNR ≤ 0.5); and 4 (LNR > 0.5). The follow-up was closed in April 2010. Kaplan-Meier survival curve and log-rank test were used to evaluate the prognostic value of LNR. A Cox regression model was used for multivariate analyses.
Results
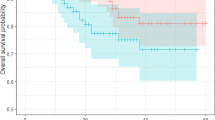
With a median follow-up period of 42.2 months, 5-year overall survival for groups LNR1, LNR2, LNR3, and LNR4 was 73%, 64%, 44%, and 22%, respectively. In the multivariate analysis, the LNR was an independent prognostic factor for survival (P < 0.001). LNR remained statistically significant (P < 0.001), both in patients with colon and rectum cancer regardless of the number of lymph nodes retrieved (≥12 or < 12). The survival rate of ratio group LNR1 was better than ratio group LNR4 (P < 0.001) for patients with the same IIIB or IIIC staging.
Conclusions
LNR is an accurate prognostic method for patients with stage III colorectal cancer. We proposed an algorithm to incorporate LNR into current AJCC staging system to form new staging.




Similar content being viewed by others
References
Garcia MJ, Ward E, Center M, et al. Global cancer facts & figures 2007. Atlanta: American Cancer Society; 2007.
Le Voyer TE, Sigurdson ER, Hanlon AL, et al. Colon cancer survival is associated with increasing number of lymph nodes analyzed: a secondary survey of intergroup trial INT-0089. J Clin Oncol. 2003;21:2912–9.
Redston M, Compton CC, Miedema BW, et al. Analysis of micrometastatic disease in sentinel lymph nodes from resectable colon cancer: results of Cancer and Leukemia Group B Trial 80001. J Clin Oncol. 2006;24:878–83.
Chapuis PH, Dent OF, Bokey EL, et al. Adverse histopathological findings as a guide to patient management after curative resection of node-positive colonic cancer. Br J Surg. 2004;91:349–54.
Wong SL, Ji H, Hollenbeck BK, et al. Hospital lymph node examination rates and survival after resection for colon cancer. JAMA. 2007;298:2149–54.
Burke HB. Outcome prediction and the future of the TNM staging system. J Natl Cancer Inst. 2004;96:1408–9.
Engstrom PF, Arnoletti JP, Benson AB 3rd, et al. NCCN clinical practice guidelines in oncology: colon cancer. J Natl Compr Cancer Netw. 2009;7:778–831.
Gajra A, Newman N, Gamble GP, et al. Effect of number of lymph nodes sampled on outcome in patients with stage I non-small-cell lung cancer. J Clin Oncol. 2003;21:1029–34.
Herr HW, Bochner BH, Dalbagni G, et al. Impact of the number of lymph nodes retrieved on outcome in patients with muscle invasive bladder cancer. J Urol. 2002;167:1295–8.
Weir L, Speers C, D’Yachkova Y, Olivotto IA. Prognostic significance of the number of axillary lymph nodes removed in patients with node-negative breast cancer. J Clin Oncol. 2002;20:1793–9.
Berger AC, Sigurdson ER, LeVoyer T, et al. Colon cancer survival is associated with decreasing ratio of metastatic to examined lymph nodes. J Clin Oncol. 2005;23:8706–12.
Greece F, Fleming I, Fritz A. AJCC cancer staging manual. New York: Springer-Verlag; 2002.
Desch CE, Benson AB 3rd, Somerfield MR, et al. Colorectal cancer surveillance: 2005 update of an American Society of Clinical Oncology practice guideline. J Clin Oncol. 2005;23:8512–9.
Sobin L, Wittekind C. TNM classification of malignant tumors. New York: Wiley-Blackwell; 2009.
Chang GJ, Rodriguez-Bigas MA, Skibber JM, Moyer VA. Lymph node evaluation and survival after curative resection of colon cancer: systematic review. J Natl Cancer Inst. 2007;99:433–41.
Vather R, Sammour T, Kahokehr A, et al. Lymph node evaluation and long-term survival in stage II and stage III colon cancer: a national study. Ann Surg Oncol. 2009;16:585–93.
Moug SJ, Saldanha JD, McGregor JR, et al. Positive lymph node retrieval ratio optimises patient staging in colorectal cancer. Br J Cancer. 2009;100:1530–3.
Park IJ, Choi GS, Jun SH. Nodal stage of stage III colon cancer: the impact of metastatic lymph node ratio. J Surg Oncol. 2009;100:240–3.
Peschaud F, Benoist S, Julie C, et al. The ratio of metastatic to examined lymph nodes is a powerful independent prognostic factor in rectal cancer. Ann Surg. 2008;248:1067–73.
Peng J, Xu Y, Guan Z, et al. Prognostic significance of the metastatic lymph node ratio in node-positive rectal cancer. Ann Surg Oncol. 2008;15:3118–23.
Lee HY, Choi HJ, Park KJ, et al. Prognostic significance of metastatic lymph node ratio in node-positive colon carcinoma. Ann Surg Oncol. 2007;14:1712–7.
Wang J, Hassett JM, Dayton MT, Kulaylat MN. Lymph node ratio: role in the staging of node-positive colon cancer. Ann Surg Oncol. 2008;15:1600–8.
Huh JW, Kim YJ, Kim HR. Ratio of metastatic to resected lymph nodes as a prognostic factor in node-positive colorectal cancer. Ann Surg Oncol. 2010; Mar 19. [Epub ahead of print].
Vaccaro CA, Im V, Rossi GL, et al. Lymph node ratio as prognosis factor for colon cancer treated by colorectal surgeons. Dis Colon Rectum. 2009;52:1244–50.
Kim YS, Kim JH, Yoon SM, et al. lymph node ratio as a prognostic factor in patients with stage III rectal cancer treated with total mesorectal excision followed by chemoradiotherapy. Int J Radiat Oncol Biol Phys. 2009;74:796–802.
Schumacher P, Dineen S, Barnett C Jr, et al. The metastatic lymph node ratio predicts survival in colon cancer. Am J Surg. 2007;194:827–31; discussion 831–2.
Acknowledgment
Supported by National Natural Science Foundation (30672408).
Author information
Authors and Affiliations
Corresponding author
Additional information
Hai-Bo Qiu and Li-Yi Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Qiu, HB., Zhang, LY., Li, YF. et al. Ratio of Metastatic To Resected Lymph Nodes Enhances To Predict Survival In Patients With Stage III Colorectal Cancer. Ann Surg Oncol 18, 1568–1574 (2011). https://doi.org/10.1245/s10434-010-1528-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1528-8