Abstract
Background
Patients with American Joint Committee on Cancer (AJCC) stage III melanoma represent patients with high risk of systemic relapse. This study evaluates the clinical utility of standardized radiographic staging.
Methods
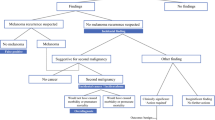
Consecutive asymptomatic patients underwent standardized radiographic staging workup within 6 weeks of diagnosis. True- and false-positive rates and number of additional examinations generated after a positive initial report were quantified. All suspicious findings were further studied by biopsy and/or by clinical or radiologic assessment.
Results
Fifty-eight patients underwent complete radiographic staging. Nineteen (33%) had ulcerated primary tumors. Forty-two patients (73%) presented with clinically negative lymph nodes that were positive on sentinel lymph node biopsy. Lymph node involvement was classified as N1a in 54%, N2a in 19%, N2b in 3%, and N3 in 22% of patients. Among 204 staging examinations in 58 patients, 52 (25%) were initially reported as positive. Three percent of all examinations proved truly positive; 23% were falsely positive. Analyzed per patient, in 37 (64%) of 58 patients, at least one examination was initially reported as positive. However, only 3 patients (5%) had a true-positive and 34 (59%) had at least one false-positive report. The positive reports of the staging scans generated 45 additional examinations (0.78 per patient).
Conclusions
Radiographic staging in asymptomatic patients with stage III melanoma detects a low number of patients with unsuspected systemic disease. The ratio of falsely to truly positive is approximately 11:1. Radiographic screening should only be considered in patients with high-risk prognostic features or symptoms, or in the context of clinical trials.
Similar content being viewed by others
References
Green FL, Page DL, Fleming ID, et al. AJCC cancer staging handbook. 6th ed. New York: Springer Verlag, 2002.
Balch CM, Soong SJ, Gershenwald JE, et al. Prognostic factors analysis of 17,600 melanoma patients: validation of the American Joint Committee on Cancer melanoma staging system. J Clin Oncol. 2001;19:3622–34.
Balch CM, Buzaid AC, Soong SJ, et al. Final version of the American Joint Committee on Cancer staging system for cutaneous melanoma. J Clin Oncol. 2001;19:3635–48.
Balch CM, Soong S, Ross MI, et al. Long-term results of a multi-institutional randomized trial comparing prognostic factors and surgical results for intermediate thickness melanomas (1.0 to 4.0 mm). Intergroup Melanoma Surgical Trial. Ann Surg Oncol. 2000;7:87–97.
Guggenheim MM, Hug U, Jung FJ, et al. Morbidity and recurrence after completion lymph node dissection following sentinel lymph node biopsy in cutaneous malignant melanoma. Ann Surg. 2008;247:687–93.
Coit DG, Andtbacka R, Bichakjian CK, et al. Melanoma. J Natl Compr Canc Netw. 2009;7:250–75.
Miranda EP, Gertner M, Wall J, et al. Routine imaging of asymptomatic melanoma patients with metastasis to sentinel lymph nodes rarely identifies systemic disease. Arch Surg. 2004;139:831–6.
Gold JS, Jaques DP, Busam KJ, et al. Yield and predictors of radiologic studies for identifying distant metastases in melanoma patients with a positive sentinel lymph node biopsy. Ann Surg Oncol. 2007;14:2133–40.
Buzaid AC, Tinoco L, Ross MI, et al. Role of computed tomography in the staging of patients with local-regional metastases of melanoma. J Clin Oncol. 1995;13:2104–8.
Aloia TA, Gershenwald JE, Andtbacka RH, et al. Utility of computed tomography and magnetic resonance imaging staging before completion lymphadenectomy in patients with sentinel lymph node-positive melanoma. J Clin Oncol. 2006;24:2858–65.
Johnson TM, Fader DJ, Chang AE, et al. Computed tomography in staging of patients with melanoma metastatic to the regional nodes. Ann Surg Oncol. 1997;4:396–402.
Kuvshinoff BW, Kurtz C, Coit DG. Computed tomography in evaluation of patients with stage III melanoma. Ann Surg Oncol. 1997;4:252–8.
Buzaid AC, Sandler AB, Mani S, et al. Role of computed tomography in the staging of primary melanoma. J Clin Oncol. 1993;11:638–43.
Longo MI, Lazaro P, Bueno C, et al. Fluorodeoxyglucose-positron emission tomography imaging versus sentinel node biopsy in the primary staging of melanoma patients. Dermatol Surg. 2003;29:245–8.
Wagner JD, Schauwecker D, Davidson D, et al. Prospective study of fluorodeoxyglucose-positron emission tomography imaging of lymph node basins in melanoma patients undergoing sentinel node biopsy. J Clin Oncol. 1999;17:1508–15.
Eigtved A, Andersson AP, Dahlstrom K, et al. Use of fluorine-18 fluorodeoxyglucose positron emission tomography in the detection of silent metastases from malignant melanoma. Eur J Nucl Med. 2000;27:70–5.
Holder WD Jr, White RL Jr, Zuger JH, et al. Effectiveness of positron emission tomography for the detection of melanoma metastases. Ann Surg. 1998;227:764–9.
Prichard RS, Hill AD, Skehan SJ, O’Higgins NJ. Positron emission tomography for staging and management of malignant melanoma. Br J Surg. 2002;89:389–96.
Rinne D, Baum RP, Hor G, Kaufmann R. Primary staging and follow-up of high risk melanoma patients with whole-body 18F-fluorodeoxyglucose positron emission tomography: results of a prospective study of 100 patients. Cancer. 1998;82:1664–71.
Horn J, Lock-Andersen J, Sjostrand H, Loft A. Routine use of FDG-PET scans in melanoma patients with positive sentinel node biopsy. Eur J Nucl Med Mol Imaging. 2006;33:887–92.
Meyers MO, Yeh JJ, Frank J, et al. Method of detection of initial recurrence of stage II/III cutaneous melanoma: analysis of the utility of follow-up staging. Ann Surg Oncol. 2009;16:941–7.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Poster presentation at the Annual Meeting of the Society of Surgical Oncology in March, 2010.
Rights and permissions
About this article
Cite this article
Pandalai, P.K., Dominguez, F.J., Michaelson, J. et al. Clinical Value of Radiographic Staging in Patients Diagnosed With AJCC Stage III Melanoma. Ann Surg Oncol 18, 506–513 (2011). https://doi.org/10.1245/s10434-010-1272-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-010-1272-0