Abstract
Background
The purpose of this study was to examine whether or not immediate microvascular free flap reconstruction influences survival among treated patients suffering from oral squamous cell carcinoma (OSCC), controlling for demographic, clinical, and tumor characteristics.
Methods
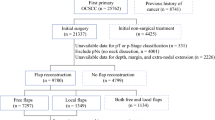
773 patients with OSCC were treated with curative intent. Two hundred and seventy-four patients were immediately reconstructed using free microsurgical flaps. All measures were collected by chart abstraction. Kaplan–Meier plots and univariate log-rank test and multivariate Cox proportional hazards regression models were used to determine the association between possible predictor variables and survival time. In addition, a randomized matched-pair analysis was conducted to compensate different patient cohorts.
Results
After controlling for age, tumor stage, nodal stage, and tumor grade, which were independent and dependent predictors of survival, microsurgical free flap reconstruction was associated with survival [hazard ratio (HR) = 0.66, P < 0.001, 95% confidence interval (CI), 0.52 to 0.83]. In the randomized matched-pair analysis this effect became more evident (HR = 0.58, P < 0.001, 95% CI, 0.44 to 0.75). Controlling for extent of tumor, only T3 and T4 tumors were significantly associated with survival (P < 0.001, HR = 0.46, 95% CI, 0.31 to 0.69) when the area of defect was reconstructed, whereas in T1 and T2 tumors no significance was noted (P = 0.08, HR = 0.74, 95% CI, 0.53 to 1.04).
Conclusions
Reconstruction of defects, especially in patients presenting with higher tumor stages, is not associated with shorter overall survival rates, as revealed in this study, and should be considered when functional deficits due to tumor ablation can be expected postoperatively.


Similar content being viewed by others
References
Cunningham MJ, Johnson JT, Myers EN, et al. Cervical lymph node metastasis after local excision of early squamous cell carcinoma of the oral cavity. Am J Surg. 1986;152:361–6.
Chang HW, Ling GS, Wei WI, et al. Smoking and drinking can induce p15 methylation in the upper aerodigestive tract of healthy individuals and patients with head and neck squamous cell carcinoma. Cancer. 2004;101:125–32.
Forastiere A, Koch W, Trotti A, et al. Head and neck cancer. N Engl J Med. 2001;345:1890–900.
Pignon JP, Bourhis J, Domenge C, et al. Chemotherapy added to locoregional treatment for head and neck squamous-cell carcinoma: three meta-analyses of updated individual data. MACH-NC Collaborative Group. Meta-Analysis of Chemotherapy on Head and Neck Cancer. Lancet 2000;355:949–55.
Shah JP, Gil Z. Current concepts in management of oral cancer–surgery. Oral Oncol. 2009;45:394–401.
Karvonen-Gutierrez CA, Ronis DL, Fowler KE, et al. Quality of life scores predict survival among patients with head and neck cancer. J Clin Oncol. 2008;26:2754–60.
Piccirillo JF. Inclusion of comorbidity in a staging system for head and neck cancer. Oncology (Williston Park). 1995;9:831–6 (discussion 841, 845-8).
Vokes EE, Weichselbaum RR, Lippman SM, et al. Head and neck cancer. N Engl J Med. 1993;328:184–94.
Schusterman MA, Horndeski G. Analysis of the morbidity associated with immediate microvascular reconstruction in head and neck cancer patients. Head Neck. 1991;13:51–5.
Boysen M, Lovdal O, Tausjo J, et al. The value of follow-up in patients treated for squamous cell carcinoma of the head and neck. Eur J Cancer. 1992;28:426–30.
Jones KR, Lodge-Rigal RD, Reddick RL, et al. Prognostic factors in the recurrence of stage I and II squamous cell cancer of the oral cavity. Arch Otolaryngol Head Neck Surg. 1992;118:483–5.
Kowalski LP. Results of salvage treatment of the neck in patients with oral cancer. Arch Otolaryngol Head Neck Surg. 2002;128:58–62.
Liu SA, Wong YK, Lin JC, et al. Impact of recurrence interval on survival of oral cavity squamous cell carcinoma patients after local relapse. Otolaryngol Head Neck Surg. 2007;136:112–8.
Nathanson A, Agren K, Biorklund A, et al. Evaluation of some prognostic factors in small squamous cell carcinoma of the mobile tongue: a multicenter study in Sweden. Head Neck. 1989;11:387–92.
Wong LY, Wei WI, Lam LK, et al. Salvage of recurrent head and neck squamous cell carcinoma after primary curative surgery. Head Neck. 2003;25:953–9.
Mücke T, Wagenpfeil S, Kesting MR, et al. Recurrence interval affects survival after local relapse of oral cancer. Oral Oncol. 2009;45:687–91.
Greenlee RT, Murray T, Bolden S, et al. Cancer statistics, 2000. CA Cancer J Clin. 2000;50:7–33.
Shah JP, Lydiatt W. Treatment of cancer of the head and neck. CA Cancer J Clin. 1995;45:352–68.
Hudgins PA. Flap reconstruction in the head and neck: expected appearance, complications, and recurrent disease. Eur J Radiol. 2002;44:130–8.
Kesting MR, Robitzky LK, Al-Benna S, et al. Bronchoscopy screening in primary oral squamous cell carcinoma: a 10-year experience. Br J Oral Maxillofac Surg. 2009;47(4):279–83.
Boysen M, Natvig K, Winther FO, et al. Value of routine follow-up in patients treated for squamous cell carcinoma of the head and neck. J Otolaryngol. 1985;14:211–4.
Abdi H. Bonferroni and Sidak corrections for multiple comparisons. In: Salkind N, editor. Encyclopedia of measurement and statistics. Thousand Oaks, CA: Sage; 2007. pp. 103–7.
Macfarlane GJ, McBeth J, Silman AJ. Widespread body pain and mortality: prospective population based study. BMJ. 2001;323:662–5.
McBeth J, Silman AJ, Macfarlane GJ. Association of widespread body pain with an increased risk of cancer and reduced cancer survival: a prospective, population-based study. Arthritis Rheum. 2003;48:1686–92.
van Bokhorst-de van der S, van Leeuwen PA, Kuik DJ, et al. The impact of nutritional status on the prognoses of patients with advanced head and neck cancer. Cancer. 1999;86:519–27.
Hassanein KA, Musgrove BT, Bradbury E. Functional status of patients with oral cancer and its relation to style of coping, social support and psychological status. Br J Oral Maxillofac Surg. 2001;39:340–5.
Holzle F, Kesting MR, Holzle G, et al. Clinical outcome and patient satisfaction after mandibular reconstruction with free fibula flaps. Int J Oral Maxillofac Surg. 2007;36:802–6.
Chen YK, Huang HC, Lin LM, et al. Primary oral squamous cell carcinoma: an analysis of 703 cases in southern Taiwan. Oral Oncol. 1999;35:173–9.
Hibbert J, Marks NJ, Winter PJ, et al. Prognostic factors in oral squamous carcinoma and their relation to clinical staging. Clin Otolaryngol Allied Sci. 1983;8:197–203.
Levy R, Segal K, Hadar T, et al. Squamous cell carcinoma of the oral tongue. Eur J Surg Oncol. 1991;17:330–4.
Gonzalez-Moles MA, Esteban F, Rodriguez-Archilla A, et al. Importance of tumour thickness measurement in prognosis of tongue cancer. Oral Oncol. 2002;38:394–7.
Koo BS, Lim YC, Lee JS, et al. Recurrence and salvage treatment of squamous cell carcinoma of the oral cavity. Oral Oncol. 2006;42:789–94.
Rogers SN, Brown JS, Woolgar JA, et al. Survival following primary surgery for oral cancer. Oral Oncol. 2009;45:201–11.
Leite IC, Koifman S: Survival analysis in a sample of oral cancer patients at a reference hospital in Rio de Janeiro, Brazil. Oral Oncol. 1998;34:347–52.
Aksu G, Karadeniz A, Saynak M, et al. Treatment results and prognostic factors in oral tongue cancer: analysis of 80 patients. Int J Oral Maxillofac Surg. 2006;35:506–13.
Carvalho AL, Nishimoto IN, Califano JA, et al. Trends in incidence and prognosis for head and neck cancer in the United States: a site-specific analysis of the SEER database. Int J Cancer. 2005;114:806–16.
Loree TR, Strong EW. Significance of positive margins in oral cavity squamous carcinoma. Am J Surg. 1990;160:410–4.
Binahmed A, Nason RW, Abdoh AA. The clinical significance of the positive surgical margin in oral cancer. Oral Oncol. 2007;43:780–4.
Brennan JA, Mao L, Hruban RH, et al. Molecular assessment of histopathological staging in squamous-cell carcinoma of the head and neck. N Engl J Med. 1995;332:429–35.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mücke, T., Wolff, KD., Wagenpfeil, S. et al. Immediate Microsurgical Reconstruction After Tumor Ablation Predicts Survival Among Patients with Head and Neck Carcinoma. Ann Surg Oncol 17, 287–295 (2010). https://doi.org/10.1245/s10434-009-0758-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-009-0758-0