Abstract
Background
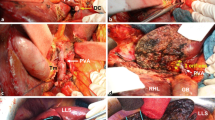
Radical operation for hilar cholangiocellular carcinoma, including extended hepatic resection, seems to improve prognosis by increasing the surgical curability rate. Nevertheless, high postoperative morbidity and mortality have been reported in patients with obstructive jaundice. We describe the technique of “high hilar resection” and a modification of bilioenteric anastomosis for drainage of the multiple secondary or tertiary biliary radicals.
Methods
Ten patients with advanced hilar cholangiocellular carcinoma underwent a high hilar resection with complete parenchymal preservation, and the biliary drainage was reconstructed by a sheath-to-enteric hepaticojejunostomy. Because of the technical difficulty caused by anastomosis line in the range of the biliary sheath, a modification was performed by dividing the biliary apertures of segments 5 and 4b.
Results
A high hilar resection was successfully performed, and all patients were discharged from the hospital in good condition. No patient died postoperatively. The proximal resection margin was tumor-free in all patients. One patient died after 29 months of peritoneal carcinomatosis. None of the patients developed local recurrence around the hepaticojejunostomy. The remaining nine patients are alive after a mean follow-up of 28.8 months after surgery without any signs of recurrence.
Conclusion
In highly selected patients with advanced hilar cholangiocellular carcinoma, a high hilar resection is technically safe and oncologically justifiable. In combination with our new technique of sheath-to-enteric anastomosis, the patients considerably benefit from the preservation of liver parenchyma with low postoperative morbidity and very short in-hospital stay.





Similar content being viewed by others
References
Vautey JN, Blumgart LH. Recent advances in the management of cholangiocarcinomas. Semin Liver Dis 1994; 14:109–14.
Khan SA, Davidson BR, Goldin R, et al. Guidelines for the diagnosis and treatment of cholangiocellular carcinoma: consensus document. Gut 2002; 51:1–9.
Bismuth H, Nakache R, Diamont T. Management strategies in resection for hilar cholangiocarcinoma. Ann Surg 1992; 215:31–8.
Tsao JI, Nimura Y, Kamiya J, et al. Management of hilar cholangiocarcinoma: comparison of an American and Japanese experience. Ann Surg 2000; 232:166–74.
Kawasaki S, Imamura H, Kobayashi A, et al. Results of surgical resection for patients with hilar bile duct cancer: application of extended hepatectomy after biliary drainage and hemihepatic portal vein embolization. Ann Surg 2003; 238:84–92.
Jarnagin WR, Fong Y, DeMatteo RP, et al. Staging, respectability, and outcome in 225 patients with hilar cholangiocarcinoma. Ann Surg 2001; 234:507–19.
Silva MA, Tekin K, Aytekin F, et al. Surgery for hilar cholangiocarcinoma; a 10 year experience of a tertiary referral centre in the UK. EJSO 2005; 31:533–9.
Jarnagin WR, Bownw W, Klimstra DS, et al. Papillary phenotype confers improved survival after resection of hilar cholangiocarcinoma. Ann Surg 2005; 241:703–14.
Liver Cancer Study Group of Japan. The General Rules for the Clinical and Pathological Study of Primary Liver Cancer. 4th edition. Tokyo: Kanehara. 2000.
Cameron JL, Pitt HA, Zinner MJ, et al. Management of proximal cholangiocarcinoma by surgical resection and radiotherapy. Am J Surg 1990; 159:91–8.
Fortner JG, Vitelli CE, Maclean BJ. Proximal extrahepatic bile duct tumors; analysis of a series of 52 consecutive patients treated over a period of 13 years. Arch Surg 1989; 124:1275–9.
Sugiura Y, Nakamura S, Iida S, et al. Extensive resection of the bile ducts combined with liver resection for cancer of the main hepatic junction: A cooperative study of the Keio Bile Duct Cancer Study Group. Surgery 1994; 115:445–51.
Seyama Y, Kubota K, Sano K, et al. Long-term outcome of extended hemihepatectomy for hilar bile duct cancer with no mortality and high survival rate. Ann Surg 2003; 238:73–83.
Bismuth H, Castaing D, Traynor O. Resection or palliation: priority of surgery in the treatment of hilar cancer. World J Surg 1988; 12:39–47.
Miyazaki M, Ito H, Nakagawa K, et al. Parenchyma-preserving hepatectomy in the surgical treatment of hilar cholangiocarcinoma. J Am Coll Surg 1999; 189:575–83.
Nagino M, Kamiya J, Arai T, et al. “Anatomic” right hepatic trisectionectomy (extended right hepatectomy) with caudate lobectomy for hilöar cholangiocarcinoma. Ann Surg 2006; 243:28–32.
Baton O, Azoulay D, Adam DVR, et al. Major hepatectomy for hilar cholangiocarcinoma type 3 and 4: prognostic factors and longterm outcomes. J Am Coll Surg 2007; 204:250–60.
Kosuge T, Yamamoto J, Shimada K, et al. Improved surgical results for hilar cholangiocarcinoma with procedures including major hepatic resection. Ann Surg 1999; 230:663–71.
Liu CL, Fan ST, Lo CM, et al. Improved operative and survival outcomes of surgical treatment for hilar cholangiocarcinoma. Br J Surg 2006; 93:1488–94.
Seyama Y, Makuuchi M. Current surgical treatment for bile duct cancer. World J Gastroenterol 2007; 13:1505–15.
Launois B, Jamieson GG. The importance of Glisson’s capsule and its sheath in the intrahepatic approach to resection of the liver. Surg Gynecol Obstet 1992; 174:7–10.
Khan AZ, Makuuchi M. Trends in the surgical management of Klatskin tumours. Br J Surg 2007; 94:393–4.
Shigeta H, Nagino M, Kamiya J, et al. Bacteremia after hepatectomy: an analysis of single center, 10-year experience with 407 patients. Langenbecks Arch Surg 2002; 387:117–24.
Yedibela S, Gohl J, Graz V, et al. Changes in indication and results after resection of hepatic metastases from noncolorectal primary tumors: a single-institutional review. Ann Surg Oncol 2005; 12:778–85.
Llovet JM, Fuster J, Bruix J. Intention-to-treat analysis of surgical treatment for early hepatocellular carcinoma: resection versus transplantation. Hepatology 1999; 30:1434–40.
Poon RT, Fan ST, Lo CM, et al. Improving perioperative expands the role of hepatectomy in management of benign and malignant hepatobiliary diseases: analysis of 1222 consecutive patients from a prospective database. Ann Surg 2004; 240:698–708.
Pichlmayr R, Weimann A, Klempnauer J, et al. Surgical treatment in proximal bile duct cancer; a single-center experience. Ann Surg 1996; 224:628–38.
Neuhaus P, Jonas S, Bechstein WO, et al. Extended resection for hilar cholangiocarcinoma. Ann Surg 1999; 230:808–19.
Kondo S, Hirano S, Ambo Y, et al. Forty consecutive resections of hilar cholangiocarcinoma with no postoperative mortality and no positive ductal margins. Ann Surg 2004; 240:95–101.
Tomioka M, Iinuma H, Okinaga K. Impaired Kupffer cell function and effect of immunotherapy in obstructive jaundice. J Surg Res 2000; 92:276–82.
Clements WD, McCaigue M, Erwin P, et al. Biliary decompression promotes Kupffer cell recovery in obstructive jaundice. Gut 1996; 38:925–31.
Katz S, Yang R, Rodefeld MJ, et al. Impaired hepatic bacterial clearance is reversed by surgical relief of obstructive jaundice. J Pediatr Surg 1991; 26:401–5.
Vane DW, Redlich P, Weber T, et al. Impaired immune function in obstructive jaundice. J Surg Res 1988; 45:287–93.
Dinant S, Gerhards MF, Rauws EAJ, et al. Improved outcome of resection of hilar cholangiocarcinoma (klatskin tumor). Ann Surg 2006; 13:872–80.
Kasai M., Kimura S, Asakura Y, et al. Surgical treatment of biliary atresia. J Pediatr Surg 1968; 3:665–75.
Icoz G, Kilic M, Zeytunlu M, et al. Biliary reconstructions and complications encountered in 50 consecutive right-lobe living donor liver transplantations. Liver Transpl 2003; 9:575–80.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aydin, U., Yedibela, S., Yazici, P. et al. A New Technique of Biliary Reconstruction After “High Hilar Resection” of Hilar Cholangiocarcinoma with Tumor Extension to Secondary and Tertiary Biliary Radicals. Ann Surg Oncol 15, 1871–1879 (2008). https://doi.org/10.1245/s10434-008-9926-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-008-9926-x