Abstract
Atopic dermatitis is a chronic inflammatory disorder with rising prevalence. The safety concerns over usually used steroids are driving the need for developing an effective atopic dermatitis treatment. The use of therapeutic agents such as cromolyn sodium (CS) is suggested. However, due to its physicochemical properties, CS permeation across the skin is a challenge. The aim of this study was to investigate the effect of sodium salts of fatty acids or their derivatives with varied carbon chain lengths as potential enhancers on the skin permeation of CS. These included sodium caprylate, salcaprozate sodium, sodium decanoate, sodium palmitate, and sodium oleate dissolved in propylene glycol along with CS (4% w/w). In vitro permeation of the formulations across the dermatomed porcine ear skin was investigated over 24 h using Franz Diffusion cells. The amount of CS permeation from propylene glycol was 5.54 ± 1.06 µg/cm2 after 24 h. Initial screening of enhancers (enhancer: drug::1:1) showed enhancement in permeation of CS using sodium oleate and sodium caprylate, which were then investigated in higher ratio of drug: enhancer (1:2). Among all the formulations tested, sodium oleate (enhancer: drug::1:2) was observed to significantly (p < 0.05) enhance the permeation of CS with the highest total delivery of 359.79 ± 78.92 µg/cm2 across skin in 24 h and higher drug retention in the skin layers (153.0 ± 24.93 µg/cm2) as well. Overall, sodium oleate was found to be the most effective enhancer followed by sodium caprylate for improving the topical delivery of CS.
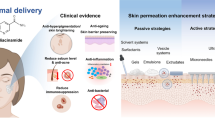
Graphical Abstract









Similar content being viewed by others
Data availability
All the data related to the study is contained within the manuscript.
Abbreviations
- AD:
-
Atopic dermatitis
- CS:
-
Cromolyn sodium
- HPLC:
-
High-performance liquid chromatography
- PE:
-
Permeation enhancer
- PG:
-
Propylene glycol
- SC:
-
Stratum corneum
- SNAC:
-
Salcaprozate sodium
References
Avena-Woods C. Overview of atopic dermatitis. Am J Manag Care [Internet]. 2017 Jun 1 [cited 2023 Jun 1];23(8 Suppl):S115–23. Available from: https://europepmc.org/article/med/28978208
Hajar T, Simpson EL. The rise in atopic dermatitis in young children: what is the explanation? JAMA Netw Open [Internet]. 2018 Nov 2 [cited 2023 Jun 1];1(7):e184205–e184205. Available from: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2712172
Kim J, Kim BE, Leung DYM. Pathophysiology of atopic dermatitis: clinical implications. Allergy Asthma Proc [Internet]. 2019 [cited 2023 Jun 1];40(2):84. Available from: /pmc/articles/PMC6399565/
Levin J, Friedlander SF, Del Rosso JQ. Atopic dermatitis and the stratum corneum: Part 1: the role of filaggrin in the stratum corneum barrier and atopic skin. J Clin Aesthet Dermatol [Internet]. 2013 Oct [cited 2023 Jun 1];6(10):16. Available from: /pmc/articles/PMC3805301/
Sandilands A, Sutherland C, Irvine AD, McLean WHI. Filaggrin in the frontline: role in skin barrier function and disease. J Cell Sci [Internet]. 2009 May 5 [cited 2023 Jun 1];122(9):1285. Available from: /pmc/articles/PMC2721001/
Wang V, Boguniewicz J, Boguniewicz M, Ong PY. The infectious complications of atopic dermatitis. Ann Allergy Asthma Immunol. 2021;126(1):3–12.
Berke R, Singh A, Guralnick M. Atopic dermatitis: an overview. Am Fam Physician [Internet]. 2012 Jul;86(1):35—42. Available from: http://europepmc.org/abstract/MED/22962911
Na CH, Chung J, Simpson EL. Quality of life and disease impact of atopic dermatitis and psoriasis on children and their families. Vol. 6, Children. 2019.
Sidbury R, Tom WL, Bergman JN, Cooper KD, Silverman RA, Berger TG, et al. Guidelines of care for the management of atopic dermatitis: Section 4. Prevention of disease flares and use of adjunctive therapies and approaches. J Am Acad Dermatol [Internet]. 2014 Dec 1 [cited 2023 Jun 2];71(6):1218–33. Available from: http://www.jaad.org/article/S0190962214018878/fulltext
Eichenfield LF, Tom WL, Berger TG, Krol A, Paller AS, Schwarzenberger K, et al. Guidelines of care for the management of atopic dermatitis: Section 2. Management and treatment of atopic dermatitis with topical therapies. J Am Acad Dermatol [Internet]. 2014 Jul 1 [cited 2023 Jun 2];71(1):116–32. Available from: http://www.jaad.org/article/S0190962214012572/fulltext
Sidbury R, Davis DM, Cohen DE, Cordoro KM, Berger TG, Bergman JN, et al. Guidelines of care for the management of atopic dermatitis: section 3. Management and treatment with phototherapy and systemic agents. J Am Acad Dermatol [Internet]. 2014 [cited 2023 Jun 2];71(2):327–49. Available from: https://pubmed.ncbi.nlm.nih.gov/24813298/
Atopic Dermatitis Treatment Market [Internet]. 2022. Atopic Dermatitis Treatment Market Analysis & Opportunity. Available from: https://www.futuremarketinsights.com/reports/atopic-dermatitis-treatment-market
Edwards AM, Stevens MT, Church MK. The effects of topical sodium cromoglicate on itch and flare in human skin induced by intradermal histamine: a randomised double-blind vehicle controlled intra-subject design trial. BMC Res Notes [Internet]. 2011 [cited 2023 Jun 3];4:47. Available from: /pmc/articles/PMC3060830/
Shapiro GG, Konig P. Cromolyn sodium: a review. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy [Internet]. 1985 May 6 [cited 2023 Jun 3];5(3):156–70. Available from: https://onlinelibrary.wiley.com/doi/full/https://doi.org/10.1002/j.1875-9114.1985.tb03412.x
Zur E. Topical use of sodium cromoglicate (cromolyn sodium) to treat atopic dermatitis and other skin allergies. Vol. 16, International journal of pharmaceutical compounding. 2012.
Kimata H, Igarashi M. Topical cromolyn (disodium cromoglycate) solution in the treatment of young children with atopic dermatitis. Clinical & Experimental Allergy. 1990;20(3).
Haider SA. Treatment of atopic eczema in children: clinical trial of 10% sodium cromoglycate ointment. Br Med J. 1977;1(6076).
Ariyanayagam M, Barlow TJ, Graham P, Hall-Smith SP, Harris JM. Topical sodium cromoglycate in the management of atopic eczema—a controlled trial. British Journal of Dermatology. 1985;112(3).
Holman M, Tijani A, Klein J, Frempong D, Dinh S, Puri A. Penetration enhancement strategies for intradermal delivery of cromolyn sodium. AAPS PharmSciTech [Internet]. 2022 Aug 1 [cited 2023 Jun 14];23(6). Available from: https://pubmed.ncbi.nlm.nih.gov/35739411/
Puri A, Murnane KS, Blough BE, Banga AK. Effects of chemical and physical enhancement techniques on transdermal delivery of 3-fluoroamphetamine hydrochloride. Int J Pharm. 2017;528(1–2):452–62.
Tavano L, Nicoletta FP, Picci N, Muzzalupo R. Cromolyn as surface active drug (surfadrug): effect of the self-association on diffusion and percutaneous permeation. Colloids Surf B Biointerfaces. 2016;1(139):132–7.
Alkilani AZ, McCrudden MTC, Donnelly RF. Transdermal drug delivery: innovative pharmaceutical developments based on disruption of the barrier properties of the stratum corneum. Pharmaceutics [Internet]. 2015 Oct 22 [cited 2023 Jun 3];7(4):438. Available from: /pmc/articles/PMC4695828/
Haque T, Talukder MMU. Chemical enhancer: a simplistic way to modulate barrier function of the stratum corneum. Adv Pharm Bull [Internet]. 2018 [cited 2023 Jun 2];8(2):169. Available from: /pmc/articles/PMC6046426/
Ibrahim SA, Li SK. Effects of chemical enhancers on human epidermal membrane: structure-enhancement relationship based on maximum enhancement (Emax). J Pharm Sci [Internet]. 2009 [cited 2023 Jun 3];98(3):926. Available from: /pmc/articles/PMC2635431/
Karande P, Mitragotri S. Enhancement of transdermal drug delivery via synergistic action of chemicals. Biochimica et Biophysica Acta (BBA) - Biomembranes. 2009 Nov 1;1788(11):2362–73.
Ibrahim SA, Li SK. Efficiency of fatty acids as chemical penetration enhancers: mechanisms and structure enhancement relationship. Pharm Res. 2010;27(1).
Kim MJ, Doh HJ, Choi MK, Chung SJ, Shim CK, Kim DD, et al. Skin permeation enhancement of diclofenac by fatty acids. Drug Deliv. 2008;15(6).
K K, N K, S A, M S. Effect of fatty acids on the permeation of melatonin across rat and pig skin in-vitro and on the transepidermal water loss in rats in-vivo. J Pharm Pharmacol [Internet]. 1999 Feb 18 [cited 2023 Jun 3];51(7):783–90. Available from: https://pubmed.ncbi.nlm.nih.gov/10467952/
Cho CW, Choi JS, Yang KH, Shin SC. Enhanced transdermal absorption and pharmacokinetic evaluation of pranoprofen-ethylene-vinyl acetate matrix containing penetration enhancer in rats. Arch Pharm Res. 2009;32(5).
Aungst BJ, J. Rogers N, Shefter E. Enhancement of naloxone penetration through human skin in vitro using fatty acids, fatty alcohols, surfactants, sulfoxides and amides. Int J Pharm. 1986 Nov 1;33(1–3):225–34.
Kim T, Kang E, Chun I, Gwak H. Pharmacokinetics of formulated tenoxicam transdermal delivery systems. Journal of Pharmacy and Pharmacology. 2010;60(1).
Choi A, Gang H, Chun I, Gwak H. The effects of fatty acids in propylene glycol on the percutaneous absorption of alendronate across the excised hairless mouse skin. Int J Pharm. 2008;357(1–2):126–31.
Twarog C, Fattah S, Heade J, Maher S, Fattal E, Brayden DJ. Intestinal permeation enhancers for oral delivery of macromolecules: a comparison between salcaprozate sodium (SNAC) and sodium caprate (c10). Vol. 11, Pharmaceutics. 2019.
Twarog C, Liu K, O’Brien PJ, Dawson KA, Fattal E, Illel B, et al. A head-to-head Caco-2 assay comparison of the mechanisms of action of the intestinal permeation enhancers: SNAC and sodium caprate (C10). Eur J Pharm Biopharm. 2020;1(152):95–107.
Ali Chisty MN, Bellantone RA, Taft DR, Plakogiannis FM. In vitro evaluation of the release of albuterol sulfate from polymer gels: effect of fatty acids on drug transport across biological membranes. https://doi.org/10.1081/DDC-120015355 [Internet]. 2002 [cited 2023 Jun 6];28(10):1221–9. Available from: https://www.tandfonline.com/doi/abs/10.1081/DDC-120015355
Del Rio Sancho S, Serna Jiménez C, Calatayud Pascual M, Balaguer Fernández C, Femenía Font A, Castillo García E, et al. Evaluation of percutaneous absorption of esculetin: effect of chemical enhancers. Planta Med. 2013;79(2).
Roy SD, Roos E, Sharma K. Transdermal delivery of buprenorphine through cadaver skin. J Pharm Sci. 1994;83(2):126–30.
Al-Akayleh F, Adwan S, Khanfer M, Idkaidek N, Al-Remawi M. A novel eutectic-based transdermal delivery system for risperidone. AAPS PharmSciTech [Internet]. 2021 Jan 1 [cited 2023 Jun 6];22(1):1–11. Available from: https://link.springer.com/article/https://doi.org/10.1208/s12249-020-01844-4
Datta D, Panchal DS, Venuganti VVK. Transdermal delivery of vancomycin hydrochloride: influence of chemical and physical permeation enhancers. Int J Pharm. 2021;1(602): 120663.
Goodman M, Barry BW. Action of penetration enhancers on human skin as assessed by the permeation of model drugs 5-fluorouracil and estradiol. I. Infinite Dose Technique. Journal of Investigative Dermatology. 1988 Oct 1;91(4):323–7.
Golden GM, McKie JE, Potts RO. Role of stratum corneum lipid fluidity in transdermal drug flux. J Pharm Sci. 1987;76(1):25–8.
Francoeur ML, Golden GM, Potts RO. Oleic acid: its effects on stratum corneum in relation to (trans)dermal drug delivery. Pharmaceutical Research: An Official Journal of the American Association of Pharmaceutical Scientists [Internet]. 1990 [cited 2023 Jun 6];7(6):621–7. Available from: https://link.springer.com/article/https://doi.org/10.1023/A:1015822312426
Kumar P, Singh S, Mishra D, Girotra P. Enhancement of ketorolac tromethamine permeability through rat skin using penetration enhancers: an ex-vivo study. Int J Pharm Investig. 2015;5(3).
Novartis Pharmaceuticals Corporation. East Hanover, NJ. 2001. Vivelle® (estradiol transdermal system) [package insert].
Puri A, Nguyen HX, Banga AK. Microneedle-mediated intradermal delivery of epigallocatechin-3-gallate. Int J Cosmet Sci. 2016;38(5).
Nguyen HX, Puri A, Bhattaccharjee SA, Banga AK. Qualitative and quantitative analysis of lateral diffusion of drugs in human skin. Int J Pharm. 2018;544(1).
ICH. ICH Topic Q2 (R1) Validation of analytical procedures : text and methodology. International Conference on Harmonization. 2005;1994(November 1996).
Tijani A, Dogra P, Peláez MJ, Wang Z, Cristini V, Puri A. Mechanistic modeling-guided optimization of microneedle-based skin patch for rapid transdermal delivery of naloxone for opioid overdose treatment. Drug Deliv Transl Res [Internet]. 2022 [cited 2022 Dec 4]; Available from: https://pubmed.ncbi.nlm.nih.gov/35879533/
Sinha VR, Pal Kaur M. Permeation enhancers for transdermal drug delivery. https://doi.org/10.1081/DDC-100100984 [Internet]. 2000 [cited 2023 Jun 7];26(11):1131–40. Available from: https://www.tandfonline.com/doi/abs/10.1081/DDC-100100984
Rakesh R, Anoop KR. Formulation and optimization of nano-sized ethosomes for enhanced transdermal delivery of cromolyn sodium. J Pharm Bioallied Sci. 2012;4(4).
Acknowledgements
Then authors would like to acknowledge Ms. Oluwatosin Tabitha Leshaodo, Mariam Al Shawi, and Rebecca Lessaint for their contribution in preparation of dermatomed skin samples and assisting with skin resistance measurements for the study.
Funding
This study was funded by the East Tennessee State University Research and Development Major Grant series.
Author information
Authors and Affiliations
Contributions
OEA: acquisition, analysis, and interpretation of data, original draft preparation, and writing—review and editing; GV: acquisition, analysis, and interpretation of data, original draft preparation, and writing—review and editing; AAD: original draft preparation and writing—review and editing; AT: original draft preparation and writing—review and editing; AP: supervision, acquisition, analysis of data, and manuscript revision; SD: conception and design of work.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Communicated by Nisarg Modi, Yousuf Mohammed, and Lakshmi Raghavan.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Akinbote, O.E., Verana, G., Dandekar, A.A. et al. Effects of Sodium Salts of Fatty Acids and Their Derivatives on Skin Permeation of Cromolyn Sodium. AAPS PharmSciTech 24, 221 (2023). https://doi.org/10.1208/s12249-023-02676-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-023-02676-8