Abstract
Palatability and swallowability in the pediatric population are perceived as true challenges in the oral administration of medication. Pediatric patients have high sensitivity to taste and reduced ability to take solid dosage forms, which can often lead to a poor therapeutic compliance. It is crucial to find new strategies to simplify the oral administration of drugs to children. The present paper reports the development of a new hydrogel vehicle adapted to the pediatric population. Several polymers with similar properties were selected and adjustments were made to obtain the desired characteristics of the final product. The developed formulations were studied for organoleptic properties, rheology, mucoadhesion properties, preservative efficacy, and stability. Physical and chemical compatibilities between the vehicle and several drugs/medicines, at the time of administration, were also studied. Six final formulations with different polymers, odor, and color were chosen, and no known interactions with medications were observed. The proposed new oral vehicles are the first sugar-free vehicle hydrogels designed to make the intake of oral solid forms a more pleasant and safer experience for pediatric patients.
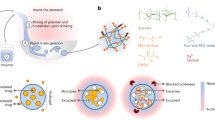
Graphical abstract






Similar content being viewed by others
References
Martir J, Flanagan T, Mann J, Fotaki N. Recommended strategies for the oral administration of paediatric medicines with food and drinks in the context of their biopharmaceutical properties: a review. J Pharm Pharmacol. 2017;69(4):384–97.
Ivanovska AV, Carin MA. Pediatric drug formulations : a review of challenges and progress. 2014;134(2):361–72.
Guidance D. Use of liquids and/or soft foods as vehicles for drug administration: general considerations for selection and in vitro methods for product quality assessments. (July 2018).
Mitra B, Thool P, Meruva S, Aycinena JA, Li J, Patel J, et al. Decoding the small size challenges of mini-tablets for enhanced dose flexibility and micro-dosing. Int J Pharm [Internet]. 2020;574:118905. Available from: https://doi.org/10.1016/j.ijpharm.2019.118905
Gupta S, Thool P, Meruva S, Li J, Patel J, Agrawal A, et al. Development of low dose micro-tablets by high shear wet granulation process. Int J Pharm [Internet]. 2020;587(July):119571. Available from: https://doi.org/10.1016/j.ijpharm.2020.119571
Lopez FL, Ernest TB, Tuleu C, Gul MO. Formulation approaches to pediatric oral drug delivery: benefits and limitations of current platforms. Expert Opin Drug Deliv. 2015;12(11):1727–40.
Liu F, Ranmal S, Batchelor HK, Orlu-Gul M, Ernest TB, Thomas IW, et al. Formulation factors affecting acceptability of oral medicines in children. Int J Pharm. 2015;492(1–2):341–3.
Squires LA, Lombardi DP, Sjostedt P, Thompson CA. A systematic literature review on the assessment of palatability and swallowability in the development of oral dosage forms for pediatric patients. Ther Innov Regul Sci. 2013;47(5):533–41.
Batchelor H, Kaukonen AM, Klein S, Davit B, Ju R, Ternik R, et al. Food effects in paediatric medicines development for products co-administered with food. Int J Pharm. 2018;536(2):530–5.
Kossoff EH, Zupec-Kania BA, Rho JM. Ketogenic diets: an update for child neurologists. J Child Neurol. 2009;24(8):979–88.
Pharmaceutical Inspection Convention - Pharmaceutical Inspection Co-operation Scheme. PIC/S Guide to good practices for the preparation of medicinal products in healthcare establishments. 2014;(March):1–56. Available from: http://www.picscheme.org/publication.php. Accessed 14 July 2014.
Silva F, Marto J, Salgado A, Machado P, Silva A, Almeida A. Nystatin and lidocaine pastilles for the local treatment of oral mucositis. Pharm Dev Technol. 2016;8:1–32.
Sriamornsak P, Wattanakorn N. Rheological synergy in aqueous mixtures of pectin and mucin. Carbohydr Polym. 2008;74(3):474–81.
Pharmacopoeia E, Pharmacopoeia E. 5.1.3. Efficacy of antimicrobial preservation. :505–6.
Niazi SK. Stability testing of new drug substances and products. Handb Pharm Manuf Formul. 2001;2020:31–40.
Marques-marinho FD, Vianna-soares CD. Cellulose and its derivatives use in the pharmaceutical compounding practice. In: Cellulose - Medical, Pharmaceutical and Electronic Applications. 2013. p. 141–62.
Pharmacopoeia E, Pharmacopoeia E. 5.1.4 Microbiological quality of non-sterile pharmaceutical preparations and substances for pharmaceutical use. :501–4.
Alves L, Costa DS, Campos MI, Druzian JI, De Oliveira AM, Nazaré E, et al. Biosynthesis of xanthan gum from fermenting shrimp shell: yield and apparent viscosity. Int J Polym Sci. 2014;1–8.
Song K, Chang G, Kuk H-Y. Rheology of concentrated xanthan gum solutions: oscillatory shear flow behavior. Korea-Australia Rheol J. 2006;18(2):67–81.
Stephen AM, Phillips GO, Williams PA. Food polysaccharides and their applications: second edition. Food Polysaccharides and Their Applications: Second Edition. 2016. 1–733 p.
Measurement T. Using a rotational rheometer to assess adhesion and tackiness. 2015;1–6.
Kossoff EH, Zupec-Kania BA, Amark PE, Ballaban-Gil KR, Christina Bergqvist AG, Blackford R, et al. Optimal clinical management of children receiving the ketogenic diet: recommendations of the International Ketogenic Diet Study Group. Epilepsia. 2009;50(2):304–17.
Rowe RCR, Sheskey PJS, Cook W. Handbook pharmaceutical excipients,sixth edition. 2009. 1064 p.
Afifi NA. Pharmaceutical solutions for oral administration. Pharm Dos Form Des. 2016;1–41.
Committee T. Commentary on breast-feeding and infant formulas, including proposed standards for formulas. Nutr Rev. 1976;34(8):248–56.
Fernández Polo A, Cabañas Poy MJ, Clemente Bautista S, Oliveras Arenas M, Castillo Salinas F, Hidalgo AE. Osmolality of oral liquid dosage forms to be administered to newborns in a hospital. Farm Hosp órgano Of expresión científica la Soc Española Farm Hosp. 2007;31(5):311–4.
Lopes AR. Caracterização de soluções poliméricas para aplicação em revestimentos para a conservação de produtos alimentares. 2016;
Espert M, Salvador A, Sanz T. Rheological and microstructural behaviour of xanthan gum and xanthan gum-Tween 80 emulsions during in vitro digestion. Food Hydrocoll. 2019;95:454–61.
Petri DFS. Xanthan gum: A versatile biopolymer for biomedical and technological applications. J Appl Polym Sci. 2015;132(23).
Vega ED, Vásquez E, Diaz JRA, Masuelli MA. Influence of the Ionic Strength in the Intrinsic Viscosity of Xanthan Gum. An Experimental Review. J Polym Biopolym Phys Chem. 2015;3(1):12–8.
Hercules Incorporated 1999. Physical and Chemical Properties of AQUALON CMC.
Funding
This research was funded by FCT (Fundação para a Ciência e a Tecnologia) through iMed.ULisboa UID/DTP/04138/2020 and UIDB/04138/2020). Joana Marto is financed through FCT, I.P., under the Scientific Employment Stimulus—Institutional Call (CEECINST/00145/2018).
Author information
Authors and Affiliations
Contributions
M. P., F. C. S., and J. M. conceived and designed the research. M. P. wrote the manuscript. M. P.., F. C. S., S. S., H. M. R., A. J. A., and J. M. reviewed and edited the manuscript. All authors have read and approved the manuscript for publication.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pereira, M., Silva, F.C., Simões, S. et al. Innovative, Sugar-Free Oral Hydrogel as a Co-administrative Vehicle for Pediatrics: a Strategy to Enhance Patient Compliance. AAPS PharmSciTech 23, 107 (2022). https://doi.org/10.1208/s12249-022-02265-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-022-02265-1