Abstract
This project aims to prepare hydrogel microneedle patches (MNs) as a painless method to deliver carbamazepine transdermally. This can be used as a sustained release system that offers the advantages of lower gastrointestinal side effects and avoids the first-pass metabolism of the drug. MNs were composed of two medicated layers, a microneedle layer and a base layer. MNs were fabricated using polyvinyl alcohol with or without polyvinylpyrrolidone Kollidon 30 as a matrix polymer and in the presence of selected solubilizing agent (polyethylene glycol 400, Tween 80, or α-tocopherol polyethylene glycol). Freezing–thawing cycle was evaluated as one of the processing parameters that may affect the drug release. The MNs were evaluated for their weight variation, base thickness, and content uniformity. The physicochemical compatibility between carbamazepine and the polymers was estimated by Fourier transform infrared spectroscopy, differential scanning calorimetry, thermogravimetric analysis, and X-ray powder diffraction. Evaluation for the in vitro release studies and ex vivo permeation studies was performed. The prepared MNs were flexible, clear, and uniform in weight, base thickness, and drug content. Physicochemical characterizations showed that carbamazepine was amorphous in most of the MNs. In vitro release and ex vivo permeation studies of carbamazepine were significantly higher for MNs containing a combination of 1:1 w/w of PEG 400 and Tween 80 as solubilizing agents where the release was extended over 96 h, with the release of 85.2% and 59.6% permeation percentage compared to other MNs. A significant effect of the freezing–thawing cycle on the release profile of the drug was observed. The hydrogel MNs are shown to be stable under the studied storage conditions.
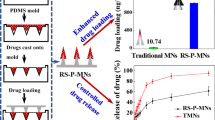
Graphical Abstract









Similar content being viewed by others
Abbreviations
- ASD:
-
Anti-seizure drug
- CBZ:
-
Carbamazepine
- DSC:
-
Differential scanning calorimetry
- FTIR:
-
Fourier transform infrared spectroscopy
- MNs:
-
Microneedles
- PEG:
-
400 Polyethylene glycol 400
- PVA:
-
Polyvinyl alcohol
- PVP K30:
-
Polyvinylpyrrolidone Kollidon 30
- SEM:
-
Scanning electron microscope
- TGA:
-
Thermogravimetric analysis
- α-TPGS:
-
α-Tocopherol polyethylene glycol of vitamin E
- XRPD:
-
X-ray powder diffraction
References
Kale SN, Kitture R, Ghosh S, Chopade BA, Yakhmi JV. Nanomaterials as enhanced antimicrobial agent/activity-enhancer for transdermal applications: a review, 2017. Antimicrobial Nanoarchitectonics, 279–321.
Abhinay C, Biplab KD. An overview on transdermal drug delivery. Indo American Journal of Pharmaceutical Research. 2016;6(07):6073–91.
Rastogi V, Yadav P. Transdermal drug delivery system: an overview. Asian Journal of Pharmaceutics. 2012;6:161–70.
Kanabar VB, Patel VP, Doshi SM. Formulation and evaluation of transdermal patch of Cefdinir with various polymers. The Pharma Innovation Journal. 2015;4(6):74–7.
Urquhart J; Chandrasekaran SK; Shaw JE. Method for administration scopolamine transdermally. 1983, US11/443, 6741.
Fischer W, Huber P. Transdermal systems for the delivery of clonidine. 2003, US 2004/0028726 A1.
Hwang SS, Gale RM. Once-A-Day replacement transdermal administration of fentanyl. 2008, US 2009/0258061 A1.
Chiang CC. Transdermal delivery of oxybutynin in gel formulations. 2004, US 2005/0064037 A1.
Ebert CD, Patel D, Heiber S. Method and systems for administering nitroglycern transdermally at enhanced transdermal fluxes. 1990, US 005202125 A.
Ciullo J. Lidocaine patch and methods of use. 2012, US 2013/ 0184351 A1.
Mantelle J. A. Transdermal testosterone device and delivery. 2010, US 009,320,742 B2.
Lúcia FS, Ilídio JC, Sofia S, João FM. Biomaterials for drug delivery patches. Eur J Pharm Sci. 2018;118:49–66.
Harneet M, Tarun G, Amit KG, Goutam R. Permeation enhancer strategies in transdermal drug delivery. 2014.
Santos LF, Correia IJ, Silva AS, Mano JF. Biomaterials for drug delivery patches. Eur J Pharm Sci. 2018;118:49–66.
Donnelly RF, Singh TRR, Garland MJ, Migalska K, Majithiya R, McCrudden CM, Kole PL, Mahmood TMT, McCarthy HO, Woolfson AD. Hydrogel-forming microneedle arrays for enhanced transdermal drug delivery. Journal of advance functional materials. 2012;22:1–12.
Lee IC, He JS, Tsai MT, Lin KC. Fabrication of a novel partial dissolving polymer microneedle patch for transdermal drug delivery. Journal of material chemistry B. 2013;2013:1–29.
Kearney MC, Salvador EC, Fallows SJ, McCarthy HO, Donnelly RF. Microneedle-mediated delivery of donepezil: potential for improved treatment options in alzheimer’s disease. Eur J Pharm Biopharm. 2016;43–50:103.
Migdadi EM, Courtenay AJ, Tekko IA, McCrudden MTC, Kearney MC, McAlister E, McCarthy HO, Donnelly RF. Hydrogel-forming microneedles enhance transdermal delivery of metformin hydrochloride. J Control Release. 2018;285:142–51.
Beydoun A, DuPont S, Zhou D, Matta M, Nagire V, Lagae L. Current role of carbamazepine and oxcarbazepine in the management of epilepsy. Seizure. 2020;83:251–63.
Spina E, Pisani F, Perucca E. Clinically significant pharmacokinetic drug interactions with carbamazepine. Clinical Pharmacokinetic. 1996;3:198–214.
Jongmans JWM. Report on the anti-epileptic action of Tegretol. Epilipsia. 1964;5:74–82.
Biom S. Trigeminal neuralgia: its treatment with a new anticonvulsant drug (G-32883). Lancet. 1962;1:839–40.
Alrashood ST. Carbamazepine. Profiles Drug Subst Excip Relat Methodol. 2016;41:133–321.
McIntyre RS, Berk M, Brietzke E, et al. Bipolar disorders. Lancet. 2020;396(10265):1841–56.
Kanner AM. Management of psychiatric and neurological comorbidities in epilepsy. Nat Rev Neurol. 2016;12(2):106–16.
Castro APBM, Redmershi MG, Pastorino AC, Paz JA, Fomin ABF, Jacob CMA. Secondary hypogammaglobilinemia after use of Carbamazepine: case report and review. Revista do Hospital das Clínicas. 2001;56(6):189–92.
Omoúlu T, Nurßin GNL. Quality control studies on conventional Carbamazepine tablets available on the Turkish drug market. Turk J Med Sci. 2005;35:217–21.
Cruccu G, Di Stefano G, Truini A. Trigeminal Neuralgia. N Engl J Med. 2020;383(8):754–62.
Isadiartuti D, Budiati T, Martodihardjo S. Solubility and dissolution study of physical mixture of carbamazepine and amino acids. Int J Pharm Pharm Sci. 2013;6(1):301–6.
Rinaki E, Valsami G, Macheras P. Quantitative biopharmaceutics classification system the central role of dose/solubility ratio. Pharm Res. 2003;20:1917–25.
Drugbank.ca. (2020). Carbamazepine-DrugBank. [online] Available at: https://www.drugbank.ca/drugs/DB00564 [Accessed 3 Jan. 2020].
Yang S, Feng Y, Zhang L, Chen N, Yuan W, Jin T. A scalable fabrication process of polymer Microneedles. Int J Nanomed. 2012;7:1415–22.
Tejwani RW, Joshi H, Varia SA, Serajuddin A. Study of phase behavior of poly (ethylene glycol)-polysorbate 80 and poly(ethylene glycol) –polysorbate 80- water mixtures. J Pharm Sci. 2000;89(7):946–50.
Amodwala S, Kumar P, Thakkar HP. Statistically optimized fast dissolving microneedle transdermal patch of meloxicam: a patient friendly approach to manage arthritis. Journal of Europe of pharmaceutical science. 2017;15(104):114–23.
Luthala S. Effect of sodium lauryl sulfate and polysorbate 80 on crystal growth and aqueous solubility of carbamazepine. Acta Pharm Nord. 1992;4(2):85–90.
Hyeongmin K, Sukkyun J, Sooho Y, Dohyun K, Young CN, Gyiae Y, Jaehwi L. Characteristics of skin deposition of itraconazole solubilized in cream formulation. Pharmaceutics. 2019;11:195.
Valentine CA, Ibbotson GATN, Akroyd DT, Kendrick JS, V. Sunesen H. Comparison of procedures used to separate the different layers of human skin biopsy samples. Covance Laboratories Ltd, 2016.
Czernicki W, Baranska M. Carbamazepine polymorphs: theoretical and experimental vibrational spectroscopy studies. Vib Spectrosc. 2012;65:12–23.
Pinto MAL., Ambrozini B, Ferreira APG, and Cavalheiro ΈTG. Thermoanalytical studies of carbamazepine: hydration/ dehydration, thermal decomposition, and solid phase transitions. Brazilian Journal of Pharmaceutical sciences, 2014, 50 (4), 877–884.
Sethia S, Squillante E. Solid dispersion of carbamazepine in PVP K30 by conventional solvent evaporation and supercritical methods. Int J Pharm. 2004;272:1–10.
Nair R, Kumar ACK, Priya VK, Yadav CM, Raju PY. Formulation and evaluation of chitosan solid lipid nanoparticles of carbamazepine. Lipids Health Dis. 2012;11:72.
Elqidra R, Ünlü N, Çapan Y, Sahin G, Dalkara T, Hincal AA. Effect of polymorphism on in vitro-in vivo properties of carbamazepine conventional tablets. Journal of drug delivery and science technology. 2004;14(2):147–53.
Douroumis D, Bouropoulos N, Fahr A. Physiochemical characterization of solid dispersions of three antiepileptic drugs prepared by solvent evaporation method. Journal of Pharmacy and Pharmacology (JPP). 2007;59:645–53.
Ma X, Müller F, Huang S, Lowinger M, Liu X, Schooler R, Williams RO III. Influence of carbamazepine dihydrate on the preparation of amorphous solid dispersion by hot melt extrusion. Pharmaceutics. 2020;12:379.
Som I, Bhatia K, Yasir M. Status of surfactants as penetration enhancers in transdermal drug delivery. Journal of pharmacy and Bioallied sciences. 2012;4(1):2–10.
Rodrigues LNC, Zanluchi JM, Grebogi IH. Percutaneous absorption enhancers: mechanisms and potential. Braz Arch Biol Technol. 2007;50(6):949–61.
Lane ME. Skin Penetration enhancers. Int J Pharm. 2013;447:12–21.
Shlichta PJ, Knox RE. Growth of crystals by centrifugation. J Cryst Growth. 1968;3(4):808–13.
Chaudhari S, Dugar R. Application of surfactants in solid dispersion technology for improving solubility of poorly water-soluble drugs. Journal of drug delivery science and technology. 2017;41:68–77.
Gouda R, Baishya H, Qing Z. Application of mathematical models in drug release kinetics of carbidopa and levodopa ER tablets. Journal of development drugs. 2017;6(2):1–8.
Nair R, Gonen S, Hoag SW. Influence of polyethylene glycol and povidone on the polymorphic transformation and solubility of carbamazepine. Int J Pharm. 2002;240:11–22.
Tang C, Saquing CD, Harding JR, Khan SA. In situ cross-linking of electrospun poly(vinyl alcohol) nanofibers. Macromolecules. 2010;43:630–7.
Marsac PJ, Rumondor ACF, Nivens DE, Kestur US, Stanciu L, Taylor LS. Effect of temperature and moisture on the miscibility of amorphous dispersions of felodipine and poly (vinyl pyrrolidone). J Pharm Sci. 2010;99(1):169–85.
Cao Y, Tao Y, Zhou Y, Gui S. Development of sinomenine hydrochloride loaded polyvinylalcohol/maltose microneedle for transdermal delivery. Journal of Drug Delivery Science and Technology. 2016;35:1–7.
Funding
For Deanship of Research at Jordan University of Science and Technology for funding this project with Fund number 517/2020.
Author information
Authors and Affiliations
Contributions
Rana Obaidat: contributed to the conception, design, and interpretation. Fatima BaniAmer: performed the research in the lab, data analysis, and writing it as part of her master’s degree thesis. Shereen Assaf: contributed to design, characterization of the patches, and writing. Ahmed Yassin: contributed to the conception, design, and writing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Obaidat, R., BaniAmer, F., Assaf, S.M. et al. Fabrication and Evaluation of Transdermal Delivery of Carbamazepine Dissolving Microneedles. AAPS PharmSciTech 22, 253 (2021). https://doi.org/10.1208/s12249-021-02136-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-021-02136-1