Abstract
Advances in drug delivery have been accelerated with the addition of polymeric drug carriers. Direct delivery to a target site is a promising step in developing effective drug and gene therapies to treat disease. The efficacy of these drug carriers heavily relies on cell uptake without compromising critical cellular processes that promote cell viability. Drug release from biodegradable polymers is mediated largely by polymer degradation, and therefore the rate of polymer degradation dictates the feasibility of drug delivery applications. Traditionally, poly(caprolactone) (PCL) has only been used in long-term biomedical applications because the degradation time is much slower than other polymers. However, the biocompatibility of this polymer and the potential for longer delivery windows renders it a promising polymer candidate for drug delivery. In this work, we outline sixteen emulsion solvent evaporation preparation methods for PCL nanoparticles and microparticles to develop particles between 300 nm and 1.7 μm and with zeta potentials of -1.8 mV. We further investigated particles in a size range suitable for systemic tumor delivery and inhaled aerosol delivery to determine cell biocompatibility with the polymer in lung adenocarcinoma, endometrial adenocarcinoma, and human embryonic kidney cells. We determined these particles aren’t detrimental to cell viability below particle monolayer coverage atop cells and therefore these formulations hold promise for the next stage of development as sustained-release drug delivery carriers.
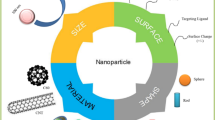
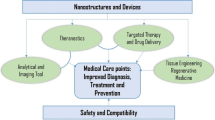
Graphical Abstract







Similar content being viewed by others
Data Availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Rathna GVN, Bhagyashri S, Gadgil T, Killi N. Polyhydroxyalkanoates: The Application of Eco-Friendly Materials. Polymers as Drug Delivery Systems. New Jersey: John Wiley & Sons; 2016. p. 2-33.
Jahangirian H, Lemraski EG, Webster TJ, Rafiee-Moghaddam R, Abdollahi Y. A review of drug delivery systems based on nanotechnology and green chemistry: green nanomedicine. Int J Nanomedicine. 2017;12:2957–78. https://doi.org/10.2147/IJN.S127683.
Xu Y, Liu H, Song L. Novel drug delivery systems targeting oxidative stress in chronic obstructive pulmonary disease: a review. J Nanobiotechnology. 2020;18(1):145. https://doi.org/10.1186/s12951-020-00703-5.
Ulucan-Karnak F, Kuru Cİ. Chapter 13 - Advantages of nanodrug targeting than conventional dosage system. In: Pratap Singh R, Rb Singh K, Singh J, Adetunji CO, editors. Nanotechnology for Drug Delivery and Pharmaceuticals. Academic Press; 2023. p. 295–310.
Chang SH, Lee HJ, Park S, Kim Y, Jeong B. Fast Degradable Polycaprolactone for Drug Delivery. Biomacromol. 2018;19(6):2302–7. https://doi.org/10.1021/acs.biomac.8b00266.
Li L, Gatto GJ, Brand RM, Krovi SA, Cottrell ML, Norton C, et al. Long-acting biodegradable implant for sustained delivery of antiretrovirals (ARVs) and hormones. J Control Release. 2021;340:188–99. https://doi.org/10.1016/j.jconrel.2021.10.021.
Acosta MF, Abrahamson MD, Encinas-Basurto D, Fineman JR, Black SM, Mansour HM. Inhalable Nanoparticles/Microparticles of an AMPK and Nrf2 Activator for Targeted Pulmonary Drug Delivery as Dry Powder Inhalers. AAPS J. 2020;23(1):2. https://doi.org/10.1208/s12248-020-00531-3.
Wiwatchaitawee K, Mekkawy AI, Quarterman JC, Naguib YW, Ebeid K, Geary SM, et al. The MEK 1/2 inhibitor PD98059 exhibits synergistic anti-endometrial cancer activity with paclitaxel in vitro and enhanced tissue distribution in vivo when formulated into PAMAM-coated PLGA-PEG nanoparticles. Drug Deliv Transl Res. 2022;12(7):1684–96. https://doi.org/10.1007/s13346-021-01065-7.
Naguib YW, Givens BE, Ho G, Yu Y, Wei SG, Weiss RM, et al. An injectable microparticle formulation for the sustained release of the specific MEK inhibitor PD98059: in vitro evaluation and pharmacokinetics. Drug Deliv Transl Res. 2021;11(1):182–91. https://doi.org/10.1007/s13346-020-00758-9.
Terry TL, Givens BE, Rodgers VGJ, Salem AK. Tunable Properties of Poly-DL-Lactide-Monomethoxypolyethylene Glycol Porous Microparticles for Sustained Release of Polyethylenimine-DNA Polyplexes. AAPS PharmSciTech. 2019;20(1):23. https://doi.org/10.1208/s12249-018-1215-9.
El-Sherbiny IM, El-Baz NM, Yacoub MH. Inhaled nano- and microparticles for drug delivery. Glob Cardiol Sci Pract. 2015;2015:2. https://doi.org/10.5339/gcsp.2015.2.
Patra JK, Das G, Fraceto LF, Campos EVR, Rodriguez-Torres MDP, Acosta-Torres LS, et al. Nano based drug delivery systems: recent developments and future prospects. J Nanobiotechnology. 2018;16(1):71. https://doi.org/10.1186/s12951-018-0392-8.
Ferrari R, Sponchioni M, Morbidelli M, Moscatelli D. Polymer nanoparticles for the intravenous delivery of anticancer drugs: the checkpoints on the road from the synthesis to clinical translation. Nanoscale. 2018;10(48):22701–19. https://doi.org/10.1039/c8nr05933k.
Choi CH, Zuckerman JE, Webster P, Davis ME. Targeting kidney mesangium by nanoparticles of defined size. Proc Natl Acad Sci U S A. 2011;108(16):6656–61. https://doi.org/10.1073/pnas.1103573108.
Kalyane D, Raval N, Maheshwari R, Tambe V, Kalia K, Tekade RK. Employment of enhanced permeability and retention effect (EPR): Nanoparticle-based precision tools for targeting of therapeutic and diagnostic agent in cancer. Mater Sci Eng C Mater Biol Appl. 2019;98:1252–76. https://doi.org/10.1016/j.msec.2019.01.066.
Maeda H, Wu J, Sawa T, Matsumura Y, Hori K. Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J Control Release. 2000;65(1–2):271–84. https://doi.org/10.1016/s0168-3659(99)00248-5.
Soppimath KS, Aminabhavi TM, Kulkarni AR, Rudzinski WE. Biodegradable polymeric nanoparticles as drug delivery devices. J Control Release. 2001;70(1–2):1–20. https://doi.org/10.1016/s0168-3659(00)00339-4.
Owens DE 3rd, Peppas NA. Opsonization, biodistribution, and pharmacokinetics of polymeric nanoparticles. Int J Pharm. 2006;307(1):93–102. https://doi.org/10.1016/j.ijpharm.2005.10.010.
Terry TL, Givens BE, Adamcakova-Dodd A, Thorne PS, Rodgers VGJ, Salem AK. Encapsulating Polyethyleneimine-DNA Nanoplexes into PEGylated Biodegradable Microparticles Increases Transgene Expression In Vitro and Reduces Inflammatory Responses In Vivo. AAPS PharmSciTech. 2021;22(2):69. https://doi.org/10.1208/s12249-021-01932-z.
Manoukian OS, Arul MR, Sardashti N, Stedman T, James R, Rudraiah S, et al. Biodegradable polymeric injectable implants for long-term delivery of contraceptive drugs. J Appl Polym Sci. 2018;135(14). https://doi.org/10.1002/app.46068.
Chandra R, Rustgi R. Biodegradable polymers. Prog Polym Sci. 1998;23(7):1273–335.
Okada M. Chemical syntheses of biodegradable polymers. Prog Polym Sci. 2002;27(1):87–133. https://doi.org/10.1016/s0079-6700(01)00039-9.
Woodring RN, Gurysh EG, Bachelder EM, Ainslie KM. Drug Delivery Systems for Localized Cancer Combination Therapy. ACS Appl Bio Mater. 2023;6(3):934–50. https://doi.org/10.1021/acsabm.2c00973.
Woodruff MA, Hutmacher DW. The return of a forgotten polymer—Polycaprolactone in the 21st century. Prog Polym Sci. 2010;35(10):1217–56. https://doi.org/10.1016/j.progpolymsci.2010.04.002.
Sun H, Mei L, Song C, Cui X, Wang P. The in vivo degradation, absorption and excretion of PCL-based implant. Biomaterials. 2006;27(9):1735–40. https://doi.org/10.1016/j.biomaterials.2005.09.019.
Abramoff MD, Magalhaes PJ, Ram SJ. Image processing with ImageJ. Biophotonics Int. 2004;11(7):36–42.
Schindelin J, Arganda-Carreras I, Frise E, Kaynig V, Longair M, Pietzsch T, et al. Fiji: an open-source platform for biological-image analysis. Nat Methods. 2012;9(7):676–82. https://doi.org/10.1038/nmeth.2019.
Prasad A, Kandasubramanian B. Fused deposition processing polycaprolactone of composites for biomedical applications. Polym-Plast Technol Mater. 2019;58(13):1365–98. https://doi.org/10.1080/25740881.2018.1563117.
Mason TG, Wilking JN, Meleson K, Chang CB, Graves SM. Nanoemulsions: formation, structure, and physical properties. J Phys: Condens Matter. 2006;18(41):R635–66. https://doi.org/10.1088/0953-8984/18/41/r01.
Witt S, Scheper T, Walter JG. Production of polycaprolactone nanoparticles with hydrodynamic diameters below 100 nm. Eng Life Sci. 2019;19(10):658–65. https://doi.org/10.1002/elsc.201800214.
Jiang D, Salem AK. Optimized dextran-polyethylenimine conjugates are efficient non-viral vectors with reduced cytotoxicity when used in serum containing environments. Int J Pharm. 2012;427(1):71–9. https://doi.org/10.1016/j.ijpharm.2011.10.032.
Stark WJ. Nanoparticles in biological systems. Angew Chem Int Ed Engl. 2011;50(6):1242–58. https://doi.org/10.1002/anie.200906684.
Huang K, Hu Y, Yu C, Boerhan R, Jiang G. Charged surface groups of nanoparticles and the adsorbed proteins codetermine the fate of nanoparticles upon interacting with cells. RSC Adv. 2016;6(63):58315–24. https://doi.org/10.1039/c6ra07468e.
Oh N, Park JH. Endocytosis and exocytosis of nanoparticles in mammalian cells. Int J Nanomed. 2014;9(Suppl 1):51–63. https://doi.org/10.2147/IJN.S26592.
Foroozandeh P, Aziz AA. Insight into Cellular Uptake and Intracellular Trafficking of Nanoparticles. Nanoscale Res Lett. 2018;13(1):339. https://doi.org/10.1186/s11671-018-2728-6.
Lukasiewicz S, Mikolajczyk A, Blasiak E, Fic E, Dziedzicka-Wasylewska M. Polycaprolactone nanoparticles as promising candidates for nanocarriers in novel nanomedicines. Pharmaceutics 2021;13(2). https://doi.org/10.3390/pharmaceutics13020191.
Bruinsmann FA, Buss JH, Souto GD, Schultze E, de Cristo SoaresAlves A, Seixas FK, et al. Erlotinib-Loaded Poly(epsilon-Caprolactone) Nanocapsules Improve In Vitro Cytotoxicity and Anticlonogenic Effects on Human A549 Lung Cancer Cells. AAPS PharmSciTech. 2020;21(6):229. https://doi.org/10.1208/s12249-020-01723-y.
Yu W, Liu R, Zhou Y, Gao H. Size-Tunable Strategies for a Tumor Targeted Drug Delivery System. ACS Cent Sci. 2020;6(2):100–16. https://doi.org/10.1021/acscentsci.9b01139.
Zhang Q, Bao J, Duan T, Hu M, He Y, Wang J, et al. Nanomicelle-microsphere composite as a drug carrier to improve lung-targeting specificity for lung cancer. Pharmaceutics 2022;14(3). https://doi.org/10.3390/pharmaceutics14030510.
Acknowledgements
The authors acknowledge the Electron Microscopy Center at the University of Kentucky for SEM images, with particular support from Nicholas Briot, PhD.
Funding
This work was supported by the University of Kentucky Clinical and Translational Sciences funded by the NIH National Center for Advancing Translational Sciences through grant number UL1TR001998. This content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Contributions
A.S. and C.R. contributed equally to concept, experimental design, experimental methods, data analysis, manuscript preparation and editing. H.S. conducted experiments and data analysis. B.G. was responsible for conceptualization, manuscript preparation and editing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest in this work.
Additional information
Communicated by Aliasger Salem.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ashbey Manning and Claire Rowlands are co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Manning, A.N., Rowlands, C.E., Saindon, H. et al. Tuning the Emulsion Properties Influences the Size of Poly(Caprolactone) Particles for Drug Delivery Applications. AAPS J 25, 100 (2023). https://doi.org/10.1208/s12248-023-00869-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-023-00869-4