Abstract
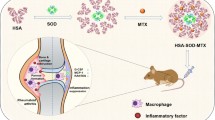
Celastrol (CLT) has shown anti-rheumatic activity against rheumatoid arthritis, while its poor water solubility and high organ toxicity restrict its further therapeutic applications. To mitigate these challenges, a reactive oxygen species (ROS)–responsive nanoparticle was developed for celastrol delivery based on the excessive ROS at the pathologic sites, which was synthesized by conjugating bilirubin to a polyethylene glycol (PEG) chain. The PEGylated bilirubin self-assembled into nanoparticle (BRNP) in aqueous solution had a hydrodynamic diameter of around 68.6 nm, and celastrol was loaded into BRNP (CLT/BRNP) with a drug encapsulation efficiency of 72.6% and a loading capacity of 6.6%. In vitro study revealed that CLT/BRNP exhibited the capacity of scavenging intracellular ROS and down-regulating the level of nitric oxide after it was effectively internalized by activated macrophages. Furthermore, in adjuvant-induced arthritis rats, BRNP was accumulated preferentially at inflamed joints, alleviating the joint swelling and bone erosion, which significantly decreased the secretion of pro-inflammatory cytokines to suppress the RA progression. Importantly, CLT/BRNP markedly enhanced its anti-arthritic effect and attenuated the toxic effect compared with free celastrol. Taken together, our results suggested that CLT/BRNP could be used for targeted drug delivery in rheumatoid arthritis.
Graphical abstract







Similar content being viewed by others
Change history
02 February 2022
A Correction to this paper has been published: https://doi.org/10.1208/s12248-022-00680-7
References
McInnes IB, Schett G. The pathogenesis of rheumatoid arthritis[J]. N Engl J Med. 2011;365(23):2205–19. https://doi.org/10.1056/NEJMra1004965.
Chen Z, Bozec A, Ramming A, et al. Anti-inflammatory and immune-regulatory cytokines in rheumatoid arthritis[J]. Nat Rev Rheumatol. 2019;15(1):9–17. https://doi.org/10.1038/s41584-018-0109-2.
Combe B, van Vollenhoven R. Novel targeted therapies: the future of rheumatoid arthritis? Mavrilumab and tabalumab as examples[J]. 2013. https://doi.org/10.1136/annrheumdis-2013-203261.
Ćalasan MB, van den Bosch OFC, Creemers MCW, et al. Prevalence of methotrexate intolerance in rheumatoid arthritis and psoriatic arthritis[J]. Arthritis Res Ther. 2013;15(6):1–5. https://doi.org/10.1186/ar4413.
Fan X, Xu M, Leung ELH, et al. ROS-responsive berberine polymeric micelles effectively suppressed the inflammation of rheumatoid arthritis by targeting mitochondria[J]. Nano-Micro Letters. 2020;12(1):1–14. https://doi.org/10.1007/s40820-020-0410-x.
Cascao R, Vidal B, Raquel H, et al. Effective treatment of rat adjuvant-induced arthritis by celastrol[J]. Autoimmun Rev. 2012;11(12):856–62. https://doi.org/10.1016/j.autrev.2012.02.022.
Xu Z, Wu G, Wei X, et al. Celastrol induced DNA damage, cell cycle arrest, and apoptosis in human rheumatoid fibroblast-like synovial cells[J]. Am J Chin Med. 2013;41(03):615–28. https://doi.org/10.1016/10.1142/S0192415X13500432.
Astry B, Venkatesha SH, Laurence A, et al. Celastrol, a Chinese herbal compound, controls autoimmune inflammation by altering the balance of pathogenic and regulatory T cells in the target organ[J]. Clin Immunol. 2015;157(2):228–38. https://doi.org/10.1016/j.clim.2015.01.011.
Gan K, Xu L, Feng X, et al. Celastrol attenuates bone erosion in collagen-Induced arthritis mice and inhibits osteoclast differentiation and function in RANKL-induced RAW264.7[J]. Int Immunopharmacol. 2015;24(2):239–46. https://doi.org/10.1016/j.intimp.2014.12.012.
Achek A, Shah M, Seo JY, Kwon HK, Gui X, Shin HJ, Cho EY, Lee BS, Kim DJ, Lee SH, Yoo TH, Kim MS, Choi S. Linear and rationally designed stapled peptides abrogate TLR4 pathway and relieve inflammatory symptoms in rheumatoid arthritis rat model. J Med Chem. 2019;62:6495–511. https://doi.org/10.1021/acs.jmedchem.9b00061.
Wong VKW, Qiu C, Xu SW, et al. Ca2+ signalling plays a role in celastrol-mediated suppression of synovial fibroblasts of rheumatoid arthritis patients and experimental arthritis in rats[J]. Br J Pharmacol. 2019;176(16):2922–44. https://doi.org/10.1111/bph.14718.
Gao Q, Qin H, Zhu L, et al. Celastrol attenuates collagen-induced arthritis via inhibiting oxidative stress in rats[J]. Int Immunopharmacol. 2020;84:106527. https://doi.org/10.1016/j.intimp.2020.106527.
Winyard PG, Ryan B, Eggleton P, et al. Measurement and meaning of markers of reactive species of oxygen, nitrogen and sulfur in healthy human subjects and patients with inflammatory joint disease[J]. Biochem Soc Trans. 2011;39(5):1226–32. https://doi.org/10.1042/BST0391226.
Phull AR, Nasir B, ulHaq I, et al. Oxidative stress, consequences and ROS mediated cellular signaling in rheumatoid arthritis[J]. Chem-Biol Interact. 2018;281:121–36. https://doi.org/10.1016/j.cbi.2017.12.024.
Khojah HM, Ahmed S, Abdel-Rahman MS, et al. Reactive oxygen and nitrogen species in patients with rheumatoid arthritis as potential biomarkers for disease activity and the role of antioxidants[J]. Free Radical Biol Med. 2016;97:285–91. https://doi.org/10.1016/j.freeradbiomed.2016.06.020.
Mateen S, Moin S, Shahzad S, et al. Level of inflammatory cytokines in rheumatoid arthritis patients: correlation with 25-hydroxy vitamin D and reactive oxygen species[J]. PLoS ONE. 2017;12(6):e0178879. https://doi.org/10.1371/journal.pone.0178879.
Smallwood MJ, Nissim A, Knight AR, et al. Oxidative stress in autoimmune rheumatic diseases[J]. Free Radical Biology and Medicine. 2018;125:3–14. https://doi.org/10.1016/j.freeradbiomed.2018.05.086.
Kim J, Kim HY, Song SY, et al. Synergistic oxygen generation and reactive oxygen species scavenging by manganese ferrite/ceria co-decorated nanoparticles for rheumatoid arthritis treatment[J]. ACS Nano. 2019;13(3):3206–17. https://doi.org/10.1021/acsnano.8b08785.
Yang Y, Guo L, Wang Z, et al. Targeted silver nanoparticles for rheumatoid arthritis therapy via macrophage apoptosis and re-polarization[J]. Biomaterials. 2021;264:120390. https://doi.org/10.1016/j.biomaterials.2020.120390.
Ni R, Song G, Fu X, et al. Reactive oxygen species-responsive dexamethasone-loaded nanoparticles for targeted treatment of rheumatoid arthritis via suppressing the iRhom2/TNF-α/BAFF signaling pathway[J]. Biomaterials. 2020;232:119730. https://doi.org/10.1016/j.biomaterials.2019.119730.
Li J, Chen L, Xu X, et al. Targeted combination of antioxidative and anti-inflammatory therapy of rheumatoid arthritis using multifunctional dendrimer-entrapped gold nanoparticles as a platform[J]. Small. 2020;16(49):2005661. https://doi.org/10.1002/smll.202005661.
Long Y, Lu Z, Mei L, et al. Enhanced melanoma-targeted therapy by “Fru-Blocked” phenyboronic acid-odified multiphase antimetastatic micellar nanoparticles[J]. Advanced Science. 2018;5(11):1800229. https://doi.org/10.1002/advs.201800229.
Liu Y, Shi J. Antioxidative nanomaterials and biomedical applications[J]. Nano Today. 2019;27:146–77. https://doi.org/10.1016/j.nantod.2019.05.008.
Stocker R, Yamamoto Y, McDonagh AF, et al. Bilirubin is an antioxidant of possible physiological importance[J]. Science. 1987;235(4792):1043–6. https://doi.org/10.1126/science.3029864.
Peng F, Deng X, Yang Y, et al. Serum bilirubin concentrations and multiple sclerosis[J]. J Clin Neurosci. 2011;18(10):1355–9. https://doi.org/10.1016/j.jocn.2011.02.023.
Horsfall LJ, Hardy R, Wong A, Kuh D, Swallow DM. Genetic variation underlying common hereditary hyperbilirubinaemia (Gilbert’s syndrome) and respiratory health in the 1946 British birth cohort. J Hepatol. 2014;61(6):1344e1351.
de Vries HS, teMorsche RHM, Jenniskens K, Peters WHM, de Jong DJ. A functional polymorphism in UGT1A1 related to hyperbilirubinemia is associated with a decreased risk for Crohn’s disease. J Crohns Colitis. 2012;6(5):597e602.
Keshavan P, Deem TL, Schwemberger SJ, Babcock GF, Cook-Mills JM, Zucker SD. Unconjugated bilirubin inhibits VCAM-1-mediated transendothelial leukocyte migration. J Immunol. 2005;174(6):3709e3718.
Wang Q, Jiang J, Chen W, et al. Targeted delivery of low-dose dexamethasone using PCL–PEG micelles for effective treatment of rheumatoid arthritis[J]. J Control Release. 2016;230:64–72. https://doi.org/10.1016/j.jconrel.2016.03.035.
Yang Y, Guo L, Wang Z, et al. Targeted silver nanoparticles for rheumatoid arthritis therapy via macrophage apoptosis and Re-polarization[J]. Biomaterials, 2021;264:120390. https://doi.org/10.1016/j.biomaterials.2020.120390.
Yeo J, Lee Y M, Lee J, et al. Nitric oxide-scavenging nanogel for treating rheumatoid arthritis[J]. Nano Lett. 2019;19(10):6716–24. https://doi.org/10.1021/acs.nanolett.9b00496.
Leech M, Metz C, Bucala R, et al. Regulation of macrophage migration inhibitory factor by endogenous glucocorticoids in rat adjuvant‐induced arthritis[J]. Arthritis & Rheumatism: Official Journal of the American College of Rheumatology. 2000;43(4):827–33. https://doi.org/10.1002/15290131(200004)43:4<827::AIDANR13>3.0.CO;2-K.
Deakin AM, Payne AN, Whittle BJ, Moncada S. The modulation of IL-6 and TNF-α release by nitric oxide following stimulation of J774 cells with LPS and IFN-γ. Cytokine. 1995;7(5):408–16. https://doi.org/10.1006/cyto.1995.0056.
Makris AC, Sotzios Y, Zhou Z, Makropoulou M, Papapetropoulos N, Zacharatos P, Pyriochou A, Roussos C, Papapetropoulos A, Vassilakopoulos T. Nitric oxide stimulates interleukin-6 production in skeletal myotubes. J Interferon Cytokine Res. 2010;30(5):321–7. https://doi.org/10.1089/jir.2009.0022.
Choi Y, Arron JR, Townsend MJ. Promising bone-related therapeutic targets for rheumatoid arthritis[J]. Nat Rev Rheumatol. 2009;5(10):543–8. https://doi.org/10.1038/nrrheum.2009.175.
Zhang Q, Dehaini D, Zhang Y, et al. Neutrophil membrane-coated nanoparticles inhibit synovial inflammation and alleviate joint damage in inflammatory arthritis[J]. Nat Nanotechnol. 2018;13(12):1182–90. https://doi.org/10.1038/s41565-018-0254-4.
Spagnolo P, Lee J S, Sverzellati N, et al. The lung in rheumatoid arthritis: focus on interstitial lung disease[J]. Arthritis Rheumatol. 2018;70(10):1544–54. https://doi.org/10.1002/art.40574.
Turesson C, O’fallon WM, Crowson CS, et al. Extra-articular disease manifestations in rheumatoid arthritis: incidence trends and risk factors over 46 years[J]. Ann Rheum Dis. 2003;62(8):722–7. https://doi.org/10.1136/ard.62.8.722.
Cortet B, Perez T, Roux N, et al. Pulmonary function tests and high resolution computed tomography of the lungs in patients with rheumatoid arthritis[J]. Ann Rheum Dis. 1997;56(10):596–600. https://doi.org/10.1136/ard.56.10.596.
Luo S, Li P, Li S, et al. N, N-dimethyl tertiary amino group mediated dual pancreas-and lung-targeting therapy against acute pancreatitis[J]. Mol Pharm. 2017;14(5):1771–81. https://doi.org/10.1021/acs.molpharmaceut.7b00028.
Cuong NV, Hsieh MF, Chen YT , et al. Synthesis and characterization of PEG-PCL-PEG triblock copolymers as carriers of doxorubicin for the treatment of breast cancer[J]. J Appl Polym Sci. 2010;117(6):3694–703. https://doi.org/10.1002/app.32266.
Cuong NV, Chen YT, Hsieh MF. Doxorubicin- loaded micelles of Y-shaped PEG-(PCL)2 against drug-resistant breast cancer cells[J]. Biomed Eng Appl Basis Commun. 2013;25(05):1340009. https://doi.org/10.4015/S1016237213400097.
Zhang J, Wang LQ , Wang H, et al. Micellization phenomena of amphiphilic block copolymers based on methoxy poly(ethylene glycol) and either crystalline or amorphous poly(caprolactone-b-lactide).[J]. Biomacromolecules. 2006:7(9):2492–500. https://doi.org/10.1021/bm0601732.
Xiaolan, Yang, Rongrong, et al. Design and synthesis of pH-sensitive polymeric micelles for oral delivery of poorly water-soluble drugs: Journal of Biomaterials Science, Polymer Edition: Vol 27, No 13[J]. J Biomater Sci Polym Ed. 2016. https://doi.org/10.1080/09205063.2016.1200248.
Li H, Niu Y. Synthesis and characterization of amphiphilic block polymer poly(ethylene glycol)-poly(propylene carbonate)-poly(ethylene glycol) for drug delivery[J]. Mater Sci Eng C. 2018;89(AUG.):160. https://doi.org/10.1016/j.msec.2018.04.002.
Sedlak TW, Saleh M, Higginson DS, et al. Bilirubin and glutathione have complementary antioxidant and cytoprotective roles[J]. Proc Natl Acad Sci. 2009;106(13):5171–6. https://doi.org/10.1073/pnas.0813132106.
Irina A, Udalova A, Mantovani M, Feldmann. Macrophage heterogeneity in the context of rheumatoid arthritis. Nat Rev Rheumatol. 2016;2(8):472–85. https://doi.org/10.1038/nrrheum.2016.91.
Yanqiong Z, Xia M, Weijie L, Wenjia C, Xiaoyue W, Zhaochen Ma, Na L. Med Res Rev. 2021;41(3):1337–374. https://doi.org/10.1002/med.21762.
Funding
This work was supported by the National Natural Science Foundation of China (No. 81673363).
Author information
Authors and Affiliations
Contributions
Xuan Zhao: Substantial contributions to the conception or design of the work and the acquisition, analysis.
Chengyuan Huang: Drafting the work or revising it critically for important intellectual content.
Meiling Su: Acquisition of data for the work.
Yu Ran: Analysis of data for the work.
Ying Wang: Drafting the work or revising it critically for important intellectual content.
Zongning Yin: Final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised to update the format of the title.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhao, X., Huang, C., Su, M. et al. Reactive Oxygen Species–Responsive Celastrol-Loaded Bilirubin Nanoparticles for the Treatment of Rheumatoid Arthritis. AAPS J 24, 14 (2022). https://doi.org/10.1208/s12248-021-00636-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12248-021-00636-3