Abstract
Background
Sex estimation using the subpubic angle of the pelvis is highly accurate for identification of unknown skeletonized remains. This study compared two methods for measuring the subpubic angle from reconstructed three-dimensional (3D) pelvic models. The aims were to quantify the differences in the subpubic angle measurement by Checkpoint (Method 1) and MeshLab + OnScreenProtractor (Method 2), to determine the 95% limits of agreement and to identify any measurement bias. Multislice computed tomography (MSCT) scans of 85 individuals were used in this study. The MSCT scans were performed on a Siemens SOMATOM Sensation 64 scanner (Siemens Germany Ltd.). Segmentation of the MSCT scans was performed using 3D Slicer to reconstruct 3D pelvic models. Subpubic angle was measured on Checkpoint using four landmarks (Method 1), and with OnScreenProtractor on MeshLab (Method 2).
Results
The intraclass correlation coefficient (ICC) showed a high correlation between repeated measurements in both methods. Subpubic angle measurements by Method 1 and Method 2 were significantly different (p < 0.05). Method 2 (M = 82.2°, SD = 13.5°), consistently showed a larger subpubic angle measurement than Method 1 (M = 77.3°, SD = 12.3°) (consistent bias). More than 95% of the differences (82/85) between Checkpoint and MeshLab fell within the 95% limits of agreement (− 1.4° and 11.4°).
Conclusion
Checkpoint and MeshLab displayed significantly different subpubic angle measurement on a 3D pelvic model, but within the 95% limits of agreement. The MeshLab tended to give a larger measurement (5°), across the magnitude of the subpubic angle. The decision to use the two methods interchangeably depended on the clinical judgment of the observer.
Similar content being viewed by others
Background
The subpubic angle has been widely accepted in different fields of physical anthropology as one of the most sexually dimorphic features of the pelvis (Rösing et al. 2007; Karakas et al. 2013). Sex estimation using the subpubic angle alone, or with other parts of the pelvis—e.g., ventral arc, ischiopubic ramus, pubis, obturator foramen—can reach an accuracy of up to 98% (Phenice 1969; Durić et al. 2005; Rösing et al. 2007). The emergence of virtual anthropology has popularized the use of virtual bone samples. For populations with limited dry bone collections, virtual bones from living contemporary population can be used to establish the morphometric standards (not limited to the subpubic angle of the pelvis, but also other bones). Many researchers have used virtual bones in their research to establish population-specific standards (Decker et al. 2011; Karakas et al. 2013; Franklin et al. 2014; Torimitsu et al. 2015a; Franklin et al. 2016). These population-specific morphometric standards may be used in a forensic scenario to establish a biological profile for identification of unknown skeletal remains, and the subpubic angle may be used for sex estimation in particular.
Several methods have been employed in morphometric studies using virtual bone samples, including photographs, projection images, radiographs, and computed tomography (CT) images (Msamati et al. 2005; Small et al. 2012). Although minimal preparation is required before bone measurement, the methods for virtual bone preparation and measurement can be costly and/ or highly technical. Methods to be employed relies on the type of virtual bone samples and resources available. Traditionally, the subpubic angle is measured on a dry pelvic bone using a protractor. However, on a virtual bone sample, various methods may be used for the subpubic angle measurement (Cignoni et al. n.d.; Decker et al. 2011; Torimitsu et al. 2015b; Franklin et al. 2016).
Checkpoint (Stratovan, Davis, CA) is a 3D shape analysis and morphometric software, which can measure an angle and take linear measurements of bones in 3D. Meanwhile, MeshLab is a free, open-source software for general 3D mesh processing system tool (Cignoni et al.). Checkpoint requires a subscription, while MeshLab is free to be installed and used. Both software offer capability to visualize 3D bone images and to take linear measurements of bones. The measurement of subpubic angle on MeshLab can be performed using an OnScreenProtractor (GNU GPLv3), while on Checkpoint, the angle can be measured using a built-in tool. This study compared between the two methods (Checkpoint and MeshLab) for measurement of subpubic angle on 3DCT pelvic models. This study is a part of research efforts to measure the subpubic angle (with a larger sample size, and other linear pelvic measurements) to establish the population-specific standards. One of these methods will be employed in future study. The results from this study (the software and the level of agreement between the software) may also be useful to other researchers who may want to use virtual pelvic bones to measure the subpubic angle in their research context (either the measurement of subpubic alone or together with other pelvic linear measurements). Thus, this study aimed (1) to quantify the mean differences in the subpubic angle, (2) to determine the 95% limits of agreement, and (3) to identify any measurement bias, between these two methods.
Materials and methods
Materials
A total of 85 abdominopelvic multislice computed tomography (MSCT) scans from individuals presented at the Radiology Department of Universiti Kebangsaan Malaysia Medical Centre (UKMMC) for a radiological investigation were included in this study. Sex and age of the individuals were documented. Anonymization of the MSCT scans was performed using the patient registration number. The samples comprised 48 male individuals (age range, 20–78 years; mean age, 46.6 ± 18.1 years) and 37 female individuals (age range, 22–79 years; mean age, 49.8 ± 13.1 years) from the modern Malaysian population. CT scans with obvious abnormalities (e.g., fractures, prostheses) were excluded from the study. The ethics approval was granted by the Research and Ethics Committee of Universiti Kebangsaan Malaysia (Research Ethics No: UKM PPI/111/8/JEP-2018-006).
Methods
Data acquisition and reconstruction
Abdominopelvic CT imaging was performed using MSCT on a Siemens SOMATOM Sensation 64 scanner (Siemens Germany Ltd.) with scanning and reconstruction protocol (120-140 kVp, variable mAs, 1.0 mm slice thickness, B30f kernel, 512 × 512 matrix). The CT scans were retrieved as Digital Imaging and Communications in Medicine (DICOM). Segmentation of the 3D volumetric data of the CT scans was performed on 3D Slicer (3D Slicer, Brigham Women’s Hospital, Boston, MA, US) (Fedorov et al. 2012), which is a free, open-source, cross-platform software program for medical image computing. Different modules of the 3D Slicer were utilized to segment the region of interest (ROI) based on the radiodensity of the structure. Unwanted parts (i.e., soft tissues, femoral heads, lumbar vertebrae) were removed using the threshold values. A 3D surface model of the pelvis was generated and automatically smoothed by Editor Module and Make Model Effect tools on the 3D Slicer. The pelvic 3DCT model was exported as a polygon file (PLY) for measurement of subpubic angle.
Method 1: Landmark application and subpubic angle measurement on Checkpoint
Application of landmarks on the 3DCT model of the pelvis was performed using Stratovan Checkpoint (Version 2018.09.07.0325). Segmentation based on the threshold density removed the pubic cartilage from the final 3D pelvic model due to its lower Hounsfield unit (HU) as compared to the pelvic bone. Four landmarks were used for measurement of the subpubic angle, to accommodate for the post-segmentation gap between the symphyses pubis. Landmarks were defined and illustrated (Table 1 and Fig. 1). Following the landmark application, the subpubic angle was automatically measured using a built-in, angle-measuring tool in the Checkpoint software. In a landmark-based measurement, the reliability of measurement depends on the repeatability of landmark identification by the observer, according to the landmark protocol (Zelditch and Swiderski n.d.). The subpubic angle was measured twice by one observer (first and second sets of measurement). The repeated measurements (first and second sets) were used in the reliability study for both methods. In the method comparison study, only one set of measurement (first set) from each method was used in the analysis (Bland and Altman 1986).
Pelvic image showing subpubic angle measurement using the Checkpoint (Method 1). Landmarks definition in Table 1
Method 2: Subpubic angle measurement on MeshLab with OnScreenProtractor
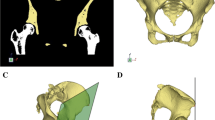
Measurement of the subpubic angle on the MeshLab was performed using an OnScreenProtractor (GNU GPLv3), which is a Java application that allows measurement of an angle on the computer screen. The 3D pelvic model was properly oriented (Fig. 2) on the MeshLab for visualization of the subpubic angle (White and Folkens 2005), before the OnScreenProtractor was used to measure the subpubic angle. During the subpubic angle measurement, the 3D pelvic model was rendered static for accurate measurement (Fig. 2). The subpubic angle was measured twice by one observer (first and second sets of measurement). The repeated measurements (first and second sets) were used in the reliability study for both methods. In the method comparison study, only one set of measurement (first set) from each method was used in the analysis.
Statistical analyses
Reliability
Intraclass correlation was performed to test the reliability of repeated measurements. The intraclass correlation coefficient (ICC) estimates and their 95% confidence intervals were based on two-way mixed effects, single measurement for absolute agreement (Bland and Altman 1986; McGraw and Wong 1996). The ICC value is between 0 to 1, in which values greater than 0.9 indicate excellent reliability, values between 0.75 to 0.9 indicate good reliability, values between 0.5 to 0.75 indicate moderate reliability, and values less than 0.5 indicate poor reliability (Koo and Li 2016).
Univariate analysis and method comparison study
Paired sample T test was performed to quantify the difference between the means of measurement by Method 1 (Checkpoint) and Method 2 (MeshLab + OnScreenProtractor). Comparison of Method 1 and Method 2 in this study was conducted according to Bland and Altman (Bland and Altman 1986). Measurement data for both methods were normally distributed (determined using Shapiro-Wilk statistic), albeit it was not necessary for both data to be normally distributed in a study of method comparison (Bland and Altman 1999). Measurement data of Method 1 and Method 2 were plotted in a scatter diagram with a line of equality (the line on which scores would lie if the two methods gave the same measurements), to demonstrate any consistent bias in the measurements by the two methods (Bland and Altman 1986).
A Bland-Altman plot was used to estimate the agreement between Method 1 and Method 2. The differences between measurements (Method 2 − Method 1) were plotted against the average measurements ((Method 1 + Method 2)/sample size). In this study, the differences between measurements were normally distributed (determined using histogram and Shapiro-Wilk statistic), which fulfilled the assumption of 95% limits of agreement in methods comparison study (Bland and Altman 1999). Horizontal lines for the mean difference and the 95% lower and upper limits of agreement (mean + 2SD, mean − 2SD) were plotted to show any measurement bias or outliers. The standard errors and 95% confidence intervals for the limits of agreement were calculated to determine the precision of the estimates. The standard error of the limits of agreement is about \( \sqrt{3\mathrm{S}{\mathrm{D}}^2/n} \), where n is the sample size (Bland and Altman 1986). The 95% confidence intervals for the limits of agreement were calculated from the observed value minus t standard errors to the observed value plus t standard errors (t value is the appropriate point in the t distribution table with n − 1). All data were analyzed using IBM SPSS® Version 25.0 statistical package for Macintosh, and the significance level was set at 0.05.
Results
Intraclass correlation coefficient
The intraclass correlation (r) for the subpubic angle by the Checkpoint was 0.999 (r 0.998 for the lower bound, and r 0.999 for the upper bound with 95% confidence interval). The measurement of the subpubic angle by the MeshLab + OnScreenProtractor exhibited an intraclass correlation of 0.998 (r 0.997 for the lower bound, and r 0.999 for the upper bound with 95% confidence interval). In the present study, for both Method 1 and Method 2, the intraclass correlation for the subpubic angle measurement indicated a strong correlation between measurements by the primary observer on two separate occasions, hence showing high reliability of measurements (McGraw and Wong 1996; Koo and Li 2016).
Univariate statistic
Table 2 represented the descriptive statistics for the subpubic angle measurements by Method 1 and Method 2. Paired sample T test showed that there was a significant difference between the two methods of subpubic angle measurement (t (84) = 14.3, p = 0.001, 95% C.I. [4.28, 5.66]). The mean measurement for Method 2 (M = 82.2°, SD = 13.5°) was significantly larger than Method 1 (M = 77.3°, SD = 12.3°).
Data plot
Scatterplot of the measurements by Method 1 and Method 2 is shown in Fig. 3. Nearly all of the points laid to the left of the line of equality, which indicated a consistent bias between both methods. Method 2 (MeshLab + OnScreenProtractor) tended to give a larger subpubic angle measurement by 5° (rounded from 4.97°), across the magnitude of the subpubic angle (Fig. 4).
Subpubic angle measured by Method 1 and Method 2, with the line of equality (the scores would lie on this line if the two methods gave the same measurements). Nearly all of the points laid to the left of the line of equality, which indicated a consistent bias between both methods. Method 2 (MeshLab + OnScreenProtractor) consistently exhibited larger subpubic angle measurement
Bland-Altman plot
The differences between measurements were plotted against the average measurements in the Bland-Altman plot (mean difference 4.97° ± 3.2°) (Fig. 4). The limits of agreement were between − 1.4° and 11.4°, which means that for 95% of individuals, the subpubic angle measurement by Method 2 would be 1.4° smaller and 11.4° larger, than that measured by Method 1. More than 95% of the differences (82/85) fell within the limits of agreement (− 1.4° and 11.4°), with one outlier above the upper limit of agreement and two outliers below the lower limit of agreement. As expected in this study sample population (n = 85), several observations (0.28 to 8.2) were probably laid outside the 95% limits of agreement (Bland and Altman 1986).
Precision of estimated limits of agreement
The limits of agreement in this study were only estimates of the values for the whole population. Standard errors and confidence intervals would illustrate the precision of the estimated limits of agreement when the differences were normally distributed (Bland and Altman 1986, 1999). In this study, the differences were indeed normally distributed. Thus, standard errors and confidence intervals could be used to illustrate the precision of the estimates. The 95% confidence intervals for the limits of agreement were illustrated (dashed lines) (Fig. 4). The confidence intervals for the lower and upper limits of agreement was − 0.2° to −2.6° and 10.2° to 12.6°, respectively.
Discussion
Different types of bone samples require different methods of preparation and analysis to obtain an accurate measurement. The current trend of using virtual bone samples includes the MSCT scan of bones, for the development of population standards to establish a biological profile of unknown skeletal remains (Franklin et al. 2016). Computed tomography (CT) bone samples can be measured using different techniques and software, ranging from free, open-source software to state-of-the-art, expensive software. This study compared the agreement of two different techniques for subpubic angle measurement by Checkpoint (Method 1), a subscription-based software, and MeshLab + OnScreenProtractor (Method 2), which were free software. Both methods were relatively easy to use, in the measurement of subpubic angle on reconstructed 3D pelvic models.
Technically, the 3D pelvic models resemble more of a real pelvic bone compared to the 2D pelvic images (e.g., photographs, radiographs, projection images). During measurement of the subpubic angle, the observer can manipulate and move a 3D bone model better than in 2D, to determine the subpubic angle. Models in 3D are flexible in 360°, while in 2D are relatively fixed in position, imposing some restrictions in their measurements. However, measurements using a 3D model with a software that measures in 2D can lead to some errors associated with measurement in 2D (Muñoz-Muñoz and Perpiñán 2010; Kula et al. 2017).
Some lack of agreement is inevitable when using different methods of measurement, to measure the same variable, on the same sample (Bland and Altman 1986). However, the amount of disagreement between the methods matters in deciding whether the new method can replace the “standard” method or the two methods (new and “standard”) can be used interchangeably (Bland and Altman 1986). It is vital that the disagreement amount does not affect the interpretation of the results (Bland and Altman 1999). Ideally, both methods in this study should be compared to the traditional method of subpubic angle measurement, using a protractor. However, this is impossible to perform as the samples were obtained from living individuals. Thus, measurement protocols nearest to the “standard” method (protractor) may be regarded as the protocol that will provide measurement closest to that measured by a protractor, which was the protocols in Method 1 using the Checkpoint (measured in 3D).
Measurement of the subpubic angle by Method 1 resembled more of a measurement on a real bone. The 3D pelvic model can be rotated 360° to determine the exact anatomical landmarks for the subpubic angle measurement defined in the study protocol (Table 1, Fig. 1). Landmarks can be moved (after the angle was initially measured using the angle measurement tool of the software) if required. The software automatically re-determined the “new” angle, until the observer was satisfied with the location of the landmarks.
In Method 2, the 3D pelvic bone model was viewed in 360° and properly oriented to visualize the subpubic angle before the measurement using the OnScreenProtractor. The OnScreenProtractor measured the subpubic angle on the model, on the computer screen, in 2 dimensions (2D). The pelvic model was rendered static during the measurement. If the pelvic model was moved, the OnScreenProtractor had to be repositioned to measure the subpubic angle.
According to Bland and Altman (Bland and Altman 1999, 2003), repeatability is also a vital characteristic in the method comparison study. In this study, both methods had achieved high repeatability between repeated measurements (using the ICC). Both methods were able to measure the subpubic angle on a 3D pelvic models reconstructed from MSCT scans. However, measurement on the MeshLab required well-defined positioning of the 3D models, before the measurement by the OnScreenProtractor. The OnScreenProtractor measured the subpubic angle in 2D, albeit the pelvic bone model was in 3D. Different positioning of the 3D model of pelvis, not according to the study protocol, will give different measurement values.
In Method 1 and Method 2 comparison, the confidence intervals for the lower limit of agreement was − 0.2° to − 2.6°, and for the upper limit of agreement was 10.2° to 12.6°. Narrow confidence intervals reflected a large sample size and small variation of the differences. Meanwhile, wide confidence intervals indicated a small sample size and large variation of the differences (Bland and Altman 2003). This study demonstrated relatively small intervals for the mean difference (4.28° to 5.66°), and the limits of agreement (lower, − 0.2° to − 2.6° and upper, 10.2° to 12.6°), between the two methods. Nevertheless, the limits of agreement were quite large (− 1.4° and 11.4°). The decision for how small the limits of agreement, and the acceptability of the degree of agreement between the two methods of measurement remains a clinical judgment, and not a statistical one (Bland and Altman 1986). Experts in physical anthropology should decide whether the limits of agreement are small enough for the two methods to be used interchangeably.
The study compared two methods to measure the subpubic angle on a virtual pelvic bone reconstructed from CT scan images, to determine the difference/agreement between these two methods. It is of practical value, which may be used in forensic studies that use similar sample (i.e., virtual pelvic bones) to measure the subpubic angle (as one of the parameters) to establish population standards. We recommended to use Method 1 because it resembles more of subpubic angle measurement on a real bone, as this method measures in 3D, while Method 2 measures in 2D. Nonetheless, the measurements using the two methods were still within the 95% limits of agreement, which means that measurement using Method 2 may also be used. The difference in subpubic angle between the two methods were about 5°. The next step from this study, we wished to use Method 1 in a study for sex estimation in the Malaysian population, with the subpubic angle as one of the parameters (using virtual bones).
Conclusions
The comparison between two methods of subpubic angle measurement (Method 1 - Checkpoint, and Method 2 - MeshLab + OnScreenProtractor), on 3D pelvic models, showed significantly different mean measurements. There was a consistent bias between these methods, in which Method 2 exhibited a larger subpubic angle measurement than those by Method 1. However, the differences between these methods of measurements fell within the 95% limits of agreement. The decision on whether these two methods could be used interchangeably depends on how the differences in the subpubic angle may affect sex estimation. Other factors that may also affect in making the decision include the availability of resources and how close the measurement technique resembles the measurement on a real pelvic bone. Future research into subpubic angle (and other bones) measurements should remain cautious of any biases in the different methods of measurement.
Availability of data and materials
Data will not be shared for public access.
Abbreviations
- 2D:
-
Two dimensional
- 3D:
-
Three dimensional
- CT:
-
Computed tomography
- DICOM:
-
Digital imaging and communication in medicine
- HU:
-
Hounsfield unit
- ICC:
-
Intraclass correlation coefficient
- MSCT:
-
Multislice computed tomography
- PLY:
-
Polygon file
- ROI:
-
Region of interest
- SD:
-
Standard deviation
References
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet (London, England) 1:307–310
Bland JM, Altman DG (1999) Measuring agreement in method comparison studies. Stat Methods Med Res 8:135–160. https://www.doi.org/10.1177/096228029900800204
Bland JM, Altman DG (2003) Applying the right statistics: analyses of measurement studies. Ultrasound Obstet Gynecol 22:85–93. https://www.doi.org/10.1002/uog.122
Cignoni P, Callieri M, Corsini M, Dellepiane M, Ganovelli F, Ranzuglia G (2008) MeshLab: an Open-Source Mesh Processing Tool. Sixth Eurographics Italian Chapter Conference, page 129–136.
Decker SJ, Davy-Jow SL, Ford JM, Hilbelink DR (2011) Virtual Determination of sex: metric and nonmetric traits of the adult pelvis from 3D computed tomography models. J Forensic Sci 56:1107–1114. https://www.doi.org/10.1111/j.1556-4029.2011.01803.x
Durić M, Rakočević Z, Donić D (2005) The reliability of sex determination of skeletons from forensic context in the Balkans. Forensic Sci Int 147:159–164. https://www.doi.org/10.1016/j.forsciint.2004.09.111
Fedorov A, Beichel R, Kalpathy-Cramer J et al (2012) 3D Slicer as an image computing platform for the Quantitative Imaging Network. Magn Reson Imaging 30:1323–1341. https://www.doi.org/10.1016/j.mri.2012.05.001
Franklin D, Cardini A, Flavel A, Marks MK (2014) Morphometric analysis of pelvic sexual dimorphism in a contemporary Western Australian population. Int J Legal Med 128:861–872. https://www.doi.org/10.1007/s00414-014-0999-8
Franklin D, Swift L, Flavel A (2016) ‘Virtual anthropology’ and radiographic imaging in the Forensic Medical Sciences. Egypt J Forensic Sci 6:31–43. https://www.doi.org/10.1016/J.EJFS.2016.05.011
Karakas HM, Harma A, Alicioglu B (2013) The subpubic angle in sex determination: anthropometric measurements and analyses on Anatolian Caucasians using multidetector computed tomography datasets. J Forensic Leg Med 20:1004–1009. https://www.doi.org/10.1016/j.jflm.2013.08.013
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155–163. https://www.doi.org/10.1016/j.jcm.2016.02.012
Kula TJ, Ghoneima A, Eckert G et al (2017) Two-dimensional vs 3-dimensional comparison of alveolar bone over maxillary incisors with A-point as a reference. Am J Orthod Dentofac Orthop 152:836–847.e2. https://www.doi.org/10.1016/j.ajodo.2017.05.030
McGraw KO, Wong SP (1996) Forming inferences about some intraclass correlation coefficients. Psychol Methods 1:30–46. https://www.doi.org/10.1016/j.ajodo.2017.05.030
Msamati BC, Igbigbi PS, Manda JK (2005) The sub-pubic angle in adult indigenous Malawian subjects. East Afr Med J 82:643–648
Muñoz-Muñoz F, Perpiñán D (2010) Measurement error in morphometric studies: comparison between manual and computerized methods. Ann. Zool. Fennici 47:46–56
Phenice TW (1969) A newly developed visual method of sexing the os pubis. Am J Phys Anthropol 30:297–301. https://www.doi.org/10.1002/ajpa.1330300214
Rösing FW, Graw M, Marré B et al (2007) Recommendations for the forensic diagnosis of sex and age from skeletons. HOMO 58:75–89. https://www.doi.org/10.1016/j.jchb.2005.07.002
Small C, Brits DM, Hemingway J (2012) Quantification of the subpubic angle in South Africans. Forensic Sci Int 222:395.e1–395.e6. https://www.doi.org/10.1016/j.forsciint.2012.06.002
Torimitsu S, Makino Y, Saitoh H et al (2015a) Stature estimation in Japanese cadavers based on pelvic measurements in three-dimensional multidetector computed tomographic images. Int J Legal Med 129:633–639. https://www.doi.org/10.1007/s00414-014-1000-6
Torimitsu S, Makino Y, Saitoh H et al (2015b) Morphometric analysis of sex differences in contemporary Japanese pelves using multidetector computed tomography. Forensic Sci Int 257:530.e1–530.e7. https://www.doi.org/10.1016/j.forsciint.2015.10.018
White TD, Folkens PA (2005) The human bone manual. Elsevier
Zelditch M, Swiderski DL (2012) Sheets HD Geometric morphometrics for biologists: a primer. Elsevier Academic Press.
Acknowledgements
We would like to express our gratitude to the staff in the Radiology department of UKM Medical Center, for giving access to the CT scan images for the study. We also offer our thanks to the Universiti Kebangsaan Malaysia for financing the research project.
Consent to participate
Not applicable (retrospective data acquired under ethics approval by the research and ethics committee of Universiti Kebangsaan Malaysia)
Funding
The research project was funded by Universiti Kebangsaan Malaysia under the university fundamental grant (Grant No: UKM FPR.4/244/FF-2018-036, Project Code No: FF 2018-036).
Author information
Authors and Affiliations
Contributions
SHMA contributed to the conceptualization, methodology, software, validation, formal analysis, investigation, resources, data curation, writing of the original draft, writing of the review and editing, visualization, and project administration. NO contributed to the methodology, validation, and investigation. MSS contributed to the methodology and resources. NANI contributed to the methodology and software. HH contributed to the methodology and software. FMN contributed to the conceptualization, methodology, software, validation, formal analysis, investigation, resources, data curation, writing of the original draft, writing of the review and editing, visualization, supervision, project administration, and funding acquisition. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The ethics approval was granted by the Research and Ethics Committee of Universiti Kebangsaan Malaysia (Research Ethics No: UKM PPI/111/8/JEP-2018-006).
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Mohd Ali, S.H., Omar, N., Shafie, M.S. et al. Comparison of two methods for subpubic angle measurement from reconstructed three-dimensional pelvic model. Egypt J Forensic Sci 9, 57 (2019). https://doi.org/10.1186/s41935-019-0163-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s41935-019-0163-1