Abstract
Background
In 2020, a new coronavirus, SARS-CoV-2, quickly spread worldwide within a few months. Although coronaviruses typically infect the upper or lower respiratory tract, the virus RNA can be detected in plasma. The risk of transmitting coronavirus via transfusion of blood products remains. As more asymptomatic infections are identified in COVID-19 cases, blood safety has become particularly important. Methylene blue (MB) photochemical technology has been proven to inactivate lipid-enveloped viruses with high efficiency and safety. The present study aimed to investigate the SARS-CoV-2 inactivation effects of MB in plasma.
Methods
The SARS-CoV-2 virus strain was isolated from Zhejiang University. The live virus was harvested from cultured VERO-E6 cells, and mixed with MB in plasma. The MB final concentrations were 0, 1, 2, and 4 μM. The “BX-1 AIDS treatment instrument” was used at room temperature, the illumination adjusted to 55,000 ± 0.5 million Lux, and the plasma was irradiated for 0, 2, 5, 10, 20, and 40 mins using light at a single wavelength of 630 nm. Virus load changes were measured using quantitative reverse transcription- PCR.
Results
BX-1 could effectively eliminate SARS-CoV-2 within 2 mins in plasma, and the virus titer declined to 4.5 log10 TCID50 (median tissue culture infectious dose)/mL.
Conclusion
BX-1 is based on MB photochemical technology, which was designed to inactivate HIV-1 virus in plasma. It was proven to be safe and reliable in clinical trials of HIV treatment. In this study, we showed that BX-1 could also be applied to inactivate SARS-CoV-2. During the current outbreak, this technique it has great potential for ensuring the safety of blood transfusions, for plasma transfusion therapy in recovering patients, and for preparing inactivated vaccines.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Corona virus disease 2019 (COVID-19) is caused by severe acute respiratory syndrome (SARS)-corona virus (CoV)-2. The first outbreak occurred at the end of 2019, causing symptoms such as fever and pneumonia. In serious cases, the patient might die. As of the early March 2021, the COVID-19 epidemic had appeared in all continents except Antarctica, about 117 million people have been diagnosed worldwide, and the death toll has approached 2.6 million, seriously threatening global public health [1].
SARS-CoV-2 was first isolated from epithelial cells of the human airway, and was identified by next-generation sequencing technology in January 2020 as a new member of the beta coronaviruses (β-CoVs) [2]. Coronaviruses are enveloped, single-stranded RNA viruses [2]. From 2002 to 2003, more than 8000 patients were infected by SARS-CoV, which causes SARS, and the World Health Organization (WHO) finally reported 774 related deaths. Since September 2012, a total of 2494 laboratory-confirmed Middle East respiratory syndrome (MERS)-CoV infected cases have been reported. The WHO has reported 858 MERS-CoV-related deaths [3, 4]. These emerging infectious diseases with global transmission are caused by β CoVs.
Although coronaviruses cause respiratory tract infections, several studies have shown that the viral RNA of SARS-CoV [5], MERS-CoV [6], or SARS-CoV-2 [7, 8] can be detected in blood plasma. As early as 2003, the WHO noted that blood products could be contaminated with SARS-CoV. Although no cases of SARS-CoV infection caused by blood transfusion have been reported, there is still a theoretical risk of transmitting SARS-CoV or other coronaviruses through blood transfusion [9]. As more asymptomatic infections are identified among COVID-19 cases [10], blood safety becomes more important [11, 12]. In addition, there are currently no specific drugs or vaccines that are effective against SARS-CoV-2. Patient convalescent plasma therapy could be a rapid and effective treatment for this epidemic situation [13]. However, the critical aspect of this method is to ensure the complete inactivation of SARS-CoV-2 in the plasma from donors. There is an urgent need for a reliable and practical method of plasma SARS-CoV-2 inactivation.
Photochemical treatment methods are used as pathogen inactivation/reduction technologies (PRTs). Photochemical methods to kill viruses are performed by adding methylene blue (MB) into blood products followed by visible light treatment. Methylene blue is a photosensitizer with a maximum absorption peak of 670 nm. It is usually used as an antidote to treat methemoglobinemia and cyanide poisoning caused by nitrite poisoning. The surface of MB carries a positive charge. It can be embedded into DNA or RNA, especially in combination with negatively charged G-C base pairs of viral nucleic acids. Under visible light, MB absorbs light energy, activates it from the ground state to a singlet state, and generates singlet oxygen through electron transfer, which damages and breaks nucleic acids to kill viruses. Viral envelopes and nucleic acids can be targets of MB attack. Alamdari and colleagues used leucomethylene blue, a reduced form of MB, as a therapeutic method for COVID-19 infection [14]. Furthermore, they used a combination of MB-vitamin C-N-acetyl Cysteine to treat five patients with COVID-19 and four out of five survived [15]. The possibility of using MB for either the prevention of viral infection or the development of photoactive fabrics has been proposed by Almeida et al. [16]. Under light, MB can cause nucleic acid strand breaks [17]. The visible light source can be a halogen lamp, a metal halide lamp, or a fluorescent lamp, with full-band white light. However, because of the low excitation efficiency of MB in full-band white light, this process also generates heat to destroy plasma components. The ‘BX-1 AIDS treatment instrument’, developed by Boxin Biotechnology Development LTD (Beijing, China), uses LED single wavelength light combined with MB and is highly effective at killing various lipid enveloped viruses, such as HIV-1 and other viruses [18, 19]. As SARS-CoV-2 is a new type of coronavirus, its tolerance to physicochemical conditions is unclear. Therefore, in the present study, the ‘BX-1 AIDS treatment instrument’ was used to study the plasma inactivation of a SARS-CoV-2 isolate from Zhejiang University.
Methods
Cells, instruments, reagents, and viruses
VERO-E6 cells bought from ATCC (Manassas, VA, USA; Cat. (ATCC® CRL-1586™) were stored in the laboratory of Zhejiang University. Dulbecco’s modified Eagle’s medium (DMEM), fetal bovine serum (FBS), penicillin/streptomycin (P/S), and phosphate-buffered saline were bought from GIBCO (Grand Island, NY, USA). MB is a product of Jichuan Pharmaceutical Group Co., Ltd. (Taixin, China). Human plasma was donated by volunteers, and written informed consents were obtained. All experimental operations involving live viruses were carried out in Zhejiang University’s Biosafety Level 3 (BSL-3) Laboratory. The research protocol was approved by the Ethics Committee of the First Affiliated Hospital of Zhejiang University School of Medicine.
Methylene blue-light inactivated virus
To 180 mL of healthy human plasma, 20 mL of live SARS-CoV-2 spike virus was added. Diluted MB was added to 200 mL of the plasma-virus mixture and mixed to a final MB concentration of 1, 2, or 4 μM. The “BX-1 AIDS treatment instrument” was used at room temperature, and illumination was adjusted to 55,000 ± 0.5 million Lux. The plasma samples were irradiated for 0, 2, 5, 10, 20, or 40 mins under light at a single wavelength of 630 nm. About 1 mL of plasma was taken at each time point, diluted 10-fold with DMEM medium containing 2% FBS, and filtered through a 0.45-μm filter (Millipore, Billerica, MA, USA) for virus titer detection. At the same time, a virus control was set (only virus in the plasma, left at room temperature for 40 mins as an untreated control), a control with pure MB was set (virus and 4 μM MB added to the plasma, with no light treatment, and allowed to stand for 40 mins as a control for the effect of MB on the virus), and finally a light-only control was set (only the virus was added to the plasma, and light was used for 40 mins as a control of the effect of light on the virus). This experiment was repeated three times.
Virus titer measurement
After trypsinization of VERO-E6 cells, 1 × 104 cells/well were inoculated into 96-well cell culture plates in 100 μL of culture medium per well. After the cells grew into a single layer in the 96-well plate, the culture medium was discarded and the treated plasma was seeded into the wells. The treated plasma was log-diluted with 2% FBS in DMEM medium from 102–107times. This process was repeated for 4 wells per dilution, 200 μL/well. Normal cell control wells were established (with cells, virus-free). The 96-well plate was placed in an incubator with 5% CO2 at 37 °C. After 3 h of incubation, the supernatant was washed off, and 200 μL /well of 2% FBS DMEM medium was added. Cell lesions were observed every 24 h until 6 d. The TCID50 (median tissue culture infectious dose) was calculated according to the Reed-Muench method. The cell culture supernatant at 6 d of the culture was pipetted, and the viral nucleic acid load was measured. This experiment was repeated three times.
Three generations of blind tests
One milliliter of the test plasma with virus and 1,2, and 4 μM MB was irradiated for 40 min. It was then diluted 10 times with 2% FBS DMEM medium, filtered through a 0.45-μm filter, and added to VERO-E6 cells. After 48 h, 1 mL of the supernatant of the culture was diluted 10 times with 2% FBS DMEM medium, and added to VERO-E6 cells for three passages. These cells were observed for cytopathic effects. For the duration of the 3rd generation of cell blind transmission, the sample was deemed positive (+) if cytopathic lesions appeared at any time, indicating that the virus was not completely inactivated; samples were deemed negative (−) if no cytopathic lesions appeared, indicating that the virus had been completely inactivated. This experiment was repeated three times.
Viral load of culture supernatant measured using quantitative reverse transcription-polymerase chain reaction (qRT-PCR)
Nucleic acid extraction: Using 200 μL of virus culture supernatant, the MVR01 magnetic bead method nucleic acid extraction kit was used (article number: ZM-0044, Shanghai Zhijiang Biotechnology Co., Ltd., Shanghai, China) in an EX2400 automatic nucleic acid extraction instrument (Shanghai Zhijiang Biotechnology Co., Ltd). Virus RNA was extracted, and the elution volume was about 50 μL.
qRT-PCR: A new coronavirus nucleic acid assay kit (Cat. No. Z-RR-0479-02-50, Shanghai Zhijiang Biotechnology Co., Ltd.) was used for qRT-PCR to detect the viral load, following the manufacturer’s instructions. Briefly, the qRT-PCR amplification reaction tube was placed on a LightCycler® 480II (Roche, Basel, Switzerland) qPCR instrument, and FAM and VIC (or TEXAS RED) fluorescence channels were selected for detection. The recommended cycle parameter settings were: 45 °C for 10 min and 95 °C for 15 min; then 45 cycles of 95 °C for 15 s and 60 °C for 60 s; with single-point fluorescence detection at 60 °C. A cycle threshold (CT) value below 35 was considered effective amplification, and a CT value above 35 was considered undetected.
Statistical analysis
The statistical analyzes were performed using SPSS 20.0 (IBM Corp., Armonk, NY USA). Student’s t-test was employed if the measurement data exhibited a normal distribution, and non-parametric test if it did not exhibit a normal distribution. P < 0.05 was considered to indicate statistical significance.
Results
Effect of SARS-CoV-2 infection on VERO-E6 cells
SARS-CoV-2 (100 μL of 4 log10 TCID50/mL) was seeded into a 96-well plate with monolayers of VERO-E6 cells and cultured to observe the CPE. SARS-CoV-2 had a strong CPE, and the infected cells showed obvious pathological necrosis and large-scale detachment (Fig. 1).
VERO-E6 cells infected by SARS-CoV-2 across different treatment groups (100 ×). To 180 mL of healthy human plasma, 20 mL of indicator virus was added at a 9: 1 (V: V) ratio, and mixed. Methylene blue (MB) was added to 200 mL of plasma virus mixture and mixed to a final concentration of 1 μM (a), 2 μM (b), or 4 (c) μM. The “BX-1 AIDS treatment instrument” was used at room temperature, the illumination adjusted to 55,000 ± 0.5 million Lux, and irradiation was carried out for 40 mins under single wavelength 630-nm light. The virus control (d) was set (only virus in the plasma, left at room temperature for 40 mins as an untreated control), and control with pure 1 μM MB (e) was set (virus and 1 μM MB added to the plasma, with no light treatment, and allowed to stand for 40 mins as a control for the effect of MB on the virus). Finally, the light-only control (f) was set (only the virus was added to the plasma, and light was used for 40 mins as a control of the effect of light on virus). This experiment was repeated three times
BX-1-MB photochemical method inactivation of SARS-CoV-2
SARS-CoV-2 (100 μL of 4 log10 TCID50/mL) was seeded into a 96-well plate with a single layer of VERO-E6 cells, and 1 μM (Fig. 1a), 2 μM (Fig. 1b), or 4 μM of MB (Fig. 1c) was added. Blue light was applied for 40 mins. The control groups were the virus only (Fig. 1d), MB plus no illumination group (Fig. 1e) and the virus-only illuminated group (Fig. 1f). All treatments were cultured and observed for the CPE. 1 μM, 2 μM, and 4 μM of MB could completely inactivate the virus, and the inactivated virus had no effect on cell growth. The non-illuminated group (Fig. 1e) and the virus-only illuminated group (Fig. 1f) were unable to inactivate the virus, and the infected cells showed significant lesion necrosis and large-scale exfoliation.
In the process of three passages of cell blind transmission, no cell lesions appeared in any generation of cells, indicating that the virus had been completely inactivated. The qPCR results indicated that virus-containing plasma treated with 1, 2, and 4 μM of MB and light could completely inactivate the virus in 2 min (Table 1).
Viral titer detection after application of the BX-1 MB photochemical method to inactivate SARS-CoV-2
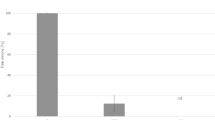
Using the CPE method, we found that the BX-1 MB photochemical method could inactivate SARS-CoV-2 in 40 mins. To further study the inactivation efficiency, we detected the viral titer of BX-1 MB photochemical-treated virus-plasma at 0, 2, 5, 10, 20, and 40 min. Viral titer tests found that virus plasma containing 1 μM and 2 μM MB had a virus reduction > 4 Log10 TCID50 for 2 mins; the group with 4 μM MB had an initial titer because differences between batches in the test (Fig. 2).
Discussion
The new coronavirus SARS-CoV-2, which appeared in December 2019, spread globally within 3 months and is being monitored closely worldwide. The following are safety considerations for blood transfusions or blood products: (1) Viral RNA in plasma or serum can be detected in patents with COVID-19 2 or 3 d before the onset of symptoms [8]; (2) most patients, especially young adults who can donate blood, experience milder symptoms than do the elderly; (3) multiple asymptomatic carriers have been found in China and other countries, which increases the possibility of blood donation by COVID-19 or virus carriers [10]; (4) infection rates of patients in the incubation period are still uncertain, and there is yet no data on viral load in plasma, serum, or lymphocytes during the incubation period. Blood transfusions carry the risk of transmitting SARS-CoV-2, and thus measures to inactivate pathogens in blood products should be explored as soon as possible.
Coronaviruses are enveloped, single-stranded RNA viruses. Previous studies indicated that coronaviruses are generally susceptible to acid, alkaline, and heat [20]. After the outbreak of SARS and MERS, some studies investigated the potential of PRTs to reduce or completely eliminate the potential risks of coronavirus transmission through blood products or derivatives [21]. Research on plasma inactivation methods has focused on heat and photochemical treatment methods. (1) Heat method, in general, 30 mins at 60 °C is sufficient to reduce SARS-CoV from cell-free plasma [22], and 25 mins at 56 °C reduced MERS virus by more than 4 log10 TCID50/mL [23]. Heating can denature proteins in blood products; therefore, it cannot be used to manufacture plasma-derived products. (2) Photochemical treatment methods. Different wavelengths of light affect the viability of SARS and MERS viruses in the blood. UV light, Amotosalen, or riboflavin can inactivate pathogenic nucleic acids [22]. Keil et al. performed SARS-CoV-2 inactivation of blood products in standard blood bags using the Riboflavin and the UV methodand the data indicated that the reductions of the viral titres were ≥ 3.40 Logs and ≥ 4.53 Logsin plasma and platelets, respectively [24], which are on the same order of magnitude as our data. It has been previously reported that MB plus visible light is capable of inactivating coronavirus in plasma [21, 25] Previously, the prototype ‘plasma virus inactivator’ JY-1 developed by Boxin (Beijing) Biotechnology Development LTD, under the condition of a single-wavelength LED illumination of 40,000 lx, was used for treatment together with 1 μM MB for 30 min [26, 27]. The new BX-1 ‘AIDS treatment instrument’ used in this study can reduce the titer of new coronavirus SARS-CoV-2 by 4.5 log10 TCID50/mL in 2 mins (Fig. 2), which is a strong advantage for inactivation of viruses in plasma.
MB and LED based BX-1 technology provides a new approach for inactivation of SARS-CoV-2 in plasma, which may be useful for convalescent plasma therapy of critical ill patients with COVID-19. Convalescent plasma therapy is a rapid and effective treatment that has been applied for severe infectious diseases for over 100 years [13]. In 1890, Emil von Behring from Germany and Saburo Kitari from Japan announced an important discovery: They kept injecting small amounts of non-lethal tetanus into animals, which produced an antitoxin in the blood. This could neutralize the bacillus toxicity of tetanus injected into the body. The serum could also be isolated from animals that have acquired tetanus immunity and injected into other animals to enhance their immunity to tetanus. Emil Behring won the 1901 Nobel Prize in Medicine for his research on diphtheria serum therapy. The earliest application of convalescent plasma therapy allowed humans to overcome diphtheria [13]. In 2014, during Ebola virus disease outbreaks, the WHO recommended the use of convalescent plasma as an empirical treatment [28]. Previously, in the clinical treatment of SARS coronavirus, doctors in Hong Kong, Taiwan, and Singapore had shown that convalescent plasma therapy could improve the conditions for critical ill patients with SARS for whom comprehensive treatment had not been effective [29]. Given this long history of serum-based treatment in the modern era, and its established safety and efficacy, convalescent plasma transfusion should be used to treat patients with COVID-19 [30].
Conclusion
BX-1 based MB photochemical technology could inactivate SARS-CoV-2 efficiently and has great potential for ensuring the safety of blood transfusions, for plasma transfusion therapy in recovering patients, and for preparing inactivated vaccines.
Availability of data and materials
The datasets used and/or analysed during the current study available from the corresponding author on reasonable request.
Change history
06 May 2021
Editor’s Note: Readers are alerted that concerns have been raised regarding the reliability of this article. Further editorial action will be taken as appropriate once the investigation into the concerns is complete and all parties have been given an opportunity to respond in full.
09 July 2021
A Correction to this paper has been published: https://doi.org/10.1186/s12879-021-06344-9
Abbreviations
- BSL-3:
-
Biosafety Levels 3
- COVID-19:
-
Coronavirus disease outbreak 2019
- CPE:
-
Cytopathic effect
- LED:
-
Light-emitting diode
- MB:
-
Methylene blue
- MERS-CoV:
-
Middle East respiratory syndrome coronavirus
- PRTs:
-
Pathogen inactivation/reduction technologies
- SARS:
-
Severe acute respiratory syndrome
- SARS-CoV-2:
-
Severe acute respiratory syndrome coronavirus type 2
- UV:
-
Ultraviolet
- WHO:
-
World Health Organization
References
WHO. WHO Coronavirus (COVID-19) dashboard. 2021, https://covid19.who.int/.
Zhu N, Zhang D, Wang W, Li X, Yang B, Song J. A novel coronavirus from patients with pneumonia in China, 2019. N Engl J Med. 2020;382(8):727–33. https://doi.org/10.1056/NEJMoa2001017.
WHO. Summary of probable SARS cases with onset of illness from 1 November 2002 to 31 July 2003. https://www.who.int/csr/sars/country/table2004_04_21/en/2004.
WHO. Middle East respiratory syndrome coronavirus (MERSCoV). https://www.who.int/emergencies/mers-cov/en/2013.
Grant PR, Garson J, Tedder RS, Chan PK, Tam JS, Sung JJ. Detection of SARS coronavirus in plasma by real-time RT-PCR. N Engl J Med. 2003;349:2468–9. https://doi.org/10.1056/nejm200312183492522.
Corman VM, Albarrak A, Omrani AS, Albarrak MM, Farah ME, Almasri M. Viral shedding and antibody response in 37 patients with Middle East respiratory syndrome coronavirus infection. Clin Infect Dis. 2016;62:477–83. https://doi.org/10.1093/cid/civ951.
Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y. Clinical features of patients infected with 2019 novel coronavirus in Wuhan. Lancet. 2020. https://doi.org/10.1016/s0140-6736(20)30183-5.
Kim JY, Ko J, Kim Y, Kim YJ, Kim JM, Chung YS, et al. Viral load kinetics of SARS-CoV-2 infection in first two patients in Korea. J Korean Med Sci. 2020;35(7):e86. https://doi.org/10.3346/jkms.2020.35.e86.
WHO: WHO recommendations on SARS and blood safety. 2003, https://www.who.int/csr/sars/guidelines/bloodsafety/en/.
Hu Z, Song C, Xu C, Jin G, Chen Y, Xu X, et al. Clinical characteristics of 24 asymptomatic infections with COVID-19 screened among close contacts in Nanjing, China. medRxiv. 2020. https://doi.org/10.1101/2020.02.20.20025619.
Bai YY, Lingsheng, Wei T, Tian F, Jin D-Y, Chen L, et al. Presumed asymptomatic carrier transmission of COVID-19. JAMA. 2020;323(14):1406–7. https://doi.org/10.1001/jama.2020.2565.
Shahul H, Ebrahim ZAM. COVID-19: preparing for superspreader potential among Umrah pilgrims to Saudi Arabia. Lancet. 2020;395(10227):e48. https://doi.org/10.1016/S0140-6736(20)30466-9.
Hifumi T, Yamamoto A, Ato M. Clinical serum therapy: benefits, cautions, and potential applications. Keio J Med. 2017;66(4):57–64. https://doi.org/10.2302/kjm.2016-0017-IR.
Alamdari DH, Moghaddam A, Amini S, Alamdari AH, Damsaz M, Yarahmadi A. The application of a reduced dye used in orthopedics as a novel treatment against coronavirus (COVID-19): a suggested therapeutic protocol. Arch Bone Jt Surg. 2020;8(Suppl1):291–4. https://doi.org/10.22038/abjs.2020.47745.2349.
Alamdari DHMA, Amini S, Keramati MR, Zarmehri AM, Alamdari AH, Damsaz M, et al. Application of methylene blue -vitamin C-N-acetyl cysteine for treatment of critically ill COVID-19 patients, report of a phase-I clinical trial. Eur J Pharmacol. 2020;885:173494. https://doi.org/10.1016/j.ejphar.2020.173494.
Almeida A, Faustino MA, Neves MG. Antimicrobial photodynamic therapy in the control of COVID-19. Antibiotics. 2020;9(6):320. https://doi.org/10.3390/antibiotics9060320.
M OJDCG. Coagulation function in fresh-frozen plasma prepared with two photochemical treatment methods:methylene blue and amotosalen. Transfusion. 2008;48(1):108–17.
Jiang M, Zhou XP, Xu JB. AIDS treatment instrument (In Chinese). CN Patent 2019, CN110124140A.
Jiang M, Wu H. Photochemical preparation method of autologous plasma inactivated vaccine for treatment of AIDS. CN Patent 2019, CN108578693B.
Rabenau HF, Cinatl J, Morgenstern B, Bauer G, Preiser W, Doerr HW. Stability and inactivation of SARS coronavirus. Med Microbiol Immunol. 2005;194(1-2):1–6. https://doi.org/10.1007/s00430-004-0219-0.
Eickmann M, Gravemann U, Handke W, Tolksdorf F, Reichenberg S, Muller TH. Inactivation of three emerging viruses—severe acute respiratory syndrome coronavirus, Crimean-Congo haemorrhagic fever virus and Nipah virus—in platelet concentrates by ultraviolet C light and in plasma by methylene blue plus visible light. Vox Sang. 2020;115(3):146–51. https://doi.org/10.1111/vox.12888.
Darnell ME, Taylor D. Evaluation of inactivation methods for severe acute respiratory syndrome coronavirus in noncellular blood products. Transfusion. 2006;46(10):1770–7. https://doi.org/10.1111/j.1537-2995.2006.00976.x.
Leclercq I, Batejat C, Burguiere AM, Manuguerra JC. Heat inactivation of the Middle East respiratory syndrome coronavirus. Influenza Other Respir Viruses. 2014;8(5):585–6. https://doi.org/10.1111/irv.12261.
Keil SD, Ragan I, Yonemura S, Hartson L, Dart NK, Bowen R. Inactivation of severe acute respiratory syndrome coronavirus 2 in plasma and platelet products using a riboflavin and ultraviolet light-based photochemical treatment. Vox Sang. 2020;115(6):495–501. https://doi.org/10.1111/vox.12937.
Eickmann M, Gravemann U, Handke W, Tolksdorf F, Reichenberg S, Muller TH. Inactivation of Ebola virus and Middle East respiratory syndrome coronavirus in platelet concentrates and plasma by ultraviolet C light and methylene blue plus visible light, respectively. Transfusion. 2018;58(9):2202–7. https://doi.org/10.1111/trf.14652.
Jinbo X, Shumin D, Xipeng Z, Ping M, Xinsheng Z, Shengyang J, et al. Inactivation of SARS coronavirus in human plasma by methylene blue / light method. Bull Acad Mil Med Sci. 2005;29:2.
Ma P, Zhou XP, Zhang YY, Li P, Jiang SY, Xu JB. Effect of methylene blue/photochemical method for virus inactivation on immunological properties of antibody in plasma. Bull Acad Mil Med Sci 2004, 28:6.
WHO: Use of convalescent whole blood or plasma collected from patients recovered from Ebola virus disease for transfusion, as an empirical treatment during outbreaks. http://apps.who.int/iris/rest/bitstreams/604045/retrieve 2014.
Syed S, Saleem A. Severe acute respiratory syndrome epidemiology and control. Lab Med. 2004;35:112.
Chen L, Xiong J, Bao L, Shi Y. Convalescent plasma as a potential therapy for COVID-19. Lancet Infect Dis. 2020;20(4):398–400. https://doi.org/10.1016/s1473-3099(20)30141-9.
Acknowledgements
We acknowledgement the Boxin (Beijing) Biotechnology Development LTD for providing ‘BX-1 AIDS treatment instrument’ for this study.
Funding
This work was supported by Boxin (Beijing) Biotechnology Development LTD, the Grant for National Key Technologies R&D Program for the 13th Five-Year Plan of China (no. 2018ZX10302–102) and an internal grant from the State Key Laboratory for Diagnosis and Treatment of Infectious Diseases (2020) to CJ. The funding bodies had no role in the design of the study and the collection, analysis, and interpretation of data, and in writing the manuscript.
Author information
Authors and Affiliations
Contributions
CJ, BY, MJ, and NW conceived and designed the study and took responsibility for the integrity of the data and the accuracy of the data analysis. CJ, HY, FL, LC, and XL performed the basic experiments and collected the data. CJ and BY processed the statistical data. CJ, JZ, XZ, HW, and BY drafted the manuscript. BY, MJ, and NW revised the final manuscript. All authors contributed to the data analysis and approved the final version.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Ethics Committee of the First Affiliated Hospital of Zhejiang University School of Medicine (Reference No. 2020-IIT-054). Written informed consents were obtained from the plasma donors.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article has been retracted. Please see the retraction notice for more detail: https://doi.org/10.1186/s12879-021-06344-9
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Jin, C., Yu, B., Zhang, J. et al. RETRACTED ARTICLE: Methylene blue photochemical treatment as a reliable SARS-CoV-2 plasma virus inactivation method for blood safety and convalescent plasma therapy for COVID-19. BMC Infect Dis 21, 357 (2021). https://doi.org/10.1186/s12879-021-05993-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12879-021-05993-0