Abstract
Background
Telaprevir is a protease inhibitor currently used in the treatment of chronic hepatitis C virus (HCV) infection. One of its adverse effects is renal impairment. The Pharmaceutical and Medical Device Agency (PMDA) in Japan reported on telaprevir-related renal dysfunction in 2012. In this study, renal adverse events of telaprevir were investigated using the Japanese Adverse Drug Event Report database. Patient profiles with adverse events might provide useful information for HCV therapy.
Methods
We screened the case reports in Japanese Adverse Drug Event Report database (JADER) of the PMDA. The profiles of patients with renal adverse events were analyzed.
Results
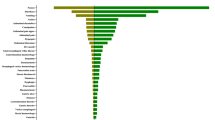
The present results showed that reports of renal adverse events were most common in male patients between 60 and 69 years of age. Significant factors that affect the clinical outcomes of renal adverse events were not detected. However, it was suggested that anorexia is associated with renal adverse events.
Conclusions
The number of reports of renal adverse events were highest in male patients 60 to 69 years of age treated with telaprevir. In addition, our findings suggested that anorexia is correlated with renal adverse events after telaprevir treatment. Further investigation is required to clarify the mechanism of renal impairments during triple therapy. Such knowledge might improve the safety of telaprevir therapy.
Similar content being viewed by others
References
Au JS, Pockros PJ. Novel therapeutic approaches for hepatitis C. Clin Pharmacol Ther. 2014;95:78–88.
Jacobson IM, McHutchison JG, Dusheiko G, et al. Telaprevir for previously untreated chronic hepatitis C virus infection. N Engl J Med. 2011;364:2405–2416.
Zeuzem S, Andreone P, Pol S, et al. Telaprevir for retreatment of HCV infection. N Engl J Med. 2011;364:2417–2428.
Mauss S, Hueppe D, Alshuth U. Renal impairment is frequent in chronic hepatitis C patients under triple therapy with telaprevir or boceprevir. Hepatology. 2014;59:46–48.
Loustaud-Ratti V, Rousseau A, Carrier P, et al. eGFR decrease during antiviral C therapy with first generation protease inhibitors: a clinical significance? Liver Int. 2015;35:71–78.
Virlogeux V, Pradat P, Bailly F, et al. Boceprevir and telaprevir-based triple therapy for chronic hepatitis C: virological efficacy and impact on kidney function and model for end-stage liver disease score. J Viral Hepat. 2014;21: e98–e107.
Kikuchi M, Okuda Y, Ueda Y, et al. Successful telaprevir treatment in combination of cyclosporine against recurrence of hepatitis C in the Japanese liver transplant patients. Biol Pharm Bull. 2014;37:417–423.
Sise ME, Backman ES, Wenger JB, et al. Short and long-term effects of telaprevir on kidney function in patients with hepatitis C virus infection: a retrospective cohort study. PLoS One. 2015;10: e0124139.
Kitano A, Motohashi H, Takayama A, Inui K, Yano Y. Valacyclovir-induced acute kidney injury in Japanese patients based on the PMDA adverse reporting database. Therap Innov Regul Sci. 2015;49:81–85.
Kunze A, Huwyler J, Camenisch G, Gutmann H. Interaction of the antiviral drug telaprevir with renal and hepatic drug transporters. Biochem Pharmacol. 2012;84:1096–1102.
Motohashi H, Inui K. Multidrug and toxin extrusion family SLC47: physiological, pharmacokinetic and toxicokinetic importance of MATE1 and MATE2-K. Mol Aspects Med. 2013;34:661–668.
Motohashi H, Nakao Y, Masuda S, et al. Precise comparison of protein localization among OCT, OAT, and MATE in human kidney. J Pharm Sci. 2013;102:3302–3308.
Motohashi H, Sakurai Y, Saito H, et al. Gene expression levels and immunolocalization of organic ion transporters in the human kidney. J Am Soc Nephrol. 2002;13:866–874.
Masuda S, Terada T, Yonezawa A, et al. Identification and functional characterization of a new human kidney-specific H+/organic cation antiporter, kidney-specific multidrug and toxin extrusion 2. J Am Soc Nephrol. 2006;17:2127–2135.
Tanihara Y, Masuda S, Sato T, Katsura T, Ogawa O, Inui K. Substrate specificity of MATE1 and MATE2-K, human multidrug and toxin extrusions/H+-organic cation antiporters. Biochem Pharmacol. 2007;74:359–371.
Kimura N, Masuda S, Katsura T, Inui K. Transport of guanidine compounds by human organic cation transporters, hOCT1 and hOCT2. Biochem Pharmacol. 2009;77:1429–1436.
Nakada T, Kito T, Inoue K, et al. Evaluation of the potency of telaprevir and its metabolites as inhibitors of renal organic cation transporters, a potential mechanism for the elevation of serum creatinine. Drug Metab Pharmacokinet. 2014;29:266–271.
Karino T, Ozeki I, Hige S, et al. Telaprevir impairs renal function and increases blood ribavirin concentration during telaprevir/pegylated interferon/ribavirin therapy for chronic hepatitis C. J Viral Hepat. 2014;21:341–347.
Hasson H, Messina E, Merli M, et al. Sustained virological response after ten days of triple anti-hepatitis C virus (HCV) therapy with telaprevir plus pegylated interferon and ribavirin in an HIV/HCV co-infected cirrhotic woman. Int J Infect Dis. 2014;29:100–102.
Khalili H, Bairami S, Kargar M. Antibiotics induced acute kidney injury: incidence, risk factors, onset time and outcome. Acta Med Iran. 2013;51:871–878.
Porter GA. Risk factors for toxic nephropathies. Toxicol Lett. 1989;46:269–279.
Manns MP, Markova AA, Calle Serrano B, Cornberg M. Phase III results of Boceprevir in treatment naive patients with chronic hepatitis C genotype 1. Liver Int. 2012;32 Suppl 1:27–31.
Jacobson IM, Dore GJ, Foster GR, et al. Simeprevir with pegylated interferon alfa 2a plus ribavirin in treatment-naive patients with chronic hepatitis C virus genotype 1 infection (QUEST-1): a phase 3, randomised, double-blind, placebo-controlled trial. Lancet. 2014;384:403–413.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ichida, A., Motohashi, H., Kitano, A. et al. Telaprevir-Induced Renal Adverse Events in Japanese Patients Reported in the PMDA Adverse Drug Reactions Reporting Database. Ther Innov Regul Sci 50, 355–360 (2016). https://doi.org/10.1177/2168479015618694
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1177/2168479015618694