Abstract
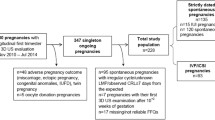
Previously, embryonic growth has been assumed to be uniform, but in recent years, it has become more clear that genetic and environmental factors may influence the intrauterine environment and therefore embryonic growth trajectories as well as pregnancy course and outcome. The objective of this study was to investigate associations between modifiable maternal nutrition and lifestyle factors during the periconception period and embryonic growth. We established a prospective cohort including 342 women less than 13 weeks pregnant. At enrollment, women filled out a questionnaire regarding demographic and medical data and a validated food frequency questionnaire. Participants received multiple 3-dimensional ultrasound examinations up until the 12th week of pregnancy, and crown–rump length (CRL) and embryonic volume (EV) were measured offline using V-Scope Virtual Reality software (version 1.0.0) in a Barco I-Space. Associations between maternal periconception vegetable and fruit intake, folic acid supplement use, smoking, and alcohol consumption and embryonic growth measurements were assessed by linear mixed models adjusted for potential confounders. No or postconception initiation of folic acid supplement use was significantly associated with a 0.76 mm (−7.8%) and 1.63 mm (−3.7%) smaller CRL and a 0.01 cm3 (−19.5%) and 0.86 cm3 (−12.2%) smaller EV at 7+0 and 11+0 weeks of gestation, respectively. Smoking, alcohol consumption, and inadequate fruit and vegetable intake showed weaker associations with embryonic growth parameters. These results emphasize the influence of periconceptional maternal folic acid supplement use on embryonic growth. Results regarding maternal nutrition and lifestyle factors also suggest an association with embryonic growth, but this has to be confirmed in a larger study.
Similar content being viewed by others
References
Blaas HG, Eik-Nes SH, Bremnes JB. The growth of the human embryo. A longitudinal biometric assessment from 7 to 12 weeks of gestation. Ultrasound Obstet Gynecol. 1998;12(5):346–354.
van Uitert EM, Exalto N, Burton GJ, et al. Human embryonic growth trajectories and associations with fetal growth and birthweight. Hum Reprod. 2013;28(7):1753–1761.
Bottomley C, Daemen A, Mukri F, et al. Assessing first trimester growth: the influence of ethnic background and maternal age. Hum Reprod. 2009;24(2):284–290.
Mook-Kanamori DO, Steegers EA, Eilers PH, Raat H, Hofman A, Jaddoe VW. Risk factors and outcomes associated with firsttrimester fetal growth restriction. JAMA. 2010;303(6):527–534.
Steegers-Theunissen RP, Steegers EA. Nutrient-gene interactions in early pregnancy: a vascular hypothesis. Eur J Obstet Gynecol Reprod Biol. 2003;106(2):115–117.
Lane M, Robker RL, Robertson SA. Parenting from before conception. Science. 2014;345(6198):756–760.
Cecchini M, Sassi F, Lauer JA, Lee YY, Guajardo-Barron V, Chisholm D. Tackling of unhealthy diets, physical inactivity, and obesity: health effects and cost-effectiveness. Lancet. 2010; 376(9754):1775–1784.
Haslam DW, James WP. Obesity. Lancet. 2005;366(9492): 1197–1209.
Collaborators GBDRF, Forouzanfar MH, Alexander L, et al. Global, regional, and national comparative risk assessment of 79 behavioural, environmental and occupational, and metabolic risks or clusters of risks in 188 countries, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2015;386(10010):2287–2323.
Gormack AA, Peek JC, Derraik JG, Gluckman PD, Young NL, Cutfield WS. Many women undergoing fertility treatment make poor lifestyle choices that may affect treatment outcome. Hum Reprod. 2015;30(7):1617–1624.
Jaddoe VW, Verburg BO, de Ridder MA, et al. Maternal smoking and fetal growth characteristics in different periods of pregnancy: the generation R study. Am J Epidemiol. 2007;165(10):1207–1215.
Lundsberg LS, Illuzzi JL, Belanger K, Triche EW, Bracken MB. Low-to-moderate prenatal alcohol consumption and the risk of selected birth outcomes: a prospective cohort study. Ann Epidemiol. 2015;25(1):46–54.e43.
Feodor Nilsson S, Andersen PK, Strandberg-Larsen K, Nybo Andersen AM. Risk factors for miscarriage from a prevention perspective: a nationwide follow-up study. BJOG. 2014; 121(11):1375–1384.
Aliyu MH, Wilson RE, Zoorob R, et al. Alcohol consumption during pregnancy and the risk of early stillbirth among singletons. Alcohol. 2008;42(5):369–374.
Gluckman PD, Hanson MA, Cooper C, Thornburg KL. Effect of in utero and early-life conditions on adult health and disease. N Engl J Med. 2008;359(1):61–73.
Jaddoe VW, de Jonge LL, Hofman A, Franco OH, Steegers EA, Gaillard R. First trimester fetal growth restriction and cardiovascular risk factors in school age children: population based cohort study. BMJ. 2014;348:g14.
Steegers-Theunissen RP, Twigt J, Pestinger V, Sinclair KD. The periconceptional period, reproduction and long-term health of offspring: the importance of one-carbon metabolism. Hum Reprod Update. 2013;19(6):640–655.
Godfrey KM, Gluckman PD, Hanson MA. Developmental origins of metabolic disease: life course and intergenerational perspectives. Trends Endocrinol Metab. 2010;21(4):199–205.
Koning AHJ, Rousian M, Verwoerd-Dikkeboom CM, Goedknegt L, Steegers EAP, van der Spek PJ. V-Scope: design and implementation of an immersive and desktop virtual reality volume visualization system. Stud Health Technol Inform. 2009;142: 136–138.
Verwoerd-Dikkeboom CM, Koning AH, Hop WC, et al. Reliability of three-dimensional sonographic measurements in early pregnancy using virtual reality. Ultrasound Obst Gyn. 2008; 32(7):910–916.
Verwoerd-Dikkeboom CM, Koning AHJ, Hop WC, van der Spek PJ, Exalto N, Steegers EAP. Innovative virtual reality measurements for embryonic growth and development. Hum Reprod. 2010;25(6):1404–1410.
Steegers-Theunissen RP, Verheijden-Paulissen JJ, van Uitert EM, et al. Cohort profile: the Rotterdam Periconceptional Cohort (PREDICT study). Int J Epidemiol. 2016;45(2):374–381.
Siebelink E, Geelen A, de Vries JH. Self-reported energy intake by FFQ compared with actual energy intake to maintain body weight in 516 adults. Br J Nutr. 2011;106(2):274–281.
The Netherlands Nutrition Centre. 2015. http://www.voedingscentrum.nl/Assets/Uploads/voedingscentrum/Documents/Profession als/Pers/Factsheets/Factsheet%20Voeding%20en%20zwangers chap.pdf. Accessed August 18, 2016.
World Health Organization. Prevention of Neural Tube Defects. Geneva: Standards for Maternal and Neonatal Care. 2006.
van Uitert EM, van der Elst-Otte N, Wilbers JJ, et al. Periconception maternal characteristics and embryonic growth trajectories: the Rotterdam Predict Study. Hum Reprod. 2013;28(12):3188–3196.
Rousian M, Koning AH, van Oppenraaij RH, et al. An innovative virtual reality technique for automated human embryonic volume measurements. Hum Reprod. 2010;25(9):2210–2216.
Lucock M. Folic acid: nutritional biochemistry, molecular biology, and role in disease processes. Mol Genet Metab. 2000;71(1-2):121–138.
Zeisel SH. Importance of methyl donors during reproduction. Am J Clin Nutr. 2009;89(2):673S-677S.
van Uitert EM, van Ginkel S, Willemsen SP, et al. An optimal periconception maternal folate status for embryonic size: the Rotterdam Predict Study. BJOG. 2014;121(7):821–829.
Koning IV, Groenenberg IA, Gotink AW, et al. Periconception maternal folate status and human embryonic cerebellum growth trajectories: the Rotterdam Predict Study. PLoS One. 2015; 10(10):e0141089.
Refsum H, Nurk E, Smith AD, et al. The Hordaland Homocysteine Study: a community-based study of homocysteine, its determinants, and associations with disease. J Nutr. 2006;136(suppl 6):1731S–1740S.
Wang N, Tikellis G, Sun C, et al. The effect of maternal prenatal smoking and alcohol consumption on the placenta-to-birth weight ratio. Placenta. 2014;35(7):437–441.
Burd L, Roberts D, Olson M, Odendaal H. Ethanol and the placenta: a review. J Matern Fetal Neonatal Med. 2007;20(5):361–375.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Van Dijk, M.R., Borggreven, N.V., Willemsen, S.P. et al. Maternal Lifestyle Impairs Embryonic Growth: The Rotterdam Periconception Cohort. Reprod. Sci. 25, 916–922 (2018). https://doi.org/10.1177/1933719117728801
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719117728801