Abstract
Objective
To evaluate the interobserver repeatability of the coronal view measurements and classification of the uterine malformations (UM) according to the ESHRE/ESGE consensus by transvaginal three-dimensional ultrasound (3D-US).
Methods
89 transvaginal 3D-US volumes acquired during the last two years at Delta Ecografia in Madrid, Spain, were selected from our archive by convenience sampling. Two expert operators blinded from each other, performed post-hoc analysis using render mode and multiplanar-Volume Contrast Imaging (VCI) navigation. Uterine wall thickness at the fundus, indentation of the cavity and indentation of the fundus were measured, classified and sub-classified following the recommendations of the ESHRE/ESGE consensus. The reproducibility of interobserver measurements and classification was examined by calculating intraclass correlation coefficients (ICC) and their 95% confidence intervals (CI) and kappa statistic (k).
Results
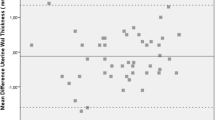
Repeatability in the measurements: uterine wall thickness: ICC = 0.93 (95% CI, 0.90–0.96), P < 0.0001; indentation of the cavity: ICC = 0.93 (95% CI, 0.86-0.96), P < 0.0001; indentation of the fundus: ICC = 0.93 (95% CI, 0.90–0.96), P < 0.0001. Level of agreement in the classification: overall (U0, UI, U2, U3, U4, U5): k = 0.73 (95% CI, 0.61–0.84), P > 0.0001; U2 (U2a, U2b): k = 0.56 (95% CI, 0.31–0.80), P < 0.001 (0.78 observed agreement compared to 0.49 expected); U3 (U3a, U3b, U3c): k = 0.69 (95% CI, 0.16-1.00), P < 0.05 (0.85 observed agreement compared to 0.53 expected); U4 (U4a, U4b): k = 1.00 (95% CI, 1.00–1.00), P < 0.0001.
Conclusions
Transvaginal 3D-US examination of the uterus allows assessment and classification of the UM by the ESHRE/ESGE criteria showing a good interobserver repeatability and reproducibility in most cases.
Similar content being viewed by others
References
Grimbizis GF, Di Spiezio Sardo A, Saravelos SH, et al. The Thessaloniki ESHRE/ESGE consensus on diagnosis of female genital anomalies. Hum Reprod. 2016;13(1):2–7.
Bermejo C, Martinez Ten P, Cantarero R, et al. Threedimensional ultrasound in the diagnosis of Mullerian duct anomalies and concordance with magnetic resonance imaging. Ultrasound Obstet Gynecol. 2010;35(5):593–601.
Bermejo C, Martinez-Ten P, Recio M, et al. Three-dimensional ultrasound and magnetic resonance imaging assessment of cervix and vagina in women with uterine malformations. Ultrasound Obstet Gynecol. 2014;43(3):336–345.
Grimbizis G, Gordts S, Di SpiezoSardo A, et al. The ESHRE/ ESGE consensus on the classification of female genital tract congenital anomalies. Hum Reprod. 2013;28(8):2032–2044.
Lantz CA, Nebenzahl E. Behavior and interpretation of the k statistic: resolution of the two paradoxes. J Clin Epidemiol. 1996;49(4):431–434.
Bland JM, Altaian DG. Statistical methods for assessing agree-ment between two methods of clinical measurement. Lancet. 1986;1(8476):307–310.
The American Fertility Society. The American Fertility Society classifications of adnexal adhesions, distal tubal obstruction, tubal occlusion secondary to tubal ligation, tubal pregnancies, Muller-ian anomalies and intrauterine adhesions. Fertil Steril. 1988; 49(6):944–955.
Di Spiezio Sardo A, Campo R, Gordts S, et al. The comprehen-siveness of the ESHRE/ESGE classification of female genital tract congenital anomalies: a systematic review of cases not classified by the AFS system. Human Reprod. 2015;30(5): 1046–1058
Acien P, Acien M. Diagnostic imaging and cataloguing of female genital malformations. Insights Imaging. 2016;7(5):713–726.
Graupera B, Pascual MA, Hereter L, et al. Accuracy of three-dimensional ultrasound compared with magnetic resonance imaging in diagnosis of Mullerian duct anomalies using ESHRE-ESGE consensus on the classification of congenital anomalies of the female genital tract. Ultrasound Obstet Gynecol. 2015;46(5): 616–622.
Ludwin A, Ludwin I. Comparison of the ESHRE-ESGE and ASRM classifications of Mullerian duct anomalies in everyday practice. Hum Reprod. 2016;30(3):569–580.
Practice Committee of the American Society for Reproductive Medicine. American Society for Reproductive Medicine, Birmingham, Alabama. Uterine septum: a guideline. Fertil Steril. 2016;3(3):530–540.
Veneris C, Papadopoulos S, Campo R, Gordts S, Tarlatzis B, Grimbizis G. Clinical implications of congenital uterine anoma-lies: a meta-analysis of comparative studies. BioMedicine Online. 2014;29(6):665–683.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bermejo, C., Marínez-Ten, P., Ruíz-López, L. et al. Classification of Uterine Anomalies by 3-Dimensional Ultrasonography Using ESHRE/ESGE Criteria: Interobserver Variability. Reprod. Sci. 25, 740–747 (2018). https://doi.org/10.1177/1933719117725825
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719117725825