Abstract
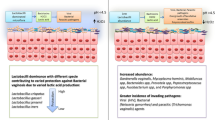
Vaginal glycogen is degraded by host α-amylase and then converted to lactic acid by Lactobacilli. This maintains the vaginal pH at ≤4.5 and prevents growth of other bacteria. Therefore, host α-amylase activity may promote dominance of Lactobacilli. We evaluated whether the α-amylase level in vaginal fluid is altered in women with bacterial vaginosis (BV) and vulvovaginal candidiasis (VVC) and whether its concentration was associated with levels of lactic acid isomers and host mediators. Vaginal fluid was obtained from 43 women with BV, 50 women with VVC, and 62 women with no vulvovaginal disorders. Vaginal fluid concentrations of α-amylase, secretory leukocyte protease inhibitor (SLPI), hyaluronan, hyaluronidase-1, β-defensin, and elafin were measured by enzyme-linked immunosorbent assay (ELISA). Vaginal concentrations of neutrophil gelatinase-associated lipocalin (NGAL), matrix metalloproteinase (MMP) 8, and d- and l-lactic acid levels in these patients were previously reported. The median vaginal fluid α-amylase level was 1.83 mU/mL in control women, 1.45 mU/mL in women with VVC, and 1.07 mU/mL in women with BV. Vaginal levels of α-amylase were correlated with d-lactic acid (P = .003) but not with l-lactic acid (P > .05) and with SLPI (P < .001), hyaluronidase-1 (P < .001), NGAL (P = .001), and MMP-8 (P = .005). The exfoliation of glycogen-rich epithelial cells into the vaginal lumen by hyaluronidase-1 and MMP-8 may increase glycogen availability and promote α-amylase activity. The subsequent enhanced availability of glycogen breakdown products would favor proliferation of Lactobacilli, the primary producers of d-lactic acid in the vagina. Concomitant production of NGAL and SLPI would retard growth of BV-related bacteria.
Similar content being viewed by others
References
Zakowski JJ, Bruns DE. Biochemistry of human alpha amylase isoenzymes. Crit Rev Clin Lab Sci. 1985;21(4):283–322.
Lee YS, Raju GC. The expression and localization of amylase in normal and malignant glands of the endometrium and endocervix. J Pathol. 1988;155(3):201–205.
Skude G, Mårdh PA, Weström L. Amylases of the genital tract. I. Isoamylases of genital tract tissue homogenates and peritoneal fluid. Am J Obstet Gynecol. 1976;126(6):652–656.
Spear GT, French AL, Gilbert D, et al. Human α-amylase present in lower-genital-tract mucosal fluid processes glycogen to support vaginal colonization by Lactobacillus. J Infect Dis. 2014;210(7): 1019–1028.
Boris S, Barbés C. Role played by lactobacilli in controlling the population of vaginal pathogens. Microbes Infect. 2000;2(5): 543–546.
Boskey ER, Cone RA, Whaley KJ, Moench TR. Origins of vaginal acidity: high D/L lactate ratio is consistent with bacteria being the primary source. Hum Reprod. 2001;16(9):1809–1813.
Linhares IM, Summers PR, Larsen B, Giraldo PC, Witkin SS. Contemporary perspectives on vaginal pH and lactobacilli. Am J Obstet Gynecol. 2011;204(2):1–5.
Cruickshank R. The biology of the vagina in the human subject. II: The bacterial flora and secretion of the vagina in relation to glycogen in the vaginal epithelium. J Obstet Gynecol Br Emp. 1934;41(2):208–226.
Mirmonsef P, Hotton AL, Gilbert D, et al. Free glycogen in vaginal fluids is associated with Lactobacillus colonization and low vaginal pH. PLoS One. 2014;9(7):e102467.
Mitchell C, Marrazzo J. Bacterial vaginosis and the cervicovaginal immune response. Am J Reprod Immunol. 2014;71(6): 555–563.
Sobel JD. Vulvovaginal candidosis. Lancet. 2007;369(9577): 1961–1971.
Zhou X, Westman R, Hickey R, et al. Vaginal microbiota of women with frequent vulvovaginal candidiasis. Infect Immun. 2009;77(9):4130–4135.
Amsel R, Totten PA, Spiegel CA, Chen KC, Eschenbach D, Holmes KK. Nonspecific vaginitis. Diagnostic criteria and microbial and epidemiologic associations. Am J Med. 1983;74(1): 14–22.
Nugent RP, Krohn MA, Hillier SL. Reliability of diagnosing bacterial vaginosis is improved by a standardized method of gram stain interpretation. J Clin Microbiol. 1991;29(2):297–301.
Beghini J, Linhares I, Giraldo P, Ledger W, Witkin S. Differential expression of lactic acid isomers, extracellular matrix metalloproteinase inducer, and matrix metalloproteinase-8 in vaginal fluid from women with vaginal disorders [published online September 8, 2014]. BJOG. 2014. doi: 10.1111/1471–0528.13072.
Beghini J, Giraldo PC, Linhares IM, Ledger WJ, Witkin SS. Regulation of neutrophil gelatinase-associated lipocalin in vaginal fluid: relation to pathogenesis [published online February 10, 2015]. Reprod Sci. 2015.
Witkin SS, Mendes-Soares H, Linhares IM, et al. Influence of vaginal bacteria and d-and l-lactic acid isomers on vaginal extracellular matrix metalloproteinase inducer: implications for protection against upper genital tract infections. MBio. 2013;4(4):e00460–13.
Boskey ER, Telsch KM, Whaley KJ, Moench TR, Cone RA. Acid production by vaginal flora in vitro is consistent with the ratio and extent of vaginal acidification. Infect Immun. 1999;67(10): 5170–5175.
Hillier SL. Diagnostic microbiology of bacterial vaginosis. Am J Obstet Gynecol. 1993;169(2 Pt 2):455–459.
Iacono KT, Brown AL, Greene MI, Saouaf SJ. CD147 immuno-globulin superfamily receptor function and role in pathology. Exp Mol Pathol. 2007;83(3):283–295.
Rampersaud R, Planet PJ, Randis TM, et al. Interolysin, a cholesterol-dependent cytolysin produced by Lactobacillus iners. J Bacteriol. 2011;193(5):1034–1041.
Simpson MA, Lokeshwar VB. Hyaluronan and hyaluronidase in genitourinary tumors. Front Biosci. 2008;13:5664–5680.
Cooper MD, Roberts MH, Barauskas OL, Jarvis GA. Secretory leukocyte protease inhibitor binds to Neisseria gonorrhoeae outer membrane opacity protein and is bactericidal. Am J Reprod Immunol. 2012;68(2):116–127.
Wiesner J, Vilcinskas A. Antimicrobial peptides: the ancient arm of the human immune system. Virulence. 2010;1(5):440–464.
Balkus J, Agnew K, Lawler R, Mitchell C, Hitti J. Effects of pregnancy and bacterial vaginosis on proinflammatory cytokine and secretory leukocyte protease inhibitor concentrations in vaginal secretions. J Pregnancy. 2010;2010:385981.
Mitchell C, Balkus J, Agnew K, Lawler R, Hitti J. Changes in the vaginal microenvironment with metronidazole treatment for bacterial vaginosis in early pregnancy. J Womens Health. 2009; 18(11):1817–1824.
Draper DL, Landers DV, Krohn MA, Hillier SL, Wiesenfeld HC, Heine RP. Levels of vaginal secretory leukocyte protease inhibitor are decreased in women with lower reproductive tract infections. Am J Obstet Gynecol. 2000;183(5): 1243–1248.
Nikolaitchouk N, Andersch B, Falsen E, Strömbeck L, Mattsby-Baltzer I. The lower genital tract microbiota in relation to cytokine-, SLPI- and endotoxin levels: application of checkerboard DNA-DNA hybridization (CDH). APMIS. 2008;116(4): 263–277.
Goetz DH, Holmes MA, Borregaard N, Bluhm ME, Raymond KN, Strong RK. The neutrophil lipocalin NGAL is a bacteriostatic agent that interferes with siderophore-mediated iron acquisition. Mol Cell. 2002;10(5):1033–1043.
Jarosik GP, Land CB, Duhon P, Chandler R Jr, Mercer T. Acquisition of iron by Gardnerella vaginalis. Infect Immun. 1998; 66(10):5041–5047.
Imbert M, Blondeau R. On the iron requirement of lactobacilli grown in chemically defined medium. Curr Microbiol. 1998;37(1):64–66.
Elli M, Zink R, Rytz A, Reniero R, Morelli L. Iron requirement of lactobacillus spp. in completely chemically defined growth media. J Appl Microbiol. 2000;88(4):695–703.
Pivarcsi A, Nagy I, Koreck A, et al. Microbial compounds induce the expression of pro-inflammatory cytokines, chemokines and human beta-defensin-2 in vaginal epithelial cells. Microbs Infect. 2005;7(9–10):1117–1127.
Curvelo JA, Barreto AL, Portela MB, et al. Effect of the secretory leukocyte proteinase inhibitor (SLPI) on Candida albicans biological processes: a therapeutic alternative?. Arch Oral Biol. 2014;59(9):928–937.
Feng Z, Jiang B, Chandra J, Ghannoum M, Nelson S, Weinberg A. Human beta-defensins: differential activeity against candida species and regulation by Candida albicans. J Dent Res. 2005; 84(5):445–450.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nasioudis, D., Beghini, J., Bongiovanni, A.M. et al. α-Amylase in Vaginal Fluid: Association With Conditions Favorable to Dominance of Lactobacillus. Reprod. Sci. 22, 1393–1398 (2015). https://doi.org/10.1177/1933719115581000
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719115581000