Abstract
Objective
This study investigated the in vitro fertilization (IVF) outcome of levonorgestrel-releasing intrauterine system (LNG-IUS) pretreatment for simple endometrial hyperplasia (EH) in patients with polycystic ovary syndrome (PCOS) undergoing IVF embryo transfer (IVF-ET).
Methods
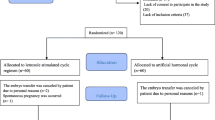
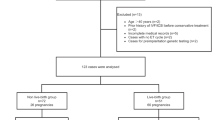
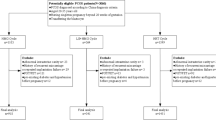
One hundred ninety patients with PCOS and simple EH without cytologic atypia were allocated randomly to 2 independent arms, that is, the LNG-IUS group (90 patients) and the non-LNG-IUS group (100 patients). Four hundred fourteen patients with PCOS without endometrial disease comprised the control group. Each patient was reevaluated by transvaginal ultrasonography (TVS) and endometrial biopsy after 6 months. For each patient, IVF outcome measures, such as number of recombinant follicle-stimulating hormone, endometrial thickness on human chorionic gonadotropin (HCG) day, hormone levels (progesterone, luetinizing hormone, and serum estradiol) on HCG day, number of oocytes, fertilization rate, clinical pregnancy rate, and miscarriage rate were compared among the 3 groups.
Results
In general, the 3 groups did not differ with respect to the main clinical and biochemical data. After 6 months, patients in LNG-IUS group had an EH resolution rate of 87.77%. In the non-LNG-IUS group, the resolution rate was 15.00%, and 3% of these patients showed progression of EH. The clinical pregnancy rates in the non-LNG-IUS group were significantly lower (28.04%) than that in the LNG-IUS group (46.06%) and the control group (44.65%). The miscarriage rate was highest in the non-LNG-IUS group, but no significant difference in miscarriage rate existed among the 3 groups.
Conclusion
The study illustrates that the LNG-IUS can be safely used for 6 months as a treatment for patients with PCOS and simple EH. Additionally, use of the LNG-IUS can increase the clinical pregnancy rates and implantation rates of patients with PCOS and simple EH who undergo gonadotropin-releasing hormone agonist IVF-ET protocols.
Similar content being viewed by others
References
Nandi A, Chen Z, Patel R, Poretsky L. Polycystic ovary syndrome. Endocrinol Metab Clin North Am. 2014;43(1):123–147.
Qiao J, Wang L, Li R, Zhang X. Microarray evaluation of endometrial receptivity in Chinese women with polycystic ovary syndrome. Reprod Biomed Online. 2008;17(3):425–435.
Cakmak H, Taylor HS. Human implantation failure: molecular mechanisms and clinical treatment. Hum Reprod Update. 2011; 17(2):242–253.
Panidis D, Tziomalos K, Papadakis E, Katsikis I. Infertility treatment in polycystic ovary syndrome: lifestyle interventions, medications and surgery. Front Horm Res. 2013;40:128–141.
Brezina PR, Mensah V, Balen A, et al. J Assist Reprod Genet. Fertility management in the PCOS population: results of a webbased survey at IVF-worldwide.com. J Assist Reprod Genet. 2013;30(9):1169–1174.
Junk SM, Yeap D. Improved implantation and ongoing pregnancy rates after single-embryo transfer with an optimized protocol for in vitro oocyte maturation in women with polycystic ovaries and polycystic ovary syndrome. Fertil Steril. 2012;98(4):888–892.
Coughlan C, Yuan X, Nafee T, Yan J, Mariee N, Li TC. The clinical characteristics of women with recurrent implantation failure. J Obstet Gynaecol. 2013;33(5):494–498
Cheung AP. Ultrasound and menstrual history in predicting endometrial hyperplasia in polycystic ovary syndrome. Obstet Gynecol. 2001;98(2):325–331.
Park JC, Lim SY, Jang TK, Bae JG, Kim JI, Rhee JH. Endometrial histology and predictable clinical factors for endometrial disease in women with polycystic ovary syndrome. Clin Exp Reprod Med. 2011;38(1):42–46.
Kurman RJ, Kaminski PF, Norris HJ. The behavior of endometrial hyperplasia. A long-term study of ‘untreated’ hyperplasia in 170 patients. Cancer. 1985;56(2):403–412.
Ip PP, Irving JA, McCluggage WG, Clement PB, Young RH. Papillary proliferation of the endometrium: a clinicopathologic study of 59 cases of simple and complex papillae without cytologic atypia. Am J Surg Pathol. 2013;37(2):167–177.
Goncharenko VM, Beniuk VA, Kalenska OV, Demchenko OM, Spivak MY, Bubnov RV. Predictive diagnosis of endometrial hyperplasia and personalized therapeutic strategy in women of fertile age. EPMA J. 2013;4(1):24–36.
Rakha E, Wong SC, Soomro I, et al. Clinical outcome of atypical endometrial hyperplasia diagnosed on an endometrial biopsy: institutional experience and review of literature. Am J Surg Pathol. 2012;36(11):1683–1690.
Haimovich S, Checa MA, Mancebo G, Fusté P, Carreras R. Treatment of endometrial hyperplasia without atypia in perimenopausal and postmenopausal women with a levonorgestrel intrauterine device. Menopause. 2008;15(5):1002–1004.
Anastasiadis PG, Skaphida PG, Koutlaki NG, Galazios GC, Tsikouras PN, Liberis VA. Descriptive epidemiology of endometrial hyperplasia in patients with abnormal uterine bleeding. Eur J Gynaecol Oncol. 2000;21(2):131–134.
Haoula ZJ, Walker KF, Powell MC. Levonorgestrel intra-uterine system as a treatment option for complex endometrial hyperplasia. Eur J Obstet Gynecol Reprod Biol. 2011;159(1):176–179.
Bese T, Vural A, Ozturk M, et al. The effect of long-term use of progesterone therapy on proliferation and apoptosis in simple endometrial hyperplasia without atypia. Int J Gynecol Cancer. 2006;16(2):809–813.
Gallos ID, Ganesan R, Gupta JK. Prediction of regression and relapse of endometrial hyperplasia with conservative therapy. Obstet Gynecol. 2013;121(6):1165–1171.
Rattanachaiyanont M, Angsuwathana S, Techatrisak K, Tanmahasamut P, Indhavivadhana S, Leerasiri P. Clinical and pathological responses of progestin therapy for non-atypical endometrial hyperplasia: a prospective study. J Obstet Gynaecol Res. 2005; 31(2):98–106.
Hurskainen R, Teperi J, Rissanen P, et al. Clinical outcomes and costs with the levonorgestrel-releasing intrauterine system or hysterectomy for treatment of menorrhagia: randomized trial 5-year follow-up. JAMA. 2004;291(12):1456–1463.
Nilsson CG, Haukkamaa M, Vierola H, Luukkainen T. Tissue concentrations of levonorgestrel in women using a levonorgestrel-releasing IUD. Clin Endocrinol. 1982;17(6): 529–536.
Ercan CM, Duru NK, Sakinci M, Alanbay I, Karasahin KE, Baser I. Successful twin pregnancy achieved by assisted reproductive technology in a patient with polycystic ovary syndrome with complex atypical endometrial hyperplasia treated with levonorgestrel-releasing intrauterine system. Gynecol Endocrinol. 2010;26(2): 125–128.
Kristensen SL, Ramlau-Hansen CH, Ernst E, et al. A very large proportion of young Danish women have polycystic ovaries: is a revision of the Rotterdam criteria needed? Hum Reprod. 2010; 25(12):3117–3122.
Sakamoto C. Sonographic criteria of phasic changes in human endometrial tissue. Int J Gynaecol Obstet. 1985;23(1):7–12.
McCormick BA1, Wilburn RD, Thomas MA, Williams DB, Maxwell R, Aubuchon M. Endometrial thickness predicts endometrial hyperplasia in patients with polycystic ovary syndrome. Fertil Steril. 2011;95(8):2625–2627.
Espindola D, Kennedy KA, Fischer EG. Management of abnormal uterine bleeding and the pathology of endometrial hyperplasia. Obstet Gynecol Clins N Am. 2007;34(4):717–737.
Moher D, Schultz KF, Altman DG, and CONSORT Group (Consolidated Standards of Reporting Trials). The CONSORT statement: revised recommendations for improving the quality of reports of parallel group randomised trials. Lancet. 2001; 357(9263):1191–1194.
Vermeulen A, Verdonck L, Kaufman JM. A critical evaluation of simple methods for the estimation of free testosterone in serum. J Clin Endocrinol Metab. 1999:84(10):3666–3672.
Puissant F, Van Rysselberge M, Barlow P, Deweze J, Leroy F. Embryo scoring as a prognostic tool in IVF treatment. Hum Reprod. 1987;2(8):705–708.
Giudice LC. Endometrium in PCOS: implantation and predisposition to endocrine CA. Best Pract Res Clin Endocrinol Metab. 2006;20(2):235–244.
Pillay OC, Te Fong LF, Crow JC, et al. The association between polycystic ovaries and endometrial cancer. Hum Reprod. 2006; 21(4):924–929.
Yan L, Wang A, Chen L, Shang W, Li M, Zhao Y. Expression of apoptosis-related genes in the endometrium of polycystic ovary syndrome patients during the window of implantation. Gene. 2012;506(2):350–354.
Ozkaya E, Korkmaz V, Ozkaya Y, Tosun A, Küçükozkan T, Bostan H. Ultrasonographic endometrial thickness measurement is predictive for treatment response in simple endometrial hyperplasia without atypia. J Turk Ger Gynecol Assoc. 2013;14(1): 19–22.
Breijer MC1, Peeters JA, Opmeer BC, et al. Capacity of endometrial thickness measurement to diagnose endometrial carcinoma in asymptomatic postmenopausal women: a systematic review and meta-analysis. Ultrasound Obstet Gynecol. 2012; 40(6):621–629.
Tingthanatikul Y, Choktanasiri W, Rochanawutanon M, Weerakeit S. Prevalence and clinical predictors of endometrial hyperplasia in anovulatory women presenting with amenorrhea. Gynecol Endocrinol. 2006;22(2):101–105.
Gruboeck K, Jurkovic D, Lawton F, Savvas M, Tailor A, Campbell S. The diagnostic value of endometrial thickness and volume measurements by three-dimensional ultrasound in patients with postmenopausal bleeding. Ultrasound Obstet Gynecol. 1996; 8(4):272–276.
Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group. Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod. 2004;19(1):41–47.
Soliman PT, Oh JC, Schmeler KM, et al. Risk factors for young premenopausal women with endometrial cancer. Obstet Gynecol. 2005;105(3):575–580.
Thigpen JT, Brady MF, Alvarez RD, et al. Oral medroxyprogesterone acetate in the treatment of advanced or recurrent endometrial carcinoma: a dose-response study by the Gynecologic Oncology Group. J Clin Onco. 1999;17(6):1736–1744.
Dhar KK, NeedhiRajan T, Koslowski M, Woolas RP. Is levonorgestrel intrauterine system effective for treatment of early endometrial cancer? Report of four cases and review of the literature. Gynecol Oncol. 2005;97(3):924–927.
Wildemeersch D, Janssens D, Pylyser K, et al. Management of patients with non-atypical and atypical endometrial hyperplasia with a levonorgestrel-releasing intrauterine system: long-term follow-up. Maturitas. 2007;57(2):210–213.
Orbo A, Arnes M, Hancke C, Vereide AB, Pettersen I, Larsen K. Treatment results of endometrial hyperplasia after prospective D-score classification: a follow-up study comparing effect of LNG-IUD and oral progestins versus observation only. Gynecol Oncol. 2008;111(1):68–73.
Varma R, Soneja H, Bhatia K, et al. The effectiveness of a levonorgestrel-releasing intrauterine system (LNG-IUS) in the treatment of endometrial hyperplasia: a long-term follow-up study. Eur J Obstet Gynecol Reprod Biol. 2008;139(2):169–175.
Vereide AB, Kaino T, Sager G, Arnes M, Orbo A. Effect of levonorgestrel IUD and oral medroxyprogesterone acetate on glandular and stromal progesterone receptors (PRA and PRB), and estrogen receptors (ER-alpha and ER-beta) in human endometrial hyperplasia. Gynecol Oncol. 2006;101(2):214–223.
Vereide AB, Arnes M, Straume B, Maltau JM, Orbo A. Nuclear morphometric changes and therapy monitoring in patients with endometrial hyperplasia: a study comparing effects of intrauterine levonorgestrel and systemic medroxyprogesterone. Gynecol Oncol. 2003;91(3):526–533.
Nilsson CG, Haukkamaa M, Vierola H, Luukkainen T. Tissue concentrations of levonorgestrel in women using a levonorgestrel-releasing IUD. Clin Endocrinol (Oxf). 1982;17(6):529–536.
Orbo A, Vereide A, Arnes M, Pettersen I, Straume B. Levonorgestrel-impregnated intrauterine device as treatment for endometrial hyperplasia: a national multicentre randomised trial. BJOG. 2014;121(4):477–486.
Karimi-Zarchi M, Dehghani-Firoozabadi R, Tabatabaie A, et al. A comparison of the effect of levonorgestrel IUD with oral medroxyprogesterone acetate on abnormal uterine bleeding with simple endometrial hyperplasia and fertility preservation. Clin Exp Obstet Gynecol. 2013;40(3):421–424.
Chen SL, Wu FR, Luo C, Chen X, Shi XY, Zheng HY. Combined analysis of endometrial thickness and pattern in predicting outcome of in vitro fertilization and embryo transfer: a retrospective cohort study. Reprod Biol Endocrinol. 2010,8(1):30–37.
Traub ML, Arsdale AV, Pal L, Jindal S, Santoro N. Endometrial thickness, Caucasian ethnicity, and age predict clinical pregnancy following fresh blastocyst embryo transfer: a retrospective cohort. Reprod Biol Endocrinol. 2009;7(1):33–40.
Detti L, Yelian FD, Kruger ML, Diamond MP, Rode A, Mitwally MFM. Endometrial thickness is related to miscarriage rate, but not the estradiol concentration, in cycles down-regulated with gonadotropin-releasing hormone antagonist. Fertil Steril. 2008; 89(4):998–1001.
Isaacs JD Jr, Wells CS, Williams DB, Odem RR, Gast MJ, Stickler RC. Endometrial thickness is a valid monitoring parameter in cycles of ovulation induction with menotropins alone. Fertil Steril. 1996;65(2):262–266.
Weissman A, Gotlieb L, Casper RF. The detrimental effect of increased endometrial thickness on implantation and pregnancy rates and outcome in an in vitro fertilization program. Fertil Steril. 1999;71(1):147–149.
Ke RW. Endocrine basis for recurrent pregnancy loss. Obstet Gynecol Clin North Am. 2014;41(1):103–112.
Palomba S, Falbo A, La Sala GB. Effects of metformin in women with polycystic ovary syndrome treated with gonadotrophins for in vitro fertilisation and intracytoplasmic sperm injection cycles: a systematic review and meta-analysis of randomised controlled trials. BJOG. 2013;120(3):267–276.
Siristatidis CS, Maheshwari A, Bhattacharya S. In vitro maturation in sub fertile women with polycystic ovarian syndrome under-going assisted reproduction. Cochrane Database Syst Rev. 2009;(1):CD006606.
Griesinger G, Diedrich K, Tarlatzis BC, Kolibianakis EM. GnRH-antagonists in ovarian stimulation for IVF in patients with poor response to gonadotrophins, polycystic ovary syndrome, and risk of ovarian hyperstimulation: a meta-analysis. Reprod Biomed Online. 2006;13(5):628–638.
MacDougall MJ, Tan SL, Balen A, Jacobs HS. A controlled study comparing patients with and without polycystic ovaries undergoing in-vitro fertilization. Hum Reprod. 1993;8(2):233–237.
Daya S. Gonadotropin releasing hormone agonist protocols for pituitary desensitization in in vitro fertilization and gamete intrafallopian transfer cycles. Cochrane Database Syst Rev. 2000;(2): CD001299.
Conn PM, Staley D, Harris C, Andrews WV, Gorospe WC, McArdle CA. Mechanism of action of gonadotropin releasing hormone. Annu Rev Physiol. 1986;48(3):495–513.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bian, J., Shao, H., Liu, H. et al. Efficacy of the Levonorgestrel-Releasing Intrauterine System on IVF-ET Outcomes in PCOS With Simple Endometrial Hyperplasia. Reprod. Sci. 22, 758–766 (2015). https://doi.org/10.1177/1933719114561553
Published:
Issue Date:
DOI: https://doi.org/10.1177/1933719114561553