Abstract
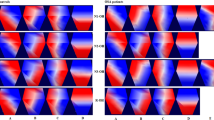
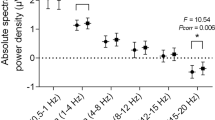
Obstructive sleep apnea (OSA) is a very serious and multifactorial sleep disorder that is closely related to the disruption of sleep homeostasis. It is known that such sleep encephalographic (EEG) phenomenon as sleep spindles (SSs) supports sleep stability and may display a sleep protective function. Thus, it is of particular interest to assess the SS pattern in OSA patients, which is the aim of the present research. We investigated whether SS activity could be altered in patients with moderate degree of OSA compared with non-OSA subjects. Twenty-nine meddle-aged OSA patients (26 male and 3 female) and 26 controls underwent full-night polysomnography (PSG). SSs were automatically detected during stage 2 (N2) of non-rapid eye movements. The SS activity characteristics involved total number, mean density, mean maximum amplitude, and mean frequency. All differences were considered statistically significant at p < 0.05. We noted a significant decrease in the density and number of central SSs in patients with OSA compared to controls; however, the amplitude is significantly higher in OSA subjects. To summarize, our results show that OSA leads to significant disruption of SS density, reduction of their number, and frequency in N2 sleep stages. These findings can be evidence of the extinction of a brain protective mechanism against exciting stimuli during apnea episodes in OSA patients with a long duration of sleep disturbances.
Similar content being viewed by others
Data availability
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
References
C. Guilleminault, W.C. Demen, Sleep Apnoea Syndromes (Liss Inc, 1978), p.374
A.M. Vein, T.S. Eligulashvili, M.G. Poluektov, Sleep Apnea Syndrome and Other Sleep-Related Breathing Disorders: Clinical Picture, Diagnosis, Treatment (M. Eidos Media, 2002), p.310
J.J. Lee, K.M. Sundar, Evaluation and management of adults with obstructive sleep apnea syndrome. Lung (2021). https://doi.org/10.1007/s00408-021-00426-w
P.E. Peppard, T. Young, J.H. Barnet, M. Palta, E.W. Hagen, K.M. Hla, Increased prevalence of sleep-disordered breathing in adults. Am. J. Epidemiol. 177(9), 1006–1014 (2013). https://doi.org/10.1093/aje/kws342
J.M. Dzierzewski, N. Dautovich, S. Ravyts, Sleep and cognition in older adults. Sleep Med. Clin. 13(1), 93–106 (2018). https://doi.org/10.1016/j.jsmc.2017.09.009
R.M. Benca, M. Teodorescu, Sleep physiology and disorders in aging and dementia. Handb. Clin. Neurol. 167, 477–493 (2019). https://doi.org/10.1016/B978-0-12-804766-8.00026-1
A.E. Mullins, K. Kam, A. Parekh, O.M. Bubu, R.S. Osorio, A.W. Varga, Obstructive sleep apnea and its treatment in aging: effects on Alzheimer’s disease biomarkers, cognition, brain structure and neurophysiology. Neurobiol. Dis.. Dis. 145, 105054 (2020). https://doi.org/10.1016/j.nbd.2020.105054
E.B. Ukhinov, I.M. Madaeva, O.N. Berdina, L.V. Rychkova, L.I. Kolesnikova, S.I. Kolesnikov, Features of the EEG pattern of sleep spindles and its diagnostic significance in ontogeny. Bull. Exp. Biol. Med. 173(4), 399–408 (2022)
C. Iber, S. Ancoli-Israel, A. Chesson, S.F. Quan, The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology, and Technical Specification (American Academy of Sleep Medicine, Westchester, IL, 2007)
S. Astori, R.D. Wimmer, A. Lüthi, Manipulating sleep spindles expanding views on sleep, memory, and disease. Trends Neurosci. 36(12), 738–748 (2013). https://doi.org/10.1016/j.tins.2013.10.001
M. Vardanian, L. Ravdin, Cognitive complaints and comorbidities in obstructive sleep apnea. Sleep Med. Clin. 17(4), 647–656 (2022). https://doi.org/10.1016/j.jsmc.2022.07.009
D.Z. Carvalho, G.J. Gerhardt Dellagustin, E.L. de Santa-Helena, N. Lemke, A.Z. Segal, S.V. Schönwald, Loss of sleep spindle frequency deceleration in obstructive sleep apnea. Clin. Neurophysiol. 125, 306–312 (2014). https://doi.org/10.1016/j.clinph.2013.07.005
C. Davies, J. Harrington, Impact of obstructive sleep apnea on neurocognitive function and impact of continuous positive air pressure. Sleep Med. Clin. V11(3), 287–298 (2016). https://doi.org/10.1016/j.jsmc.2016.04.006
I. Madaeva, O. Berdina, L. Rychkova, O. Bugun, Sleep spindle characteristics in overweight adolescents with obstructive sleep apnea syndrome. Sleep Biol. Rhythms 15(3), 251–257 (2017). https://doi.org/10.1007/s41105-017-0104-z
O. Berdina, I. Madaeva, S. Bolshakova, E. Ukhinov, L. Sholokhov, L. Rychkova, Sleep EEG oscillation associations with plasma amyloid-β42 in apneic adolescents: a cross section study. Eur. Phys. J. Spec. Top. 232, 547–555 (2023). https://doi.org/10.1140/epjs/s11734-023-00777-w
American Academy of Sleep Medicine, International classification of sleep disorders, in Diagnostic and Coding Manual, 3rd edn. (Darien, IL, American Academy of Sleep Medicine, 2014). https://doi.org/10.1007/978-1-4939-6578-6_27
V.K. Kapur, D.H. Auckley, S. Chowdhuri, D.C. Kuhlmann, R. Mehra, K. Ramar, C.G. Harrod, Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American academy of sleep medicine clinical practice guideline. J. Clin. Sleep Med. 13(3), 479–504 (2017). https://doi.org/10.5664/jcsm.6506
R.B. Berry, R. Budhiraja, D.J. Gottlieb et al., Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the sleep apnea definitions task force of the American academy of sleep medicine. J. Clin. Sleep Med.Clin Sleep Med. 8(05), 597–619 (2012). https://doi.org/10.5664/jcsm.2172
S.M. Fogel, C.T. Smith, The function of the sleep spindle: a physiological index of intelligence and a mechanism for sleep-dependent memory consolidation. Neurosci. Biobehav. Rev. 35(5), 1154–1165 (2011). https://doi.org/10.1016/j.neubiorev.2010.12.003
L.M.J. Fernandez, A. Lüthi, Sleep spindles: mechanisms and functions. Physiol. Rev. 100(2), 805–868 (2020). https://doi.org/10.1152/physrev.00042.2018
I.M. Madaeva, O.N. Berdina, N.V. Semenova, L.I. Kolesnikova, Evaluation of the structural organization of sleep in obstructive apnea syndrome from the perspective of modern pathophysiology. Zhurnal Nevrol Psikhiatrii imeni S.S. Korsakova 120(92), 80–84 (2020). https://doi.org/10.17116/jnevro202012009280. (in Russian)
I.M. Madaeva, N.A. Kurashova, N.V. Semenova, E.B. Ukhinov, O.N. Berdina, T.A. Bairova, A.V. Belskikh, L.I. Kolesnikova, S.I. Kolesnikov, Obstructive sleep apnea syndrome: association of serum melatonin, increased daytime sleepiness, and intermitting night hypoxemia. Pulmonologiya 31(6), 768–775 (2021). https://doi.org/10.18093/0869-0189-2021-31-6-768-775. (in Russian)
I.M. Madaeva, O.N. Berdina, N.A. Kurashova et al., Sleep apnea and serum serotonin level pre- and post-PAP therapy: a preliminary study. Neurol Ther 10, 1095–1102 (2021). https://doi.org/10.1007/s40120-021-00290-z
S.V. Schönwald, D.Z. Carvalho, E.L. de Santa-Helena, N. Lemke, G.J. Gerhardt, Topography-specific spindle frequency changes in obstructive sleep apnea. BMC Neurosci. 31(13), 89 (2012). https://doi.org/10.1186/1471-2202-13-89.PMID:22985414;PMCID:PMC3496607
W. Li, Y. Duan, J. Yan, H. Gao, X. Li, Association between loss of sleep-specific waves and age, sleep efficiency, body mass index, and apnea-hypopnea index in human N3 sleep. Aging Dis. 11, 73–81 (2020). https://doi.org/10.14336/AD.2019.0420
H. Mohammadi, A. Aarabi, M. Rezaei, H. Khazaie, S. Brand, Sleep spindle characteristics in obstructive sleep apnea syndrome (OSAS). Front. Neurol. 25(12), 598632 (2021). https://doi.org/10.3389/fneur.2021.598632
S.L. Himanen, J. Virkkala, E. Huupponen, J. Hasan, Spindle frequency remains slow in sleep apnea patients throughout the night. Sleep Med. 4(4), 361–366 (2003). https://doi.org/10.1016/s1389-9457(03)00155-2
E. Huupponen, S.L. Himanen, J. Hasan, A. Värri, Automatic analysis of electro-encephalogram sleep spindle frequency throughout the night. Med. Biol. Eng. Comput. 41(6), 727–732 (2003). https://doi.org/10.1007/BF02349981
V. Guadagni, H. Byles, A.V. Tyndall, J. Parboosingh, R.S. Longman, D.B. Hogan, P.J. Hanly, M. Younes, M.J. Poulin, Association of sleep spindle characteristics with executive functioning in healthy sedentary middle-aged and older adults. J. Sleep Res. 30(2), e13037 (2021). https://doi.org/10.1111/jsr.13037
Y. Ozkan, A. Deniz, Effect of CPAP on sleep spindles in patients with OSA. Respir. Physiol. Neurobiol. 247, 71–73 (2018). https://doi.org/10.1016/j.resp.2017.09.008
O.M. Weiner, T.T. Dang-Vu, Spindle oscillations in sleep disorders: a systematic review. Neural Plast.Plast. 2016, 1–30 (2016). https://doi.org/10.1155/2016/7328725
R.G. Averkin, V. Szemenyei, S. Bordé, G. Tamás, Identified Cellular correlates of neocortical ripple and high-gamma oscillations during spindles of natural sleep. Neuron 92(4), 916–928 (2016). https://doi.org/10.1016/j.neuron.2016.09.032
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparation, data collection, and analysis were performed by IM, OB, ET, and LK. The first draft of the manuscript was written by IM, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No financial or nonfinancial interests and funding.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Madaeva, I., Berdina, O., Titova, E. et al. Pattern of “sleep spindles” in obstructive sleep apnea patients. Eur. Phys. J. Spec. Top. (2023). https://doi.org/10.1140/epjs/s11734-023-01049-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1140/epjs/s11734-023-01049-3