Abstract
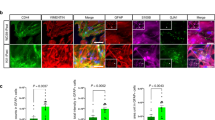
L-Aminoadipic acid (L-AA) is known to have toxic effects on astroglia. The purpose of the work is to characterize the morphological changes in astrocytes in vitro and in vivo under the influence of L-AA. The effect of L-AA in the concentration range 0.17–1.4 mM on astrocytes was evaluated in primary dissociated cultures of the rat cerebral cortex and cerebellum, as well as upon stereotaxic injection (20 μg) into the striatum of rats. Concentrations of 0.35–1.4 mM L-AA caused a decrease in the expression of acidic glyofibrillar protein (GFAP), damage and death of astrocytes, pyknosis, and activation of lysosomes (increased LAMP2 expression). On the second day after the injection of L-AA into the striatum of rats, an extensive lesion area devoid of GFAP-positive staining was formed. The data obtained showed that the use of L-aminoadipic acid is promising for modeling damage to astroglia in neurodegenerative diseases.



Similar content being viewed by others
REFERENCES
Anderson, M.A., Burda, J.E., Ren, Y., Ao, Y., O’Shea, T.M., Kawaguchi, R., Coppola, G., Khakh, B.S., Deming, T.J., and Sofroniew, M.V., Astrocyte scar formation aids central nervous system axon regeneration, Nature, 2016, vol. 532, p. 195.
Banasr, M. and Duman, R.S., Glial loss in the prefrontal cortex is sufficient to induce depressive-like behaviors, Biol. Psychiatry, 2008, vol. 64, p. 863.
Billet, F., Costentin, J., and Dourmap, N., Influence of glial cells in the dopamine releasing effect resulting from the stimulation of striatal δ-opioid receptors, Neuroscience, 2007, vol. 150, p. 131.
Brown, D.R. and Kretzschmar, H.A., The glio-toxic mechanism of alpha-aminoadipic acid on cultured astrocytes, J. Neurocytol., 1998, vol. 27, p. 109.
Buffo, A. and Rossi, F., Origin, lineage and function of cerebellar glia, Prog. Neurobiol., 2013, vol. 109, p. 42.
Buffo, A., Rite, I., Tripathi, P., Lepier, A., Colak, D., Horn, A.-P., Mori, T., and Götz, M., Origin and progeny of reactive gliosis: a source of multipotent cells in the injured brain, Proc. Natl. Acad. Sci. U. S. A., 2008, vol. 105, p. 3581.
Cerrato, V., Parmigiani, E., Figueres-Oñate, M., Betizeau, M., Aprato, J., Nanavaty, I., Berchialla, P., Luzzati, F., de’Sperati, C., López-Mascaraque, L., and Buffo, A., Multiple origins and modularity in the spatiotemporal emergence of cerebellar astrocyte heterogeneity, PLoS Biol., 2018, vol. 16, e2005513. https://doi.org/10.1371/journal.pbio.2005513
Chang, Y.F., Cauley, R.K., Chang, J.D., and Rao, V.V., L‑Alpha-aminoadipate inhibits kynurenate synthesis in rat brain hippocampus and tissue culture, Neurochem. Res., 1997, vol. 22, p. 825.
Chiu, C.-D., Yao, N.-W., Guo, J.-H., Shen, C.-C., Lee, H.-T., Chiu, Y.-P., Ji, H.-R., Chen, X., Chen, C.-C., and Chang, C., Inhibition of astrocytic activity alleviates sequela in acute stages of intracerebral hemorrhage, Oncotarget, 2017, vol. 8, p. 94850.
da Silva, J.C., Amaral, A.U., Cecatto, C., Wajner, A., dos Santos Godoy, K., Ribeiro, R.T., de Mello Gonçalves, A., Zanatta, Â., da Rosa, M.S., Loureiro, S.O., Vargas, C.R., Leipnitz, G., de Souza, D.O.G., and Wajner, M., α-Ketoadipic acid and α-aminoadipic acid cause disturbance of glutamatergic neurotransmission and induction of oxidative stress in vitro in brain of adolescent rats, Neurotox. Res., 2017, vol. 32, p. 276.
Faiz, M., Sachewsky, N., Gascón, S., Bang, K.W.A., Morshead, C.M., and Nagy, A., Adult neural stem cells from the subventricular zone give rise to reactive astrocytes in the cortex after stroke, Cell. Stem Cell, 2015, vol. 17, p. 624.
Ge, W.-P., Miyawaki, A., Gage, F.H., Jan, Y.N., and Jan, L.Y., Local generation of glia is a major astrocyte source in postnatal cortex, Nature, 2012, vol. 484, p. 376.
Hayakawa, K., Nakano, T., Irie, K., Higuchi, S., Fujioka, M., Orito, K., Iwasaki, K., Jin, G., Lo, E.H., Mishima, K., and Fujiwara, M., Inhibition of reactive astrocytes with fluorocitrate retards neurovascular remodeling and recovery after focal cerebral ischemia in mice, J. Cereb. Blood. Flow. Metab., 2010, vol. 30, p. 871.
Huck, S., Grass, F., and Hortnagl, H., The glutamate analogue alpha-aminoadipic acid is taken up by astrocytes before exerting its gliotoxic effect in vitro, J. Neurosci., 1984, vol. 4, p. 2650.
Iglesias, J., Morales, L., and Barreto, G.E., Metabolic and inflammatory adaptation of reactive astrocytes: role of PPARs, Mol. Neurobiol., 2017, vol. 54, p. 2518. https://doi.org/10.1007/s12035-016-9833-2
Jäkel, S. and Dimou, L., Glial cells and their function in the adult brain: a journey through the history of their ablation, Front. Cell. Neurosci., 2017, vol. 11. https://doi.org/10.3389/fncel.2017.00024
Katsouri, L., Birch, A.M., Renziehausen, A.W.J., Zach, C., Aman, Y., Steeds, H., Bonsu, A., Palmer, E.O.C., Mirzaei, N., Ries, M., and Sastre, M., Ablation of reactive astrocytes exacerbates disease pathology in a model of Alzheimer’s disease, Glia, 2020, vol. 68, p. 1017.
Khaspekov, L.G. and Frumkina, L.E., Molecular mechanisms mediating involvement of glial cells in plastic brain reorganization in epilepsy, Biochemistry, 2017, vol. 18, no. 3, p. 528.
Khurgel, M., Koo, A.C., and Ivy, G.O., Selective ablation of astrocytes by intracerebral injections of α-aminoadipate, Glia, 1996, vol. 16, p. 351.
Kuter, K., Olech, Ł., Głowacka, U., and Paleczna, M., Astrocyte support is important for the compensatory potential of the nigrostriatal system neurons during early neurodegeneration, J. Neurochem., 2019, vol. 148, p. 63.
Lee, H.J., Jang, H.B., Kim, W.H., Park, K.J., Kim, K.Y., Park, S.I., and Lee, H.J., 2-Aminoadipic acid (2-AAA) as a potential biomarker for insulin resistance in childhood obesity, Sci. Rep., 2019, vol. 9, p. 13610. https://doi.org/10.1038/s41598-019-49578-z
Liu, F., Dai, S., Feng, D., Peng, X., Qin, Z., Kearns, A.C., Huang, W., Chen, Y., Ergün, S., Wang, H., Rappaport, J., Bryda, E.C., Chandrasekhar, A., Aktas, B., Hu, H., et al., Versatile cell ablation tools and their applications to study loss of cell functions, Cell. Mol. Life Sci., 2019, vol. 76, p. 4725.
Madadi, S., Pasbakhsh, P., Tahmasebi, F., Mortezaee, K., Khanehzad, M., Boroujeni, F.B., Noorzehi, G., and Kashani, I.R., Astrocyte ablation induced by L-α-aminoadipate (L-AAA) potentiates remyelination in a cuprizone demyelinating mouse model, Metab. Brain Dis., 2019, vol. 34, p. 593.
McConnell, H.L., Li, Z., Woltjer, R.L., and Mishra, A., Astrocyte dysfunction and neurovascular impairment in neurological disorders: correlation or causation?, Neurochem. Int., 2019, vol. 128, p. 70.
Morales, I., Sanchez, A., Rodriguez-Sabate, C., and Rodriguez, M., Striatal astrocytes engulf dopaminergic debris in Parkinson’s disease: a study in an animal model, PLoS One, 2017, vol. 12, e0185989. https://doi.org/10.1371/journal.pone.0185989
Morizawa, Y.M., Hirayama, Y., Ohno, N., Shibata, S., Shigetomi, E., Sui, Y., Nabekura, J., Sato, K., Okajima, F., Takebayashi, H., Okano, H., and Koizumi, S., Reactive astrocytes function as phagocytes after brain ischemia via A-BCA1-mediated pathway, Nat. Commun., 2017, vol. 8, p. 28. https://doi.org/10.1038/s41467-017-00037-1
Nishimura, R.N., Santos, D., Fu, S.T., and Dwyer, B.E., Induction of cell death by L-alpha-aminoadipic acid exposure in cultured rat astrocytes: relationship to protein synthesis, Neurotoxicology, 2000, vol. 21, p. 313.
O’Neill, E., Chiara Goisis, R., Haverty, R., and Harkin, A., L-alpha-aminoadipic acid restricts dopaminergic neurodegeneration and motor deficits in an inflammatory model of Parkinson’s disease in male rats, J. Neurosci. Res., 2019, vol. 97, p. 804.
Olney, J.W., de Gubareff, T., and Collins, J.F., Stereospecificity of the gliotoxic and anti-neurotoxic actions of alpha-aminoadipate, Neurosci. Lett., 1980, vol. 19, p. 277.
Pekny, M. and Pekna, M., Reactive gliosis in the pathogenesis of CNS diseases, Biochim. Biophys. Acta, 2016, vol. 1862, p. 483.
Pow, D.V., Visualising the activity of the cystine-glutamate antiporter in glial cells using antibodies to aminoadipic acid, a selectively transported substrate, Glia, 2001, vol. 34, p. 27.
Qin, A.P., Liu, C.F., Qin, Y.Y., Hong, L.Z., Xu, M., Yang, L., Liu, J., Qin, Z.H., and Zhang, H.L., Autophagy was activated in injured astrocytes and mildly decreased cell survival following glucose and oxygen deprivation and focal cerebral ischemia, Autophagy, 2010, vol. 6, p. 738.
Saffran, B.N. and Crutcher, K.A., Putative gliotoxin, α‑aminoadipic acid, fails to kill hippocampal astrocytes in vivo, Neurosci. Lett., 1987, vol. 81, p. 215.
Śmiałowska, M., Szewczyk, B., Woźniak, M., Wawrzak-Wleciał, A., and Domin, H., Glial degeneration as a model of depression, Pharmacol. Rep., 2013, vol. 65, p. 1572.
Sofroniew, M.V., Molecular dissection of reactive astrogliosis and glial scar formation, Trends Neurosci., 2009, vol. 32, p. 638. https://doi.org/10.1016/j.tins.2009.08.002
Stavrovskaya, A.V., Voronkov, D.N., Ol’shansky, A.S., Gushchina, A.S., and Yamshchikova, N.G., Experimental parkinsonism in modeling striatal astrocyte damage, Annaly Klin. Eksp. Nevrol., 2019, vol. 13, no. 3, p. 28.
Takeda, M., Takamiya, A., Jiao, J.W., Cho, K.S., Trevino, S.G., Matsuda, T., and Chen, D.F., Alpha-aminoadipate induces progenitor cell properties of Müller glia in adult mice, Investig. Opthalmol. Vis. Sci., 2008, vol. 49, p. 1142. https://doi.org/10.1167/iovs.07-0434
Tang, G., Yue, Z., Talloczy, Z., and Goldman, J.E., Adaptive autophagy in Alexander disease-affected astrocytes, Autophagy, 2008, vol. 4, p. 701.
Verkhratsky, A. and Nedergaard, M., Physiology of astroglia, Physiol. Rev., 2018, vol. 98, p. 239.
Wang, J.-L. and Xu, C.-J., Astrocytes autophagy in aging and neurodegenerative disorders, Biomed. Pharmacother., 2020, vol. 122, p. 109691. https://doi.org/10.2147/DDDT.S105362
Wang, T.J., Ngo, D., Psychogios, N., Dejam, A., Larson, M.G., Vasan, R.S., Ghorbani, A., O’Sullivan, J., Cheng, S., Rhee, E.P., Sinha, S., McCabe, E., Fox, C.S., O’Donnell, C.J., Ho, J.E., et al., 2-Aminoadipic acid is a biomarker for diabetes risk, J. Clin. Invest., 2013, vol. 123, p. 4309.
Wang, X., Su, J., Ding, J., et al., α-Aminoadipic acid protects against retinal disruption through attenuating Muller cell gliosis in a rat model of acute ocular hypertension, Drug Des. Devel. Ther., 2016, vol. 10, p. 3449.
Watmuff, B., Berkovitch, S.S., Huang, J.H., Iaconelli, J., Toffel, S., and Karmacharya, R., Disease signatures for schizophrenia and bipolar disorder using patient-derived induced pluripotent stem cells, Mol. Cell Neurosci., 2016, vol. 73, p. 96.
West, E.L., Pearson, R.A., Tschernutter, M., Sowden, J.C., MacLaren, R.E., and Ali, R.R., Pharmacological disruption of the outer limiting membrane leads to increased retinal integration of transplanted photoreceptor precursors, Exp. Eye Res., 2008, vol. 86, p. 601.
Funding
The work was carried out at the expense of budgetary funding of the Federal State Budgetary Scientific Institution Scientific Center of Neurology within the framework of a state assignment.
Author information
Authors and Affiliations
Contributions
Research concept and design—D.N. Voronkov, Yu.V. Dikalova; analysis and interpretation of data— R.M. Khudoerkov, Voronkov D.N., Dikalova Yu.V.; holding experiment and material processing—A.A. Lyzhin, D.N. Voronkov, Yu.V. Dikalova, A.V. Stavrovskaya; statistical processing—D.N. Voronkov, Yu.V. Dikalova; writing work—D.N. Voronkov, R.M. Khudoerkov, Yu.V. Dikalova, L.G. Khaspekov; final editing of the text—R.M. Khudoerkov, L.G. Khaspekov, Yu.V. Dikalova.
Corresponding author
Ethics declarations
Conflict of interest. The authors declare that they have no conflicts of interest.
Statement on the welfare of animals. Manipulations with animals were carried out in accordance with regulatory documents (Principles Good Laboratory Practice 2009, GOST R 53434-200 and EU recommendations “Euthanasia of experimental animals,” 1997, ISBN 92-827-9694-9). The number of the decision of the local ethics committee no. 2-5/19 from February 20, 2019.
Additional information
Abbreviations: GFAP—acidic glyofibrillar protein, L-AA—L‑aminoadipic acid.
Rights and permissions
About this article
Cite this article
Voronkov, D.N., Lyzhin, A.A., Dikalova, Y.V. et al. Features of Brain Astrocyte Damage under the Influence of L-Aminoadipic Acid In Vitro and In Vivo. Cell Tiss. Biol. 15, 347–355 (2021). https://doi.org/10.1134/S1990519X21040106
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S1990519X21040106