Abstract
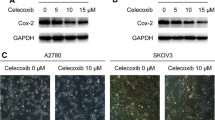
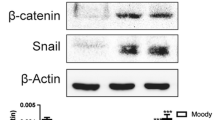
Epithelial ovarian cancer (EOC) has the highest mortality among various types of gynecological malignancies. Most patients die of metastasis and recurrence due to cisplatin resistance. Thus, it is urgent to develop novel therapies to cure this disease. CCK-8 assay showed that nigericin exhibited strong cytotoxicity on A2780 and SKOV3 cell lines. Flow cytometry indicated that nigericin could induce cell cycle arrest at G0/G1 phase and promote cell apoptosis. Boyden chamber assay revealed that nigericin could inhibit migration and invasion in a dose-dependent manner by suppressing epithelial–mesenchymal transition (EMT) in EOC cells. These effects were mediated, at least partly, by the Wnt/β-catenin signaling pathway. Our results demonstrated that nigericin could inhibit EMT during cell invasion and metastasis through the canonical Wnt/β-catenin signaling pathway. Nigericin may prove to be a novel therapeutic strategy that is effective in patients with metastatic EOC.
Similar content being viewed by others
Abbreviations
- EMT:
-
epithelial–mesenchymal transition
- EOC:
-
epithelial ovarian cancer
References
Siegel, R., Naishadham, D., and Jemal, A. (2012) Cancer statistics, 2012, Cancer J. Clin., 62, 10–29.
Siegel, R., Ward, E., Brawley, O., and Jemal, A. (2011) Cancer statistics, 2011: the impact of eliminating socioeconomic and racial disparities on premature cancer deaths, Cancer J. Clin., 61, 212–236.
Vergara, D., Merlot, B., Lucot, J. P., Collinet, P., Vinatier, D., Fournier, I., and Salzet, M. (2010) Epithelial-mesenchymal transition in ovarian cancer, Cancer Lett., 291, 59–66.
Davidson, B., Trope, C. G., and Reich, R. (2012) Epithelial-mesenchymal transition in ovarian carcinoma, Front. Oncol., 2, 33.
Huang, R. Y., Chung, V. Y., and Thiery, J. P. (2012) Targeting pathways contributing to epithelial-mesenchymal transition (EMT) in epithelial ovarian cancer, Curr. Drug Targets, 13, 1649–1653.
Turley, E. A., Veiseh, M., Radisky, D. C., and Bissell, M. J. (2008) Mechanisms of disease: epithelial-mesenchymal transition–does cellular plasticity fuel neoplastic progression? Nat. Clin. Pract. Oncol., 5, 280–290.
Thiery, J. P. (2002) Epithelial-mesenchymal transitions in tumour progression, Nat. Rev. Cancer, 2, 442–454.
Vaupel, P. (2004) Tumor microenvironmental physiology and its implications for radiation oncology, Semin. Radiat. Oncol., 14, 198–206.
Lu, D., Choi, M. Y., Yu, J., Castro, J. E., Kipps, T. J., and Carson, D. A. (2011) Salinomycin inhibits Wnt signaling and selectively induces apoptosis in chronic lymphocytic leukemia cells, Proc. Natl. Acad. Sci. USA, 108, 13253–13257.
Zhou, H. M., Dong, T. T., Wang, L. L., Feng, B., Zhao, H. C., Fan, X. K., and Zheng, M. H. (2012) Suppression of colorectal cancer metastasis by nigericin through inhibition of epithelial-mesenchymal transition, World J. Gastroenterol., 18, 2640–2648.
Xu, S., and Gotlieb, A. I. (2013) Wnt3a/beta-catenin increases proliferation in heart valve interstitial cells, Cardiovasc. Pathol., 22, 156–166.
Goodell, M. A. (2005) Stem cell identification and sorting using the Hoechst 33342 side population (SP), Curr. Protoc. Cytom., Chapt. 9, Unit 9.18.
Yilmaz, M., and Christofori, G. (2009) EMT, the cytoskeleton, and cancer cell invasion, Cancer Metastasis Rev., 28, 15–33.
Sung, P. L., Jan, Y. H., Lin, S. C., Huang, C. C., Lin, H., Wen, K. C., Chao, K. C., Lai, C. R., Wang, P. H., Chuang, C. M., Wu, H. H., Twu, N. F., Yen, M. S., Hsiao, M., and Huang, C. Y. (2016) Periostin in tumor microenvironment is associated with poor prognosis and platinum resistance in epithelial ovarian carcinoma, Oncotarget, 7, 4036–4047.
Gupta, P. B., Onder, T. T., Jiang, G., Tao, K., Kuperwasser, C., Weinberg, R. A., and Lander, E. S. (2009) Identification of selective inhibitors of cancer stem cells by high-throughput screening, Cell, 138, 645–659.
Yi, B. R., Kim, T. H., Kim, Y. S., and Choi, K. C. (2015) Alteration of epithelial-mesenchymal transition markers in human normal ovaries and neoplastic ovarian cancers, Int. J. Oncol., 46, 272–280.
Fernando, G., Paul, F., Laura, J., Alejandra, A. M., Gabriela, M., and Alberto, P. L. (2016) Is the Wnt/beta catenin signalling pathway activated in seminoma? An immunohistochemical study, J. Cancer Res. Ther., 12, 1075–1079.
Yang, C., Du, W., and Yang, D. (2016) Inhibition of green tea polyphenol EGCG((–)-epigallocatechin-3-gallate) on the proliferation of gastric cancer cells by suppressing canonical Wnt/beta-catenin signalling pathway, Int. J. Food Sci. Nutr., 67, 818–827.
Mittag, S., Valenta, T., Weiske, J., Bloch, L., Klingel, S., Gradl, D., Wetzel, F., Chen, Y., Petersen, I., Basler, K., and Huber, O. (2016) A novel role for the tumour suppressor Nitrilase1 modulating the Wnt/beta-catenin signalling pathway, Cell Discov., 2, 15039.
Van Zuylen, W. J., Rawlinson, W. D., and Ford, C. E. (2016) The Wnt pathway: a key network in cell signalling dysregulated by viruses, Rev. Med. Virol., 26, 340–355.
Patel, S., Doble, B., and Woodgett, J. R. (2004) Glycogen synthase kinase-3 in insulin and Wnt signalling: a doubleedged sword? Biochem. Soc. Trans., 32, 803–808.
Mashima, T. (2017) Cancer stem cells (CSCs) as a rational therapeutic cancer target, and screening for CSC-targeting drugs, Yakugaku Zasshi, 137, 129–132.
Najumudeen, A. K., Jaiswal, A., Lectez, B., Oetken-Lindholm, C., Guzman, C., Siljamaki, E., Posada, I. M., Lacey, E., Aittokallio, T., and Abankwa, D. (2016) Cancer stem cell drugs target K-ras signaling in a stemness context, Oncogene, 35, 5248–5262.
Wei, Z., Liu, Y., Wang, Y., Zhang, Y., Luo, Q., Man, X., Wei, F., and Yu, X. (2016) Downregulation of Foxo3 and TRIM31 by miR-551b in side population promotes cell proliferation, invasion, and drug resistance of ovarian cancer, Med. Oncol., 33, 126.
Author information
Authors and Affiliations
Additional information
Published in Russian in Biokhimiya, 2017, Vol. 82, No. 8, pp. 1209-1219.
Rights and permissions
About this article
Cite this article
Wang, W., Zhao, Y., Yao, S. et al. Nigericin inhibits epithelial ovarian cancer metastasis by suppressing the cell cycle and epithelial−mesenchymal transition. Biochemistry Moscow 82, 933–941 (2017). https://doi.org/10.1134/S0006297917080089
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0006297917080089