Summary
Question of the study
Previous studies showed that disturbed sleep is a common and frequent complaint reported by tinnitus patients. The purpose of this small pilot study was to investigate the impact of tinnitus as a cause of secondary insomnia.
Patients and methods
We compared polysomnographic records of ten patients with presently untreated chronic tinnitus and a complaint of disturbed sleep with those of 20 patients with primary insomnia and 20 age- and gender-matched healthy controls. Psychometric measurements were also performed using a tinnitus-standard rating scale, PSQI, SF-A, and BDI.
Results
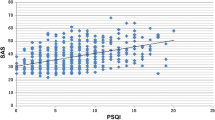
Concerning subjective sleep quality, both tinnitus and insomnia patients rated their sleep as significantly impaired compared to controls. Differences between patients and healthy controls were also observed with respect to their sleep patterns, with tinnitus patients showing a decreased sleep efficiency (P=0.049) and total sleep time (P=0.035) and an increased frequency of awakenings (P=0.016).
Conclusions
The results indicate that tinnitus is associated with subjective and objective sleep disturbances and stress the important impact of sleep disturbances in these patients.
Zusammenfassung
Fragestellung
In früheren Studien wurden Schlafstörungen als generelle und häufige Beschwerden bei Tinnitus genannt. In dieser Pilot-Studie wird die Bedeutung des Tinnitus als Ursache der sekundären Insomnie untersucht.
Patienten und Methodik
Es wurden polysomnographische Schlafparameter von 10 Patienten mit chronischem unbehandeltem Tinnitus, die über Schlafstörungen klagten, mit denen von 20 Patienten mit primärer Insomnie und 20 gesunden Probanden verglichen. Psychometrische Befunde wurden durch eine Tinnitus-Beurteilungsskala, SF-A, PSQI und BDI erfasst.
Ergebnisse
Hinsichtlich der subjektiven Schlafeinschätzung ergab sich ein signifikant schlechterer Schlaf bei den Tinnitus-Patienten und Insomniepatienten gegenüber den gesunden Probanden. Die polysomnographischen Ableitungen ergaben bei den Tinnitus-Patienten ein schlechteres Schlafprofil im Vergleich zu den gesunden Probanden mit signifikant reduzierter Schlafeffizienz (P=0,049), reduzierter Schlafzeit (P=0,035), sowie erhöhtem Anteil an Wachperioden (P=0,016).
Schlussfolgerung
Tinnitus ist assoziiert mit subjektiven und objektiven Schlafstörungen; dies unterstreicht die Bedeutung von Schlafstörungen für das Gesamtbeschwerdebild dieser Patienten.
Similar content being viewed by others
References
Alster J, Shemesh Z, Oman M, Attias J: Sleep disturbance associated with chronic tinnitus. Biol Psychiatry 24: 84–90, 1993.
American Sleep Disorders Association and Sleep Research Society. EEG Arousals: scoring rules and examples. Sleep 15: 173–185, 1992.
Axelsson A, Ringdahl A: Tinnitus: a study of its prevalence and characteristics. Br J Audiol 23: 53–62, 1989.
Bayar N, Boke B, Turan E, Belgien E: Efficacy of amitryptiline in the treatment of subjective tinnitus. J Otolaryngology 30(5): 300–303, 2001.
Buysse DJ, Reynolds CF, Monte TH, Berman SR, Kupfer DJ: The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res 28: 193–213, 1989.
Dobie RA: A review of randomized clinical trials in tinnitus. Laryngoscope 109(8): 1202–1211, 1999.
Folmer RL: Long-term reductions in tinnitus severity. BMC Ear Nose Throat Disorder 2: 3, 2002.
Folmer RL, Griest SE: Tinnitus and insomnia. Am J Otolaryngol 21(5): 287–293, 2000.
Goebel G, Hiller W: Tinnitus-Fragebogen (TF). Hogrefe, Göttingen, 1998.
Görtelmeyer R: Schlaffragebogen SF-A und SF-B. Collegium Internationale Psychiatriae Scolarum (CIPS). Internationale Skalen für Psychiatrie, Beltz, Weinheim, 1981.
Hajak G, Rodenbeck A, Voderholzer U, Riemann D, Cohrs S, Hohagen F et al.: Doxepin in the treatment of primary isomnia: a placebo-controlled, double-blind, polysomnographic study. J Clin Psychiatry 62(6): 453–463, 2000.
Halford JB, Anderson SD: Anxiety and depression in tinnitus sufferers. J Psychosom Res 35(4): 383–390, 1991.
Hautzinger M, Bailer M, Worall H, Keller F: Das Beck Depression-Inventar (BDI). Huber, Bern, 1993.
Hohagen F, Montero RF, Weiss E, Lis S, Schonbrun E. Dressing H et al.: Treatment of primary insomnia with trimipramine: an alternative to benzodiazepine hypnotics?. Eur Arch Psychiatry Clin Neurosci 244(2): 65–72, 1994.
Jakes S, Hallam R, Chambers C, Hinchcliffe R: A factor analytical study of tinnitus complaint behavior. Audiology 24: 195–206, 1985.
Meikle MB, Vernon J, Johnson RM: The perceived severity of tinnitus. Otolaryngolog Head Neck Surg 92(6): 689–696, 1984.
Moller AR: Pathophysiology of tinnitus. Otolaryngol Clin North Am 36(2): 249–266, 2003.
Notzinger EA, Buysee DJ, German A, Price JC, Miewald JM, Kupfer DJ: Functional neuroimaging evidence for hyperarousal in insomnia. Am J Psychiatry 161: 2126–2129, 2004.
Pilgramm M, Rychlick R, Lebisch H, Siedentop H, Goebel G, Kirchhoff D: Tinnitus in the Federal Republic of Germany: a representative epidemiological study. Proceedings of the Sixth International Tinnitus Seminar. Cambridge, pp 64–67, 1999.
Rechtschaffen A, Kales A: A manual of standardized terminology, techniques and scoring system for sleep stages of human subjects. US Government Printing Office, Public Health Service, Washington, DC, 1968.
Riemann D, Volderholzer U, Cohrs S, Rodenbeck A, Hajak G, Ruther E et al.: Timipramine in primary insomnia: results of a polysomnographic double blind controlled study. Pharmacopsychiatry 35(5): 165–174, 2002.
Scott B, Lindberg P, Melin L, Lyttkens L: Predictors of tinnitus discomfort, adaptation and subjective loudness. Br J Audiology 24: 51–62, 1990.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Burgos, I., Feige, B., Hornyak, M. et al. Chronic tinnitus and associated sleep disturbances. Somnologie 9, 133–138 (2005). https://doi.org/10.1111/j.1439-054X.2005.00056.x
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1111/j.1439-054X.2005.00056.x