Abstract
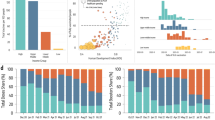
Inequalities in the accessibility and utilization of quality, safe, and effective coronavirus disease 2019 (COVID-19) vaccines across and within countries limited their value in protecting health during the COVID-19 pandemic. We quantified cross-country, income-associated inequality in COVID-19 vaccination using statistical models based on the data for 79 countries through December 2021. We found notable inequality in vaccinations per capita. At least 11.9% of doses administered in high-income countries could be redistributed to low-income countries to substantially reduce income-associated inequality in vaccinations. The results of this modeling study indicate that reliance on multiple doses of vaccine to attain optimal protection from COVID-19 is a significant contributor to inequality in vaccinations per capita. Dose-sharing mechanisms should account for and include efforts to optimize the capabilities of health systems to deliver vaccines.





Similar content being viewed by others
Data availability
The raw datasets used in the current study are publicly available and can be efficiently extracted from the sources indicated in the Methods. The processed datasets that were entered into the models and the analytical or statistical source code used are not publicly available but are available from the corresponding author upon reasonable request. These are currently being used for further research. Data and code sharing will require a Materials Transfer Agreement (MTA).
References
World Bank. World Bank country and lending groups. Washington, DC: World Bank; 2021.
Solís Arce JS, Warren SS, Meriggi NF, et al. COVID-19 vaccine acceptance and hesitancy in low- and middle-income countries. Nat Med. 2021;27:1385–94.
Moon S, Armstrong J, Hutler B, et al. Governing the access to COVID-19 tools accelerator: towards greater participation, transparency, and accountability. Lancet. 2022;399:487–94.
Gavi, The Vaccine Alliance. COVAX. Geneva: Gavi, The Vaccine Alliance; 2022.
Storeng KT, Stein F, de Puyvallée AB. COVAX and the many meanings of sharing. BMJ Glob Health. 2021;6: e007763.
Africa Renewal. COVID-19 vaccines: AU, Africa CDC and COVAX call on donors and manufacturers to accelerate access. New York: United Nations; 2021.
Asian Development Bank. ADB’s support to enhance COVID-19 vaccine access. Mandaluyong: Asian Development Bank; 2020.
World Health Organization. Strategy to achieve global COVID-19 vaccination by mid-2022. Geneva: World Health Organization; 2021.
World Health Organization. WHO coronavirus (COVID-19) dashboard. Geneva: World Health Organization; 2022.
Nature Biotechnology. How biomanufacturing can save the world. Nat Biotechnol. 2021;39:1315.
de Bengy PA, Storeng KT. COVAX, vaccine donations and the politics of global vaccine inequity. Glob Health. 2022;18:26.
Mathieu E, Ritchie H, Ortiz-Ospina E, et al. A global database of COVID-19 vaccinations. Nat Hum Behav. 2021;5:947–53.
United Nations Statistics Division. GNI, per capita GNI—US dollars. New York: United Nations Statistics Division; 2021.
United Nations, Department of Economic and Social Affairs, Population Division. World population prospects 2019. rev. 1. New York: United Nations, Department of Economic and Social Affairs, Population Division; 2019.
Stevens GA, Alkema L, Black RE, et al. Guidelines for Accurate and Transparent Health Estimates Reporting: the GATHER statement. Lancet. 2016;388:e19-23.
Bzdok D, Altman N, Krzywinski M. Statistics versus machine learning. Nat Methods. 2018;15:233–4.
Bergen N, Kirkby K, Fuertes CV, et al. Global state of education-related inequality in COVID-19 vaccine coverage, structural barriers, vaccine hesitancy, and vaccine refusal: findings from the Global COVID-19 Trends and Impact Survey. Lancet Glob Health. 2023;11:e207–17.
Duffy C, Newing A, Górska J. Evaluating the geographical accessibility and equity of COVID-19 vaccination sites in England. Vaccines (Basel). 2021;10:50.
Bayati M, Noroozi R, Ghanbari-Jahromi M, Jalali FS. Inequality in the distribution of COVID-19 vaccine: a systematic review. Int J Equity Health. 2022;21:122.
Tatar M, Shoorekchali JM, Faraji MR, Wilson FA. International COVID-19 vaccine inequality amid the pandemic: perpetuating a global crisis? J Glob Health. 2021;11:03086.
Suárez-Álvarez A, López-Menéndez AJ. Is COVID-19 vaccine inequality undermining the recovery from the COVID-19 pandemic? J Glob Health. 2022;12:05020.
Lazarus JV, Abdool Karim SS, van Selm L, et al. COVID-19 vaccine wastage in the midst of vaccine inequity: causes, types and practical steps. BMJ Glob Health. 2022;7: e009010.
Koolman X, van Doorslaer E. On the interpretation of a concentration index of inequality. Health Econ. 2004;13:649–56.
Graña C, Ghosn L, Evrenoglou T, et al. Efficacy and safety of COVID-19 vaccines. Cochrane Database Syst Rev. 2022;12:CD015477.
Pereira B, Fehl AG, Finkelstein SR, Jiga-Boy GM, Caserotti M. Scarcity in COVID-19 vaccine supplies reduces perceived vaccination priority and increases vaccine hesitancy. Psychol Mark. 2022;39:921–36.
Amimo F, Lambert B, Magit A, Hashizume M. A review of prospective pathways and impacts of COVID-19 on the accessibility, safety, quality, and affordability of essential medicines and vaccines for universal health coverage in Africa. Glob Health. 2021;17:42.
World Health Organization. Global action plan on antimicrobial resistance. Geneva: World Health Organization; 2015.
Acknowledgements
Not applicable.
Funding
None.
Author information
Authors and Affiliations
Contributions
FA contributed to conceptualization, methodology, software, validation, formal analysis, investigation, resources, data curation, writing—original draft, writing—review and editing, visualization, project administration, and funding acquisition. AM contributed to writing—reviewing and editing and funding acquisition. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
FA reports consultancy fees from the WHO. AM has none to declare.
Ethical approval
Ethical approval is not necessary because this research did not collect identifiable human material and data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
List of abbreviations and acronyms
List of abbreviations and acronyms
See Supplementary Material Part 3.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Amimo, F., Magit, A. Measuring income-associated inequalities in COVID-19 vaccination on a global scale: a modeling study. J Public Health Pol 44, 449–463 (2023). https://doi.org/10.1057/s41271-023-00433-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1057/s41271-023-00433-6