Abstract
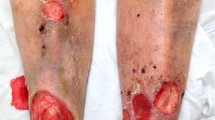
Rapidly evolving multidrug resistance renders conventional antimicrobial strategies increasingly inefficient. This urges the exploration of alternative strategies with a lower potential of resistance development to control microbial infections. A promising option is antimicrobial photodynamic therapy (aPDT), especially in the setting of wound infections. In this study its effectiveness was tested as a treatment option for polymicrobially infected wounds in both in vitro and in vivo models. First, aPDT was applied to wound-relevant Gram-positive and Gram-negative bacteria in planktonic culture as the standard in vitro test system and compared different media to show a possible dependency of the therapy on the surrounding environment. In a second step, aPDT was investigated in an in vitro model mimicking the wound bed conditions using fibrin-coated culture plates. Finally, we tested aPDT in vivo in a polymicrobial infected wound healing model in immunocompromised BALB/c mice. In vitro, it was shown that the bactericidal effectiveness of aPDT was strongly dependent on the surrounding environment of the phototoxic reaction. In vivo, the significant delay in wound healing induced by polymicrobial infection was drastically diminished by a two-times application of aPDT using 100 μM methylene blue (generally regarded as safe for topical application on human skin) and 24 J cm−2 pulsed red LED light. Our experiments suggest that aPDT is capable of significantly improving wound healing also in complicated polymicrobially infected wound situations.
Similar content being viewed by others
References
WHO, Antimicrobial resistance: global report on surveillance 2014. 2014, World Health Organization, p. 257, http://www.who.int.
R. I. Aminov, A brief history of the antibiotic era: lessons learned and challenges for the future, Front. Microbiol., 2010, 1, 134, DOI: 10.3389/fmicb.2010.00134.
R. Laxminarayan, et al., Access to effective antimicrobials: a worldwide challenge, Lancet, 2016, 387(10014), 168–175, DOI: 10.1016/S0140-6736(15)00474-2.
M. J. Renwick, V. Simpkin and E. Mossialos, in Targeting innovation in antibiotic drug discovery and development: The need for a One Health - One Europe - One World Framework, Copenhagen, Denmark, 2016.
A. Cassini, et al., Attributable deaths and disabilityadjusted life-years caused by infections with antibioticresistant bacteria in the EU and the European Economic Area in 2015: a population-level modelling analysis, Lancet Infect. Dis., 2019, 19(1), 56–66, DOI: 10.1016/S1473-3099(18) 30605-4.
O. Raab, Ueber die Wirkung fluorescirender Stoffe auf Infusorien, Verlag nicht ermittelbar, 1900.
M. D. Daniell and J. S. Hill, A history of photodynamic therapy, Aust. N. Z.J. Surg., 1991, 61(5), 340–348.
G. O. Schenck, Photosensitization, Ind. Eng. Chem., 1963, 55(6), 40–43, DOI: 10.1021/ie50642a006.
K. Gollnick, Type II Photooxygenation Reactions in Solution, in Advances in Photochemistry, 1968.
L. Huang, et al., Type I and Type II mechanisms of antimicrobial photodynamic therapy: an in vitro study on Gram-negative and Gram-positive bacteria, Lasers Surg. Med., 2012, 44(6), 490–499, DOI: 10.1002/lsm.22045.
M. Wainwright, Photodynamic antimicrobial chemotherapy (PACT), J. Antimicrob. Chemother., 1998, 42(1), 13–28.
N. Kashef and M. R. Hamblin, Can microbial cells develop resistance to oxidative stress in antimicrobial photodynamic inactivation?, Drug Resist. Updates, 2017, 31, 31–42, DOI: 10.1016/j.drup.2017.07.003.
A. Felgentrager, et al., Hydrogen bond acceptors and additional cationic charges in methylene blue derivatives: photophysics and antimicrobial efficiency, BioMed Res. Int., 2013, 2013, 482167, DOI: 10.1155/2013/482167.
A. S. Garcez and M. R. Hamblin, Methylene Blue and Hydrogen Peroxide for Photodynamic Inactivation in Root Canal - A New Protocol for Use in Endodontics, Eur. Endod. J., 2017, 2(1), 29, DOI: 10.5152/eej.2017.17023.
V. Klepac-Ceraj, et al., Photodynamic effects of methylene blue-loaded polymeric nanoparticles on dental plaque bacteria, Lasers Surg. Med., 2011, 43(7), 600–606, DOI: 10.1002/lsm.21069.
S. M. Yang, et al., Hydrogen Peroxide Enhances the Antibacterial Effect of Methylene Blue-based Photodynamic Therapy on Biofilm-forming Bacteria, Photochem. Photobiol., 2018, 95, 833–838, DOI: 10.1111/php.13056.
F. L. Esteban Florez, et al., Bioluminescence Analysis of Antibacterial Photodynamic Therapy Using Methylene Blue Mediated by Low-Intensity Level Laser Against Cariogenic Biofilms, Photomed. Laser Surg., 2018, 36(5), 258–265, DOI: 10.1089/pho.2017.4326.
F. Freire, et al., Photodynamic therapy of oral Candida infection in a mouse model, J. Photochem. Photobiol., B, 2016, 159, 161–168, DOI: 10.1016/j.jphotobiol.2016.03.049.
P. V. Araujo, et al., Antimicrobial effect of photodynamic therapy in carious lesions in vivo, using culture and realtime PCR methods, Photodiagn. Photodyn. Then., 2015, 12(3), 401–407, DOI: 10.1016/j.pdpdt.2015.06.003.
M. Marcolan De Mello, et al., Antimicrobial photodynamic therapy against clinical isolates of carbapenem-susceptible and carbapenem-resistant Acinetobacter baumannii, Lasers Med. Scl, 2019, 34, 1755–1761, DOI: 10.1007/s10103-019-02773-w.
N. Kashef, et al., Photodynamic inactivation of drug-resistant bacteria isolated from diabetic foot ulcers, Iran.J. Microbiol., 2011, 3(1), 36–41. PMC3279799.
A. H. C. Pereira, et al., Methylene blue internalization and photodynamic action against clinical and ATCC Pseudomonas aeruginosa and Staphyloccocus aureus strains, Photodiagn. Photodyn. Ther., 2018, 22, 43–50, DOI: 10.1016/j.pdpdt.2018.02.008.
S. R. de Annunzio, et al., Susceptibility of Enterococcus faecalis and Propionibacterium acnes to antimicrobial photodynamic therapy, J. Photochem. Photobiol., B, 2018, 178, 545–550, DOI: 10.1016/j.jphotobiol.2017.11.035.
M. D. Mastropaolo, et al., Synergy in polymicrobial infections in a mouse model of type 2 diabetes, Infect. Immun., 2005, 73(9), 6055–6063, DOI: 10.1128/IAI.73.9.6055-6063.2005.
K. J. Hendricks, et al., Synergy between Staphylococcus aureus and Pseudomonas aeruginosa in a rat model of complex orthopaedic wounds, J. Bone Jt. Surg., Am. Vol., 2001, 83(6), 855–861, DOI: 10.2106/00004623-200106000-00006.
T. Dalton, et al., An in vivo polymicrobial biofilm wound infection model to study interspecies interactions, PLoS One, 2011, 6(11), e27317, DOI: 10.1371/journal. pone.0027317.
N. Andreu, et al., Optimisation of bioluminescent reporters for use with mycobacteria, PLoS One, 2010, 5(5), e10777, DOI: 10.1371/journal.pone.0010777.
M. E. Starr, et al., A new cecal slurry preparation protocol with improved long-term reproducibility for animal models of sepsis, PLoS One, 2014, 9(12), e115705, DOI: 10.1371/journal.pone. 0115705.
A. F. Zuluaga, et al., Neutropenia induced in outbred mice by a simplified low-dose cyclophosphamide regimen: characterization and applicability to diverse experimental models of infectious diseases, BMC Infect. Dis., 2006, 6, 55, DOI: 10.1186/1471–2334-6-55.
F. Gad, et al., Targeted photodynamic therapy of established soft-tissue infections in mice, Photochem. Photobiol. Scl., 2004, 3(5), 451–458, DOI: 10.1039/b311901g.
Z. Malik, H. Ladan and Y. Nitzan, Photodynamic inactivation of Gram-negative bacteria: problems and possible solutions, J. Photochem. Photobiol., B, 1992, 14(3), 262–266, DOI: 10.1016/1011-1344(92)85104-3.
M. Wainwright, et al., Photobactericidal activity of phenothiazinium dyes against methicillin-resistant strains of Staphylococcus aureus, FEMS Microbiol. Lett., 1998, 160(2), 177–181, DOI: 10.1111/j.1574-6968.1998.tb12908.x.
G. Broughton, 2nd, J. E. Janis and C. E. Attinger, The basic science of wound healing, Plast. Reconstr. Surg., 2006, 117(7 Suppl), 12S–34S, DOI: 10.1097/01. prs.0000225430.42531.c2.
H. Ceri, et al., The Calgary Biofilm Device: new technology for rapid determination of antibiotic susceptibilities of bacterial biofilms, J. Clin. Microbiol., 1999, 37(6), 1771–1776. PMC84946.
S. Shani, M. Friedman and D. Steinberg, The anticariogenic effect of amine fluorides on Streptococcus sobrinus and glucosyltransferase in biofilms, Caries Res, 2000, 34(3), 260–267, DOI: 10.1159/000016600.
T. Dai, et al., Photodynamic therapy for Acinetobacter baumannii burn infections in mice, Antimicrob. Agents Chemother., 2009, 53(9), 3929–3934, DOI: 10.1128/AAC.00027-09.
L. R. Hoffman, et al., Selection for Staphylococcus aureus small-colony variants due to growth in the presence of Pseudomonas aeruginosa, Proc. Natl. Acad. Sci. U. S. A., 2006, 103(52), 19890–19895, DOI: 10.1073/pnas.0606756104.
A. P. Magalhaes, S. P. Lopes and M. O. Pereira, Insights into Cystic Fibrosis Polymicrobial Consortia: The Role of Species Interactions in Biofilm Development, Phenotype, and Response to In-Use Antibiotics, Front. Microbiol., 2016, 7, 2146, DOI: 10.3389/fmicb.2016.02146.
Z. M. Xiong, et al., Anti-Aging Potentials of Methylene Blue for Human Skin Longevity, Sci. Rep., 2017, 7(1), 2475, DOI: 10.1038/S41598-017-02419-3.
A. V. Corazza, et al., Photobiomodulation on the angiogenesis of skin wounds in rats using different light sources, Photomed. Laser Surg., 2007, 25(2), 102–106, DOI: 10.1089/pho.2006.2011.
Y. Li, et al., Effects of 630 nm Red and 460 nm Blue Light Emitting Diode Irradiation on Healing of the Skin Wound in Japanese Big-ear White Rabbit, Zhongguo Yixue Kexueyuan Xuebao, 2017, 39(3), 301–306, DOI: 10.3881/j. issn.1000-503X.2017.03.001.
P. Dungel, et al., Low level light therapy by LED of different wavelength induces angiogenesis and improves ischemic wound healing, Lasers Surg. Med., 2014, 46(10), 773–780, DOI: 10.1002/lsm.22299.
M. H. de Vasconcelos Catao, et al., Effects of red laser, infrared, photodynamic therapy, and green LED on the healing process of third-degree burns: clinical and histological study in rats, Lasers Med. Sci., 2015, 30(1), 421–428, DOI: 10.1007/S10103-014-1687-0.
B. Kofler, et al., Photodynamic Effect of Methylene Blue and Low Level Laser Radiation in Head and Neck Squamous Cell Carcinoma Cell Lines, Int. J. Mol. Sci., 2018, 19(4), 1107, DOI: 10.3390/ijms19041107.
C. Dunnill, et al., Reactive oxygen species (ROS) and wound healing: the functional role of ROS and emerging ROS-modulating technologies for augmentation of the healing process, Int. Wound J., 2017, 14(1), 89–96, DOI: 10.1111/iwj.12557.
E. M. Tuite and J. M. Kelly, Photochemical interactions of methylene blue and analogues with DNA and other biological substrates, J. Photochem. Photobiol., B, 1993, 21(2–3), 103–124, DOI: 10.1016/1011-1344(93) 80173-7.
J. P. Tardivo, et al., Methylene blue in photodynamic therapy: From basic mechanisms to clinical applications, Photodiagn. Photodyn. Ther., 2005, 2(3), 175–191, DOI: 10.1016/S1572-1000(05)00097-9.
Author information
Authors and Affiliations
Corresponding author
Additional information
Electronic supplementary information (ESI) available. See DOI: 10.1039/d0pp00108b
Rights and permissions
About this article
Cite this article
Karner, L., Drechsler, S., Metzger, M. et al. Antimicrobial photodynamic therapy fighting polymicrobial infections – a journey from in vitro to in vivo. Photochem Photobiol Sci 19, 1332–1343 (2020). https://doi.org/10.1039/d0pp00108b
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1039/d0pp00108b