Abstract
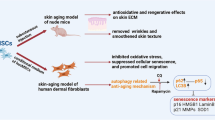
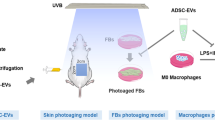
Ultraviolet B (UVB) radiation is a major cause of aging in dermal fibroblasts. Human umbilical cord mesenchymal stem cell-derived extracellular vesicles (MSC-EVs) show antioxidant activity. In this study, the anti-aging effects of MSC-EVs on dermal fibroblast photoaging induced by UVB radiation were evaluated, and the effects of extracellular vesicles derived from dermal fibroblasts (Fb-EVs) were compared Human umbilical cord mesenchymal stem cells and human dermal fibroblasts were cultured, and MSC-EVs and Fb-EVs were isolated and characterized. Human dermal fibroblasts were cultured in the absence or presence of different concentrations of EVs 24 hours prior to UVB radiation exposure. Cell proliferation and cell cycle were evaluated, and senescent cells and intracellular ROS were detected. The expressions of matrix metalloproteinase-1 (MMP-1), extracellular matrix protein collagen type 1 (Col-1), and antioxidant proteins such as glutathione peroxidase 1 (GPX-1), superoxide dismutase (SOD), and cata-lase were also analyzed. Pretreatment with MSC-EVs or Fb-EVs significantly inhibited the production of ROS induced by UVB radiation, increased dermal fibroblast proliferation, protected cells against UVB-nduced cell death and cell cycle arrest, and remarkably decreased the percentage of aged cells. Pretreatment with MSC-EVs or Fb-EVs promoted the expressions of GPX-1 and Col-1 and decreased the expression of MMP-1. Both MSC-EVs and Fb-EVs protected dermal fibroblasts from UVB-induced photoaging, likely through their antioxidant activity.
Similar content being viewed by others
References
B. A. Gilchrest, Photoaging, J. Invest. Dermatol, 2013, 133(E1), E2–E6.
A. Kammeyer and R. M. Luiten, Oxidation events and skin aging, Ageing Res. Rev., 2015, 21, 16–29.
Y. R. Lee, E. M. Noh, E. Y. Jeong, et al., Cordycepin inhibits UVB-induced matrix metalloproteinase expression by suppressing the NF-kappaB pathway in human dermal fibroblasts, Exp. Mol. Med., 2009, 41(8), 548–554.
F. Poon, S. Rang and A. L. Chien, Mechanisms and treatments of photoaging, Photodermatol., Photoimmunol. Photomed., 2015, 31(2), 65–74.
M. Wlaschek, I. Tantcheva-Poor, L. Naderi, et al., Solar UV irradiation and dermal photoaging, J. Photochem. Photobiol., B, 2001, 63(1–3), 41–51.
R. S. Stern, Clinical practice. Treatment of photoaging, N. Engl J. Med., 2004, 350(15), 1526–1534.
Y. Lee, A. S. El and M. J. Wood, Exosomes and microvesi-cles: extracellular vesicles for genetic information transfer and gene therapy, Hum. Mol. Genet, 2012, 21(R1), R125–R134.
N. Chaput and C. Thery, Exosomes: immune properties and potential clinical implementations, Semin. Immunopathol, 2011, 33(5), 419–440.
M. Z. Ratajczak, M. Kucia, T. Jadczyk, et al., Pivotal role of paracrine effects in stem cell therapies in regenerative medicine: can we translate stem cell-secreted paracrine factors and microvesicles into better therapeutic strategies?, Leukemia, 2012, 26(6), 1166–1173.
G. Raposo, H. W. Nijman, W. Stoorvogel, et al., B lymphocytes secrete antigen-presenting vesicles, J. Exp. Med., 1996, 183(3), 1161–1172.
R. C. Lai, T. S. Chen and S. K. Lim, Mesenchymal stem cell exosome: a novel stem cell-based therapy for cardiovascular disease, Regener. Med., 2011, 6(4), 481–492.
J. Ratajczak, K. Miekus, M. Kucia, et al., Embryonic stem cell-derived microvesicles reprogram hematopoietic progenitors: evidence for horizontal transfer of mRNA and protein delivery, Leukemia, 2006, 20(5), 847–856.
C. I. Del, C. N. Shrimpton, P. Thiagarajan, et al., Tissue-factor-bearing microvesicles arise from lipid rafts and fuse with activated platelets to initiate coagulation, Blood, 2005, 106(5), 1604–1611.
S. Bruno, C. Grange, F. Collino, et al., Microvesicles derived from mesenchymal stem cells enhance survival in a lethal model of acute kidney injury, PLoS One, 2012, 7(3), e33115.
S. Bian, L. Zhang, L. Duan, et al., Extracellular vesicles derived from human bone marrow mesenchymal stem cells promote angiogenesis in a rat myocardial infarction model, J. Mol Med., 2014, 92(4), 387–397.
S. Keshtkar, N. Azarpira and M. H. Ghahremani, Mesenchymal stem cell-derived extracellular vesicles: novel frontiers in regenerative medicine, Stem Cell Res. Ther., 2018, 9(1), 63.
B. Zhang, L. Shen, H. Shi, et al., Exosomes from Human Umbilical Cord Mesenchymal Stem Cells: Identification, Purification, and Biological Characteristics, Stem Cells Int., 2016, 2016, 1–11.
Y. Yan, W. Jiang, Y. Tan, et al., hucMSC Exosome-Derived GPX1 Is Required for the Recovery of Hepatic Oxidant Injury, Mol. Ther., 2017, 25(2), 465–479.
Y. Yan, W. Xu, H. Qian, et al., Mesenchymal stem cells from human umbilical cords ameliorate mouse hepatic injury in vivo, Liver Int., 2009, 29(3), 356–365.
F. G. Chen, W. J. Zhang, D. Bi, et al., Clonal analysis of nestin(-) vimentin(+) multipotent fibroblasts isolated from human dermis, J. Cell Sci, 2007, 120(Pt 16), 2875–2883.
H. Woo, V. Sunkara, J. Park, et al., Exodisc for Rapid, Size-Selective, and Efficient Isolation and Analysis of Nanoscale Extracellular Vesicles from Biological Samples, ACS Nano, 2017, 11(2), 1360–1370.
H. M. Chiang, T. J. Lin, C. Y. Chiu, et al., Coffea arabica extract and its constituents prevent photoaging by suppressing MMPs expression and MAP kinase pathway, Food Chem. Toxicol, 2011, 49(1), 309–318.
G. P. Dimri, X. Lee, G. Basile, et al., A biomarker that identifies senescent human cells in culture and in aging skin in vivo, Proc. Natl. Acad. Sci. U. S. A., 1995, 92(20), 9363–9367.
C. Jia, Y. Lu, B. Bi, et al., Platelet-rich plasma ameliorates senescence-like phenotypes in a cellular photoaging model, RSC Adv., 2017, 7(6), 3152–3160.
K. J. Livak and T. D. Schmittgen, Analysis of relative gene expression data using real-time quantitative PCR and the 2(-DeIta Delta C(T)) Method, Methods, 2001, 25(4), 402–408.
P. Brenneisen, H. Sies and K. Scharffetter-Kochanek, Ultraviolet-B irradiation and matrix metalloproteinases: from induction via signaling to initial events, Ann. N. Y. Acad. Sci., 2002, 973, 31–43.
Z. A. Abdel-Malek, A. L. Kadekaro and V. B. Swope, Stepping up melanocytes to the challenge of UV exposure, Pigm. Cell Melanoma Res., 2010, 23(2), 171–186.
S. Q. Wang, Y. Balagula and U. Osterwalder, Photoprotection: a review of the current and future technologies, Dermatol Ther., 2010, 23(1), 31–47.
M. Tkach and C. Thery, Communication by Extracellular Vesicles: Where We Are and Where We Need to Go, Cell, 2016, 164(6), 1226–1232.
S. Cosenza, M. Ruiz, M. Maumus, et al., Pathogenic or Therapeutic Extracellular Vesicles in Rheumatic Diseases: Role of Mesenchymal Stem Cell-Derived Vesicles, Int. J. Mol. Sci, 2017, 18(4), 889.
V Borger, M. Bremer, R. Ferrer-Tur, et al., Mesenchymal Stem/Stromal Cell-Derived Extracellular Vesicles and Their Potential as Novel Immunomodulatory Therapeutic Agents, Int. J. Mol. Sci, 2017, 18(7), 1450.
B. Giebel, L. Kordelas and V Borger, Clinical potential of mesenchymal stem/stromal cell-derived extracellular vesicles, Stem Cell Invest., 2017, 4(10), 84.
L. S. Meirelles, A. M. Fontes, D. T. Covas, et al., Mechanisms involved in the therapeutic properties of mesenchymal stem cells, Cytokine Growth Factor Rev., 2009, 20(5–6), 419–427.
J. Stephen, E. L. Bravo, D. Colligan, et al., Mesenchymal stromal cells as multifunctional cellular therapeutics - a potential role for extracellular vesicles, Transfus. Apher. Sci, 2016, 55(1), 62–69.
H. Xie, Z. Wang, L. Zhang, et al., Development of an angio-genesis-promoting microvesicle-alginate-polycaprolactone composite graft for bone tissue engineering applications, Peer J, 2016, 4, e2040.
H. Xie, Z. Wang, L. Zhang, et al., Extracellular Vesicle-func-tionalized Decalcified Bone Matrix Scaffolds with Enhanced Pro-angiogenic and Pro-bone Regeneration Activities, Sci. Rep., 2017, 7, 45622.
H. Huang, S. Feng, W. Zhang, et al., Bone marrow mesenchymal stem cell derived extracellular vesicles improve the survival of transplanted fat grafts, Mol. Med. Rep., 2017, 16(3), 3069–3078.
F. G. Chen, W. J. Zhang, D. Bi, et al., Clonal analysis of nestin(-) vimentin(+) multipotent fibroblasts isolated from human dermis, J. Cell Sci., 2007, 120(Pt 16), 2875–2883.
Y. P. Hwang, K. N. Oh, H. J. Yun, et al., The flavonoids api-genin and Iuteolin suppress ultraviolet A-induced matrix metalloproteinase-1 expression via MAPKs and AP-1–depen-dent signaling in HaCaT cells, J. Dermatol. Sci., 2011, 61(1), 23–31.
T. Ohba, M. Ishisaka, S. Tsujii, et al., Crocetin protects ultraviolet A-induced oxidative stress and cell death in skin in vitro and in vivo, Eur. J. Pharmacol., 2016, 789, 244–253.
R. L. Rajendran, P. Gangadaran, S. S. Bak, et al., Extracellular vesicles derived from MSCs activates dermal papilla cell in vitro and promotes hair follicle conversion from telogen to anagen in mice, Sci Rep., 2017, 7(1), 15560.
G. Zhang, X. Zou, Y. Huang, et al., Mesenchymal Stromal Cell-Derived Extracellular Vesicles Protect Against Acute Kidney Injury Through Anti-Oxidation by Enhancing Nrf2/ ARE Activation in Rats, Kidney Blood Pressure Res., 2016, 41(2), 119–128.
G. W. Hu, Q. Li, X. Niu, et al., Exosomes secreted by human-induced pluripotent stem cell-derived mesenchymal stem cells attenuate limb ischemia by promoting angiogenesis in mice, Stem Cell Res. Then, 2015, 6, 10.
Author information
Authors and Affiliations
Corresponding author
Additional information
These authors contributed equally to this work.
Rights and permissions
About this article
Cite this article
Deng, M., Yu, T.Z., Li, D. et al. Human umbilical cord mesenchymal stem cell-derived and dermal fibroblast-derived extracellular vesicles protect dermal fibroblasts from ultraviolet radiation-induced photoaging in vitro. Photochem Photobiol Sci 19, 406–414 (2020). https://doi.org/10.1039/c9pp00421a
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1039/c9pp00421a