Abstract
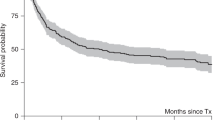
The role of high-dose chemotherapy (HDCT) in patients with refractory breast cancer is not well established. Forty-two female patients (median age of 46 years) with breast cancer refractory to neoadjuvant chemotherapy received HDCT (cyclophosphamide, carmustine and thiotepa) supported by an autologous peripheral blood stem cells transplant. Their disease had been refractory (defined as less than partial response) to one (18 patients) or two (24 patients) regimens of neoadjuvant chemotherapy. Twenty-nine patients had surgery before HDCT. The best response after surgery, HDCT, and radiation therapy was assessed 60 days after transplantation. Thirty patients had complete remission, eight had a PR, one had a minor response, and three had progressive disease. In seven of 13 patients whose disease was inoperable before HDCT, it became operable. After a median follow-up of 42 months, 21 patients were alive, and 15 remained disease free. Five-year overall survival (OS) was 57% (CI, 50–64%), and the estimated 5-year progression-free survival was 40% (CI, 32–48%). Both OS and PFS were better in patients whose disease became operable after chemotherapy than in those whose disease remained inoperable. A randomized study is warranted in this patient population.






Similar content being viewed by others
References
Bonadonna G, Valagussa P, Brambilla C, Ferrari L, Moliterni A, Terenziani M et al. Primary chemotherapy in operable breast cancer: eight-year experience at the Milan Cancer Institute. J Clin Oncol 1998; 16: 93–100.
Kuerer HM, Newman LA, Smith TL, Ames FC, Hunt KK, Dhingra K et al. Clinical course of breast cancer patients with complete pathologic primary tumor and axillary lymph node response to doxorubicin-based neoadjuvant chemotherapy. J Clin Oncol 1999; 17: 460–469.
Cristofanilli M, Buzdar AU, Hortobagyi GN . Update on the management of inflammatory breast cancer. Oncologist 2003; 8: 141–148.
Buchholz TA, Hunt KK, Whitman GJ, Sahin AA, Hortobagyi GN . Neoadjuvant chemotherapy for breast carcinoma: multidisciplinary considerations of benefits and risks. Cancer 2003; 98: 1150–1160.
Valero V, Buzdar AU, McNeese M, Singletary E, Hortobagyi GN . Primary chemotherapy in the treatment of breast cancer: the University of Texas M. D. Anderson Cancer Center experience. Clin Breast Cancer 2002; 3 (Suppl 2): S63–S68.
Chen AM, Meric-Bernstam F, Hunt KK, Thames HD, Oswald MJ, Outlaw ED et al. Breast conservation after neoadjuvant chemotherapy: the M.D. Anderson cancer center experience. J Clin Oncol 2004; 22: 2303–2312.
Bear HD, Anderson S, Brown A, Smith R, Mamounas EP, Fisher B et al. The effect on tumor response of adding sequential preoperative docetaxel to preoperative doxorubicin and cyclophosphamide: preliminary results from National Surgical Adjuvant Breast and Bowel Project Protocol B-27. J Clin Oncol 2003; 21: 4165–4174.
Schwartz GF, Hortobagyi GN, Masood S, Palazzo J, Holland R, Page D et al. Proceedings of the consensus conference on neoadjuvant chemotherapy in carcinoma of the breast, April 26–28, 2003, Philadelphia, PA. Hum Pathol 2004; 35: 781–784.
Buchholz TA, Hill BS, Tucker SL, Frye DK, Kuerer HM, Buzdar AU et al. Factors predictive of outcome in patients with breast cancer refractory to neoadjuvant chemotherapy. Cancer J 2001; 7: 413–420.
Montemurro F, Rondâon G, Munsell M, Smith TL, Donato ML, Gajewski JL et al. Predicting outcome based on Swenerton score in patients with metastatic breast cancer undergoing high-dose chemotherapy and autologous hematopoietic stem cell transplantation: implications for patient selection. Biol Blood Marrow Transplant 2003; 9: 330–340.
Montemurro F, Rondâon G, Ueno NT, Munsell M, Gajewski JL, Champlin RE . Factors affecting progression-free survival in hormone-dependent metastatic breast cancer patients receiving high-dose chemotherapy and hematopoietic progenitor cell transplantation: role of maintenance endocrine therapy. Bone Marrow Transplant 2002; 29: 861–866.
Rahman ZU, Frye DK, Buzdar AU, Smith TL, Asmar L, Champlin RE et al. Impact of selection process on response rate and long-term survival of potential high-dose chemotherapy candidates treated with standard-dose doxorubicin-containing chemotherapy in patients with metastatic breast. J Clin Oncol 1997; 15: 3169–3170.
Schwartzberg L, Weaver C, Lewkow L, McAneny B, Zhen B, Birch R et al. High-dose chemotherapy with peripheral blood stem cell support for stage IIIB inflammatory carcinoma of the breast. Bone Marrow Transplant 1999; 24: 981–987.
Viens P, Penault-Llorca F, Jacquemier J, Gravis G, Cowen D, Bertucci F et al. High-dose chemotherapy and haematopoietic stem cell transplantation for inflammatory breast cancer: pathologic response and outcome. Bone Marrow Transplant 1998; 21: 249–254.
Adkins D, Brown R, Trinkaus K, Maziarz R, Luedke S, Freytes C et al. Outcomes of high-dose chemotherapy and autologous stem-cell transplantation in stage IIIB inflammatory breast cancer. J Clin Oncol 1999; 17: 2006–2014.
Ayash LJ, Elias A, Ibrahim J, Schwartz G, Wheeler C, Reich E et al. High-dose multimodality therapy with autologous stem-cell support for stage IIIB breast carcinoma. J Clin Oncol 1998; 16: 1000–1007.
Buchholz TA, Tucker SL, Moore RA, McNeese MD, Strom EA, Jhingrin A et al. Importance of radiation therapy for breast cancer patients treated with high-dose chemotherapy and stem cell transplant. Int J Radiat Oncol Biol Phys 2000; 46: 337–343.
Wong R, Rondon G, Saliba RM, Shannon VR, Giralt SA, Champlin RE et al. Idiopathic pneumonia syndrome after high-dose chemotherapy and autologous hematopoietic stem cell transplantation for high-risk breast cancer. Bone Marrow Transplant 2003; 31: 1157–1163.
Acknowledgements
We thank Christine Wogan of Department of Scientific Publications at M.D. Anderson Cancer Center for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ueno, N., Konoplev, S., Buchholz, T. et al. High-dose chemotherapy and autologous peripheral blood stem cell transplantation for primary breast cancer refractory to neoadjuvant chemotherapy. Bone Marrow Transplant 37, 929–935 (2006). https://doi.org/10.1038/sj.bmt.1705355
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705355
- Springer Nature Limited