Abstract
Study design:
A retrospective cohort study.
Objectives:
To review demographic trends in traumatic spinal cord injury (TSCI) and non-traumatic spinal cord injury (NTSCI).
Setting:
The Queen Elizabeth National Spinal Injuries Unit (QENSIU), sole provider of treatment for TSCI in Scotland; a devolved region of the UK National Health Service.
Methods:
A retrospective review of the QENSIU database was performed between 1994 and 2013. This database includes demographic and clinical data from all new TSCI patients in Scotland, as well as patients with severe NTSCI.
Results:
Over this 20-year period there were 1638 new cases of TSCI in Scotland; 75.2% occurring in males. TSCI incidence increased non-significantly (13.3 per million population to 17.0), while there were significant increases in mean age at time of TSCI (44.1–52.6 years), the proportion of TSCIs caused by falls (41–60%), the proportion of TSCIs resulting in an American Spinal Injury Association Impairment Scale score of C and D on admission (19.7–28.6% and 34.5–39.5%, respectively) and the proportion of cervical TSCIs (58.4–66.3%). The increase in cervical TSCI was specifically due to an increase in C1–C4 lesions (21.7–31.2%). NTSCI patients (n=292) were 5 years older at injury, more likely to be female (68.1% male) and had a range of diagnoses.
Conclusion:
This study supports the suggestion that demographic profiles in SCI are subject to change. In this population, of particular concern is the increasing number of older patients and those with high level tetraplegia, due to their increased care needs. Prevention programmes, treatment pathways and service provision need to be adjusted for optimum impact, improved outcome and long-term care for their target population.
Similar content being viewed by others
Introduction
Spinal cord injury (SCI) and its resultant disability has a high impact on individuals, families and society.1, 2 Low volume, highly specialised, immediate care followed by comprehensive rehabilitation results in a significant life expectancy for the majority of this population.3 With high lifetime care costs, estimated in 2011 at $5.4 million for a 25-year-old with a C1−C4 lesion in the USA,4 understanding the epidemiology of SCI is important to develop prevention strategies, assess treatments and for planning the provision of immediate and long-term care.5
In the USA all Model SCI centres are required to submit information to the National Spinal Cord Injury Statistical Center database. These data includes aetiology, gender, age and injury level of each patient.6 A number of studies having been conducted using these data. These studies contain large sample sizes, a range of longitudinal information and excellent internal data quality,7, 8, 9 and are widely cited in SCI literature. However, this data only represents ~13% of all new SCIs in the USA.10
In Europe, there has been a number of region-specific studies investigating the epidemiology of Traumatic SCI (TSCI),11, 12, 13, 14, 15 with only a limited number of population-based studies.16, 17, 18 Recognising the potential value of such data, the WHO (World Health Organisation) and International Spinal Cord Society have expressed the need for more comprehensive national data of SCI epidemiology.19 For the past 20 years funding patterns and geographical factors have resulted in all new TSCIs in Scotland being treated at the Queen Elizabeth National Spinal Injuries Unit (QENSIU). The demographic data from the QENSIU can be used to reliably assess changing trends in TSCI epidemiology at a national level.
The aim of this study was to describe the incidence and demographics of SCI in Scotland over a 20-year period and to use this longitudinal data to identify changing trends in TSCI and NTSCI epidemiology.
Materials and methods
Study setting
The QENSIU was purpose-built in 1993 as the sole provider of initial treatment, rehabilitation and lifelong care for patients with an SCI over the age of 12 in Scotland; a devolved region of the UK National Health Service (NHS). It is the hub of a managed clinical network funded by NHS Scotland. The unit provides care for a population of 5.3 million and admits all patients with TSCI and patients who have a spinal fracture with the risk of an SCI. Owing to the diverse primary diagnosis and a wide spectrum of disability, resulting in a variable need for SCI rehabilitation, only patients with severe NTSCI are admitted to the QENSIU, with other patients managed in regional neurorehabilitation units. In addition, Scottish residents sustaining a TSCI while abroad are repatriated for rehabilitation at the QENSIU, accounting for ~2% of all admissions.20 In 2013, 47% of patients were admitted to the QENSIU within 48 h of injury, and 68% within 1 week.20
Details of the aetiology, gender, age and injury level of all new admissions are entered into the QENSIU database. This database encompasses all new TSCIs in Scotland. The database does not include deaths caused by SCI before admission.
Approval for the collection and evaluation of data within the database was granted by the National Services Division of the Scottish Government.
Analysis
All patients admitted to the QENSIU with an SCI were included in this study. The neurological level of injury and degree of impairment after SCI was assessed by a spinal injuries consultant on admission and defined according to the International Neurological Classification of Spinal Injury using the American Spinal Injury Association Impairment Scale (AIS),21 with consistent AIS scores available for all patients admitted after 1998. Patients who had an AIS score of E on admission, that is, normal function and no SCI,21 were not included in this study. TSCI aetiology was classified in accordance with the International SCI core data set as assault, fall, road traffic collision, sports (including falls that occurred during sporting activities, such as rock and mountain climbing) and other traumatic (including deliberate self harm (DSH), iatrogenic,22 industrial and unclassified).23 NTSCI aetiology was classified in accordance with level two of The International Spinal Cord Injury Data Sets for NTSCI as infection; inflammatory and auto-immune disease, neoplastic, skeletal malformation, spinal dysraphism, vascular disorder and vertebral column degenerative disorder.24
Crude annual incidence rates were calculated using the mid-year population estimate for each year,25 and were age and gender adjusted for the years 1994–2003 using population information from the 1991 Scottish census26 and for the years 2004–2013 using population information from the 2011 Scottish census.27 Descriptive data are presented as the mean values over a 5-year time block, as well as the mean values over the 20-year study duration.28
A Poisson regression model was used to assess for trends in temporal TSCI data, while a Cuzick’s test for trend was used to assess for trends in continuous TSCI and NTSCI data. A two-sample independent t-test was used to test for a significant difference between the age of people sustaining a TSCI through falling and all other aetiologies. These comparisons were made using annual results. Comparisons of incidence rate and age at injury were made between patients between 16 and 50 years of age and between 51 and 85 years of age, providing an equal distribution for each group. No statistical testing was performed on temporal NTSCI data due to the low sample size. A significance level of 5% (P<0.05) was used and all confidence intervals are expressed at 95% (95% CI).
Results
Between 1994 and 2013 1638 patients sustained a TSCI in Scotland, with a further 292 patients with NTSCI admitted to the QENSIU for specialist care. Population-based results for TSCI are presented first, followed by admissions after NTSCI.
Traumatic SCI
Incidence
Between 1994 and 2013 the mean Scottish population was 5 144 625, resulting in a mean TSCI incidence rate of 15.9 per million (Table 1,Supplementary Table A1). This incidence rate increased non-significantly (β=0.016, 95% CI: −0.002, 0.035) over the study duration, from 13.3 per million between 1994 and 1998 to 17.0 between 2009 and 2013 (Figure 1). For patients between 51 and 85 years of age the incidence rate increased significantly (β=0.052, 95% CI: 0.032, 0.073) over the study duration, while there was no significant change for patients between 16 and 50 years of age (β=−0.013, 95% CI: −0.03, −0.01; Figures 1 and 2).
Incidence rate of traumatic spinal cord injury in Scotland between 1994 and 2013. All patients are shown in black, patients between the ages of 16 and 50 are shown in dark grey and patients between 51 and 85 years of age are shown in light grey. Results are presented as mean annual incidence rate over a 5-year period.
Aetiology
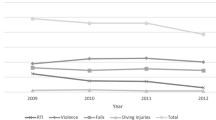
The most common cause of TSCI in Scotland was falls, responsible for 51.7% of TSCIs over the study duration (Supplementary Table A2). This proportion of TSCI caused by falls increased significantly (β=0.022, 95% CI: 0.011, 0.033) over the study duration, from 41.6% between 1994 and 1998 to 60.0% between 2009 and 2013 (Figure 3). In 2013, 61 patients sustained a TSCI from a fall of which the height was known. Twenty-seven (44.3%) of these falls were from a height of >2 m. While the distribution of fall height was similar for both males and females (43.6 and 45.5% from a height of >2 m, respectively), patients under the age of 65 were more likely to have a fall from a height of >2 m than those over 65 (60.0% versus 29.0%, respectively). The second most common cause of TSCI was road traffic collision (24.4%), with 38% of such patients driving, 33% passengers, 22% motorcyclists and 7% pedestrians. The third most common cause of TSCI was sports (10.2%), where cycling was the leading cause (30%), followed by diving/swimming (26%), horse riding (12%) and rugby (11%). Scotland’s geography makes it worth noting that of these sports related TSCIs, only nine were secondary to a mountaineering accident.
Age at Injury
The mean age at which TSCI occurred in Scotland was 47.2 years. The mean age at injury increased significantly (z=7.25, P<0.001) from 44.1 years (median 41.4 years) between 1994 and 1998 to 52.6 years (median 54.1 years) between 2009 and 2013 (Table 1). There was a significant increase in the mean age of patients between 51 and 85 years of age (z=2.17, P=0.03), while there was no significant change in the mean age of patients between 16 and 50 years of age (z=1.31, P=0.191). The mean age at injury of people who suffered a TSCI caused by falls (54.2 years) was significantly greater (P<0.000) than for all other aetiologies (39.5 years).
Gender
Between 1994 and 2013, 75.2% of TSCIs in Scotland occurred in males. This gender variation remained relatively stable over the study duration (β=−0.001, 95% CI: −0.009, 0.008; Table 1). Of the 344 patients with a TSCI over the age of 65, 31% were female, compared with 23% in under 65s. Overall, 30% of patients who suffered a TSCI due to fall were female, compared with 21% for all other aetiologies.
Injury Level
In all, 60.6% of TSCIs in Scotland resulted in a cervical injury, which increased significantly (β=0.01, 95% CI: 0.001, 0.020) over the study duration from 58.4% between 1994 and 1998 to 66.3% between 2009 and 2013 (Figure 4). This increase can be attributed almost solely to an increase in C1–C4 lesions, which increased significantly (β=0.027, 95% CI: 0.012, 0.043) from 21.7% of all TSCIs between 1994 and 1998 to 31.2% between 2009 and 2013, while C5−C8 lesions decreased non-significantly (β=−0.0004, 95% CI: −0.013, 0.012) from 36.7 to 35.2% over this period (Figure 4).
Percentage of new traumatic spinal cord injuries resulting in a cervical injury in Scotland between 1994 and 2013. All cervical injuries are shown in black, C1–C4 injuries are shown in dark grey, while C5–C8 injuries are shown in light grey. Results are presented as mean percentage of new injuries per year over a 5-year period.
Neurological Deficit
Between 1999 and 2013, the most common AIS score at admission for patients with a new TSCI in Scotland was D (36.1%), followed by A (29.9%). The proportion of patients with an AIS score of both C and D increased significantly (β=0.048, 95% CI: 0.022, 0.073 and β=0.033, 95% CI: 0.012, 0.054, respectively) from 19.7 and 34.5% between 1999 and 2003 to 28.6 and 39.5% between 2009 and 2013, respectively. The proportion of patients with an AIS score of B decreased significantly (β=−0.053, 95% CI: −0.093, −0.012), from 13.1% between 1999 and 2003 to 5.9% between 2009 and 2013, respectively. There was a decrease in the proportion of patients with an AIS score of A from 32.7% between 1999 and 2003 to 25.9% between 2009 and 2013, respectively, however this change was not significant (β=−0.019, 95% CI: −0.042, 0.005) (Figure 5).
American Spinal Injury Association Impairment Scale score at admission for patients with new traumatic spinal cord injuries in Scotland between 1999 and 2013. AIS A are shown in black, AIS B are shown in dark grey with a dashed line, AIS C are shown in grey with a solid line and AIS D are shown in light grey with a dashed line. Results are presented as mean percentage of new injuries per year over a 5-year period.
Non-Traumatic SCI
The incidence and demographics of patients admitted to the QENSIU with a new NTSCI between 1994 and 2013 are shown in Table 2 (annual rates shown in Supplementary Table A3). The mean age of patients with a new NTSCI increased significantly over the study duration (z=2.87, P=0.004), while the proportion of males appeared to decrease over the study duration. The most common causes of NTSCI were vascular disorders, infections and vertebral column degenerative disorders (Table 3).
Discussion
The aim of this study was to describe the incidence and demographics of SCI in Scotland over a 20-year period and to identify changing trends over this time. There was a significant increase in mean age of patients with a new TSCI, the proportion of such patients sustaining a cervical injury (specifically due to a significant increase in C1–C4 lesions) and the proportion of TSCIs caused by falls.
The mean incidence rate of TSCI in Scotland (15.9 per million) is comparable with that found in other studies in Western Europe,11, 12, 17 but is lower than the global incidence rate of 23 per million predicted by Lee et al.29 Such global variations may be explained by diversity in assessment methodology (such as the inclusion of patients with an AIS score of E on admission), inclusion of individuals who die at the scene and the social and economic conditions of the country.13, 30
The proportion of TSCIs caused by falls in Scotland increased significantly throughout the study duration, a trend also reported in Europe and the USA.10, 11, 12, 16 The mean age of these patients was significantly (14.7 years) older than the remainder of the TSCI population, with falls in patients over the age of 65 more likely to be from a lower height. As a result, this trend can likely be attributed to low domestic falls occurring in the ageing population. In countries where the population is predicted to age it can be expected that there will be an increase in the proportion of TSCIs caused by falls.
The high proportion of TSCIs caused by falls in Scotland is influenced by low number of TSCIs caused by assault (2.9% Scotland, 12% USA6) and DSH (2.4% Scotland, 6.8% Denmark31). Notably, 36% of TSCIs caused by DSH in Scotland occurred in females, agreeing with previous studies reporting a greater proportion of females being treated for TSCI after DSH compared with the general SCI population.15, 31, 32 This may be because males use methods of DSH that do not cause SCI or have a greater risk of mortality.33 Despite RTCs being the leading cause of TSCI worldwide,5 in Scotland, as with much of Europe,11, 14, 17, 18 rates of TSCI caused by road traffic collision are lower than that caused by falls. As well as increasing rates of TSCI caused by falls amongst the elderly, possible further explanations for this are a lower average passenger miles of exposure, greater use of seat belts, or safer driving habits and road conditions.10
The mean age at injury for TSCI in Scotland (46.8 years) is higher than in much of Europe and the USA,13, 16, 17, 34 which may be related to a greater proportion of TSCIs caused by elderly domestic falls and a lower proportion caused by violence. The mean age at injury increased significantly over the study duration, with similar increases reported in Finland,17 Spain12 and the USA.34 In Scotland this trend mirrors an increasing median age of the general population (from 35 years in 199126 to 41 years in 201127), with an associated significant increase in the number of new patients with TSCI over the age of 50.
The proportion of new TSCIs occurring in males (75.2%) is within 5% of the rate found in the majority of studies in Europe.12, 14, 15, 16, 17, 30, 35 While this rate remained relatively stable throughout this study, the proportion of females suffering a TSCI was 8% greater for those over the age of 65 and 9% greater for those suffering TSCI from falls, compared with the general TSCI population. This agrees with previous studies that have suggested that the rates of TSCI among the elderly are more evenly split between males and females than for other age groups.10 For populations predicted to age, with an associated increase in the number of TSCIs caused by falls in the elderly, it is expected the proportion of females sustaining a TSCI will rise.
The proportion of new TSCIs in Scotland caused by a cervical injury (60.6%) is higher than in Spain (57%)35 and the USA (54%),8 while the significant longitudinal increase in the proportion of cervical injuries seen in Scotland has also been observed in Finland,17 Spain12 and the USA.36 In Scotland, the increase can be attributed to a significant increase in C1–C4 lesions, a trend also observed in the USA,34 which may be attributed to improved health care in the peri-accident and acute stage of injury.
While international comparisons of neurological deficit after TSCI are hampered by changing definitions and the assessment being conducted at different time points, the proportion of complete TSCIs (AIS A)21 on admission in Scotland between 1999 and 2013 (29.8%) appears to be similar to that reported in Finland (31.7%)17 and lower than that reported in Iceland (39%),16 Italy (54.7%)15 and the USA (48.7%).6 In Scotland, the statistically significant increase in AIS scores of C and D on admission may be due to the increased number of TSCIs caused by low domestic falls in the elderly population, which often results in a less severe neurological deficit than those injuries caused by other aetiologies.
As some patients with NTSCI in Scotland are treated in regional neurorehabilitation units, the incidence rates for NTSCI reported here and comparisons of incidence between NTSCI and TSCI must be made with caution. However, the demographic data is noteworthy when assessing the epidemiology of severe NTSCI. The mean age of patients with a new NTSCI in Scotland (51.8 years) is comparable to Italy (55 years).37 However, the 5-year difference in the mean age of patients with NTSCI and TSCI is lower than that found in Italy (13.9 years)15 and the USA (22.6 years).38 The percentage of males affected by NTSCI in Scotland (68.1%) is higher than in Italy (63.3%),37 Spain (53%)39 and the USA (47.6% and 50%).38, 40 However, the proportion of males with NTSCI appears to be decreasing, a trend also observed in Spain.39 However, when comparing such figures it is necessary to consider that the incidence of NTSCI is influenced by the age demographics and the health profile of the individual country along with availability and effectiveness of local health services.
Comparison of studies reporting the different demographics and aetiologies of NTSCI is made difficult by the reporting of different classifications, different admission policies and the fewer patients than TSCI studies.19 This is demonstrated by the fact that this study along with two studies from both Italy and the USA all report different leading causes of NTSCI.15, 37, 38, 40 However, the complexity of the classification of NTSCI should not mask the importance of the incidence of mild-to-moderate neurological deficits secondary to degenerative disease.
Impact of findings
If the trends reported here continue, the age at which TSCIs occur, the proportion of new injuries occurring in the elderly population and the proportion of cervical TSCIs will all continue to increase. Increased age at injury is associated with poorer functional outcomes41, 42 and increases in comorbidities and secondary complications.43 It has been reported that patients with a C1–C4 lesion spend 27% longer in acute care than patients with a C5–C8 lesion, and 77% longer than patients with paraplegia.44 In addition, the lifetime cost of care for a 25-year-old with a C1–C4 lesion is 30% greater than for a C5–C8 lesion and 89% greater than paraplegia.4 Therefore, these factors must be considered when planning future service provision for the changing SCI population, with the trends identified in this study likely to have a significant impact on the type and cost of rehabilitation and the long-term outcomes for this population.
The WHO predicts that RTCs will increase from the ninth leading cause of worldwide disability-adjusted life years in 2004 to the third leading cause in 2030, primarily due to increased motor vehicle ownership and use in low- and middle-income countries.45 While this is unlikely to affect Scotland or similar post industrial countries, any global changes in the demographics of TSCI caused by an increase in RTCs will be augmented by the changing trends in TSCI epidemiology reported here.
The majority of NTSCI are as a result of age related degenerative conditions. It can be assumed that the increasing age of the global population will lead to increasing rates of NTSCI, with a corresponding increase in demand for the delivery of acute care and rehabilitation for the NTSCI population. This population generally has better rehabilitation outcomes than those with TSCI, with secondary complications occurring less frequently and being of a less severe nature.40, 46, 47 However, annual health care costs among patients with TSCI and NTSCI are not significantly different.48 This must be considered when planning provision of care.
Limitations
People with an SCI who died before being admitted to the QENSIU were not included in this study, due to a lack of consistent data. Therefore, like all hospital based studies, the incidence rates reported in this manuscript may be an underestimate due to failure to capture peri-accident mortality.
Conclusion
This study presents a population-based study of SCI epidemiology over a 20-year period in a population of 5.3 million. In Scotland, the average age at injury, rates of high level cervical TSCI (C1–C4), the proportion of TSCIs resulting in an AIS score of C and D on admission and the proportion caused by falls all increased significantly over the study duration. While the incidence and causation of SCI varies globally and reflects the society, demographics and industrialisation of the country or region, the findings of this study are mirrored in many post industrial nations and highlight a pressing need for a change in TSCI service provision. These findings will have a significant long-term impact on health service design, research strategy and the increased need for long-term community support. This study also identifies a need for improvement in the documentation and classification of NTSCI, to enable more effective measurement of the burden of the disease on the community.
Data archiving
There were no data to deposit.
References
Anderson KD . Targeting recovery: priorities of the spinal cord-injured population. J Neurotrauma 2004; 21: 1371–1383.
Furlan JC, Noonan V, Singh A, Fehlings MG . Assessment of impairment in patients with acute traumatic spinal cord injury: a systematic review of the literature. J Neurotrauma 2011; 28: 1445–1477.
Strauss DJ, Devivo MJ, Paculdo DR, Shavelle RM . Trends in life expectancy after spinal cord injury. Arch Phys Med Rehabil 2006; 87: 1079–1085.
Cao Y, Chen Y, DeVivo MJ . Lifetime direct costs after spinal cord injury. Top Spinal Cord Inj Rehabil 2011; 16: 10–16.
Singh A, Tetreault L, Kalsi-Ryan S, Nouri A, Fehlings MG . Global prevalence and incidence of traumatic spinal cord injury. Clin Epidemiol 2014; 6: 309–331.
DeVivo MJ . Epidemiology of spinal cord injury. In: Lin VW . (ed). Spinal Cord Medicine Principles and Practice.: Demos Medical Publishing: New York, NY, USA. 2010, pp 78–84.
Nobunaga AI, Go BK, Karunas RB . Recent demographic and injury trends in people served by the Model Spinal Cord Injury Care Systems. Arch Phys Med Rehabil 1999; 80: 1372–1382.
Jackson AB, Dijkers M, Devivo MJ, Poczatek RB . A demographic profile of new traumatic spinal cord injuries: change and stability over 30 years. Arch Phys Med Rehabil 2004; 85: 1740–1748.
DeVivo MJ . Sir Ludwig Guttmann Lecture: trends in spinal cord injury rehabilitation outcomes from model systems in the United States: 1973-2006. Spinal Cord 2007; 45: 713–721.
DeVivo MJ . Epidemiology of traumatic spinal cord injury: trends and future implications. Spinal Cord 2012; 50: 365–372.
Hagen EM, Eide GE, Rekand T, Gilhus NE, Gronning M . A 50-year follow-up of the incidence of traumatic spinal cord injuries in Western Norway. Spinal Cord 2010; 48: 313–318.
van den Berg M, Castellote JM, Mahillo-Fernandez I, de Pedro-Cuesta J . Incidence of traumatic spinal cord injury in Aragon, Spain (1972-2008). J Neurotrauma 2011; 28: 469–477.
Sabre L, Hagen EM, Rekand T, Asser T, Korv J . Traumatic spinal cord injury in two European countries: why the differences? Eur J Neurol 2013; 20: 293–299.
Soopramanien A . Epidemiology of spinal injuries in Romania. Paraplegia 1994; 32: 715–722.
Celani MG, Spizzichino L, Ricci S, Zampolini M, Franceschini M, Retrospective Study Group on SCI. Spinal cord injury in Italy: a multicenter retrospective study. Arch Phys Med Rehabil 2001; 82: 589–596.
Knutsdottir S, Thorisdottir H, Sigvaldason K, Jonsson H Jr., Bjornsson A, Ingvarsson P . Epidemiology of traumatic spinal cord injuries in Iceland from 1975 to 2009. Spinal Cord 2012; 50: 123–126.
Ahoniemi E, Alaranta H, Hokkinen EM, Valtonen K, Kautiainen H . Incidence of traumatic spinal cord injuries in Finland over a 30-year period. Spinal Cord 2008; 46: 781–784.
Sabre L, Pedai G, Rekand T, Asser T, Linnamagi U, Korv J . High incidence of traumatic spinal cord injury in Estonia. Spinal Cord 2012; 50: 755–759.
Bickenbach J, Boldt I, Brinkhof M, Chamberlain J, Cripps R, Fitzharris M et al. A global picture of spinal cord injury. In: Bickenbach J (ed.). International Perspectives on Spinal Cord Injury. Geneva, Switzerland. 2013, pp 11–42.
Queen Elizabeth National Spinal Injuries Unit. Annual Report 2013–2014. Glasgow, Scotland, 2013.
Kirshblum SC, Burns SP, Biering-Sorensen F, Donovan W, Graves DE, Jha A et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med 2011; 34: 535–546.
ICECI Coordination and Maintenance Group International Classification of External Causes of Injuries (ICECI) version 1.2. Consumer Safety Institute and AIHW National Injury Surveillance Unit: Adelaide, Australia. 2004.
Biering-Sorensen F, Charlifue S, DeVivo M, Noonan V, Post M, Stripling T et al. International Spinal Cord Injury Data Sets. Spinal Cord 2006; 44: 530–534.
New PW, Marshall R . International Spinal Cord Injury Data Sets for non-traumatic spinal cord injury. Spinal Cord 2014; 52: 123–132.
Annual Report of the Registrar General of Births, Deaths and Marriages for Scotland 2013. 159th Edition ed: General Register Office for Scotland; 2014.
Scotland’s Census 1991, Age by single year: General Register Office for Scotland; 1991.
Scotland’s Census 2011, QS103SC- Age by single year: National Records of Scotland; 2011.
DeVivo MJ, Biering-Sorensen F, New P, Chen Y . International Spinal Cord Injury Data Sets. Standardization of data analysis and reporting of results from the International Spinal Cord Injury Core Data Set. Spinal Cord 2011; 49: 596–599.
Lee BB, Cripps RA, Fitzharris M, Wing PC . The global map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate. Spinal Cord 2014; 52: 110–116.
Martins F, Freitas F, Martins L, Dartigues JF, Barat M . Spinal cord injuries—epidemiology in Portugal's central region. Spinal Cord 1998; 36: 574–578.
Biering-Sørensen F, Pedersen W, Müller PG . Spinal cord injury due to suicide attempts. Paraplegia 1992; 30: 139–144.
Anderson J, Allan DB . Vertebral fracture secondary to suicide attempt: demographics and patient outcome in a Scottish spinal rehabilitation unit. J Spinal Cord Med 2011; 34: 380–387.
Stark C, Hopkins P, Gibbs D, Rapson T, Belbin A, Hay A . Trends in suicide in Scotland 1981 - 1999: age, method and geography. BMC Public Health 2004; 4: 49.
DeVivo MJ, Chen Y . Trends in new injuries, prevalent cases, and aging with spinal cord injury. Arch Phys Med Rehabil 2011; 92: 332–338.
Perez K, Novoa AM, Santamarina-Rubio E, Narvaez Y, Arrufat V, Borrell C et al. Incidence trends of traumatic spinal cord injury and traumatic brain injury in Spain, 2000-2009. Accid Anal Prev 2012; 46: 37–44.
Ho CH, Wuermser LA, Priebe MM, Chiodo AE, Scelza WM, Kirshblum SC . Spinal cord injury medicine. 1. Epidemiology and classification. Arch Phys Med Rehabil 2007; 88: S49–S54.
Citterio A, Franceschini M, Spizzichino L, Reggio A, Rossi B, Stampacchia G et al. Nontraumatic spinal cord injury: an Italian survey. Arch Phys Med Rehabil 2004; 85: 1483–1487.
McKinley WO, Seel RT, Hardman JT . Nontraumatic spinal cord injury: incidence, epidemiology, and functional outcome. Arch Phys Med Rehabil 1999; 80: 619–623.
van den Berg ME, Castellote JM, Mahillo-Fernandez I, de Pedro-Cuesta J . Incidence of nontraumatic spinal cord injury: a Spanish cohort study (1972-2008). Arch Phys Med Rehabil 2012; 93: 325–331.
Ones K, Yilmaz E, Beydogan A, Gultekin O, Caglar N . Comparison of functional results in non-traumatic and traumatic spinal cord injury. Disabil Rehabil 2007; 29: 1185–1191.
Rodakowski J, Skidmore ER, Anderson SJ, Begley A, Jensen MP, Buhule OD et al. Additive effect of age on disability for individuals with spinal cord injuries. Arch Phys Med Rehabil 2014; 95: 1076–1082.
Wilson JR, Davis AM, Kulkarni AV, Kiss A, Frankowski RF, Grossman RG et al. Defining age-related differences in outcome after traumatic spinal cord injury: analysis of a combined, multicenter dataset. Spine J 2014; 14: 1192–1198.
DeVivo MJ, Kartus PL, Rutt RD, Stover SL, Fine PR . The influence of age at time of spinal cord injury on rehabilitation outcome. Arch Neurol 1990; 47: 687–691.
DeVivo MJ, Chen Y, Mennemeyer ST, Deutsch A . Costs of Care Following Spinal Cord Injury. Top Spinal Cord Inj Rehabil 2011; 16: 1–9.
The Global Burden of Disease: 2004 Update. World Health Orginazation: Geneva, Switzerland. 2008.
McKinley WO, Tewksbury MA, Godbout CJ . Comparison of medical complications following nontraumatic and traumatic spinal cord injury. J Spinal Cord Med 2002; 25: 88–93.
New PW, Rawicki HB, Bailey MJ . Nontraumatic spinal cord injury: demographic characteristics and complications. Arch Phys Med Rehabil 2002; 83: 996–1001.
St. Andre JR, Smith BM, Stroupe KT, Burns SP, Evans CT, Cowper Ripley D et al. A comparison of costs and health care utilization for veterans with traumatic and nontraumatic spinal cord injurya comparison of costs and health care utilization for veterans with traumatic and nontraumatic spinal cord injury. Top Spinal Cord Inj Rehabil 2011; 16: 27–42.
Acknowledgements
The authors would like to thank all the QENSIU staff involved in maintaining the database and the Scottish Government Health Directorates for funding to help support this work (EJM).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Spinal Cord website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
McCaughey, E., Purcell, M., McLean, A. et al. Changing demographics of spinal cord injury over a 20-year period: a longitudinal population-based study in Scotland. Spinal Cord 54, 270–276 (2016). https://doi.org/10.1038/sc.2015.167
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sc.2015.167
- Springer Nature Limited
This article is cited by
-
The impact of COVID-19 and associated lockdowns on traumatic spinal cord injury incidence: a population based study
Spinal Cord (2024)
-
Spinal cord injury as a result of Staphylococcus aureus pyogenic spinal infection complicating infected atopic eczema: two case reports
Spinal Cord Series and Cases (2023)
-
A systematic review and meta-analysis of the global epidemiology of pediatric traumatic spinal cord injuries
European Journal of Pediatrics (2023)
-
Is procalcitonin a reliable indicator of sepsis in spinal cord injury patients: an observational cohort study
European Spine Journal (2023)
-
The value of the whole picture: rehabilitation outcome measurement using patient self-report and clinician-based assessments after spinal cord injury
Spinal Cord (2022)