Abstract
To date and to the best of our knowledge, there have been limited studies on the risk factor of clavicle fracture combined with congenital muscular torticollis (CMT), despite it being the most common fracture in newborns. So, the aim of this study was to investigate the risk factors associated with clavicular fracture combined with CMT, and its effect on prognosis. In this study, a total of 134 infants with CMT were included. The risk factors associated with clavicular fracture combined with CMT were analyzed. To analyze the correlation between the clinical parameters and the clavicular fracture in patients with CMT, demographic data, such as body weight at birth, maternal age, gender, gestational age, delivery method, sternocleidomastoid (SCM) thickness of ipsilateral side, its ratio between the ipsilateral and contralateral side, and the first visitation date after birth were evaluated. In the results of this study, the clavicular fracture was found in 15 of 134 patients with CMT (19%). In multivariate logistic analysis, the body weight at birth was the only significant parameter for predicting clavicular fracture in patients with CMT (p-value < 0.05). However, there was no significant difference of treatment duration between CMT infants with or without clavicular fracture. In infants with CMT, the area under the ROC curve of the body weight at birth for predicting clavicular fracture was 0.659 (95% CI, 0.564–0.745.; p < 0.05). The optimal cut-off value obtained from the maximum Youden index J was 3470 g (sensitivity: 57.14%, specificity: 75.76%), and the odd ratio of clavicular fracture in patients with CMT increased by 1.244 times for every 100 g of body weight at birth. In conclusion, birth weight appears to be a clinical predictor of clavicular fracture in infants with CMT. More studies and discussions are needed on whether any screening should be recommended for detecting the concurrent clavicular fracture in subjects with CMT.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Introduction
Congenital muscular torticollis (CMT) is one of the most common musculoskeletal problems in children, and the overall incidence rate can be as high as 1:250 live births1,2. The reported incidence rate varied from 0.3 to 16.0%1,2,3,4,5. CMT is a group of clinical presentations caused by the shortening of the unilateral sternocleidomastoid muscle (SCM), which begins during the prenatal or perinatal period6,7. CMT can usually be subdivided into two phenotypes2; (1) the sternocleidomastoid tumor (SMT) type, which consists of torticollis with a palpable tumor (fibromatosis colli), and (2) the muscular torticollis, which consists of torticollis with a tightness of SCM without a palpable mass. The former is a mass that may be tender to palpation and decreases in size within the first year after birth. And postural torticollis (PT) may be classified as one of subtypes of CMT, although there are differences between studies2,3.
Congenital muscular torticollis (CMT) is known to occur concurrently with other conditions, including brachial plexus injury (BPI), developmental dysplasia of the hip (DDH), or clavicular fracture8,9,10,11. In previous study, the incidence of perinatal torticollis occurring concurrently with neonatal BPI was 43%9. And the incidence of perinatal torticollis occurring concurrently with neonatal BPI ranged from 2% to 19%11. To date and to the best of our knowledge, there have been limited studies on the risk factor of clavicle fracture combined with CMT, despite it being the most common fracture in newborns12. Although one previous study showed that clavicular fracture tends to develop on the contralateral side of CMT, the risk factors of clavicular fracture in patients with CMT have not been fully evaluated6. Therefore, the aim of this study was to investigate the risk factors associated with clavicular fracture in infants with CMT and its effect on prognosis.
Material and Method
Ethics statement
This study was approved by the Institutional Review Board of Daegu Fatima Hospital. Declaration of Helsinki protocols are being followed, and informed consent was obtained from a parent and/or legal guardian.
Patients
Between January 2016 and June 2018, subjects who visited our rehabilitation outpatient clinic due to abnormal posture of the head and neck were included. The medical records along with radiological findings were reviewed. Among them, subjects who met the following criteria were excluded: (1) subjects with no specific finding on ultrasonography; (2) subjects who did not undergo plain radiography of the cervical spine and/or clavicles.
CMT was diagnosed when subjects met the following criteria: (1) thickness of the involved SCM ≥ 2 mm greater than that of the contralateral side, along with increased echogenicity on ultrasonography13; and (2) subjects who showed shortening of the unilateral SCM since childhood, ending up with a limitation of passive range of rotation of the chin toward ipsilateral shoulder and/or limitation of passive range of lateral flexion toward contralateral shoulder. Plain radiographs (X-ray) of the cervical spines and/or clavicles were evaluated, using the reference set to any clavicular fracture and any structural abnormalities on cervical spine. Clavicular fracture was diagnosed when the fracture lines and/or callus were detectable by a naked eye on the clavicle on antero-posterior plain radiographs of the cervical spines and/or clavicles6 and confirmed by radiologists who were specialized at musculoskeletal disease. Therefore, we retrospectively reviewed the medical records of 134 patients with congenital muscular torticollis in the rehabilitation unit.
Parameters associated with clavicular fracture in CMT patients
Demographic data, such as body weight at birth, maternal age, gender, gestational age, delivery method, SCM thickness of ipsilateral side, and its ratio between the ipsilateral and contralateral side, treatment duration, in addition to the first visitation date after birth, were collected by reviewing the medical records.
Statistical analysis
To find the difference of the demographic data between CMT patients with and without clavicular fracture, an independent T-test, Fisher’s exact test, or chi-square test were performed. In addition, to analyze the correlation between the clinical parameters and the clavicular fracture in patients with CMT, multivariate logistic analysis through forward stepwise selection was then performed. To evaluate the accuracy of predictive factors for clavicular fracture in CMT patients, we performed a receiver operating characteristic (ROC) analysis in each group. All statistical analyses were conducted using MedCalc and SPSS version. 22.0 (IBM, Armonk, NY, USA).
Results
Demographics and concurrence rate of CMT and clavicular fracture
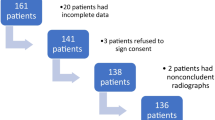
Between January 2016 and June 2018, 449 patients visited our rehabilitation outpatient clinic due to abnormal posture of the head and neck. The medical records along with radiological findings were reviewed. Among them, 315 subjects who met the exclusion criteria were excluded (Fig. 1). Finally, a total 134 infants with CMT were included in this study. Moreover, the clavicular fracture was found in 15 of 134 infants, with the concurrent rate being 11.19% (Table 1).
Contralateral involvement of CMT and clavicular fracture
CMT and clavicular fracture occurred on the opposite side of each other in 13 out of 15 subjects (86.7%; Table 2). Table 2 is the contingency table between the side of CMT and the side of clavicular fracture. In chi-square analysis, discordance of side between CMT and clavicular fracture was significant (P = 0.004).
Risk factor of clavicular fracture in infants with CMT
In a comparison of the demographic data between CMT infants with or without clavicular fracture, there was a significant difference in delivery mode (p-value < 0.05) (Table 1). There was a significant difference in the birth weight between CMT infants with or without clavicular fracture (p-value < 0.05) (Table 1). However, there was no significant difference in the maternal age, gestational age, SCM thickness ratio, first visitation to the clinic, and gender. In a multivariate logistic analysis, the birth weight was the only significant parameter for predicting clavicular fracture in CMT infants (p-value < 0.05) (Table 1). In infants with CMT, the area under the ROC curve of the birth weight for predicting clavicular fracture was 0.659 (95% CI, 0.564–0.745.; p < 0.05) (Table 3). The optimal cut-off value obtained from the maximum Youden index J was 3470 g (sensitivity: 57.14%, specificity: 75.76%), and the odd ratio of clavicular fracture in CMT infants increased by 1.244 times for every 100 g of birth weight (Fig. 2).
In patients with CMT, the area under the ROC curve of the body weight at birth for predicting clavicular fracture was 0.659 (95% CI, 0.564–0.745.; p < 0.05). The optimal cut-off value obtained from the maximum Youden index J was 3470 g (sensitivity: 57.14%, specificity: 75.76%), and the odd ratio of clavicular fracture in patients with CMT increased by 1.244 times at every 100 g of body weight at birth.
Clinical parameters correlated with treatment duration
There was no significant difference of treatment duration between CMT infants with or without clavicular fracture. (Table 1) In a multivariate regression analysis, the SCM thickness ratio was the only significant parameter for predicting treatment duration in infants with CMT (p-value < 0.05) (Table 4).
Discussion
The causes of CMT remain contentious to date2. Multiple theories exist, including intrauterine crowding8,14 or fibrosis from peripartum bleeding, vascular phenomenon, primary myopathy of the SCM, and compartment syndrome15,16. A difficult birth history has been reported in 30–60% of patients with CMT17,18. In a study of 996 patients with CMT, Yim et al.6 suggested a hypothesis that CMT may likely develop during vaginal delivery. For an effective expulsion of the baby’s head during vaginal delivery, the antero-posterior axis of baby’s head needs to be parallel with the antero-posterior axis of the mother’s pelvis, by simultaneous internal rotation of both the head and trunk of the baby, in addition to neck flexion6. Moreover, external rotation of the shoulder occurs so that the right-left axis of the baby’s shoulders becomes parallel to the antero-posterior axes of the mother’s pelvis for expulsion of the baby’s shoulder6. However, Yim et al.6 suggested that an isolated internal rotation of the baby’s head that occurs during head expulsion, instead of simultaneous internal rotation of both the head and shoulder, can cause overstretching and damages to SCM. Moreover, they also suggested that a downward traction of the assistive maneuver, which may facilitate delayed delivery of the baby’s shoulder, may cause fracture of the clavicle (contralateral side of damaged SCM), which is in the anterior shoulder. As aforementioned, clavicular fracture is significantly correlated with vaginal delivery and body weight at birth. The suggestions made by Yim et al. and our findings support that clavicular fractures in patients with CMT are associated with difficult vaginal delivery. Interestingly, however, there was no significant difference of treatment duration between CMT infants with or without clavicular fracture. In this study, the only risk factor correlated with treatment duration was SCM thickness ratio.
Although other theories aside from difficult vaginal delivery, such as vascular phenomenon, primary myopathy of the SCM, compartment syndrome, hereditary hypothesis, and infection, have also been proposed, the pathogenesis of CMT remains uncertain. Injury to the SCM muscle can occur as a result of muscle disease, such as muscular dystrophy, exposure to myotoxic agents, ischemia, and exposure to hot or cold temperatures19. However, focal myopathy in the SCM muscle may be rare, and neonates of uncomplicated pregnancy may rarely have events causing injury to the SCM muscle, such as exposure to hot or cold temperatures and ischemia. In addition, our data, which shows the correlation between clavicular fracture in patients with CMT and body weight at birth, suggests that mechanical injury to SCM by overstretching – as a result of difficult delivery – could cause ischemia, compartment syndrome, and/or hematoma of SCM that have been known to be related to the development of CMT. However, CMT occurs not only in subjects born through vaginal delivery, but also in those born through cesarean section. Therefore, other causes should not be excluded.
The incidence of clavicular fractures in newborns ranges from 0.01 to 1.65 percent, and the incidence of clavicular fracture in patients with CMT in the study of 996 patients with CMT was 2.01%6,20,21,22,23. Considering the prevalence of CMT, the prevalence of clavicle fractures in CMT patients is very low in infants as a whole. However, in our study, the incidence of clavicular fracture in patients with CMT was 11.19%. This is likely due to two reasons: First, we did not perform routine x-ray examinations for clavicular fractures in all CMT children, but performed in patients with suspected clavicular fractures on physical examination, such as decreased Moro reflex, swelling, mass, tenderness, and crepitation of the affected side. However, in our study, only CMT patients who received x-rays were enrolled; the incidence of clavicular fracture in CMT patients seems to be higher than in previous studies. Second, more complicated SCM patients tend to be admitted to our hospital, as they are referred from local primary clinics due to the nature of the medical system in Korea. However, considering the relatively high incidence rate of clavicular fracture in CMT patients and the association between clavicular fracture and increased body weight at birth, a more thorough evaluation seems necessary. In this study, only a conservative treatment was performed in CMT patients with clavicular fracture, except for the incorporation of stretching exercise and home education for CMT. On follow-up plain radiography, however, most of the CMT patients with clavicular fracture showed a tendency to recover well without deformation of the clavicle (Figs 3 and 4).
An infant who visited our hospital for left torticollis. In ultrasound examination, there was muscular fibromatosis in right SCM. (A) At 4 days after birth, left clavicular fracture was seen (arrow). (B) Follow-up plain radiograph at 21 days after birth. A callus formation was seen around fracture site of left clavicle (arrowhead). For clavicular fracture, only a conservative treatment was performed except stretching exercise and home education for right CMT. (C) Follow-up plain radiograph at 22 month after birth. Callus formation was disappeared, and it is difficult to find the difference between left and right clavicle. CMT; congenital muscular torticollis, SCM; sternocleidomastoid.
An infant who visited our hospital for left torticollis at 1 month after birth. In ultrasound examination, there was muscular fibromatosis in left SCM. (A) At 1 month after birth, callus formation around the fracture site of right clavicle was seen (arrow). For clavicular fracture, only a conservative treatment was performed except stretching exercise and home education for left CMT. (B) Follow-up plain radiograph at 4 month after birth. Callus formation was nearly disappeared, and it is difficult to find the difference between left and right clavicle (arrowhead).
There are several limitations in our study. First, the number of CMT patients with clavicular fracture included was relatively small. However, since clavicular fracture in patients with CMT is rare, this study, evaluating its risk factors, may be meaningful. In the future, further studies with a large number of patients may be necessary to better evaluate the risk factors of clavicular fracture in CMT patients. Second, selection bias may be present due to the retrospective nature of this study. As aforementioned, we did not perform radiologic evaluation on all CMT children; These may have impacted our incidence rate of clavicular fracture in patients with CMT. However, to the best of our knowledge, this is the first report on the risk factor of clavicular fracture in infants with CMT. The results of our study may be helpful in diagnosing clavicular fracture in CMT infants by informing clinicians with the relevant risk factors for clavicular fractures that may be under-diagnosed.
Conclusions
This is the first report on the risk factors of clavicular fracture in CMT infants and its effect on prognosis. Birth weight can be a clinical predictor for clavicular fracture in CMT infants. However, presence of clavicular fracture is not associated with treatment duration. This study suggests that physiatrists need to be aware of the possibility of a clavicular fracture in CMT infants when the birth weight is greater than 3470 g. More studies and discussions are needed on whether screening test should be recommended for detecting the concurrent clavicular fracture in CMT infants.
References
Cheng, J. C. & Au, A. W. Infantile torticollis: a review of 624 cases. Journal of pediatric orthopedics 14, 802–808 (1994).
Do, T. T. Congenital muscular torticollis: current concepts and review of treatment. Current opinion in pediatrics 18, 26–29, https://doi.org/10.1097/01.mop.0000192520.48411.fa (2006).
Nilesh, K. & Mukherji, S. Congenital muscular torticollis. Annals of maxillofacial surgery 3, 198–200, https://doi.org/10.4103/2231-0746.119222 (2013).
Stellwagen, L., Hubbard, E., Chambers, C. & Jones, K. L. Torticollis, facial asymmetry and plagiocephaly in normal newborns. Archives of disease in childhood 93, 827–831, https://doi.org/10.1136/adc.2007.124123 (2008).
Aarnivala, H. E., Valkama, A. M. & Pirttiniemi, P. M. Cranial shape, size and cervical motion in normal newborns. Early human development 90, 425–430, https://doi.org/10.1016/j.earlhumdev.2014.05.007 (2014).
Yim, S. Y., Chang, K., Ahn, A. R., Park, E. J. & Kim, J. Contralateral Involvement of Congenital Muscular Torticollis and Clavicular Fracture. American journal of physical medicine & rehabilit ation 97, 375–378, https://doi.org/10.1097/PHM.0000000000000862 (2018).
Kim, M. Y., Kwon, D. R. & Lee, H. I. Therapeutic effect of microcurrent therapy in infants with congenital muscular torticollis. PM & R: the journal of injury, function, and rehabilitation 1, 736–739, https://doi.org/10.1016/j.pmrj.2009.06.008 (2009).
Lee, S. J. et al. Comparison of clinical severity of congenital muscular torticollis based on the method of child birth. Annals of rehabilitation medicine 35, 641–647, https://doi.org/10.5535/arm.2011.35.5.641 (2011).
Hervey-Jumper, S. L., Justice, D., Vanaman, M. M., Nelson, V. S. & Yang, L. J. Torticollis associated with neonatal brachial plexus palsy. Pediatric neurology 45, 305–310, https://doi.org/10.1016/j.pediatrneurol.2011.08.013 (2011).
Nath, R. K., Avila, M. B., Karicherla, P. & Somasundaram, C. Assessment of triangle tilt surgery in children with obstetric brachial plexus injury using the pediatric outcomes data collection instrument. The open orthopaedics journal 5, 385–388, https://doi.org/10.2174/1874325001105010385 (2011).
von Heideken, J. et al. The relationship between developmental dysplasia of the hip and congenital muscular torticollis. Journal of pediatric orthopedics 26, 805–808, https://doi.org/10.1097/01.bpo.0000235398.41913.51 (2006).
Rutgers, R. A., Bilo, R. A., Nijs, H. G., Bosschaart, A. N. & van Rijn, R. R. [Fractures in full-term neonates]. Nederlands tijdschrift voor geneeskunde 151, 1043; author reply 1043–1044 (2007).
Yim, S. Y. et al. The laryngeal cough reflex in congenital muscular torticollis: is it a new finding? American journal of physical medicine & rehabilitation 89, 147–152, https://doi.org/10.1097/PHM.0b013e3181b7275b (2010).
Lee, Y. T. et al. Risk factors for intrauterine constraint are associated with ultrasonographically detected severe fibrosis in early congenital muscular torticollis. Journal of pediatric surgery 46, 514–519, https://doi.org/10.1016/j.jpedsurg.2010.08.003 (2011).
Davids, J. R., Wenger, D. R. & Mubarak, S. J. Congenital muscular torticollis: sequela of intrauterine or perinatal compartment syndrome. Journal of pediatric orthopedics 13, 141–147 (1993).
Tang, S., Liu, Z., Quan, X., Qin, J. & Zhang, D. Sternocleidomastoid pseudotumor of infants and congenital muscular torticollis: fine-structure research. Journal of pediatric orthopedics 18, 214–218 (1998).
Hollier, L., Kim, J., Grayson, B. H. & McCarthy, J. G. Congenital muscular torticollis and the associated craniofacial changes. Plastic and reconstructive surgery 105, 827–835 (2000).
Cheng, J. C. et al. Clinical determinants of the outcome of manual stretching in the treatment of congenital muscular torticollis in infants. A prospective study of eight hundred and twenty-one cases. The Journal of bone and joint surgery. American volume 83-A, 679–687 (2001).
Seo, S. J. et al. Is craniofacial asymmetry progressive in untreated congenital muscular torticollis? Plastic and reconstructive surgery 132, 407–413, https://doi.org/10.1097/PRS.0b013e3182959e30 (2013).
Bhat, B. V., Kumar, A. & Oumachigui, A. Bone injuries during delivery. Indian journal of pediatrics 61, 401–405 (1994).
Beals, R. K. & Sauser, D. D. Nontraumatic disorders of the clavicle. The Journal of the American Academy of Orthopaedic Surgeons 14, 205–214 (2006).
Kaplan, B. et al. Fracture of the clavicle in the newborn following normal labor and delivery. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics 63, 15–20 (1998).
Lurie, S., Wand, S., Golan, A. & Sadan, O. Risk factors for fractured clavicle in the newborn. The journal of obstetrics and gynaecology research 37, 1572–1574, https://doi.org/10.1111/j.1447-0756.2011.01576.x (2011).
Acknowledgements
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT and Future Planning (NRF- 2017R1D1A1B03033127). No commercial party having a direct financial interest in the results of the research supporting this article has or will confer a benefit upon the authors or upon any organization with which the authors are associated.
Author information
Authors and Affiliations
Contributions
Joo Young Cho: Analysis of data, writing a manuscript. Zeeihn Lee: Study concept and design. Jong Min Kim: revision of manuscript. Byung Joo Lee: revision of manuscript. Donghwi Park: Study concept and design, and critical revision of manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lee, Z., Cho, J.Y., Lee, B.J. et al. Body Weight at Birth: The Only Risk Factor Associated with Contralateral Clavicular Fracture in Patients with Congenital Muscular Torticollis. Sci Rep 9, 13801 (2019). https://doi.org/10.1038/s41598-019-50370-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-50370-2
- Springer Nature Limited