Abstract
Background
Obesity and kidney damage have been closely linked in adults, but little is still known in childhood.
Objective
To identify predictors of kidney damage in children with metabolically healthy (MHO) and metabolically unhealthy (MUO) obesity phenotypes.
Methods
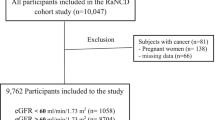
We retrospectively examined 396 children with obesity (mean age 10.72 ± 2.71 years, body mass index-standard deviation score, BMI-SDS, 2.23 ± 0.57) stratified according to metabolic phenotypes. Kidney damage was defined as the presence of reduced estimated glomerular filtration rate (eGFR < 90 mL/min/1.73m2) and/or albuminuria (≥ 30 mg/g urinary creatinine).
Results
Kidney damage was found in 20.9% of the study population. Children with kidney damage had higher BMI-SDS, homeostasis model assessment of insulin resistance (HOMA-IR), and inflammation markers levels and increased prevalence of non-alcoholic fatty liver disease (NAFLD) than those without kidney damage (all p < 0.005). MUO and MHO subjects had respectively an odds ratio (OR) to show kidney damage of of 1.92 (95%CI:1.22–3.01; p = 0.005) and 1.05 (95%CI:1.00–1.09; p = 0.028) after adjustments. Moreover, we found that only HOMA-IR was closely associated to kidney damage in MUO group (OR = 2.07;95%CI:1.20–3.57; p = 0.007), while HOMA-IR (OR = 1.15;95%CI:1.02–1.29; p = 0.011) and uric acid (OR = 1.15;95% CI:1.02–1.30; p = 0.010) were the only significant risk factors for kidney damage in MHO group.
Conclusion
An increased risk of kidney damage has been observed in children with obesity and in particular in those with MUO phenotype. As their role on kidney function, HOMA-IR should be monitored in MUO children and both HOMA-IR and uric acid in MHO children.
Access this article
We’re sorry, something doesn't seem to be working properly.
Please try refreshing the page. If that doesn't work, please contact support so we can address the problem.

Similar content being viewed by others
Data availability
The data presented in this study are available on request from the corresponding author. The data are not publicly available due to the presence of information that could compromise research participant privacy.
References
Jebeile H, Kelly AS, O’Malley G, Baur LA. Obesity in children and adolescents: epidemiology, causes, assessment, and management. Lancet Diabetes Endocrinol. 2022;10:351–65.
Di Bonito P, Pacifico L, Licenziati MR, Maffeis C, Morandi A, Manco M, et al. Elevated blood pressure, cardiometabolic risk and target organ damage in youth with overweight and obesity. Nutr Metab Cardiovasc Dis. 2020;30:1840–7.
Marzuillo P, Grandone A, Di Sessa A, Guarino S, Diplomatico M, Umano GR, et al. Anthropometric and Biochemical Determinants of Estimated Glomerular Filtration Rate in a Large Cohort of Obese Children. J Ren Nutr. 2018;28:359–62.
Eslam M, Alkhouri N, Vajro P, Baumann U, Weiss R, Socha P, et al. Defining paediatric metabolic (dysfunction)-associated fatty liver disease: an international expert consensus statement. Lancet Gastroenterol Hepatol. 2021;6:864–73.
Di Sessa A, Guarino S, Umano GR, Arenella M, Alfiero S, Quaranta G, et al. MAFLD in Obese Children: A Challenging Definition. Children (Basel). 2021;8:247.
Lonardo A, Mantovani A, Lugari S, Targher G. Epidemiology and pathophysiology of the association between NAFLD and metabolically healthy or metabolically unhealthy obesity. Ann Hepatol. 2020;19:359–66.
Genovesi S, Antolini L, Orlando A, Gilardini L, Bertoli S, Giussani M, et al. Cardiovascular Risk Factors Associated With the Metabolically Healthy Obese (MHO) Phenotype Compared to the Metabolically Unhealthy Obese (MUO) Phenotype in Children. Front Endocrinol (Lausanne). 2020;11:27.
Damanhoury S, Newton AS, Rashid M, Hartling L, Byrne JLS, Ball GDC. Defining metabolically healthy obesity in children: a scoping review. Obes Rev. 2018;19:1476–91.
Di Bonito P, Miraglia Del Giudice E, Chiesa C, Licenziati MR, Manco M, Franco F, et al. Preclinical signs of liver and cardiac damage in youth with metabolically healthy obese phenotype. Nutr Metab Cardiovasc Dis. 2018;28:1230–6.
Eckel N, Meidtner K, Kalle-Uhlmann T, Stefan N, Schulze MB. Metabolically healthy obesity and cardiovascular events: A systematic review and meta-analysis. Eur J Prev Cardiol. 2016;23:956–66.
Rhee CM, Ahmadi SF, Kalantar-Zadeh K. The dual roles of obesity in chronic kidney disease: a review of the current literature. Curr Opin Nephrol Hypertens. 2016;25:208–16.
Panwar B, Hanks LJ, Tanner RM, Muntner P, Kramer H, McClellan WM, et al. Obesity, metabolic health, and the risk of end-stage renal disease. Kidney Int. 2015;87:1216–22.
Savino A, Pelliccia P, Chiarelli F, Mohn A. Obesity-related renal injury in childhood. Horm Res Paediatr. 2010;73:303–11.
Di Bonito P, Di Sessa A. New Diagnostic Criteria for Hypertension in Children and Adolescents: Lights and Shadows. Children (Basel). 2020;7:196.
Martinez-Montoro JI, Morales E, Cornejo-Pareja I, Tinahones FJ, Fernandez-Garcia JC. Obesity-related glomerulopathy: Current approaches and future perspectives. Obes Rev. 2022;23:e13450.
Castro BBA, Foresto-Neto O, Saraiva-Camara NO, Sanders-Pinheiro H. Renal lipotoxicity: Insights from experimental models. Clin Exp Pharmacol Physiol. 2021;48:1579–88.
Colasante AM, Bartiromo M, Nardolillo M, Guarino S, Marzuillo P, Mangoni di SSG, et al. Tangled relationship between insulin resistance and microalbuminuria in children with obesity. World J Clin Pediatr. 2022;11:455–62.
Abdelhafiz AH, Ahmed S, El Nahas M. Microalbuminuria: marker or maker of cardiovascular disease. Nephron Exp Nephrol. 2011;119:e6–10.
Andrassy KM. Comments on ‘KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease’. Kidney Int. 2013;84:622–3.
Kovesdy CP, Furth SL, Zoccali C. World Kidney Day Steering C. Obesity and Kidney Disease: Hidden Consequences of the Epidemic. Can J Kidney Health Dis. 2017;4:2054358117698669.
Kotsis V, Martinez F, Trakatelli C, Redon J. Impact of Obesity in Kidney Diseases. Nutrients. 2021;13:4482.
Nawaz S, Chinnadurai R, Al-Chalabi S, Evans P, Kalra PA, Syed AA, et al. Obesity and chronic kidney disease: A current review. Obes Sci Pract. 2023;9:61–74.
Sanad M, Gharib A. Evaluation of microalbuminuria in obese children and its relation to metabolic syndrome. Pediatr Nephrol. 2011;26:2193–9.
Di Sessa A, Umano GR, Cirillo G, Passaro AP, Verde V, Cozzolino D, et al. Pediatric non-alcoholic fatty liver disease and kidney function: Effect of HSD17B13 variant. World J Gastroenterol. 2020;26:5474–83.
Flynn JT, Kaelber DC, Baker-Smith CM, Blowey D, Carroll AE, Daniels SR, et al. Clinical Practice Guideline for Screening and Management of High Blood Pressure in Children and Adolescents. Pediatrics. 2017;140:e20171904.
Gicchino MF, Di Sessa A, Guarino S, Miraglia Del Giudice E, Olivieri AN, Marzuillo P. Prevalence of and factors associated to chronic kidney disease and hypertension in a cohort of children with juvenile idiopathic arthritis. Eur J Pediatr. 2021;180:655–61.
Marzuillo P, Di Sessa A, Cirillo G, Umano GR, Pedulla M, La Manna A, et al. Transmembrane 6 superfamily member 2 167K allele improves renal function in children with obesity. Pediatr Res. 2020;88:300–4.
Marzuillo P, Guarino S, Di Sessa A, Rambaldi PF, Reginelli A, Vacca G, et al. Congenital Solitary Kidney from Birth to Adulthood. J Urol. 2021;205:1466–75.
Cho MH. Measurement of urinary protein in children. Child Kidney Dis. 2022;26:69–73.
Correia-Costa L, Schaefer F, Afonso AC, Bustorff M, Guimaraes JT, Guerra A, et al. Normalization of glomerular filtration rate in obese children. Pediatr Nephrol. 2016;31:1321–8.
Mackowiak-Lewandowicz K, Ostalska-Nowicka D, Zaorska K, Kaczmarek E, Zachwieja J, Witt M, et al. Chronic kidney disease predictors in obese adolescents. Pediatr Nephrol. 2022;37:2479–88.
Cheng CH. Albuminuria in childhood is a risk factor for chronic kidney disease and end-stage renal disease. Pediatr Neonatol. 2016;57:263–4.
Sarafidis PA. Obesity, insulin resistance and kidney disease risk: insights into the relationship. Curr Opin Nephrol Hypertens. 2008;17:450–6.
Correia-Costa L, Azevedo A, Caldas, Afonso A. Childhood Obesity and Impact on the Kidney. Nephron. 2019;143:8–11.
Garcia-Carro C, Vergara A, Bermejo S, Azancot MA, Sellares J, Soler MJ. A Nephrologist Perspective on Obesity: From Kidney Injury to Clinical Management. Front Med (Lausanne). 2021;8:655871.
De Cosmo S, Menzaghi C, Prudente S, Trischitta V. Role of insulin resistance in kidney dysfunction: insights into the mechanism and epidemiological evidence. Nephrol Dial Transplant. 2013;28:29–36.
Spoto B, Pisano A, Zoccali C. Insulin resistance in chronic kidney disease: a systematic review. Am J Physiol Renal Physiol. 2016;311:F1087–F108.
Rodenbach KE, Schneider MF, Furth SL, Moxey-Mims MM, Mitsnefes MM, Weaver DJ, et al. Hyperuricemia and Progression of CKD in Children and Adolescents: The Chronic Kidney Disease in Children (CKiD) Cohort Study. Am J Kidney Dis. 2015;66:984–92.
Tsai WC, Wu HY, Peng YS, Ko MJ, Wu MS, Hung KY, et al. Risk Factors for Development and Progression of Chronic Kidney Disease: A Systematic Review and Exploratory Meta-Analysis. Medicine (Baltimore). 2016;95:e3013.
La Scola C, Guarino S, Pasini A, Capalbo D, Liguori L, Di Sessa A, et al. Effect of Body Mass Index on Estimated Glomerular Filtration Rate Levels in Children With Congenital Solitary Kidney: A Cross-Sectional Multicenter Study. J Ren Nutr. 2020;30:261–7.
Joo HJ, Kim GR, Choi DW, Joo JH, Park EC. Uric acid level and kidney function: a cross-sectional study of the Korean national health and nutrition examination survey (2016-2017). Sci Rep. 2020;10:21672.
Souweine JS, Corbel A, Rigothier C, Roque CD, Hadjadj S, Cristol JP, et al. Interest of albuminuria in nephrology, diabetology and as a marker of cardiovascular risk. Ann Biol Clin (Paris). 2019;77:26–35.
Tsioufis C, Mazaraki A, Dimitriadis K, Stefanidis CJ, Stefanadis C. Microalbuminuria in the paediatric age: current knowledge and emerging questions. Acta Paediatr. 2011;100:1180–4.
Calcaterra V, Larizza D, De Silvestri A, Albertini R, Vinci F, Regalbuto C, et al. Gender-based differences in the clustering of metabolic syndrome factors in children and adolescents. J Pediatr Endocrinol Metab. 2020;33:279–88.
Barstad LH, Juliusson PB, Johnson LK, Hertel JK, Lekhal S, Hjelmesaeth J. Gender-related differences in cardiometabolic risk factors and lifestyle behaviors in treatment-seeking adolescents with severe obesity. BMC Pediatr. 2018;18:61.
Gerdts E, Regitz-Zagrosek V. Sex differences in cardiometabolic disorders. Nat Med. 2019;25:1657–66.
Zhernakova DV, Sinha T, Andreu-Sánchez S, Prins JR, Kurilshikov A, Balder JW, et al. Age-dependent sex differences in cardiometabolic risk factors. Nat Cardiovasc Res. 2022;1:844–854.
Spaziani M, Tarantino C, Tahani N, Gianfrilli D, Sbardella E, Lenzi A, et al. Hypothalamo-Pituitary axis and puberty. Mol Cell Endocrinol. 2021;520:111094.
Breehl L, Caban O. Physiology, Puberty. StatPearls. Treasure Island (FL) 2023.
Warady BA, Chadha V. Chronic kidney disease in children: the global perspective. Pediatr Nephrol. 2007;22:1999–2009.
Xu Q, Zhang J, Han H, Chen N, Lai F, Liu Y, et al. Association between intrahepatic triglyceride content in subjects with metabolically healthy abdominal obesity and risks of pre-diabetes plus diabetes: an observational study. BMJ Open. 2022;12:e057820.
Valenzuela PL, Carrera-Bastos P, Castillo-Garcia A, Lieberman DE, Santos-Lozano A, Lucia A. Obesity and the risk of cardiometabolic diseases. Nat Rev Cardiol. 2023;20:475–94.
Drozdz D, Alvarez-Pitti J, Wojcik M, Borghi C, Gabbianelli R, Mazur A, et al. Obesity and Cardiometabolic Risk Factors: From Childhood to Adulthood. Nutrients. 2021;13:4176.
Marzuillo P, Grandone A, Perrone L, Miraglia Del Giudice E. Controversy in the diagnosis of pediatric non-alcoholic fatty liver disease. World J Gastroenterol. 2015;21:6444–50.
Funding
This paper was supported by funding with protocol number 204328/20 provided by Department of Woman, Child and of General and Specialized Surgery, Università degli Studi della Campania “Luigi Vanvitelli”.
Author information
Authors and Affiliations
Contributions
Conceptualization, ADS and PM; methodology, ADS, EMDG; software, ADS, PM, AP; validation, EMDG, PM; formal analysis, ADS, PM; investigation, AP, SG, EMDG; data curation, APP, AMC, SC, GRU; writing—original draft preparation, ADS, PM; writing—review and editing, ADS, PM, EMDG; visualization, PM, AP; supervision, PM. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Di Sessa, A., Passaro, A.P., Colasante, A.M. et al. Kidney damage predictors in children with metabolically healthy and metabolically unhealthy obesity phenotype. Int J Obes 47, 1247–1255 (2023). https://doi.org/10.1038/s41366-023-01379-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01379-1
- Springer Nature Limited