Abstract
Dietary sodium and potassium intake can influence blood pressure. The effects of salt substitution on patients with hypertension and normotensive family member controls, however, have not been evaluated in a rural Chinese population. The objective of this study, accordingly, was to assess the long-term effects of salt substitution on blood pressure. We conducted a double-blind, randomized controlled trial among 200 families in rural China to establish the 2-year effects of a reduced-sodium, high-potassium salt substitute (65% sodium chloride, 25% potassium chloride, 10% magnesium sulfate) compared with normal salt (100% sodium chloride) on blood pressure. Of the 462 individuals in the trial, 372 completed the study (81%). For normotensive subjects, the mean overall difference in systolic and diastolic blood pressure between the two groups at the 24-month follow-up was 2 mm Hg (95% confidence interval (CI) 0–4 mm Hg, P<0.05) and 2 mm Hg (95% CI 1–3 mm Hg, P<0.05), respectively. For subjects with hypertension, the mean overall decrease in systolic blood pressure showed a 4-mm Hg (95% CI 2–6 mm Hg, P<0.05) decrease between the two groups. Diastolic blood pressure was not affected by salt use in the hypertensive group. Salt substitution lowers systolic blood pressure in hypertensive patients and lowers both systolic and diastolic blood pressure in normotensive controls. Salt substitution, therefore, may be an effective adjuvant therapy for hypertensive patients and the potential efficacy in preventing hypertension in normotensive individuals.




Similar content being viewed by others
References
Organization WH. World Health Report 2002: Reducing Risks, Promoting Healthy Life. World Health Organization: Geneva, Switzerland, World Wide Web URL 2002. http://www.who int/whr/2002/en 2002.
Appel LJ, Moore TJ, Obarzanek E, Vollmer WM, Svetkey LP, Sacks FM et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med. 1997; 336: 1117–1124.
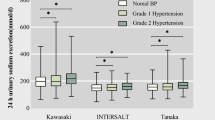
Intersalt Cooperative Research Group. Intersalt: an international study of electrolyte excretion and blood pressure. Results for 24 h urinary sodium and potassium excretion. Intersalt Cooperative Research Group. BMJ 1988; 297: 319–328.
Poulter NR, Khaw KT, Hopwood BE, Mugambi M, Peart WS, Rose G et al. The Kenyan Luo migration study: observations on the initiation of a rise in blood pressure. BMJ 1990; 300: 967–972.
Forte JG, Miguel JM, Miguel MJ, de Padua F, Rose G . Salt and blood pressure: a community trial. J Hum Hypertens. 1989; 3: 179–184.
He FJ, MacGregor GA . Effect of modest salt reduction on blood pressure: a meta-analysis of randomized trials. Implications for public health. J Hum Hypertens. 2002; 16: 761–770.
Denton D, Weisinger R, Mundy NI, Wickings EJ, Dixson A, Moisson P et al. The effect of increased salt intake on blood pressure of chimpanzees. Nat Med. 1995; 1: 1009–1016.
Lifton RP . Molecular genetics of human blood pressure variation. Science 1996; 272: 676–680.
Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. N Engl J Med. 2001; 344: 3–10.
Grobbee DE . Electrolytes and hypertension: results from recent studies. Am J Med Sci. 1994; 307 (Suppl 1): S17–S20.
Khaw KT, Thom S . Randomised double-blind cross-over trial of potassium on blood-pressure in normal subjects. Lancet 1982; 2 (8308): 1127–1129.
He FJ, MacGregor GA . Effect of longer-term modest salt reduction on blood pressure. Cochrane Database Syst Rev. 2004; (3): CD004937.
Dyer AR, Elliott P, Shipley M . Urinary electrolyte excretion in 24 h and blood pressure in the INTERSALT Study. II. Estimates of electrolyte-blood pressure associations corrected for regression dilution bias. The INTERSALT Cooperative Research Group. Am J Epidemiol. 1994; 139: 940–951.
Whelton PK, He J, Cutler JA, Brancati FL, Appel LJ, Follmann D et al. Effects of oral potassium on blood pressure. Meta-analysis of randomized controlled clinical trials. JAMA 1997; 277: 1624–1632.
Dahlmann A, Pradervand S, Hummler E, Rossier BC, Frindt G, Palmer LG . Mineralocorticoid regulation of epithelial Na+ channels is maintained in a mouse model of Liddle’s syndrome. Am J Physiol Renal Physiol. 2003; 285: F310–F318.
Geleijnse JM, Witteman JC, Bak AA, den Breeijen JH, Grobbee DE . Reduction in blood pressure with a low sodium, high potassium, high magnesium salt in older subjects with mild to moderate hypertension. BMJ 1994; 309: 436–440.
Little P, Kelly J, Barnett J, Dorward M, Margetts B, Warm D . Randomised controlled factorial trial of dietary advice for patients with a single high blood pressure reading in primary care. BMJ 2004; 328: 1054.
China Salt Substitute Study Collaborative Group. Salt substitution: a low-cost strategy for blood pressure control among rural Chinese. A randomized, controlled trial. J Hypertens. 2007; 25: 2011–2018.
Shi JP, Wang HL, Li H, Dong W, Fu LY, Qi GX et al. The epidemiological survey of prevalence rate of hypertension in the countryside of Zhangwu county, Liaoning province. Zhonghua Liu Xing Bing Xue Za Zhi. 2003; 24: 547–550.
Karppanen H, Tanskanen A, Tuomilehto J, Puska P, Vuori J, Jantti V et al. Safety and effects of potassium- and magnesium-containing low sodium salt mixtures. J Cardiovasc Pharmacol. 1984; 6 (Suppl 1): S236–S243.
Fu L, Zhao Y, Wu X, Liu H, Shi J, Lu J et al. CYP7A1 genotypes and haplotypes associated with hypertension in an obese Han Chinese population. Hypertens Res. 2011; 34: 722–727.
MacGregor GA, Markandu ND, Sagnella GA, Singer DR, Cappuccio FP . Double-blind study of three sodium intakes and long-term effects of sodium restriction in essential hypertension. Lancet 1989; 2: 1244–1247.
He FJ, MacGregor GA . A comprehensive review on salt and health and current experience of worldwide salt reduction programmes. J Hum Hypertens. 2009; 23: 363–384.
Cappuccio FP, MacGregor GA . Does potassium supplementation lower blood pressure? A meta-analysis of published trials. J Hypertens. 1991; 9: 465–473.
He FJ, MacGregor GA . Potassium intake and blood pressure. Am J Hypertens. 1999; 12: 849–851.
He FJ, MacGregor GA . Fortnightly review: Beneficial effects of potassium. BMJ 2001; 323: 497–501.
Mizushima S, Cappuccio FP, Nichols R, Elliott P . Dietary magnesium intake and blood pressure: a qualitative overview of the observational studies. J Hum Hypertens. 1998; 12: 447–453.
Laurant P, Touyz RM . Physiological and pathophysiological role of magnesium in the cardiovascular system: implications in hypertension. J Hypertens. 2000; 18: 1177–1191.
Jee SH, Miller ER, Guallar E, Singh VK, Appel LJ, Klag MJ . The effect of magnesium supplementation on blood pressure: a meta-analysis of randomized clinical trials. Am J Hypertens. 2002; 15: 691–696.
Touyz RM . Role of magnesium in the pathogenesis of hypertension. Mol Aspects Med. 2003; 24: 107–136.
Song Y, Sesso HD, Manson JE, Cook NR, Buring JE, Liu S . Dietary magnesium intake and risk of incident hypertension among middle-aged and older US women in a 10-year follow-up study. Am J Cardiol. 2006; 98: 1616–1621.
Tian HG, Guo ZY, Hu G, Yu SJ, Sun W, Pietinen P et al. Changes in sodium intake and blood pressure in a community-based intervention project in China. J Hum Hypertens. 1995; 9: 959–968.
Cutler JA, Follmann D, Allender PS . Randomized trials of sodium reduction: an overview. Am J Clin Nutr. 1997; 65: 643S–651S.
Rodgers A, Lawes C, MacMahon S . Reducing the global burden of blood pressure-related disease. J Hypertens. 2000; 18: S3–S6.
China Ministry of Health, China Ministry of Science and Technology, and China State Bureau of Statistics. The Nutrition and Health Status of the Chinese People. In: Material for the press conference of the State Council Information Office, October 2004 Ministry of Health, China Ministry of Science and Technology, and China State Bureau of Statistics: Beijing: China, 2004.
He J, Klag MJ, Wu Z, Whelton PK . Stroke in the People’s Republic of China. Geographic variations in incidence and risk factors. Stroke 1995; 26: 2222–2227.
Tumbull F and Blood Pressure Lowering Treatment Trialists’ Collaboration. Effects of different blood pressure lowering regimens on major cardiovascular events: second cycle of prospectively designed overviews. Lancet 2003; 362: 1527–1535.
Lawes CM, Rodgers A, Bennett DA, Parag V, Suh I, Ueshima H et al. Blood pressure and cardiovascular diseases in the Asia-Pacific region. J Hypertens. 2003; 21: 707–716.
Bazzano LA, He J, Ogden LG, Vupputuri S, Loria C, Myers L et al. Dietary potassium intake and risk of stroke in US men and women: National Health and Nutrition Examination Survey I epidemiologic follow-up study. Stroke 2001; 32: 1473–1480.
Schmieder RE, Messerli FH, Garavaglia GE, Nunez BD . Dietary salt intake. a determinant of cardiac involvement in essential hypertension. Circulation 1988; 78: 951–956.
Fujiwara T, Kawamura M, Nakajima J, Adachi T, Hiramori K . Seasonal differences in diurnal blood pressure of hypertensive patients living in a stable environmental temperature. J Hypertens. 1995; 13: 1747–1752.
Law MR, Frost CD, Wald NJ . By how much does dietary salt reduction lower blood pressure? III. Analysis of data from trials of salt reduction. BMJ 1991; 302: 819–824.
Graudal NA, Galloe AM, Garred P . Effects of sodium restriction on blood pressure, renin, aldosterone, catecholamines, cholesterols, and triglyceride: a meta-analysis. JAMA 1998; 279: 1383–1391.
Turnbull F . Effects of different blood-pressure-lowering regimens on major cardiovascular events: results of prospectively-designed overviews of randomised trials. Lancet 2003; 362: 1527–1535.
Acknowledgements
This work was supported by the grants from Program of the National Natural Science Foundation of China (30800944 and 30671796).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhou, B., Wang, HL., Wang, WL. et al. Long-term effects of salt substitution on blood pressure in a rural North Chinese population. J Hum Hypertens 27, 427–433 (2013). https://doi.org/10.1038/jhh.2012.63
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2012.63
- Springer Nature Limited
Keywords
This article is cited by
-
A prediction model for the impact of environmental and genetic factors on cardiovascular events: development in a salt substitutes population
Journal of Translational Medicine (2023)
-
Effectiveness of a community health worker-led low-sodium salt intervention to reduce blood pressure in rural Bangladesh: protocol for a cluster randomized controlled trial
Trials (2023)
-
Hypertension in China: epidemiology and treatment initiatives
Nature Reviews Cardiology (2023)
-
Strengthening Knowledge to Practice on Effective Salt Reduction Interventions in Low- and Middle-Income Countries
Current Nutrition Reports (2021)
-
The hypotensive effect of salt substitutes in stage 2 hypertension: a systematic review and meta-analysis
BMC Cardiovascular Disorders (2020)