Abstract
Background/Objectives:
In animal models, a role in the regulation of energy expenditure (EE) has been ascribed to sphingolipids, active components of cell membranes participating in cellular signaling. In humans, it is unknown whether sphingolipids have a role in the modulation of EE and, consequently, influence weight gain. The present study investigated the putative association of EE and weight gain with sphingolipid levels in the human skeletal muscle, a component of fat-free mass (the strongest determinant of EE), in adipose tissue and plasma.
Subjects/Methods:
Twenty-four-hour EE, sleeping metabolic rate (SMR) and resting metabolic rate (RMR) were assessed in 35 healthy Native Americans of Southwestern heritage (24 male; 30.2±7.73 years). Sphingolipid (ceramide, C; sphingomyelin, SM) concentrations were measured in skeletal muscle tissue, subcutaneous adipose tissue and plasma samples. After 6.68 years (0.26–12.4 years), follow-up weights were determined in 16 participants (4 females).
Results:
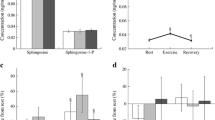
Concentrations of C24:0, SM18:1/26:1 and SM18:0/24:1 in muscle were associated with 24-h EE (r=−0.47, P=0.01), SMR (r=−0.59, P=0.0008) and RMR (r=−0.44, P=0.01), respectively. Certain muscle sphingomyelins also predicted weight gain (for example, SM18:1/23:1, r=0.74, P=0.004). For specific muscle sphingomyelins that correlated with weight gain and EE (SM18:1/23:0, SM18:1/23:1 and SMR, r=−0.51, r=−0.41, respectively, all P<0.03; SM18:1/24:2 and RMR, r=−0.36, P=0.03), associations could be reproduced with SMR in adipose tissue (all r<−0.46, all P<0.04), though not in plasma.
Conclusions:
This study provides preliminary, novel evidence, that specific muscle and adipose tissue sphingolipid compounds are associated with EE and weight gain in Native Americans of Southwestern heritage. Further studies are warranted to investigate whether sphingolipids of different body compartments act in concert to modulate energy balance in humans.




Similar content being viewed by others
References
Weyer C, Snitker S, Rising R, Bogardus C, Ravussin E . Determinants of energy expenditure and fuel utilization in man: effects of body composition, age, sex, ethnicity and glucose tolerance in 916 subjects. Int J Obes Relat Metab Disord 1999; 23: 715–722.
Ravussin E, Lillioja S, Anderson TE, Christin L, Bogardus C . Determinants of 24-hour energy expenditure in man. Methods and results using a respiratory chamber. J Clin Invest 1986; 78: 1568.
Ravussin E, Bogardus C . A brief overview of human energy metabolism and its relationship to essential obesity. Am J Clin Nutr 1992; 55: 242S–245S.
Piaggi P, Thearle MS, Bogardus C, Krakoff J . Lower energy expenditure predicts long-term increases in weight and fat mass. J Clin Endocrinol Metab 2013; 98: E703–E707.
Reinhardt M, Thearle MS, Ibrahim M, Hohenadel MG, Bogardus C, Krakoff J et al. A human thrifty phenotype associated with less weight loss during caloric restriction. Diabetes 2015; 64: 2859–2867.
Qi Y, Takahashi N, Hileman SM, Patel HR, Berg AH, Pajvani UB et al. Adiponectin acts in the brain to decrease body weight. Nat Med 2004; 10: 524–529.
Krakoff J, Ma L, Kobes S, Knowler WC, Hanson RL, Bogardus C et al. Lower metabolic rate in individuals heterozygous for either a frameshift or a functional missense MC4R variant. Diabetes 2008; 57: 3267–3272.
Ogden CL, Carroll MD, Kit BK, Flegal KM . Prevalence of obesity and trends in body mass index among US children and adolescents, 1999-2010. JAMA 2012; 307: 483–490.
Michel V, Bakovic M . Lipid rafts in health and disease. Biol Cell 2007; 99: 129–140.
Park T-S, Panek RL, Mueller SB, Hanselman JC, Rosebury WS, Robertson AW et al. Inhibition of sphingomyelin synthesis reduces atherogenesis in apolipoprotein E-knockout mice. Circulation 2004; 110: 3465–3471.
Hojjati MR, Li Z, Zhou H, Tang S, Huan C, Ooi E et al. Effect of myriocin on plasma sphingolipid metabolism and atherosclerosis in apoE-deficient mice. J Biol Chem 2005; 280: 10284–10289.
Milhas D, Clarke CJ, Hannun YA . Sphingomyelin metabolism at the plasma membrane: implications for bioactive sphingolipids. FEBS Lett 2010; 584: 1887–1894.
Gillard B, Thomas J, Nell L, Marcus D . Antibodies against ganglioside GT3 in the sera of patients with type I diabetes mellitus. J Immunol 1989; 142: 3826–3832.
Holland WL, Adams AC, Brozinick JT, Bui HH, Miyauchi Y, Kusminski CM et al. An FGF21-adiponectin-ceramide axis controls energy expenditure and insulin action in mice. Cell Metab 2013; 17: 790–797.
Finck BN, Han X, Courtois M, Aimond F, Nerbonne JM, Kovacs A et al. A critical role for PPARα-mediated lipotoxicity in the pathogenesis of diabetic cardiomyopathy: modulation by dietary fat content. Proc Natl Acad Sci 2003; 100 (3): 1226–1231.
Yang G, Badeanlou L, Bielawski J, Roberts AJ, Hannun YA, Samad F . Central role of ceramide biosynthesis in body weight regulation, energy metabolism, and the metabolic syndrome. Am J Physiol 2009; 297: E211–E224.
Turpin SM, Nicholls HT, Willmes DM, Mourier A, Brodesser S, Wunderlich CM et al. Obesity-induced CerS6-dependent C 16: 0 ceramide production promotes weight gain and glucose intolerance. Cell Metab 2014; 20: 678–686.
Vidal-Puig A, Solanes G, Grujic D, Flier JS, Lowell BB . UCP3: an uncoupling protein homologue expressed preferentially and abundantly in skeletal muscle and brown adipose tissue. Biochem Biophys Res Commun 1997; 235: 79–82.
Smith ME, Tippetts TS, Brassfield ES, Tucker BJ, Ockey A, Swensen AC et al. Mitochondrial fission mediates ceramide-induced metabolic disruption in skeletal muscle. Biochem J 2013; 456: 427–439.
Contreras C, González-García I, Martínez-Sánchez N, Seoane-Collazo P, Jacas J, Morgan DA et al. Central ceramide-induced hypothalamic lipotoxicity and ER stress regulate energy balance. Cell Rep 2014; 9: 366–377.
Genuth S, Alberti K, Bennett P, Buse J, DeFronzo R, Kahn R et al. Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care 2003; 26: 3160–3168.
Realini N, Solorzano C, Pagliuca C, Pizzirani D, Armirotti A, Luciani R et al. Discovery of highly potent acid ceramidase inhibitors with in vitro tumor chemosensitizing activity. Sci Rep 2013; 3: 1035.
Basit A, Piomelli D, Armirotti A . Rapid evaluation of 25 key sphingolipids and phosphosphingolipids in human plasma by LC-MS/MS. Anal Bioanal Chem 2015; 407: 5189–5198.
Knowler WC, Pettitt DJ, Saad MF, Charles MA, Nelson RG, Howard BV et al. Obesity in the Pima Indians: its magnitude and relationship with diabetes. Am J Clin Nutr 1991; 53: 1543S–1551S.
Schutz Y, Ravussin E, Diethelm R, Jequier E . Spontaneous physical activity measured by radar in obese and control subject studied in a respiration chamber. Int J Obes 1981; 6: 23–28.
van Marken Lichtenbelt WD, Vanhommerig JW, Smulders NM, Drossaerts JM, Kemerink GJ, Bouvy ND et al. Cold-activated brown adipose tissue in healthy men. N Engl J Med 2009; 360: 1500–1508.
Walls SM Jr, Attle SJ, Brulte GB, Walls ML, Finley KD, Chatfield DA et al. Identification of sphingolipid metabolites that induce obesity via misregulation of appetite, caloric intake and fat storage in Drosophila. PLoS Genet 2013; 9: e1003970.
Kopecký J, Rossmeisl M, Flachs P, Bardova K, Brauner P . Mitochondrial uncoupling and lipid metabolism in adipocytes. Biochem Soc Trans 2001; 29: 791–797.
Ibrahim SH, Kohli R, Gores GJ . Mechanisms of lipotoxicity in NAFLD and clinical implications. J Pediatr Gastroenterol Nutr 2011; 53: 131–140.
Choi S, Snider AJ . Sphingolipids in high fat diet and obesity-related diseases. Mediators Inflamm 2015; 2015: 12.
Virtue S, Vidal-Puig A . Adipose tissue expandability, lipotoxicity and the metabolic syndrome—an allostatic perspective. Biochim Biophys Acta 2010; 1801: 338–49.
Mitsutake S, Zama K, Yokota H, Yoshida T, Tanaka M, Mitsui M et al. Dynamic modification of sphingomyelin in lipid microdomains controls development of obesity, fatty liver, and type 2 diabetes. J Biol Chem 2011; 286: 28544–28555.
Gluck ME, Venti CA, Salbe AD, Votruba SB, Krakoff J . Higher 24‐h respiratory quotient and higher spontaneous physical activity in nighttime eaters. Obesity 2011; 19: 319–323.
Piaggi P, Krakoff J, Bogardus C, Thearle MS . Lower 'awake and fed thermogenesis' predicts future weight gain in subjects with abdominal adiposity. Diabetes 2013; 62: 4043–4051.
Burgess HJ, Trinder J, Kim Y, Luke D . Sleep and circadian influences on cardiac autonomic nervous system activity. Am J Physiol 1997; 273: H1761–H1768.
Rolfe DF, Newman JM, Buckingham JA, Clark MG, Brand MD . Contribution of mitochondrial proton leak to respiration rate in working skeletal muscle and liver and to SMR. Am J Physiol 1999; 276: C692–C699.
Zurlo F, Larson K, Bogardus C, Ravussin E . Skeletal muscle metabolism is a major determinant of resting energy expenditure. J Clin Invest 1990; 86: 1423.
Stefan N, Stumvoll M, Weyer C, Bogardus C, Tataranni P, Pratley R . Exaggerated insulin secretion in Pima Indians and African‐Americans but higher insulin resistance in Pima Indians compared to African‐Americans and Caucasians. Diabet Med 2004; 21: 1090–1095.
Seino Y, Nanjo K, Tajima N, Kadowaki T, Kashiwagi A, Araki E et al. Report of the committee on the classification and diagnostic criteria of diabetes mellitus. J Diabetes Investig 2010; 1: 212–228.
Acknowledgements
We thank all volunteers whose participation in clinical trials contributed to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on International Journal of Obesity website
Supplementary information
Rights and permissions
About this article
Cite this article
Heinitz, S., Piaggi, P., Vinales, K. et al. Specific skeletal muscle sphingolipid compounds in energy expenditure regulation and weight gain in Native Americans of Southwestern heritage. Int J Obes 41, 1585–1593 (2017). https://doi.org/10.1038/ijo.2017.143
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.143
- Springer Nature Limited