Abstract
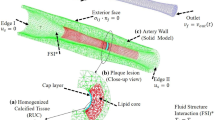
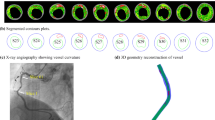
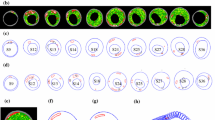
A three-dimensional (3D) MRI-based computational model with multicomponent plaque structure and fluid–structure interactions (FSI) is introduced to perform mechanical analysis for human atherosclerotic plaques and identify critical flow and stress/strain conditions which may be related to plaque rupture. Three-dimensional geometry of a human carotid plaque was reconstructed from 3D MR images and computational mesh was generated using Visualization Toolkit. Both the artery wall and the plaque components were assumed to be hyperelastic, isotropic, incompressible, and homogeneous. The flow was assumed to be laminar, Newtonian, viscous, and incompressible. The fully coupled fluid and structure models were solved by ADINA, a well-tested finite element package. Results from two-dimensional (2D) and 3D models, based on ex vivo MRI and histological images (HI), with different component sizes and plaque cap thickness, under different pressure and axial stretch conditions, were obtained and compared. Our results indicate that large lipid pools and thin plaque caps are associated with both extreme maximum (stretch) and minimum (compression when negative) stress/strain levels. Large cyclic stress/strain variations in the plaque under pulsating pressure were observed which may lead to artery fatigue and possible plaque rupture. Large-scale patient studies are needed to validate the computational findings for possible plaque vulnerability assessment and rupture predictions.
Similar content being viewed by others
REFERENCES
Bathe, K. J. Finite Element Procedures. New Jersey: Prentice-Hall, 1996.
Bathe, K. J., Ed. Theory and Modeling Guide, Vols. I&II. Watertown, MA: ADINA and ADINA-F, ADINA R&D, 2002.
Bathe, K. J., Ed. ADINA Verification Manual. Watertown, MA: ADINA R&D, 2002.
Beattie, D., C. Xu, R. P. Vito, S. Glagov, and M. C. Whang. Mechanical analysis of heterogeneous, atherosclerotic human aorta. J.Biomech.Eng. 120:602–607, 1998.
Berry, J. L., A. Santamarina, J. E. Moore, Jr., S. Roychowdhury, and W. D. Routh. Experimental and computational flow evaluation of coronary stents. Ann.Biomed.Eng. 28:386–398, 2000.
Bock, R. W., A. C. Gray-Weale, F. P. Mock, M. A. Stats, D. A. Robinson, L. Irwig, and R. J. Lusby. The natural history of asymptomatic carotid artery disease. J.Vasc.Surg. 17:160–171, 1993.
Boyle, J. J. Association of coronary plaque rupture and atherosclerotic inflammation. J.Pathol. 181:93–99, 1997.
Brossollet, L. J., and R. P. Vito. A new approach to mechanical testing and modeling of biological tissues, with application to blood vessels. J.Biomech.Eng. 118:433–439, 1996.
Burke, A. P., A. Farb, G. T. Malcom, Y. H. Liang, J. E. Smialek, and R. Virmani. Plaque rupture and sudden death related to exertion in men with coronary artery disease. JAMA 281:921–926, 1999.
Cai, J. M., T. S. Hatsukami, M. S. Ferguson, R. Small, N. L. Polissar, and C. Yuan. Classification of human carotid atherosclerotic lesions with in vivo multicontrast magnetic resonance imaging. Circulation 106:1368–1373, 2002.
Cheng, G. C., H. M. Loree, R. D. Kamm, M. C. Fishbein, and R. T. Lee. Distribution of circumferential stress in ruptured and stable atherosclerotic lesions, a structural analysis with histopathological correlation. Circulation 87:1179–1187, 1993.
Davies, M. J., and A. C. Thomas. Plaque fissuring-the cause of acute myocardial infarction, sudden ischemic death, and crecendo angina. Br.Heart J. 53:363–373, 1985.
Falk, E., P. K. Shah, and V. Fuster. Coronary plaque disruption. Circulation 92:657–671, 1995.
Fayad, Z. A., J. T. Fallon, M. Shinnar, S. Wehrli, H. M. Dansky, M. Poon, J. J. Badimon, S. A. Charlton, E. A. Fisher, J. L. Breslow, and V. Fuster. Noninvasive in vivo high-resolution MRI of atherosclerotic lesions in genetically engineered mice. Circulation 98:1541–1547, 1998.
Friedman, M. H. Arteriosclerosis research using vascular flow models: From 2-D branches to compliant replicas. J.Biomech.Eng. 115:595–601, 1993.
Fuster, V., B. Stein, J. A. Ambrose, L. Badimon, J. J. Badimon, and J. H. Chesebro. Atherosclerotic plaque rupture and throm-bosis, evolving concept. Circulation 82(Suppl. II):II-47–II-59, 1990.
Giddens, D. P., C. K. Zarins, and S. Glagov. Responses of arteries to near-wall fluid dynamic behavior. Appl.Mech.Rev. 43:S98–S102, 1990.
Giddens, D. P., C. K. Zarins, and S. Glagov. The role of fluid mechanics in the localization and detection of atherosclerosis. J.Biomech.Eng. 115:588–594, 1993.
Hafner, C. D. Minimizing the risks of carotid endarterectomy. J.Vasc.Surg. 1(3):392–397, 1984.
Hatsukami, T. S., R. Ross, N. L. Polissar, and C. Yuan. Visualization of fibrous cap thickness and rupture in human atherosclerotic carotid plaque in vivo with high-resolution magnetic resonance imaging. Circulation 102:959–964, 2000.
Huang, H., R. Virmani, H. Younis, A. P. Burke, R. D. Kamm, and R. T. Lee. The impact of calcification on the biomechanical stability of atherosclerotic plaques. Circulation 103:1051–1056, 2001.
Kaazempur-Mofrad, M. R., M. Bathe, H. Karcher, H. F. Younis, H. C. Seong, E. B. Shim, R. C. Chan, D. P. Hinton, A. G. Isasi, A. Upadhyaya, M. J. Powers, L. G. Griffith, and R. D. Kamm. Role of simulation in understanding biological systems. Comput.Struct. 81:715–726, 2003.
Kobayashi, S., D. Tsunoda, Y. Fukuzawa, H. Morikawa, D. Tang, and N. Ku. Flow and compression in arterial models of steno-sis with lipid core. Proceedings of 2003 ASME Summer Bio-engineering Conference, pp. 497–498, Miami, FL, June 25–29, 2003.
Ku, D. N. Blood flowin arteries. Annu.Rev.Fluid Mech. 29:399–434, 1997.
Ku, D. N., D. P. Giddens, C. K. Zarins, and S. Glagov. Pulsatile flow and atherosclerosis in the human carotid bifurcation: Posi-tive correlation between plaque location and low and oscillating shear stress. Arteriosclerosis 5:293–302, 1985.
Ku, D. N., M. Zeigler, R. L. Binnes, and M. T. Stewart. A study of predicted and experimental wall collapse in models of highly stenotic arteries. In: Biofluid Mechanics: Blood Flow in Large Vessels, edited by Dieter Liepsch. New York: Springer-Verlag, 1990, pp. 409–416.
Lee, R. T., A. J. Grodzinsky, E. H. Frank, R. D. Kamm, and F. J. Schoen. Structure-dependent dynamic mechanical behavior of fibrous caps from human atherosclerotic plaques. Circulation 83(5):1764–1770, 1991.
Lee, R. T., and R. D. Kamm. Vascular mechanics for the cardiologist. J.Am.Coll.Cardiol. 23(6):1289–1295, 1994.
Lee, R. T., F. J. Schoen, H. M. Loree, M. W. Lark, and P. Libby. Circumferential stress and matrix metalloproteinase 1 in human coronary atherosclerosis. Implications for plaque rupture. Arterioscler.Thromb.Vasc.Biol. 16:1070–1073, 1996.
Lei, M., D. P. Giddens, S. A. Jones, F. Loth, and H. Bassiouny. Pulsatile flow in an end-to-side vascular graft model: Compar-ison of computations with experimental data. J.Biomech.Eng. 123:80–87, 2001.
Long, Q., X. Y. Xu, M. Bourne, and T. M. Griffith. Numerical study of blood flow in an anatomically realistic aorta–iliac bifur-cation generated from MRI data. Magn.Reson.Med. 43:565–576, 2000.
Long, Q., X. Y. Xu, K. V. Ramnarine, and P. Hoskins. Numerical investigation of physiologically realistic pulsatile flow through arterial stenosis. J.Biomech. 34:1229–1242, 2001.
Loree, H. M., R. D. Kamm, R. G. Stringfellow, and R. T. Lee. Effects of fibrous cap thickness on peak circumferential stress in model atherosclerotic vessels. Circ.Res. 71:850–858, 1992.
Loree, H. M., B. J. Tobias, L. J. Gibson, R. D. Kamm, D. M. Small, and R. T. Lee. Mechanical properties of model atheroscle-rotic lesion lipid pools. Arterioscler.Thromb. 14(2):230–234, 1994.
McCord, B. N. Fatigue of Atherosclerotic Plaque. PhD Thesis, Georgia Institute of Technology, 1992.
Pedersen, P. C., J. Chakareski, and R. Lara-Montalvo. Ultra-sound characterization of arterial wall structures based on inte-grated backscatter profiles. Proceedings for the 2003 SPIE Med-ical Imaging Symposium, San Diego, CA, 2003, pp. 115–126.
Perktold, K., G. Rappotsch, M. Hofer, G. Karner, and K. Andlinger. Effects of vessel wall compliance on flow and stress patterns in arterial bends and bifurcations. Adv.Bioeng.BED 33:329–330, 1996.
Peskin, C. S. Mathematical Aspects of Heart Physiology. Lecture notes of Courant Institute of Mathematical Sciences, New York, 1975.
Peskin, C. S. Numerical analysis of blood flow in the heart. J.Comp.Phys. 25:220–252, 1977.
Peskin, C. S. A three-dimensional computational method for blood flow in the heart. J.Comp.Phys. 81:372–405, 1989.
Ravn, H. B., and E. Falk. Histopathology of plaque rupture. Cardiol.Clin. 17:263–270, 1999.
Schroeder, W., K. Martin, and B. Lorensen. The Visualization Toolkit, An Object-Oriented Approach To 3D Graphics, 2nd ed. New Jersey: Prentice-Hall, 1998.
Steinman, D. A., J. B. Thomas, H. M. Ladak, J. S. Milner, B. K. Rutt, and J. D. Spence. Reconstruction of carotid bifurcation hemodynamics and wall thickness using computational fluid dynamics and MRI. Magn.Reson.Med. 47(1):149–159, 2002.
Tang, D., C. Yang, S. Kobayashi, and D. N. Ku. Steady flow and wall compression in stenotic arteries: A 3-D thick-wall model with fluid–wall interactions. J.Biomech.Eng. 123:548–557, 2001.
Tang, D., C. Yang, S. Kobayashi, and D. N. Ku. Simulating cyclic artery compression using a 3-D unsteady model with fluid– structure interactions. Comput.Struct. 80:1651–1665, 2002.
Tang, D., C. S. Kobayashi, and D. N. Ku. Effect of a lipid pool on stress/strain distributions in stenotic arteries: 3D FSI models. J.Biomech.Eng., in press.
Tang, D., C. Yang, H. F. Walker, S. Kobayashi, J. Zheng, and D. N. Ku. 2-D and 3-D multi-physics models for flow and non-linear stress/strain analysis of stenotic arteries with lipid cores. In: Computational Fluid and Solid Mechanics, edited by K. J. Bathe, Vol. 2. New York: Elsevier, 2003, pp. 1829–1832.
Tang, D., C. Yang, J. Zheng, and R. P. Vito. Effects of steno-sis asymmetry on blood flow and artery compression: A three-dimensional fluid–structure interaction model. Ann.Biomed.Eng. 31:1182–1193, 2003.
Toussaint, J. F., G. M. LaMuraglia, J. F. Southern, V. Fuster, and H. L. Kantor. MRimages of lipid, fibrous, calcified, hemorrhagic and thrombotic components of human atherosclerosis in vivo. Circulation 94:932–938, 1996.
van der Wal, A. C., A. E. Becker, C. M. van der Loos, and P. K. Das. Site of intimal rupture or erosion of thrombosed coro-nary atherosclerotic plaques is characterized by an inflammatory process irrespective of the dominant plaque morphology. Circulation 89:36–44, 1994.
Williamson, S. D., Y. Lam, H. F. Younis, H. Huang, S. Patel, M. R. Kaazempur-Mofrad, and R. D. Kamm. On the sensitivity of wall stresses in diseased arteries to variable material properties. J.Biomech.Eng. 125:147–155, 2003.
Yuan, C., B. W. Beath, L. H. Smith, and T. S. Hatsukami. Measurement of atherosclerotic carotid plaque size in vivo using high resolution Magnetic Resonance Imaging. Circulation 98:2666–2671, 1998.
Yuan, C., T. S. Hatsukami, and K. D. O'Brien. High resolution magnetic resonance imaging of normal and atherosclerotic human coronary arteries ex vivo: Discrimination of plaque tissue components. J.Med.Investig. 49(16):491–499, 2001.
Yuan, C., W. S. Kerwin, M. S. Ferguson, N. Polissar, S. X. Zhang, J. M. Cai, and T. S. Hatsukami. Contrast enhanced high resolu-tion MRI for atherosclerotic carotid artery tissue characterization. JMRI 15:62–67, 2002.
Yuan, C., L. M. Mitsumori, K. W. Beach, and K. R. Maravilla. Special review: Carotid atherosclerotic plaque: Noninvasive MR characterization and identification of vulnerable lesions. Radiology 221:285–299, 2001.
Yuan, C., L. M. Mitsumori, M. S. Ferguson, N. L. Polissar, D. E. Echelard, G. Ortiz, R. Small, J. W. Davies, W. S. Kerwin, and T. S. Hatsukami. In vivo accuracy of multispectral MR imaging for identifying lipid-rich necrotic cores and intraplaque hemorrhage in advanced human carotid plaques. Circulation 104:2051–2056, 2001.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Tang, D., Yang, C., Zheng, J. et al. 3D MRI-Based Multicomponent FSI Models for Atherosclerotic Plaques. Annals of Biomedical Engineering 32, 947–960 (2004). https://doi.org/10.1023/B:ABME.0000032457.10191.e0
Issue Date:
DOI: https://doi.org/10.1023/B:ABME.0000032457.10191.e0