Abstract
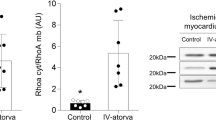
Previous studies have suggested that the 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase inhibitors attenuate ischemia-reperfusion injury by increasing the activity of endothelial nitric oxide synthase (eNOS). We assessed whether short-term treatment with atorvastatin reduces myocardial infarct size in the rat. Rats (male Sprague-Dawley) received atorvastatin 2 mg/kg per day (n = 9), 10 mg/kg per day (n = 8), or 75 mg/kg per day (n = 11), or placebo (n = 11) by gastric gavage for 3 days. Two additional groups received atorvastatin 10 mg/kg (n = 7) or placebo (n = 7) for 3 days and the nonselective nitric oxide synthase inhibitor, NG-nitro-L-arginine methyl ester (L-NAME), 15 mg/kg intravenously 15 min before surgery. All rats underwent 30 min of coronary artery occlusion followed by 180 min of reperfusion. Ischemic myocardium at risk was assessed with blue dye and infarct size by triphenyltetrazolium chloride. Ischemic myocardium at risk was comparable among groups. Infarct size, expressed as a percentage of the myocardium at risk, was significantly smaller in the atorvastatin 75 mg/kg group (22.6 ± 2.8%; p = 0.035 vs. placebo) and atorvastatin 10 mg/kg (20.3 ± 3.8%; p = 0.022 vs. placebo) compared with placebo (37.5 ± 4.3%). The effect of atorvastatin 2 mg/kg was of smaller magnitude and did not reach statistical significance (infarct size 30.6 ± 4.2% of the myocardium at risk). L-NAME abolished the protective effect of atorvastatin 10 mg/kg per day. Infarct size was 43.0 ± 4.1% in the atorvastatin group and 39.4 ± 3.3% in the placebo group (p = 0.503).
In conclusion, short-term (3 days) atorvastatin (10–75 mg/kg/d) significantly reduced myocardial infarct size. The protective effect was completely abolished by L-NAME, strongly suggesting that this protective effect is mediated via the nitric oxide synthase pathway.
Similar content being viewed by others
References
Goldstein JL, Brown MS.Regulation of the mevalonate pathway. Nature 1990;343:425-430.
Executive Summary of The Third Report of The National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment Panel III). JAMA 2001;285:2486-2497.
Randomised trial of cholesterol lowering in 4444 patients with coronary heart disease: The Scandinavian Simvastatin Survival Study (4S). Lancet 1994;344:1383-1389.
Sacks FM, Pfeffer MA, Moye LA, et al. The effect of pravastatin on coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events Trial investigators. N Engl J Med 1996;335:1001-1009.
Prevention of cardiovascular events and death with pravastatin in patients with coronary heart disease and a broad range of initial cholesterol levels. The Long-Term Intervention with Pravastatin in Ischaemic Disease (LIPID) Study Group. N Engl J Med 1998;339:1349-1357.
Libby P. Molecular bases of the acute coronary syndromes. Circulation 1995;91:2844-2850.
Influence of pravastatin and plasma lipids on clinical events in the West of Scotland Coronary Prevention Study (WOSCOPS). Circulation 1998;97:1440-1445.
O'Driscoll G, Green D, Taylor RR. Simvastatin, an HMGcoenzyme A reductase inhibitor, improves endothelial function within 1 month. Circulation 1997;95:1126-1131.
Williams JK, Sukhova GK, Herrington DM, Libby P. Pravastatin has cholesterol-lowering independent effects on the artery wall of atherosclerotic monkeys. J Am Coll Cardiol 1998;31:684-691.
Ridker PM, Rifai N, Pfeffer MA, et al. Inflammation, pravastatin, and the risk of coronary events after myocardial infarction in patients with average cholesterol levels. Cholesterol and Recurrent Events (CARE) Investigators. Circulation 1998;98:839-844.
Kluft C, de Maat MP, Gevers Leuven JA, Potter van Loon BJ, Mohrschladt MF. Statins and C-reactive protein. Lancet 1999;353:1274.
Ridker PM. Are statins anti-inflammatory? Issues in the design and conduct of the pravastatin inflammation C-reactive protein evaluation. Curr Cardiol Rep 2000;2:269-273.
Dzien A, Dzien-Bischinger C, Hoppichler F, Lechleitner M. Statin therapy and plasma C-reactive protein levels in primary prevention. Cardiovasc Drugs Ther 2000;14:699-700.
Joukhadar C, Klein N, Prinz M, et al. Similar effects of atorvastatin, simvastatin and pravastatin on thrombogenic and inflammatory parameters in patients with hypercholesterolemia. Thromb Haemost 2001;85:47-51.
Endres M, Laufs U, Huang Z, et al. Stroke protection by 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase inhibitors mediated by endothelial nitric oxide synthase. Proc Natl Acad Sci USA 1998;95:8880-8885.
Amin-Hanjani S, Stagliano NE, Yamada M, Huang PL, Liao JK, Moskowitz MA. Mevastatin, an HMG-CoA reductase inhibitor, reduces stroke damage and upregulates endothelial nitric oxide synthase in mice. Stroke 2001;32:980-986.
Laufs U, Gertz K, Huang P, et al. Atorvastatin upregulates type III nitric oxide synthase in thrombocytes, decreases platelet activation, and protects from cerebral ischemia in normocholesterolemic mice. Stroke 2000;31:2442-2449.
Laufs U, Gertz K, Dirnagl U, Bohm M, Nickenig G, Endres M. Rosuvastatin, a new HMG-CoA reductase inhibitor, upregulates endothelial nitric oxide synthase and protects from ischemic stroke in mice. Brain Res 2002;942:23-30.
Laufs U, Endres M, Stagliano N, et al. Neuroprotection mediated by changes in the endothelial actin cytoskeleton. J Clin Invest 2000;106:15-24.
Bauersachs J, Galuppo P, Fraccarollo D, Christ M, Ertl G. Improvement of left ventricular remodeling and function by hydroxymethylglutaryl coenzyme a reductase inhibition with cerivastatin in rats with heart failure after myocardial infarction. Circulation 2001;104:982-985.
Hayashidani S, Tsutsui H, Shiomi T, et al. Fluvastatin, a 3-hydroxy-3-methylglutaryl coenzyme a reductase inhibitor, attenuates left ventricular remodeling and failure after experimental myocardial infarction. Circulation 2002;105:868-873.
Pisarenko OI, Studneva IM, Lankin VZ, et al. Inhibitor of beta-hydroxy-beta-methylglutaryl coenzymeAreductase decreases energy supply to the myocardium in rats. Bull Exp Biol Med 2001;132:956-958.
Satoh K, Ichihara K. Effects of 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors on mitochondrial respiration in ischemic rat hearts. Eur J Pharmacol 1995;292:271-275.
Satoh K, Ichihara K. Lipophilic HMG-CoA reductase inhibitors increase myocardial stunning in dogs. J Cardiovasc Pharmacol 2000;35:256-262.
Ichihara K, Satoh K, Abiko Y. Influences of pravastatin and simvastatin, HMG-CoA reductase inhibitors, on myocardial stunning in dogs. J Cardiovasc Pharmacol 1993;22:852-856.
Di Napoli P, Antonio Taccardi A, Grilli A, et al. Simvastatin reduces reperfusion injury by modulating nitric oxide synthase expression: An ex vivo study in isolated working rat hearts. Cardiovasc Res 2001;51:283-293.
Lefer AM, Campbell B, Shin YK, Scalia R, Hayward R, Lefer DJ. Simvastatin preserves the ischemic-reperfused myocardium in normocholesterolemic rat hearts. Circulation 1999;100:178-184.
Scalia R, Gooszen ME, Jones SP, et al. Simvastatin exerts both anti-inflammatory and cardioprotective effects in apolipoprotein E-deficient mice. Circulation 2001;103:2598-2603.
Lefer DJ, Scalia R, Jones SP, et al. HMG-CoA reductase inhibition protects the diabetic myocardium from ischemiareperfusion injury. Faseb J 2001;15:1454-1456.
Jones SP, Trocha SD, Lefer DJ. Pretreatment with simvastatin attenuates myocardial dysfunction after ischemia and chronic reperfusion. Arterioscler Thromb Vasc Biol 2001;21:2059-2064.
Jones S, Gibson M, Rimmer D, Gibson T, Sharp B, Lefer D. Direct vascular and cardioprotective effects of rosuvastatin, a new HMG-CoA reductase inhibitor. J Am Coll Cardiol 2002;40:1172.
Satoh K, Nakai T, Ichihara K. Influence of 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors on mitochondrial respiration in rat liver during ischemia. Eur J Pharmacol 1994;270:365-369.
Satoh K, Yamato A, Nakai T, Hoshi K, Ichihara K. Effects of 3-hydroxy-3-methylglutaryl coenzyme A reductase inhibitors on mitochondrial respiration in ischaemic dog hearts. Br J Pharmacol 1995;116:1894-1898.
Baxter GF, Ferdinandy P. Delayed preconditioning of myocardium: Current perspectives. Basic Res Cardiol 2001;96:329-344.
Huang PL, Huang Z, Mashimo H, et al. Hypertension in mice lacking the gene for endothelial nitric oxide synthase. Nature 1995;377:239-242.
Sharp BR, Jones SP, Rimmer DM, Lefer DJ. Differential response to myocardial reperfusion injury in eNOS-deficient mice. Am J Physiol Heart Circ Physiol 2002;282:H2422-H2426.
Sumeray MS, Rees DD, Yellon DM. Infarct size and nitric oxide synthase in murine myocardium. J Mol Cell Cardiol 2000;32:35-42.
Jones SP, Girod WG, Palazzo AJ, et al. Myocardial ischemiareperfusion injury is exacerbated in absence of endothelial cell nitric oxide synthase. Am J Physiol 1999;276:H1567-H1573.
Lefer DJ, Jones SP, Girod WG, et al. Leukocyte-endothelial cell interactions in nitric oxide synthase-deficient mice. Am J Physiol 1999;276:H1943-H1950.
Kanno S, Lee PC, Zhang Y, et al. Attenuation of myocardial ischemia/reperfusion injury by superinduction of inducible nitric oxide synthase. Circulation 2000;101:2742-2748.
Takano H, Manchikalapudi S, Tang XL, et al. Nitric oxide synthase is the mediator of late preconditioning against myocardial infarction in conscious rabbits. Circulation 1998;98:441-449.
Bolli R, Manchikalapudi S, Tang XL, et al. The protective effect of late preconditioning against myocardial stunning in conscious rabbits is mediated by nitric oxide synthase. Evidence that nitric oxide acts both as a trigger and as a mediator of the late phase of ischemic preconditioning. Circ Res 1997;81:1094-1107.
Guo Y, Jones WK, Xuan YT, et al. The late phase of ischemic preconditioning is abrogated by targeted disruption of the inducibleNOsynthase gene. Proc Natl Acad Sci USA 1999;96:11507-11512.
Zhao L, Weber PA, Smith JR, Comerford ML, Elliott GT. Role of inducible nitric oxide synthase in pharmacological “preconditioning” with monophosphoryl lipid A. J Mol Cell Cardiol 1997;29:1567-1576.
Zhao T, Xi L, Chelliah J, Levasseur JE, Kukreja RC. Inducible nitric oxide synthase mediates delayed myocardial protection induced by activation of adenosine A(1) receptors: Evidence from gene-knockout mice. Circulation 2000;102:902-907.
Xi L, Kukreja RC. Pivotal role of nitric oxide in delayed pharmacological preconditioning against myocardial infarction. Toxicology 2000;155:37-44.
Hattori R, Otani H, Maulik N, Das DK. Pharmacological preconditioning with resveratrol: Role of nitric oxide. Am J Physiol Heart Circ Physiol 2002;282:H1988-H1995.
Xuan YT, Tang XL, Qiu Y, et al. Biphasic response of cardiac NO synthase isoforms to ischemic preconditioning in conscious rabbits. Am J Physiol Heart Circ Physiol 2000;279:H2360-H2371.
Bell RM, Smith CC, Yellon DM. Nitric oxide as a mediator of delayed pharmacological (A(1) receptor triggered) preconditioning; is eNOS masquerading as iNOS? Cardiovasc Res 2002;53:405-413.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Birnbaum, Y., Ashitkov, T., Uretsky, B.F. et al. Reduction of Infarct Size by Short-Term Pretreatment with Atorvastatin. Cardiovasc Drugs Ther 17, 25–30 (2003). https://doi.org/10.1023/A:1024251607923
Issue Date:
DOI: https://doi.org/10.1023/A:1024251607923