Abstract
Purpose : To determine the rates of pregnancy complications following in vitro fertilization in comparison with those in a matched control group.
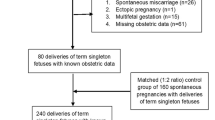
Methods : A total of 13,543 deliveries at the Department of Obstetrics and Gynecology, University of Szeged, between January 1, 1995 and February 28, 2002 were subjected to retrospective analysis. The 230 (1.7%) pregnancies following IVF-ET were evaluated and matched with spontaneous pregnancies concerning age, parity, gravidity, and previous obstetric outcome. Demographic and selected maternal characteristics, pregnancy and labor complications, and neonatal outcome were compared in the two groups.
Results : The pregnancy complication rate was partly significantly higher among the singleton IVF-ET pregnancies. The obstetric risk was elevated, though not significantly concerning twin pregnancies.
Conclusions : IVF-ET presents an additional obstetric risk. The neonatal outcome displays a significant difference only concerning an increased premature birth rate of singleton pregnancies. Triplet IVF-ET pregnancies involve a much higher risk of both pregnancy complications and neonatal outcome.
Similar content being viewed by others
References
Steptoe PC, Edwards RG: Birth after the reimplantation of a human embryo. Lancet 1978;2:366
Bergh T, Ericson A, Hillensjo T, Nygren KG, Wennerholm UB: Deliveries and children born after in-vitro fertilisation in Sweden 1982–95: A retrospective cohort study. Lancet 1999;354:1579-1585
Koudstaal J, Braat DDM, Bruinse HW, Naaktgeboren N, Vermeiden JPW, Visser GHA: Obstetric outcome of singleton pregnancies after IVF: A matched control study in four Dutch University hospitals. Hum Reprod 2000;15:1819-1825
Lambalk CB, van Hooff M: Natural versus induced twinning and pregnancy outcome: A Dutch nationwide survey of primiparous dizygotic twin deliveries. Fertil Steril 2001;4:731-736
Lancaster PAL: Australian In Vitro Fertilization Collaborative Group. High incidence of preterm births and early losses in pregnancy after IVF. BMJ 1985;291:1160-1163
Doyle P, Beral V, Macononchie N: Preterm delivery, low birth weight and small-for-gestational-age in liveborn singleton babies resulting from in-vitro fertilization. Hum Reprod 1992;7:425-428
Seoud MA, Toner JP, Kruithoff C, Muasher SJ: Outcome of twin, triplet and quadruplet in vitro fertilization pregnancies: The Norfolk experience. Fertil Steril, 1992;57:825-834
Hansen M, Kurinczuk JJ, Bower C, Webb S: The risk of major birth defects after intracytoplasmic sperm injection and in vitro fertilization. N Eng J Med 2002;346:725-730
Ericson A, Källen B: Congenital malformations in infants born after IVF: A population-based study. Hum Reprod 2001;16:504-509
Bonduelle M, Liebaers I, Deketerlaere V, Derde M-P, Camus M, Devroey P, Steirteghem AV: Neonatal data on a cohort of 2889 infants born after ICSI (1991–1999) and of 2995 infants born after IVF (1983–1999). Hum Reprod 2002;3:671-694
Reubinoff BE, Samueloff A, Friedler S, Schenker JG, Lewin A: Is the obstetric outcome of in vitro fertilized singleton gestations different from natural ones? A controlled study. Fertil Steril, 1997;67:1077-1083
Tan SL, Doyle P, Campbell S, Beral V, Risk B, Brinsden P: Obstetric outcome of in-vitro fertilization pregnancies compared with normally conceived pregnancies. Am J Obstet Gynecol 1992;167:778-784
Verlaenen H, Cammu H, Derde MP, Amy JJ: Singleton pregnancy after in-vitro fertilization: Expectations and outcome. Obstet Gynecol 1995;86:906-910
Koudstaal J, Bruinse HW, Helmerhorst FM, Vermeiden JPW, Willemsen WNP, Visser GHA: Obstetric outcome of twin pregnancies after in-vitro fertilization: A matched control study in four Dutch University hospitals. Hum Reprod 2000;15: 935-940
Hungarian Statistical Office: Demographic Year Book. Budapest, Hungarian Statistical Office, 2001
SPSS for Windows, Chicago: SPSS, 1999 (software)
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Zádori, J., Kozinszky, Z., Orvos, H. et al. Dilemma of Increased Obstetric Risk in Pregnancies Following IVF-ET. J Assist Reprod Genet 20, 216–221 (2003). https://doi.org/10.1023/A:1024103427374
Issue Date:
DOI: https://doi.org/10.1023/A:1024103427374