Abstract
Purpose. This study compared the sensitivity of rat prostate MAT-LyLu primary and lymph node metastatic tumors to taxol.
Methods. Tumors were established by subcutaneous implantation of tumor cells in a hind leg (primary site) of male Copenhagen rats. Lymph node metastases were used for serial transplantation. Eleven pairs of primary and metastatic tumors between the sixth and twentieth generations were harvested and maintained as 3-dimensional histocultures. The effects of taxol (24 hr treatment at 1 nM to 10 µM) were measured by the appearance of apoptotic cells, and by the inhibition of DNA precursor (thymidine) incorporation. To determine the basis of differential sensitivity of primary and metastatic tumors to the DNA inhibition, we examined the expression of multidrug resistance p-glycoprotein (Pgp) and the accumulation of 3H-taxol after 24 hr exposure and the retention after a 48 hr washout period.
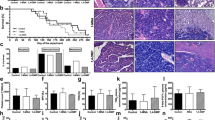
Results. The fraction of apoptotic cells increased linearly with the logarithm of taxol concentration to a maximal value of 25%; the concentration-response curves for primary and metastatic tumors were superimposable. Taxol produced a sigmoidal, concentration-dependent inhibition of thymidine incorporation; the maximal inhibition of ~40% was reached at 0.1 and 1 µM for primary and metastatic tumors, respectively. Within the primary or metastatic subgroups, the IC30 (drug concentration that produced a 30% inhibition of DNA synthesis) among consecutive generations varied by < 5 fold, but the primary tumor consistently showed a lower IC30 than the daughter or the parent metastatic tumor (mean, 20-fold; median, 15-fold; range, 6- to 56-fold). The finding that the lower drug sensitivity in metastatic tumors was not exhibited in its daughter primary tumor but was regained in its daughter metastatic tumors suggests that the chemoresistant phenotype is maintained only in lymph nodes and not in the primary site. There were no differences in the Pgp status (neither tumor expressed Pgp), accumulation and retention of taxol in primary and metastatic tumors.
Conclusions. Taxol induced apoptosis and inhibited DNA synthesis in the rat MAT-LyLu primary and lymph node metastatic tumors. The apoptotic effect was not different among the two tumors, whereas the primary tumor was more sensitive to the inhibition of DNA synthesis. The differential sensitivity of the two tumors to the DNA effect is not associated with a difference in Pgp expression, drug accumulation nor drug retention, and appears to be associated with changes that are linked to lymph node metastasis.
Similar content being viewed by others
REFERENCES
E. K. Rowinsky, N. Onetto, R. M. Canetta, and S. G. Arbuck. Taxol: the first of the taxanes, an important new class of antitumor agents. Semin. Oncol. 19:646–662 (1992).
S. G. Arbuck and B. Blaylock. Taxol: Clinical results and current issues in development. In Suffness, M. (ed), Taxol-Science and Applications, Boca Raton, 1995, pp. 379–415.
S. B. Horwitz. Taxol (paclitaxel): Mechanism of action. Annuals Oncol. 5:53–56 (1994).
K. L. Crossin and D. H. Carney. Microtubule stabilization by taxol inhibits initiation of DNA synthesis by thrombin and epidermal growth factor. Cell 27:341–350 (1981).
Y. Liu, K. Bhalla, C. Hill, and D. G. Priest. Evidence for involvement of tyrosine phosphorylation in taxol-induced apoptosis in a human ovarian tumor cell line. Biochem. Pharmacol. 48:1265–1272 (1994).
K. Bhalla, A. M. Ilerado, E. Tourkina, C. Tang, M. E. Mahoney, and Y. Huang. Taxol induces internucleosomal DNA fragmentation associated with programmed cell death in human myeloid leukemia cells. Leukemia 7:563–568 (1993).
L. Milas, N. R. Hunter, and B. Kurdoglu. Kinetics of mitotic arrest and apoptosis in murine mammary and ovarian tumors treated with taxol. Cancer Chemother. Pharmacol. 35:297–303 (1995).
M. E. Stearns and M. Wang. Taxol blocks processes essential for prostate tumor cell (PC-3 ML) invasion and metastasis. Cancer Res. 52:3776–3781 (1992).
S. B. Horwitz, D. Cohen, S. Rao, I. Ringel, H. J. Shen and C. P. H. Yang. Taxol: Mechanisms of action and resistance. J. Natl. Cancer Inst. 15:55–61 (1993).
S. Roy and S. B. Horwitz. A phosphoglycoprotein associated with taxol-resistance in J774.2 cells. Cancer Res. 45:3856–3863 (1985).
K. Bhalla, Y. Huang, C. Tang, S. Self, S. Ray, M. E. Mahoney, V. Ponnathpur, E. Tourkina, A. M. Ibrado, and G. Bullock. Characterization of a human myeloid cell line highly resistant to taxol. Leukemia 8:465–475 (1994).
L. A. Speicher, L. R. Barone, A. E. Chapman, G. R. Hudes, N. Laning, C. D. Smith, and K. D. Tew. P-glycoprotein binding and modulation of the multidrug-resistant phenotype by estramustine. J. Natl. Cancer Inst. 86:688–694 (1994).
G. H. Mickisch, T. Licht, G. T. Merlino, M. M. Gottesman, and I. Pastan. Chemotherapy and chemosensitization of transgenic mice which express the human multidrug resistance gene in bone marrow: efficacy, potency, and toxicity. Cancer Res. 51:5417–5424 (1991).
B. Jachez, R. Nordmann, and F. Loor. Restoration of taxol sensitivity of multidrug-resistant cells by the cyclosporine SDZ PSC 833 and the cyclopeptolide SDZ 280–446. J. Natl. Cancer Inst. 85:478–483 (1993).
M. Lenert, S. Emerson, S. D. William, R. de Giuli, and S. E. Salmon. In vitro evaluation of chemosensitizers for clinical reversal of p-glycoprotein-associated taxol resistance. Monogr. Natl. Cancer Inst. 15:63–67 (1993).
J. R. Roberts, D. C. Allison, R. C. Sonehower, E. K. Rowinsky. Development of polyploidization in taxol-resistant human leukemia cells in vitro. Cancer Res. 50:710–716 (1990).
J. E. Liebmann, S. M. Hahn, J. A. Cook, C. Lipschultz, J. B. Mitchell, and D. C. Kaufman. Glutathione depletion of L-buthionine sulfoximine antagonizes taxol cytotoxicity. Cancer Res. 53:2066–2070 (1993).
F. C. Lowe, and J. T. Isaacs. Biochemical methods for predicting metastatic ability of prostatic cancer utilizing the Dunning R-3327 rat prostatic adenocarcinoma system as a model. Cancer Res. 44:744–752 (1984).
R. A. Vesico, C. H. Redfern, T. J. Nelson, S. Ugoretz, P. H. Stern, and R. M. Hoffman. In vivo-like drug responses of human tumors growing in three-dimensional gel-supported primary culture. Proc. Natl. Acad. Sci. U.S.A. 84:5029–5033 (1987).
F. H. Schroeder and S. J. Mackensen. Human prostatic adenoma and carcinoma in cell culture-effects of androgen-free culture medium. Invest. Urol. 12:176–181 (1974).
D. D. Mickey. Growth and differentiation factors in prostatic tissue. In M. Motta and M. Serio (eds), Hormonal therapy of prostatic diseases: basic and clinical aspects, Medicom, Bussum, The Netherlands, 1988, pp 13–47.
M. G. Wientjes, T. G. Pretlow, R. A. Badalament, J. K. Burgers, and J. L.-S. Au. Histocultures of human prostate tissues for pharmacologic evaluation. J. Urol. 153:1299–1302 (1995).
D. R. Kohler, and B. R. Goldspiel. Paclitaxel (taxol). Pharmacotherapy 14:3–34 (1994).
J. F. R. Kerr, M. Clay, and B. V. Harmon. Apoptosis: Its significance in cancer and cancer therapy. Cancer 73:2013–2026 (1994).
Y. Gan, M. G. Wientjes, D. E. Schuller, and J. L.-S. Au. Pharmacodynamics of taxol in human head and neck tumors. Cancer Res. 56:2086–2093 (1996).
N. M. Lopes, E. G. Adams, T. W. Pitts, B. K. Bhuyan. Cell kill kinetics and cell cycle effects of taxol on human and hamster ovarian cell lines. Cancer Chemother. Pharmacol. 32:235–242 (1993).
J. Liebmann, J. A. Cook, C. Lipschultz, D. Teague, J. Fisher, and J. B. Mitchell. The influence of Cremophor EL on the cell cycle effects of paclitaxel (taxol) in human tumor cell lines. Cancer Chemother. Pharmacol. 33:331–339 (1994).
J. L.-S. Au, N. E. Millenbaugh, J. E. Kalns, C. T. Chen, and M. G. Wientjes. Pharmacodynamics of taxol in human solid tumors. Proc. Am. Assoc. Cancer Res. 35:426 (1994).
J. L.-S. Au, M. G. Wientjes, T. J. Rosol, A. Koolemans-Beynen, E. A. Goebel, and D. E. Schuller. Histocultures of patient head and neck tumors for pharmacodynamic studies. Pharm. Res. 10:1493–1499 (1993).
T. S. Schmittgen, M. G. Wientjes, R. A. Badalament, and J. L.-S. Au. Pharmacodynamics of mitomycin C in cultured human bladder tumors. Cancer Res. 51:3849–3856 (1991).
Y. Gan, M. G. Wientjes, R. A. Badalament, and J. L.-S. Au. Pharmacodymamics of doxorubicin in human bladder tumors. Clin. Cancer Res. In press (1996).
T. Cresteil, B. Monsarrat, P. Alvinerie, J. M. Treluyer, I. Vieira, and M. Wright. Taxol metabolism by human liver microsomes: identification of cytochrome p450 isozymes involved in its transformation. Cancer Res. 54:386–392 (1994).
I. Kjonniksen, B. Knut, and O. Fodstad. Site-dependent differences in sensitivity of LOX human melanoma tumors in nude rats to dacarbazine and mitozolomide but not to doxorubicin and cisplatin. Cancer Res. 52:1347–1351 (1992).
C. Wilmanns, D. Fan, C. A. O'Brian, C. D. Bucana, and I. J. Fidler. Orthotopic and ectopic organ environments differentially influence the sensitivity of murine colon carcinoma cells to doxorubicin and 5-fluorouracil. In. J. Cancer. 52:98–104 (1992).
C. Wilmanns, D. Fan, C. A. O'Brian, R. Radinsky, C. D. Bucana, R. Tsan and I. J. Fidler. Modulation of doxorubicin sensitivity and level of P-glycoprotein expression in human colon carcinoma cells by ectopic and orthotopic environments in nude mice. Int. Oncol. 3:413–422 (1993).
T. Furukawa, T. Kubota, M. Watanabe, T.-H. Kuo, M. Kitajima, and R. M. Hoffman. Differential chemosensitivity of local and metastatic human gastric cancer after orthotopic transplantation of histologically intact tumor tissue in nude mice. Int. J. Cancer. 54:397–401 (1993).
I. J. Fidler, C. Wilmanns, A. Staroselsky, R. Radinsky, Z. Dong, and D. Fan. Modulation of tumor cell response to chemotherapy by the organ environment. Cancer Metast. Rev. 13:209–222 (1994).
B. A. Teicher, T. S. Herman, S. A. Holden, Y. Wang, M. R. Pfeffer, J. W. Crawford, and E. Frei. Tumor resistance to alkylating agents conferred by mechanisms operative only in vivo. Science 247:1457–1461 (1990).
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Yen, WC., Wientjes, M.G. & Au, J.LS. Differential Effect of Taxol in Rat Primary and Metastatic Prostate Tumors: Site-Dependent Pharmacodynamics. Pharm Res 13, 1305–1312 (1996). https://doi.org/10.1023/A:1016053412582
Issue Date:
DOI: https://doi.org/10.1023/A:1016053412582