Abstract
Our Department of Plastic and Reconstructive Surgery has routinely been using amnion preserved in glycerol for the treatment of debrided II° burns. This treatment is almost pain free and requires fewer changes of dressings and fewer anaesthetics. It also prevents overgrowing granulation tissue and lessens scarring.
Since 1910 amnion has been used as biological wound dressing. Its advantages such as reduced loss of protein and electrolytes, fluids and energy as well as reducing the risk of infection and accelerated regeneration of the epithelium have been well documented in medical literature.
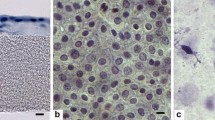
In order to more closely examine the question of possible changes to the micro structure of the amnion through preservation and rehydration as well as the interaction between transplanted tissue and recipient, we have carried out several light and electron microscopic studies.
Results showed that neither the treatment with glycerol, nor the pretransplantation rehydration eliminates the monolayer of surface epithelium of the amnion. Its complex architecture remains intact during the preservation process and is therefore suitable as a matrix for the growth of keratinocytes and thereby the healing process.
In clinical use we found amnion to be an excellent wound dressing as it allows proper control of fluid, has sufficient permeability for gases, has good thermal properties, is impervious to micro-organisms and is free from toxic material.
Similar content being viewed by others
References cited
Bankiewicz K,Palmatier M,Plunkett R,Cummins A andOldfield E (1994) Reversal of hemiparkinsonian syndrome in nonhuman primates by amnion implantation into caudate nucleus. J Neurosurg 81: 869–876
Basile A RD (1982) A comparative study of glycerinized and lyophilized porcine skin in dressing for third-degree burns. Plast Reconstr Surg 69: 969–974
Bose B (1979) Burn wound dressing with human amniotic membrane. Ann Royal College of Surgeons of Engl 61: 444–447
Colocho G,Graham WP,Greene AE,Matheson DW andLynch D (1974) Human amniotic membrane as a physiologic wound dressing. Arch Surg 109: 370–373
Davis GE,Blaker SN,Engvall E,Varon S,Manthorpe M andGage FH 1987) Human amnion membrane serves as a substratum for growing axons in vitro and in vivo. Science 236: 1106–1110
Göbel P andSchubert W (1990) Unsere Erfahrungen mit der Deckung kindlicher Verbrennungswunden durch Amnion. Beitr Orthop Traumatol 37: 495–498
Hermans MHE (1989) Clinical experience with glycerol preserved donor skin treatment in partial thickness burns. Burns 14: 57–59
Horibe N,Okamoto T,Itakura A,Nakanishi T,Suzuki T,Kazeto S andTomoda Y (1995) Levels of hepatocyte growth factor in maternal serum and amniotic fluid. Am J Obstetrics and Gynecology 173: 937–942
Klima G,Zerlauth B,Richter J andSchmidt W (1989) Die Mikrotextur von Amnion-und Chorionbindegewebe. Anatomischer Anzeiger 168: 395–400
Kruse FE, Rohrschneider K and Völcker HE (1998) Transplantation von Amnionmembran zur Rekonstruktion der Augenoberfläche. Ophthalmologe 95: 114–119
Lin SN,Lai CS,Hou MF andYang ChCh (1985) Amnion overlay meshed skin autograft. Burns 11: 374–378
Malak TM,Ocleford CD,Bell SC,Dalgleish R,Bright N andMacvicar J (1993) Confocal immunofluorescence localization of collagen types I, III, IV, V and VI and their ultrastructural organization in term human fetal membranes. Placenta 14: 385–406
Maral T,Borman H,Arslan H,Demirhan B,Akinbingol G andHaberal M (1999) Effectiveness of human amnion preserved long-term in glycerol as a temporary biological dressing. Burns 25: 625–635
Rao TV andChandrasekharam V (1981) Use of dry human and bovine amnion as a biological dressing. Arch Surg 116: 891–896
Robson MC andKrizek TJ (1973) The effect of human amniotic membranes on the bacteria population of infected rat burn. Ann Surg 177: 144–149
Ramakrishnan KM andJayaraman V (1997) Management of partial-thickness burn wounds by amniotic membrane: a costeffective treatment in developing countries. Burns 23 (Suppl.1): 33–36
Sabella N (1913) Use of fetal membranes in skin grafting. Medical Records of New York 83: 478 quoted in Maral et al. (1999)
Sakuragawa N,Yoshikawa H andSasaki M (1992) Amniotic tissue transplantation: clinical and biochemical evaluations. Brain and Development 14: 7–11
Scaggiante B,Pineschi A,Sustersich M,Adolina M,Agosti E andRomeo D (1987) Successful therapy of Niemann-Pick disease by implantation of human amniotic membrane. Transplantation 44: 59–61
Schmidt W,Pfaller K andSchwarzfurtner H (1982) Licht-und Elektronen-mikroskopische Untersuchungen an den Eihäuten des Menschen. Zentralblatt für Gynäkologie 104: 385–396
Talmi YP,Sigler L,Inge E,Finkelstein Y andZohar Y (1991) Antibacterial properties of human amniotic membranes. Placenta 12: 285–288
Tseng SCG,Prabhasawat P,Barton K,Gray T andMeller D (1998) Amniotic membrane transplantation with or without limbal allografts for corneal surface reconstruction in patients with limbal stem cell deficiency. Arch Ophthalmol 116: 431–441
van Baare J,Ligtvoet EEJ andMiddelkoop E (1998) Microbiological evaluation of glycerolized cadaveric donor skin. Transplantation 65: 966–970
Ward DM,Benneth JP,Burgos H andFabre J (1989) The healing of chronic venous leg ulcers with prepared human amnion. Br J Plastic Surg 42: 463–467
Zohar Y,Talmi YP,Finkelstein Y,Shvili Y,Sadov R andLaurian N (1987) Use of human amniotic membrane in otolaryngologic practise. Laryngoscope 97: 978–980
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rejzek, A., Weyer, F., Eichberger, R. et al. Physical Changes of Amniotic Membranes Through Glycerolization for The Use as an Epidermal Substitute. Light and Electron Microscopic Studies. Cell Tissue Banking 2, 95–102 (2001). https://doi.org/10.1023/A:1014316232009
Issue Date:
DOI: https://doi.org/10.1023/A:1014316232009