Abstract
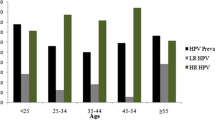
The association between certain human papillomaviruses (HPV) and cervical intraepithelial neoplasia (CIN) is well documented, but still unknown among Croatian women. In 1995, women between the age of 17 and 64 with cytomorphologically abnormal smears (CIN I–IV) were tested for the presence of HPV. Consensus and specific primers were used in the polymerase chain reaction (PCR) to detect the most common types: 6, 11, 16, 18, 31 and 33, as well as the unknown-risk HPV types (HPV X). Out of 379 specimens, 163 (43%) contained one or more HPV types. Coinfection with different HPV types in the same sample was observed in 16 cases. Beside low-risk HPV 6/11 (25.8%) the most frequently observed types were high-risk HPV types 16 (20.2%) and 31 (17.8%). Globally, the HPV positivity rate declines with age. The presence of HPV DNA significantly increased from 35.5 to 61.1% along with the severity of the cervical intraepithelial neoplasia (CIN I– IV). HPV type 6/11 was strongly associated with CIN I (33.8%), HPV type 31 with CIN II (22.9%), and HPV type 16 with CIN III (50%).
Similar content being viewed by others
References
zur Hausen H. Molecular pathogenesis of cancer of the cervix and its causation by specific human papillomavirus types. Curr Topics Microbiol Immunol 1994; 186: 131–155.
Muñoz N, Bosch FX, de Sanjosé S, et al. The causal link between human papillomavirus and invasive cervical cancer, a population based study in Columbia and Spain. Int J Cancer 1992; 52: 743–749.
Bosch FX, Manos MM, Muñoz N, et al (The IBSCC study group). Prevalence of human papillomavirus in cervical cancer: A worldwide perspective. J Nat Cancer Inst 1995; 87: 796–802.
de Villiers EM. Human pathogenic papillomavirus types: An update. Curr Topics Microbiol Immunol 1994; 186: 1–12.
Schneider A. Natural history of genital papillomavirus infections. Intervirology 1994; 37: 201–214.
Richart RM. Cervical intraepithelial neoplasia: A review. Pathol Annu 1973; 3: 301–328.
Van Ranst M, Kaplan JB, Burk RD. Phylogenetic classification of human papillomaviruses: Correlation with clinical manifestation. J Gen Virol 1992; 66: 5714–5725.
Lörincz AT, Reid R, Jenson AB, et al. Human papillomavirus infection of the cervix: Relative risk associations of 15 common anogenital types. Obstet Gynecol 1992; 79: 328–337.
Gravitt PE, Manos MM. Polymerase chain reactionbased methods for the detection of human papillomavirus DNA. In: Muñoz N, Bosch FX, Shah KV, Meheus A (eds), The epidemiology of cervical cancer and human papillomavirus. Lyon: IARC, 1992: 121–133.
Maniatis T, Frisch EF, Sambrook J (eds). Molecular Cloning. Cold Spring Harbor, NY: Cold Spring Harbor Laboratory, 1982 (A laboratory manual).
Manos MM, Ting Y, Wright DK, et al. The use of polymerase chain reaction amplification for the detection of genital human papillomaviruses. In: Furth M, Greaves M (eds), Molecular diagnostics of human cancer: Cancer cells. Cold Spring Harbor, NY: Cold Spring Harbor Laboratory, 1989: 209–214.
Novelli G, Gennarelli M, de Santis, et al. Inosine-containing primers in human papillomavirus detection by polymerase chain reaction. Biomed Pharmacother 1992; 46: 167–169.
Bell DA, Taylor JA, Paulson DF, et al. Genetic risk and carcinogen exposure: A common inherited defect of the carcinogen-metabolism gene glutathione Stransferase M1 (GSTM1) that increase susceptibility to bladder cancer. J Nat Cancer Inst 1993; 85: 1159–1164.
Soler C, Allibewrt P, Chardonnet Y, et al. Detection of human papillomavirus types 6, 11, 16 and 18 in mucosal and cutaneous lesions by the multiplex polymerase chain reaction. J Virol Methods 1991; 35: 143–157.
van den Brule AJC, Meijer CLJ, Bakels V, et al. Rapid detection of human papillomavirus in cervical scrapes by combined general primer-mediated and type-specific polymerase chain reaction. J Clin Microbiol 1990; 28: 2739–2743.
Saiki RK, Scharf S, Faloona F, et al. Enzymatic amplification of beta-globin genomic sequences and restriction site analysis for diagnosis of sickle cell anemia. Science 1985; 130: 1350–1354.
Grce M, Magdić L, Kocijan I, Pavelić K. Increase of genital human papillomavirus infection among men and women in Croatia. Anticancer Res 1996; 16: 1039–1042.
Gjooen K, Olsen AO, Magnus P, et al. Prevalence of human papillomavirus in cervical scrapes, as analyzed by PCR, in a population-based sample of women with and without cervical dysplasia. APMIS 1996; 104: 68–74.
Figueroa JP, Ward E, Luthi TE, et al. Prevalence of human papillomavirus among STD clinic attenders in Jamaica: Association of younger age and increased sexual activity. Sex Trans Dis 1995; 22: 114–118.
Melkert PW, Hopman E, van den Brule AJ, et al. Prevalence of HPV in cytomorphologically normal cervical smears, as determined by the polymerase chain reaction, is age-dependent. Int J Cancer 1993; 53: 919–923.
zur Hausen H, de Villiers EM. Human papillomaviruses. Ann Rev Microbiol 1994; 48: 427–447.
Remmink AJ, Walboomers JMM, Helmerhorst TJM, et al. The presence of persistent high-risk HPV geno-types in dysplastic cervical lesions is associated with progressive disease: Natural history up to 36 months. Int J Cancer 1995; 61: 306–311.
Barrett TJ, Silbar JD, McGinley JP. Genital warts: A veneral disease. JAMA 1954; 154: 333–334.
Barrasso R, de Brux J, Croissant O, Orth G. High prevalence of papillomavirus-associated penile intraepithelial neoplasia in sexual partners of women with cervical intraepithelial neoplasia. N Engl J Med 1987; 317: 916–923.
Campion MJ, McCance DJ, Mitchell HS, et al. Subclinical penile human papillomavirus infection and dysplasia in consorts of women with cervical neoplasia. Genitourin Med 1988; 64: 90–99.
Kaye JN, Starkey WG, Kell B, et al. Human papillomavirus type 16 in infants: Use of DNA sequence analyses to determine the source of infection. J Gen Virol 1996; 77: 1139–1143.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Grce, M., Husnjak, K., Magdić, L. et al. Detection and typing of human papillomaviruses by polymerase chain reaction in cervical scrapes of Croatian women with abnormal cytology. Eur J Epidemiol 13, 645–651 (1997). https://doi.org/10.1023/A:1007323405069
Issue Date:
DOI: https://doi.org/10.1023/A:1007323405069