Abstract
The aim of our study was firstly to assess whether areas of capillary non-perfusion in diabetic retinopathy are associated with reduction of retinal light sensitivity and secondly to assess whether automated perimetry can serve as a screening method for evaluation of retinal perfusion.
32 eyes with diabetic retinopathy and 30 eyes of controls underwent visual field testing on the 30-2program of the Humphrey field analyser and fluorescein angiography. The results are compared with the‘superimposition technique’.
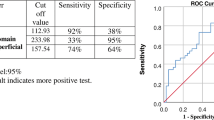
In 93.4% of our diabetic eyes (30 from 32) areas of capillary non-perfusion demonstrated by fluorescein angiography were associated with areas of reduced retinal sensitivity. The correlation between visual field defects and areas of reduced retinal perfusion was significant with probability more than 99% (P<0.01).
In view of our findings we recommend automated static perimetry as a very sensitive method for evaluation of retinal perfusion in diabetic patients.
Similar content being viewed by others
References
Statpac Users Guide. San Leandro, CA, Allergan Humphrey, 1986.
Flammer J. Automatisierte Perimetrie. Therapeutische Umschau 1990; 47(4): 298–302.
Anderson DR. Automatic Static Perimetry. St.Louis: Mosby Year Book, 1992.
Stewart WC. Avoiding mistakes in interpreting visual fields, Part I: Basic Concepts. Clinical Signs in Ophthalmol 1993; 14(3): 2–15.
Stewart WC. Avoiding mistakes in interpreting visual fields, Part II: Evaluating the Printout. Clinical Signs in Ophthalmol 1993; 14(4): 2–15.
Quigley HA, Dunkelberger GR, Green WR. Retinal ganglion cell atrophy correlated with automated perimetry in human eyes with glaucoma. Am J Ophthalmol 1989; 107: 543–64.
Tric GL, Burde RM, Gordon MO, et al. The relationship between hue discrimination and contrast sensitivity deficits in patients with diabetes mellitus. Ophthalmology 1988; 95: 693–8.
Roy MS, McCulloch C, Hanna AK, Mortimer C. Colour vision in long-standing diabetes mellitus. Br J Ophthalmol 1984; 68: 215–7.
Arden GB, Hamilton AMP, Wilson-Hoyt J, et al. Pattern electroretinograms become abnormal when background retinopathy deteriorates to a preproliferative stage: possible use as a screening test. Br J Ophthalmol 1986; 70: 330–5.
Trick GL, Trick LR, Kilo C. Visual field defects in patients with insulin-dependent and noninsulin-dependent diabetes. Ophthalmology 1990; 97: 475–82.
Roth JA. Central visual field in diabetes. Br J Ophthalmol 1969; 53: 16–25.
Wisznia KI, Liebermann TW, Leopold IH. Visual fields in diabetic retinopathy. Br J Ophthalmol 1971; 55: 183–8.
Greite JH, Zumbansen HP, Adamczyk R. Visual field in diabetic retinopathy. In: Greve EL, Verriest G. Fourth International Visual Field Symposium, Bristol, April 13–16, 1980. The Hague: W Junk, 1981: 25–32 (Doc Ophthalmol Proc Series 26).
Chee CKL, Flanagan DW. Visual field loss with capillary non-perfusion in preproliferative and early proliferative diabetic retinopathy. Br J Ophthalmol 1993; 77: 726–30.
Khosla PK, Gupta V, Tewari HK, Kumar A. Automated Perimetric Changes Following Panretinal Photocoagolation in Diabetic Retinopathy. Ophthalmic Surg 1993; 24(4): 256–61.
Bek T, Lund-Anderson H. Localized blood-retinal barrier leakage and retinal light sensitivity in diabetic retinopathy. Br J Ophthalmol 1990; 74: 388–92.
Bek T, Lund-Anderson H. Cotton-wool spots and retinal light sensitivity in diabetic retinopathy. Br J Ophthalmol 1991; 75: 13–7.
Bell JA, Feldon SE. Retinal microangiopathy: correlation of Octopus perimetry with fluorescein angiography. Arch Ophthalmol 1984; 102: 1294–8.
Diezel PB, Willert HG. Morphologie und Histochemie der harten und weichen Exudate der Retina bei Diabetes mellitus und essentieller Hypertonie. Klin Monatsbl Augenheilkd 1961; 139: 475–91.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Pahor, D. Automated static perimetry as a screening method for evaluation of retinal perfusion in diabetic retinopathy. Int Ophthalmol 21, 305–309 (1997). https://doi.org/10.1023/A:1006024305992
Issue Date:
DOI: https://doi.org/10.1023/A:1006024305992