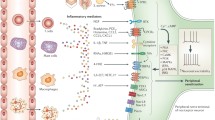
Summary
Neuropathic pain syndromes arise from dysfunction of the nerve itself, through traumatic or nontraumatic injury. Unlike acute pain syndromes, the pain is long-lasting and does not respond to common analgesic therapies. Drugs that disrupt nerve conduction and transmission or central sensitization, currently the only effective treatments, are only modestly effective for a portion of the patients suffering from neuropathic pain and come with the cost of serious adverse effects. Neurodegeneration, as a reaction to nerve trauma or chronic metabolic or chemical intoxication, appears to be an underlying cause of neuropathic pain. Identifying mechanisms of neurodegeneration and designing neuroprotective therapies is an ambitious goal toward treating or even preventing the development of these disabling disorders.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Cata JP, Weng HR, Lee BN, Reuben JM, Dougherty PM. Clinical and experimental findings in humans and animals with chemotherapy-induced peripheral neuropathy. Minerva Anestesiol 2006;72: 151–169.
Davies M, Brophy S, Williams R, Taylor A. The prevalence, severity, and impact of painful diabetic peripheral neuropathy in type 2 diabetes. Diabetes Care 2006;29: 1518–1522.
Vincent AM, Russell JW, Low P, Feldman EL. Oxidative stress in the pathogenesis of diabetic neuropathy. Endocr Rev 2004;25: 612–628.
Leinninger GM, Edwards JL, Lipshaw MJ, Feldman EL. Mechanisms of disease: mitochondria as new therapeutic targets in diabetic neuropathy. Nat Clin Pract Neurol 2006;2: 620–628.
Tomlinson DR, Gardiner NJ. Glucose neurotoxicity. Nat Rev Neurosci 2008;9: 36–45.
McArthur JC, Brew BJ, Nath A. Neurological complications of HIV infection. Lancet Neurol 2005;4: 543–555.
Childs EA, Lyles RH, Selnes OA, et al. Plasma viral load and CD4 lymphocytes predict HIV-associated dementia and sensory neuropathy. Neurology 1999;52: 607–613.
Tagliati M, Grinnell J, Godbold J, Simpson DM. Peripheral nerve function in HIV infection: clinical, electrophysiologic, and laboratory findings. Arch Neurol 1999;56: 84–89.
Schifitto G, McDermott MP, McArthur JC, et al. Markers of immune activation and viral load in HIV-associated sensory neuropathy. Neurology 2005;64: 842–848.
Lichtenstein KA, Armon C, Baron A, Moorman AC, Wood KC, Holmberg SD; HIV Outpatient Study Investigators. Modification of the incidence of drug-associated symmetrical peripheral neuropathy by host and disease factors in the HIV outpatient study cohort. Clin Infect Dis 2005;40: 148–157.
Ferrari S, Vento S, Monaco S, et al. Human immunodeficiency virus-associated peripheral neuropathies. Mayo Clin Proc 2006; 81: 213–219.
Pardo CA, McArthur JC, Griffin JW. HIV neuropathy: insights in the pathology of HIV peripheral nerve disease. J Peripher Nerv Syst 2001;6: 21–27.
Simpson DM, Kitch D, Evans SR, et al.; ACTG A5117 Study Group. HIV neuropathy natural history cohort study: assessment measures and risk factors. Neurology 2006;66: 1679–1687.
Cherry CL, Skolasky RL, Lal L, et al. Antiretroviral use and other risks for HIV-associated neuropathies in an international cohort. Neurology 2006;66: 867–873.
Keswani SC, Jack C, Zhou C, Höke A. Establishment of a rodent model of HIV-associated sensory neuropathy. J Neurosci 2006; 26: 10299–10304.
Pettersen JA, Jones G, Worthington C, et al. Sensory neuropathy in human immunodeficiency virus/acquired immunodeficiency syndrome patients: protease inhibitor-mediated neurotoxicity. Ann Neurol 2006;59: 816–824.
Ellis RJ, Marquie-Beck J, Delaney P, et al.; CHARTER Group. Human immunodeficiency virus protease inhibitors and risk for peripheral neuropathy. Ann Neurol 2008;64: 566–572.
Cherry CL, McArthur JC, Hoy JF, Wesselingh SL. Nucleoside analogues and neuropathy in the era of HAART. J Clin Virol 2003;26: 195–207.
Dalakas MC, Semino-Mora C, Leon-Monzon M. Mitochondrial alterations with mitochondrial DNA depletion in the nerves of AIDS patients with peripheral neuropathy induced by 2′3′-dideoxycytidine (ddC). Lab Invest 2001;81: 1537–1544.
Keswani SC, Chander B, Hasan C, Griffin JW, McArthur JC, Hoke A. FK506 is neuroprotective in a model of antiretroviral toxic neuropathy. Ann Neurol 2003;53: 57–64.
Zhu Y, Antony JM, Martinez JA, et al. Didanosine causes sensory neuropathy in an HIV/AIDS animal model: impaired mitochondrial and neurotrophic factor gene expression. Brain 2007;130: 2011–2023.
Robinson B, Li Z, Nath A. Nucleoside reverse transcriptase inhibitors and human immunodeficiency virus proteins cause axonal injury in human dorsal root ganglia cultures. J Neurovirol 2007;13: 160–167.
El Idrissi A, Trenkner E. Growth factors and taurine protect against excitotoxicity by stabilizing calcium homeostasis and energy metabolism. J Neurosci 1999;19: 9459–9468.
Markham A, Cameron I, Franklin P, Spedding M. BDNF increases rat brain mitochondrial respiratory coupling at complex I, but not complex II. Eur J Neurosci 2004;20: 1189–1196.
Wolf S, Barton D, Kottschade L, Grothey A, Loprinzi C. Chemotherapy-induced peripheral neuropathy: prevention and treatment strategies. Eur J Cancer 2008;44: 1507–1515.
Wilkes G. Peripheral neuropathy related to chemotherapy. Semin Oncol Nurs 2007;23: 162–173.
Hausheer FH, Schilsky RL, Bain S, Berghorn EJ, Lieberman F. Diagnosis, management, and evaluation of chemotherapy-induced peripheral neuropathy. Semin Oncol 2006;33: 15–49.
Rao RD, Michalak JC, Sloan JA, et al.; North Central Cancer Treatment Group. Efficacy of gabapentin in the management of chemotherapy-induced peripheral neuropathy: a phase 3 randomized, double-blind, placebo-controlled, crossover trial (N00C3). Cancer 2007;110: 2110–2118.
McDonald ES, Randon KR, Knight A, Windebank AJ. Cisplatin preferentially binds to DNA in dorsal root ganglion neurons in vitro and in vivo: a potential mechanism for neurotoxicity. Neurobiol Dis 2005;18: 305–313.
Scuteri A, Galimberti A, Maggioni D, et al. Role of MAPKs in platinum-induced neuronal apoptosis. Neurotoxicology 2009;30: 312–319.
James SE, Burden H, Burgess R, et al. Anti-cancer drug induced neurotoxicity and identification of Rho pathway signaling modulators as potential neuroprotectants. Neurotoxicology 2008;29: 605–612.
Graham J, Mushin M, Kirkpatrick P. Oxaliplatin. Nat Rev Drug Discov 2004;3: 11–12.
Grolleau F, Gamelin L, Boisdron-Celle M, Lapied B, Pelhate M, Gamelin E. A possible explanation for a neurotoxic effect of the anticancer agent oxaliplatin on neuronal voltage-gated sodium channels. J Neurophysiol 2001;85: 2293–2297.
Adelsberger H, Quasthoff S, Grosskreutz J, Lepier A, Eckel F, Lersch C. The chemotherapeutic oxaliplatin alters voltage-gated Na+ channel kinetics on rat sensory neurons. Eur J Pharmacol 2000;406: 25–32.
Gamelin L, Capitain O, Morel A, et al. Predictive factors of oxaliplatin neurotoxicity: the involvement of the oxalate outcome pathway. Clin Cancer Res 2007;13: 6359–6368.
Quasthoff S, Hartung HP. Chemotherapy-induced peripheral neuropathy. J Neurol 2002;249: 9–17.
Apfel SC, Lipton RB, Arezzo JC, Kessler JA. Nerve growth factor prevents toxic neuropathy in mice. Ann Neurol 1991;29: 87–90.
Cavaletti G, Cavalletti E, Montaguti P, Oggioni N, De Negri O, Tredici G. Effect on the peripheral nervous system of the short-term intravenous administration of paclitaxel in the rat. Neurotoxicology 1997;18: 137–145.
Cavaletti G, Tredici G, Braga M, Tazzari S. Experimental peripheral neuropathy induced in adult rats by repeated intraperitoneal administration of taxol. Exp Neurol 1995; 133: 64–72.
Authier N, Gillet JP, Fialip J, Eschalier A, Coudore F. Description of a short-term taxol-induced nociceptive neuropathy in rats. Brain Res 2000;887: 239–249.
Polomano RC, Mannes AJ, Clark US, Bennett GJ. A painful peripheral neuropathy in the rat produced by the chemotherapeutic drug, paclitaxel. Pain 2001;94: 293–304.
Flatters SJ, Bennett GJ. Studies of peripheral sensory nerves in paclitaxel-induced painful peripheral neuropathy: evidence for mitochondrial dysfunction. Pain 2006;122: 245–257.
Siau C, Xiao W, Bennett GJ. Paclitaxel- and vincristine-evoked painful peripheral neuropathies: loss of epidermal innervation and activation of Langerhans cells. Exp Neurol 2006;201: 507–514.
Thant M, Hawley RJ, Smith MT, et al. Possible enhancement of vincristine neuropathy by VP-16. Cancer 1982;49: 859–864.
Evtodienko YV, Teplova VV, Sidash SS, Ichas F, Mazat JP. Microtubule-active drugs suppress the closure of the permeability transition pore in tumour mitochondria. FEBS Lett 1996;393: 86–88.
André N, Braguer D, Brasseur G, et al. Paclitaxel induces release of cytochrome c from mitochondria isolated from human neuroblastoma cells. Cancer Res 2000;60: 5349–5353.
Helgason S, Petursson G, Gudmundsson S, Sigurdsson JA. Prevalence of postherpetic neuralgia after a first episode of herpes zoster: prospective study with long term follow up. BMJ 2000; 321: 794–796.
Kost RG, Straus SE. Postherpetic neuralgia: pathogenesis, treatment, and prevention. N Engl J Med 1996;335: 32–42.
Rowbotham MC, Fields HL. Post-herpetic neuralgia: the relation of pain complaint, sensory disturbance, and skin temperature. Pain 1989;39: 129–144.
Fields HL, Rowbotham M, Baron R. Postherpetic neuralgia: irritable nociceptors and deafferentation. Neurobiol Dis 1998;5: 209–227.
Backonja M, Wallace MS, Blonsky ER, et al.; NGX-4010 C116 Study Group. NGX-4010, a high-concentration capsaicin patch, for the treatment of postherpetic neuralgia: a randomised, double-blind study [Erratum in: Lancet Neurol 2009;8:31]. Lancet Neurol 2008;7: 1106–1112.
Christo PJ, Hobelmann G, Maine DN. Post-herpetic neuralgia in older adults: evidence-based approaches to clinical management. Drugs Aging 2007;24: 1–19.
Sampathkumar P, Drage LA, Martin DP. Herpes zoster (shingles) and postherpetic neuralgia. Mayo Clin Proc 2009;84: 274–280.
Osterberg A, Boivie J, Thuomas KA. Central pain in multiple sclerosis: prevalence and clinical characteristics. Eur J Pain 2005; 9: 531–542.
Boivie J, Leijon G, Johansson I. Central post-stroke pain: a study of the mechanisms through analyses of the sensory abnormalities. Pain 1989;37: 173–185.
Finnerup NB, Jensen TS. Spinal cord injury pain: mechanisms and treatment. Eur J Neurol 2004;11: 73–82.
Bowsher D. Central pain: clinical and physiological characteristics. J Neurol Neurosurg Psychiatry 1996;61: 62–69.
Österberg A, Boivie J. Central pain in multiple sclerosis: sensory abnormalities. Eur J Pain 2009 Apr 8; [Epub ahead of print].
Lubetzki C, Williams A, Stankoff B. Promoting repair in multiple sclerosis: problems and prospects. Curr Opin Neurol 2005;18: 237–244.
Lopez-Diego RS, Weiner HL. Novel therapeutic strategies for multiple sclerosis: a multifaceted adversary. Nat Rev Drug Discov 2008;7: 909–925.
Sah DW, Ossipo MH, Porreca F. Neurotrophic factors as novel therapeutics for neuropathic pain. Nat Rev Drug Discov 2003;2: 460–472.
Wang X, Ratnam J, Zou B, England PM, Basbaum AI. TrkB signaling is required for both the induction and maintenance of tissue and nerve injury-induced persistent pain. J Neurosci 2009;29: 5508–5515.
Hefti FF, Rosenthal A, Walicke PA, et al. Novel class of pain drugs based on antagonism of NGF. Trends Pharmacol Sci 2006; 27: 85–91.
Gardell LR, Wang R, Ehrenfels C, et al. Multiple actions of systemic artemin in experimental neuropathy. Nat Med 2003;9: 1383–1389.
Brenner GJ, Ji RR, Shaffer S, Woolf CJ. Peripheral noxious stimulation induces phosphorylation of the NMDA receptor NR1 subunit at the PKC-dependent site, serine-896, in spinal cord dorsal horn neurons. Eur J Neurosci 2004;20: 375–384.
Ma QP, Woolf CJ. Noxious stimuli induce an N-methyl-d-aspartate receptor-dependent hypersensitivity of the flexion withdrawal reflex to touch: implications for the treatment of mechanical allodynia. Pain 1995;61: 383–390.
Caterina MJ, Schumacher MA, Tominaga M, Rosen TA, Levine JD, Julius D. The capsaicin receptor: a heat-activated ion channel in the pain pathway. Nature 1997;389: 816–824.
Szallasi A, Blumberg PM. Vanilloid (capsaicin) receptors and mechanisms. Pharmacol Rev 1999;51: 159–212.
Gavva NR, Bannon AW, Surapaneni S, et al. The vanilloid receptor TRPV1 is tonically activated in vivo and involved in body temperature regulation. J Neurosci 2007;27: 3366–3374.
Waxman SG, Dib-Hajj S, Cummins TR, Black JA. Sodium channels and pain. Proc Natl Acad Sci U S A 1999;96: 7635–7639.
Gold MS, Weinreich D, Kim CS, et al. Redistribution of Nav1.8 in uninjured axons enables neuropathic pain. J Neurosci 2003;23: 158–166.
Fang X, Djouhri L, McMullan S, et al. trkA is expressed in nociceptive neurons and influences electrophysiological properties via Nav1.8 expression in rapidly conducting nociceptors. J Neurosci 2005;25: 4868–4878.
Cox JJ, Reimann F, Nicholas AK, et al. An SCN9A channelopathy causes congenital inability to experience pain. Nature 2006; 444: 894–898.
Fertleman CR, Baker MD, Parker KA, et al. SCN9A mutations in paroxysmal extreme pain disorder: allelic variants underlie distinct channel defects and phenotypes. Neuron 2006;52: 767–774.
Lai J, Gold MS, Kim CS, et al. Inhibition of neuropathic pain by decreased expression of the tetrodotoxin-resistant sodium channel, Nav1.8. Pain 2002;95: 143–152.
Ekberg J, Jayamanne A, Vaughan CW, et al. μO-conotoxin MrVIB selectively blocks Nav1.8 sensory neuron specific sodium channels and chronic pain behavior without motor deficits. Proc Natl Acad Sci U S A 2006;103: 17030–17035.
Nassar MA, Stirling LC, Forlani G, et al. Nociceptor-specific gene deletion reveals a major role for Nav1.7 (PN1) in acute and inflammatory pain. Proc Natl Acad Sci U S A 2004;101: 12706–12711.
Nassar MA, Levato A, Stirling LC, Wood JN. Neuropathic pain develops normally in mice lacking both Nav1.7 and Nav1.8. Mol Pain 2005;1: 24.
Abrahamsen B, Zhao J, Asante CO, et al. The cell and molecular basis of mechanical, cold, and inflammatory pain. Science 2008; 321: 702–705.
Waxman SG. Axonal conduction and injury in multiple sclerosis: the role of sodium channels. Nat Rev Neurosci 2006;7: 932–941.
Petronilli V, Costantini P, Scorrano L, Colonna R, Passamonti S, Bemardi P. The voltage sensor of the mitochondrial permeability transition pore is tuned by the oxidation-reduction state of vicinal thiols: increase of the gating potential by oxidants and its reversal by reducing agents. J Biol Chem 1994;269: 16638–16642.
McStay GP, Clarke SJ, Halestrap AP. Role of critical thiol groups on the matrix surface of the adenine nucleotide translocase in the mechanism of the mitochondrial permeability transition pore. Biochem J 2002;367: 541–548.
Veenman L, Shandalov Y, Gavish M. VDAC activation by the 18 kDa translocator protein (TSPO), implications for apoptosis. J Bioenerg Biomembr 2008;40: 199–205.
Leung AW, Halestrap AP. Recent progress in elucidating the molecular mechanism of the mitochondrial permeability transition pore. Biochim Biophys Acta 2008;1777: 946–952.
Pastorino JG, Hoek JB. Regulation of hexokinase binding to VDAC. J Bioenerg Biomembr 2008;40: 171–182.
Carré M, André N, Carles G, et al. Tubulin is an inherent component of mitochondrial membranes that interacts with the voltage-dependent anion channel. J Biol Chem 2002;277: 33664–33669.
Lowell BB, Shulman GI. Mitochondrial dysfunction and type 2 diabetes. Science 2005;307: 384–387.
Leinninger GM, Backus C, Sastry AM, Yi YB, Wang CW, Feldman EL. Mitochondria in DRG neurons undergo hyperglycemic mediated injury through Bim, Bax and the fission protein Drpl. Neurobiol Dis 2006;23: 11–22.
Siau C, Bennett GJ. Dysregulation of cellular calcium homeostasis in chemotherapy-evoked painful peripheral neuropathy. Anesth Analg 2006;102: 1485–1490.
Shu XQ, Mendell LM. Neurotrophins and hyperalgesia. Proc Natl Acad Sci U S A 1999;96: 7693–7696.
Ogun-Muyiwa P, Helliwell R, McIntyre P, Winter J. Glial cell line derived neurotrophic factor (GDNF) regulates VR1 and substance P in cultured sensory neurons. Neuroreport 1999;10: 2107–2111.
Hudson LJ, Bevan S, Wotherspoon G, Gentry C, Fox A, Winter J. VR1 protein expression increases in undamaged DRG neurons after partial nerve injury. Eur J Neurosci 2001;13: 2105–2114.
Zhang XF, Zhu CZ, Thimmapaya R, et al. Differential action potentials and firing patterns in injured and uninjured small dorsal root ganglion neurons after nerve injury. Brain Res 2004; 1009: 147–158.
Mansour HH. Protective role of camitine ester against radiation-induced oxidative stress in rats. Pharmacol Res 2006;54: 165–171.
Ferraresi R, Troiano L, Roat E, et al. Protective effect of acetyl-l-carnitine against oxidative stress induced by antiretroviral drugs. FEBS Lett 2006;580: 6612–6616.
Manfridi A, Forloni GL, Arrigoni-Martelli E, Mancia M. Culture of dorsal root ganglion neurons from aged rats: effects of acetyl-lL-carnitine and NGF. Int J Dev Neurosci 1992;10: 321–329.
Liu J, Killilea DW, Ames BN. Age-associated mitochondrial oxidative decay: improvement of carnitine acetyltransferase substrate-binding affinity and activity in brain by feeding old rats acetyl-l-carnitine and/or R-α-lipoic acid [Erratum in: Proc Natl Acad Sci U S A 2002;99:7184]. Proc Natl Acad Sci U S A 2002;99: 1876–1881.
Picconi B, Barone I, Pisani A, et al. Acetyl-l-carnitine protects striatal neurons against in vitro ischemia: the role of endogenous acetylcholine. Neuropharmacology 2006;50: 917–923.
Alves E, Binienda Z, Carvalho F, et al. Acetyl-l-carnitine provides effective in vivo neuroprotection over 3,4-methylenedioximethamphetamine-induced mitochondrial neurotoxicity in the adolescent rat brain. Neuroscience 2009;158: 514–523.
Fernandez E, Pallini R, Gangitano C, et al. Effects of l-carnitine, l-acetylcarnitine and gangliosides on the regeneration of the transected sciatic nerve in rats. Neurol Res 1989;11: 57–62.
Mamoulakis D, Galanakis E, Dionyssopoulou E, Evangeliou A, Sbyrakis S. Camitine deficiency in children and adolescents with type 1 diabetes. J Diabetes Complications 2004;18: 271–274.
Famularo G, Moretti S, Marcellini S, et al. Acetyl-carnitine deficiency in AIDS patients with neurotoxicity on treatment with antiretroviral nucleoside analogues. AIDS 1997;11: 185–190.
Ido Y, McHowat J, Chang KC, et al. Neural dysfunction and metabolic imbalances in diabetic rats: prevention by acetyl-l-carnitine. Diabetes 1994;43: 1469–1477.
Lowitt S, Malone JI, Salem AF, Korthals J, Benford S. Acetyl-l-carnitine corrects the altered peripheral nerve function of experimental diabetes. Metabolism 1995;44: 677–680.
Nakamura J, Koh N, Sakakibara F, et al. Polyol pathway hyperactivity is closely related to carnitine deficiency in the pathogenesis of diabetic neuropathy of streptozotocin-diabetic rats. J Pharmacol Exp Ther 1998;287: 897–902.
Stevens MJ, Lattimer SA, Feldman EL, et al. Acetyl-l-carnitine deficiency as a cause of altered nerve myo-inositol content, Na,K-ATPase activity, and motor conduction velocity in the streptozotocin-diabetic rat. Metabolism 1996;45: 865–872.
Sima AA, Ristic H, Merry A, et al. Primary preventive and secondary interventionary effects of acetyl-l-carnitine on diabetic neuropathy in the bio-breeding Worcester rat. J Clin Invest 1996;97: 1900–1907.
Ohsawa M, Miyata S, Carlsson A, Kamei J. Preventive effect of acetyl-l-carnitine on the thermal hypoalgesia in streptozotocin-induced diabetic mice. Eur J Pharmacol 2008;588: 213–216.
Pisano C, Pratesi G, Laccabue D, et al. Paclitaxel and cisplatin-induced neurotoxicity: a protective role of acetyl-l-carnitine. Clin Cancer Res 2003;9: 5756–5767.
Ghirardi O, Lo Giudice P, Pisano C, et al. Acetyl-l-carnitine prevents and reverts experimental chronic neurotoxicity induced by oxaliplatin, without altering its antitumor properties. Anticancer Res 2005;25: 2681–2687.
Flatters SJ, Xiao WH, Bennett GJ. Acetyl-l-carnitine prevents and reduces paclitaxel-induced painful peripheral neuropathy. Neurosci Lett 2006;397: 219–223.
Xiao W, Bennett GJ. Chemotherapy-evoked neuropathic pain: abnormal spontaneous discharge in A-fiber and C-fiber primary afferent neurons and its suppression by acetyl-l-carnitine. Pain 2008;135: 262–270.
Piovesan P, Pacifici L, Taglialatela G, Ramacci MT, Angelucci L. Acetyl-l-carnitine treatment increases choline acetyltransferase activity and NGF levels in the CNS of adult rats following total fimbria-fornix transection. Brain Res 1994;633: 77–82.
Foreman PJ, Perez-Polo JR, Angelucci L, Ramacci MT, Taglialatela G. Effects of acetyl-l-carnitine treatment and stress exposure on the nerve growth factor receptor (p75NGFR) mRNA level in the central nervous system of aged rats. Prog Neuropsychopharmacol Biol Psychiatry 1995;19: 117–133.
Barhwal K, Hota SK, Prasad D, Singh SB, Ilavazhagan G. Hypoxia-induced deactivation of NGF-mediated ERK1/2 signaling in hippocampal cells: neuroprotection by acetyl-l-carnitine. J Neurosci Res 2008;86: 2705–2721.
Di Cesare Mannelli L, Ghelardini C, Calvani M, et al. Protective effect of acetyl-l-carnitine on the apoptotic pathway of peripheral neuropathy. Eur J Neurosci 2007;26: 820–827.
Pettegrew JW, Levine J, McClure RJ. Acetyl-l-carnitine physical-chemical, metabolic, and therapeutic properties: relevance for its mode of action in Alzheimer’s disease and geriatric depression. Mol Psychiatry 2000;5: 616–632.
Jin HW, Flatters SJ, Xiao WH, Mulhern HL, Bennett GJ. Prevention of paclitaxel-evoked painful peripheral neuropathy by acetyl-l-carnitine: effects on axonal mitochondria, sensory nerve fiber terminal arbors, and cutaneous Langerhans cells. Exp Neurol 2008;210: 229–237.
Chiechio S, Caricasole A, Barletta E, et al. l-Acetylcarnitine induces analgesia by selectively up-regulating mGlu2 metabotropic glutamate receptors. Mol Pharmacol 2002;61: 989–996.
Chiechio S, Copani A, De Petris L, Morales ME, Nicoletti F, Gereau RW 4th. Transcriptional regulation of metabotropic glutamate receptor 2/3 expression by the NF-κB pathway in primary dorsal root ganglia neurons: a possible mechanism for the analgesic effect of l-acetylcarnitine. Mol Pain 2006;2: 20.
Ghelardini C, Galeotti N, Calvani M, Mosconi L, Nicolai R, Bartolini A. Acetyl-l-carnitine induces muscarinic antinociception in mice and rats. Neuropharmacology 2002;43: 1180–1187.
Di Cesare Mannelli L, Ghelardini C, Calvani M, et al. Neuroprotective effects of acetyl-l-carnitine on neuropathic pain and apoptosis: a role for the nicotinic receptor. J Neurosci Res 2009; 87: 200–207.
Grandis DD. Tolerability and efficacy of l-acetylcarnitine in patients with peripheral neuropathies: a short-term, open multicentre study. Clin Drug Investig 1998;15: 73–79.
Evans JD, Jacobs TF, Evans EW. Role of acetyl-l-carnitine in the treatment of diabetic peripheral neuropathy. Ann Pharmacother 2008;42: 1686–1691.
Sima AA, Calvani M, Mehra M, Amato A; Acetyl-l-Camitine Study Group. Acetyl-l-carnitine improves pain, nerve regeneration, and vibratory perception in patients with chronic diabetic neuropathy: an analysis of two randomized placebo-controlled trials. Diabetes Care 2005;28: 89–94.
Bianchi G, Vitali G, Caraceni A, et al. Symptomatic and neurophysiological responses of paclitaxel- or cisplatin-induced neuropathy to oral acetyl-l-carnitine. Eur J Cancer 2005;41: 1746–1750.
Maestri A, De Pasquale Ceratti A, Cundari S, Zanna C, Cortesi E, Crinò L. A pilot study on the effect of acetyl-l-carnitine in paclitaxel- and cisplatin-induced peripheral neuropathy. Tumori 2005;91: 135–138.
Hart AM, Wilson AD, Montovani C, et al. Acetyl-l-carnitine: a pathogenesis based treatment for HIV-associated antiretroviral toxic neuropathy. AIDS 2004;18: 1549–1560.
Herzmann C, Johnson MA, Youle M. Long-term effect of acetyl-l-carnitine for antiretroviral toxic neuropathy. HIV Clin Trials 2005;6: 344–350.
Valcour V, Yeh TM, Bartt R, et al. Acetyl-l-carnitine and nucleoside reverse transcriptase inhibitor-associated neuropathy in HIV infection. HIV Med 2009;10: 103–110.
Bordet T, Buisson B, Michaud M, et al. Identification and characterization of cholest-4-en-3-one, oxime (TRO19622), a novel drug candidate for amyotrophic lateral sclerosis. J Pharmacol Exp Ther 2007;322: 709–720.
Rostovtseva TK, Sheldon KL, Hassanzadeh E, et al. Tubulin binding blocks mitochondrial voltage-dependent anion channel and regulates respiration. Proc Natl Acad Sci U S A 2008;105: 18746–18751.
Bordet T, Buisson B, Michaud M, et al. Specific antinociceptive activity of cholest-4-en-3-one, oxime (TRO19622) in experimental models of painful diabetic and chemotherapy-induced neuropathy. J Pharmacol Exp Ther 2008;326: 623–632.
Pabbidi RM, Cao DS, Parihar A, Pauza ME, Premkumar LS. Direct role of streptozotocin in inducing thermal hyperalgesia by enhanced expression of transient receptor potential vanilloid 1 in sensory neurons. Mol Pharmacol 2008;73: 995–1004.
Simiand J, Keane PE, Barnouin MC, Keane M, Soubrié P, Le Fur G. Neuropsychopharmacological profile in rodents of SR 57746A, a new, potent 5-HT1A receptor agonist. Fundam Clin Pharmacol 1993;7: 413–427.
Labie C, Lafon C, Marmouget C, et al. Effect of the neuroprotective compound SR57746A on nerve growth factor synthesis in cultured astrocytes from neonatal rat cortex. Br J Pharmacol 1999;127: 139–144.
Fournier J, Steinberg R, Gauthier T, et al. Protective effects of SR 57746A in central and peripheral models of neurodegenerative disorders in rodents and primates. Neuroscience 1993;55: 629–641.
Cassidy J, Bjamason GA, Hickish T. Randomized double blind (DB) placebo (Plcb) controlled phase III study assessing the efficacy of xaliproden (X) in reducing the cumulative peripheral sensory neuropathy (PSN) induced by the oxaliplatin (Ox) and 5-FU/LV combination (FOLFOX4) in firstline treatment of patients (pts) with metastatic colorectal cancer (MCRC). J Clin Oncol 2006;24 Suppl 18S: 3507 (abstract).
Susman E. Xaliproden lessens oxaliplatin-mediated neuropathy. Lancet Oncol 2006;7: 288.
Kakinoki B, Sekimoto S, Yuki S, et al. Orally active neurotrophin-enhancing agent protects against dysfunctions of the peripheral nerves in hyperglycemic animals. Diabetes 2006;55: 616–621.
Calcutt NA, Freshwater JD, Hauptmann N, Taylor EM, Mizisin AP. Protection of sensory function in diabetic rats by Neotrofin. Eur J Pharmacol 2006;534: 187–193.
Gavish M, Bachman I, Shoukrun R, et al. Enigma of the peripheral benzodiazepine receptor. Pharmacol Rev 1999;51: 629–650.
Galiegue S, Tinel N, Casellas P. The peripheral benzodiazepine receptor: a promising therapeutic drug target. Curr Med Chem 2003;10: 1563–1572.
Veenman L, Papadopoulos V, Gavish M. Channel-like functions of the 18-kDa translocator protein (TSPO): regulation of apoptosis and steroidogenesis as part of the host-defense response. Curr Pharm Des 2007;13: 2385–2405.
Vin V, Leducq N, Bono F, Herbert JM. Binding characteristics of SSR180575, a potent and selective peripheral benzodiazepine ligand. Biochem Biophys Res Commun 2003;310: 785–790.
Ferzaz B, Brault E, Bourliaud G, et al. SSR180575 (7-chloro-N,N,5-trimethyl-4-oxo-3-phenyl-3,5-dihydro-4H-pyridazino[4,5-b]indole-1-acetamide), a peripheral benzodiazepine receptor ligand, promotes neuronal survival and repair. J Pharmacol Exp Ther 2002;301: 1067–1078.
Gibson GE, Karuppagounder SS, Shi Q. Oxidant-induced changes in mitochondria and calcium dynamics in the pathophysiology of Alzheimer’s disease. Ann N Y Acad Sci 2008;1147: 221–232.
Apfel SC, Schwartz S, Adornato BT, et al.; rhNGF Clinical Investigator Group. Efficacy and safety of recombinant human nerve growth factor in patients with diabetic polyneuropathy: a randomized controlled trial. JAMA 2000;284: 2215–2221.
Schifitto G, Yiannoutsos C, Simpson DM, et al.; AIDS Clinical Trials Group Team 291. Long-term treatment with recombinant nerve growth factor for HIV-associated sensory neuropathy. Neurology 2001;57: 1313–1316.
Wellmer A, Misra VP, Sharief MK, Kopelman PG, Anand P. A double-blind placebo-controlled clinical trial of recombinant human brain-derived neurotrophic factor (rhBDNF) in diabetic polyneuropathy. J Peripher Nerv Syst 2001;6: 204–210.
Evans SR, Simpson DM, Kitch DW, et al. A randomized trial evaluating Prosaptide for HIV-associated sensory neuropathies: use of an electronic diary to record neuropathic pain. PLoS One 2007;2: e551.
Reljanovic M, Reichel G, Rett K, et al. Treatment of diabetic polyneuropathy with the antioxidant thioctic acid (α-lipoic acid): a two year multicenter randomized double-blind placebo-controlled trial (ALADIN II). Alpha Lipoic Acid in Diabetic Neuropathy. Free Radic Res 1999;31: 171–179.
Ziegler D, Ametov A, Barinov A, et al. Oral treatment with α-lipoic acid improves symptomatic diabetic polyneuropathy: the SYDNEY 2 trial. Diabetes Care 2006;29: 2365–2370.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bordet, T., Pruss, R.M. Targeting neuroprotection as an alternative approach to preventing and treating neuropathic pain. Neurotherapeutics 6, 648–662 (2009). https://doi.org/10.1016/j.nurt.2009.07.001
Issue Date:
DOI: https://doi.org/10.1016/j.nurt.2009.07.001