Abstract
Background
The mechanism of dipyridamole-induced abnormal increased T1-201 lung uptake in patients without coronary artery disease is poorly understood. The purpose of this study was to evaluate the relation between dipyridamole-induced abnormal T1-201 lung uptake and left ventricular (LV) diastolic indexes using Doppler, color M-mode and Tissue Doppler modalities at rest, and at dipyridamole stress echocardiograpy (DSE) in patients with normal myocardial perfusion and LV function.
Methods and Results
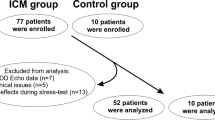
18 consecutive patients (mean age 64 ± 7 years) with normal myocardial perfusion and increased lung T1-201 uptake on dipyridamole stress-redistribution single photon emission computed tomography (SPECT) were included in our study. These patients were compared with 18 age-matched control patients with normal perfusion and normal T1-201 lung uptake. All patients underwent DSE. A good correlation was found between the T-201 lung uptake, the peak early velocity of mitral inflow (E, r _ 0.57) and estimated pulmonary capillary wedge pressure (PCWP _ 1.24[E/Ea] _ 1.9, r _ 0.68). In patients with increased L/H ratio compared to control group, the E and the PCWP were significantly higher at baseline 81 ± 18 vs 68 ± 11 (cm/s) and 13 ± 3 vs 10.2 ± 2 (mmHg). An additional significant increase of E to 91 ± 23 (cm/s (P ± 0.001)) and PCWP to 14.8 ± 3 (P_ 0.005) after dipyridamole administration was seen; in contrast to a nonsignificant change observed in control group. For the detection of a dipyridamole induced PCWP >12 mmHg, a L/H ratio of ≥50% had a sensitivity of 72% and a specificity of 83%, resulting in a positive and a negative predictive value of 81% and 75%, respectively.
Conclusions
A dipyridamole-induced abnormal T1-201 lung uptake in patients with normal myocardial perfusion and systolic function is predictive of elevated filling pressures at rest and in response to dipyridamole administration, probably reflecting an intrinsic resting diastolic dysfunction and a further abnormal response to vasodilatation.
Similar content being viewed by others
References
Boucher CA, Zir LM, Beller GA, et al. Increased lung uptake of thallium-201 during exercise myocardial imaging: clinical, hemodynamic and angiographic implications in patients with coronary artery disease. Am J Cardiol 1980;46:189–96.
Lio P, Kiess M, Okada RD, et al. Increased thallium lung uptake after exercise in isolated left anterior descending coronary artery disease. Am J Cardiol 1985;55:1969–73.
Brown KA, Makay R, Heller GV, et al. Hemodynamic determinants of thallium-201 lung uptake in patients during atrial pacing stress. Am Heart J 1986;111:103–7.
Nishimura S, Mahmarian J, Verani MS. Significance of increased lung thallium uptake during adenosine thallium-201 scintigraphy. J Nucl Med 1992;33:1600–7.
Mahmood S, Buscombc JR, Ell PJ. The use of thallium-201 lung/heart ratio. Eur J Nucl Med 1992;19:807–14.
Ogilby JD, Abdulmassih S, Iskandrian A, et al. Effect of intravenous adenosine infusion on myocardial perfusion and function. Circulation 1992;86:887–95.
NaguehSF, Middleton KJ, Kopelen HA, Zoghbi WA, Quinoones MA. Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol 1997;30:1527–33.
Ommen SR, Nishimura RA, Appleton CP, et al. Clinical utility of Doppler echocardiography and tissue Doppler imaging estimation of left ventricular filling pressure: a comparative simultaneous Doppler-catheterization study. Circulation 2000;102:1788–94.
Kurata C, Tawaraha K, Taguchi T, et al. Lung thallium uptake during exercise emission computed tomography. Nucl Med 1991; 32:417–23.
Aksut SA, Malavarapu C, Russell J, Heo J, Iskandrian AS. Implication of increased thallium lung uptake during exercise single photon emission computed tomography imaging. Am Heart J 1995;130:367–73.
Kaul S, Finkelshtein DM, Homma S, et al. Superiority of quantitative exercise thallium-201 variables in determining long term prognosis in ambulatory patients with chest pain: a comparison with cardiac catheterization. J Am Coll Cardiol 1988;12:25–34.
Gill JB, Ruddy TD, Newell JB, et al. Prognostic importance of thallium uptake by the lungs during exercise in coronary artery disease. N Engl J Med 1987;317:1485–9.
O’Rourke RA. Lung uptake of thallium as a prognostic indicator. N Engl J Med 1987;317:1532–4.
Brown KA. Prognostic value of thallium-201 myocardial perfusion imaging in three primary patient populations. Am J Cardiol 1992;70:23E-9E.
Jain D, Lahiri A, Raftery E. Clinical and prognostic significance of lung thallium uptake on rest imaging in acute myocardial infarction. Am J Cardiol 1990;65:154–9.
Chin BB, Moshin J, Bouchard M, et al. Hemodynamic indices of myocardial dysfunction correlate with dipyridamole thallium-201 SPECT. J Nucl Med 1996;37:723–9.
Verani MS. The adenosine saga: one more piece of the puzzle. But does it cause wall motion abnormalities? Circulation 1992;86:1038–40.
Zafrir N, Dahlberg ST, Villegas BJ, Leppo JA. Prognostic utility of increased pulmonary thallium uptake in patients without ischemia. J Nucl Cardiol 1996;3:301–7.
Beleslin BD, Ostojic M, Djordjevic-Dikic A, et al. Coronary vasodilation without myocardial erection. Eur Heart J 1997;18:1166–74.
Vogel P, Mark W, Apstein CS, et al. Acute alternations in left ventricular diastole chamber stiffness: role of the “erectile” effect of coronary arterial pressure and flow in normal and damaged hearts. Circ Res 1982;51:465–78.
Nussbacher A, Arie S, Kalil R, et al. Mechanism of adenosineinduced elevation of pulmonary capillary wedge pressure in humans. Circulation 1995;92:371–9.
Nagueh SF, Kopelen HA, Zoghbi WA. Effects of adenosine on left ventricular filling dynamics in patients with and without coronary artery disease: a Doppler echocardiographic study. Am Heart J 1998;135:647–54.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Goland, S., Shimoni, S., Livschitz, S. et al. Dipyridamole-induced abnormal Tl-201 lung uptake in patients with normal myocardial perfusion: A marker of increased left ventricular filling pressures. J Nucl Cardiol 11, 305–311 (2004). https://doi.org/10.1016/j.nuclcard.2004.02.006
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1016/j.nuclcard.2004.02.006