Abstract
Background
Implementation of a coordinated multidisciplinary postoperative pathway has been shown to reduce length of stay after posterior spinal fusion (PSF) for adolescent idiopathic scoliosis. This study sought to compare the outcomes of nonambulatory cerebral palsy (CP) patients treated with PSF and cared for using an accelerated discharge (AD) pathway with those using a more traditional discharge (TD) pathway.
Methods
A total of 74 patients with Gross Motor Function Classification System (GMFCS) class 4/5 CP undergoing PSF were reviewed. Thirty consecutive patients were cared for using a TD pathway, and 44 patients were subsequently treated using an AD pathway. The cohorts were then evaluated for postoperative complications and length of stay.
Results
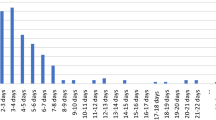
Length of stay (LOS) was 19% shorter in patients managed with the AD pathway (AD 4.0 days [95% CI 2.5-5.5] vs. TD 4.9 days [95% CI 3.5-6.3], p = .01). There was no difference between groups with respect to age at surgery, GMFCS class, preoperative curve magnitude, pelvic obliquity, kyphosis, postoperative curve correction, fusion to the pelvis, or length of fusion between groups. Length of stay remained significantly shorter in the AD group by 0.9 days when controlling for estimated blood loss (EBL) and length of surgery. Complication rates trended lower in the AD group (33% AD vs. 52% TD, p = .12), including pulmonary complications (21% AD vs. 38% TD, p = .13). There was no significant difference in wound complications, return to the operating room, or medical readmissions between groups.
Conclusions
Adoption of a standardized postoperative pathway reduced LOS by 19% in nonambulatory CP patients. Overall, complications, including pulmonary, trended lower in the AD group. Early discharge appears to be possible in this challenging patient population. Although the AD pathway may not be appropriate for all patients, the utility of the AD pathway in optimizing care for more routine PSF for this patient subset appears to be worthwhile.
Level of Evidence
Level III, therapeutic.
Similar content being viewed by others
References
Saito N, Ebara S, Ohotsuka K, et al. Natural history of scoliosis in spastic cerebral palsy. Lancet 1998;351:1687–92.
Hasler C. Operative treatment for spinal deformities in cerebral palsy. J Child Orthop 2013;7:419–23.
Fletcher ND, Andras LM, Lazarus DE, et al. Use of a novel pathway for early discharge was associated with a 48% shorter length of stay after posterior spinal fusion for adolescent idiopathic scoliosis. J Pediatr Orthop 2017;37:92–7.
Jevsevar D, Karlin L. The relationship between preoperative nutritional status and complications after an operation for scoliosis in patients who have cerebral palsy. J Bone Joint Surg Am 1993;75:880–4.
Barsdorf A, Sproule D, Kaufmann P. Scoliosis surgery in children with neuromuscular disease: findings from the US National Inpatient Sample, 1997 to 2003. Arch Neurol 2010;67:231–5.
Benson ER, Thomson JD, Smith BG, Banta JV. Results and morbidity in a consecutive series of patients undergoing spinal fusion for neuromuscular scoliosis. Spine 1998;23:2308–18.
Borgwardt L, Zerahn B, Bliddal H, et al. Similar clinical outcome after unicondylar knee arthroplasty using a conventional or accelerated care program: a randomized, controlled study of 40 patients. Acta Orthop 2009;80:334–7.
Husted H, Hansen H, Holm G, et al. Accelerated versus conventional hospital stay in total hip and knee arthroplasty III: patient satisfaction. Ugeskr Laeger 2006;168:2148–51.
Renkawitz T, Rieder T, Handel M, et al. Comparison of two accelerated clinical pathways—after total knee replacement how fast can we really go? Clin Rehabil 2010;24:230–9.
Fletcher ND, Shourbaji N, Mitchell PM, et al. Clinical and economic implications of early discharge following posterior spinal fusion for adolescent idiopathic scoliosis. J Child Orthop 2014;8:257–63.
Jain A, Sponseller PD, Shah SA, et al. Subclassification of GMFCS level-5 cerebral palsy as a predictor of complications and health-related quality of life after spinal arthrodesis. J Bone Joint Surg Am 2016;98:1821–8.
Jain A, Sponseller PD, Shah SA, et al. Incidence of and risk factors for loss of 1 blood volume during spinal fusion surgery in patients with cerebral palsy. J Pediatr Orthop 2017;37:e484–7.
Borden TC, Bellaire LL, Fletcher ND. Improving perioperative care for adolescent idiopathic scoliosis patients: the impact of a multidis-ciplinary care approach. J Multidiscip Healthc 2016;9:435–45.
Cobb J. Outline for the study of scoliosis. Am Acad Orthop Surg Instr Course Lect 1948;5:261–75.
Watanabe K, Lenke L, Daubs M, et al. Is spine deformity surgery in patients with spastic cerebral palsy truly beneficial? A patient/parent evaluation. Spine 2009;34:2222–32.
Mercado E, Alman B, Wright J. Does spinal fusion influence quality of life in neuromuscular scoliosis? Spine 2007;32:S120–5.
Jones K, Sponseller P, Shindle M, McCarthy M. Longitudinal parental perceptions of spinal fusion for neuromuscular spine deformity in patients with totally involved cerebral palsy. J Pediatr Orthop 2003;23:143–9.
Larsson E, Aaro S, Normelli H, Oberg B. Longterm follow-up of functioning after spinal surgery in patients with neuromuscular scoliosis. Spine 2005;30:2145–52.
Murphy NA, Firth S, Jorgensen T, Young PC. Spinal surgery in children with idiopathic and neuromuscular scoliosis. What’s the difference? J Pediatr Orthop 2006;26:216–20.
Diefenbach C, Ialenti MN, Lonner BS, et al. Hospital cost analysis of neuromuscular scoliosis surgery. Bull Hosp Joint Dis 2013;71: 272–7.
Sarwahi V, Sarwark J, Schafer M. Standards in anterior spine surgery in pediatric patients with neuromuscular scoliosis. J Pediatr Orthop 2001;21:756.
Yuan N, Skaggs D, Dorey F, Keens T. Preoperative predictors of prolonged postoperative mechanical ventilation in children following scoliosis repair. Pediatr Pulmonol 2005;40:414–9.
Perrin C, Unterborn J, Ambrosio C, Hill N. Pulmonary complications of chronic neuromuscular diseases and their management. Muscle Nerve 2004;29:5–27.
Kang G, Suh S, Lee I. Preoperative predictors of postoperative pulmonary complications in neuromuscular scoliosis. J Orthop Sci 2011;16:139–47.
Mohamad F, Parent S, Pawelek J, et al. Perioperative complications after surgical correction in neuromuscular scoliosis. J Pediatr Orthop 2007;27:392–7.
Rumalla K, Yarbrough CK, Pugely AJ, et al. Spinal fusion for pediatric neuromuscular scoliosis: national trends, complications, and in-hospital outcomes. J Neurosurg Spine 2016;25:500–8.
Lonstein JE, Koop SE, Novachek TF, Perra JH. Results and complications after spinal fusion for neuromuscular scoliosis in cerebral palsy and static encephalopathy using Luque Galveston instrumentation: experience in 93 patients. Spine (Phila Pa 1976) 2012;37:583–91.
Ramo BA, Roberts DW, Tuason D, et al. Surgical site infections after posterior spinal fusion for neuromuscular scoliosis: a thirty-year experience at a single institution. J Bone Joint Surg Am 2014;96:2038–48.
McLeod L, Flynn J, Erickson M, et al. Variation in 60-day readmission for surgical-site infections (SSIs) and reoperation following spinal fusion operations for neuromuscular scoliosis. J Pediatr Orthop 2016;36:634–9.
Martin CT, Pugely AJ, Gao Y, Weinstein SL. Causes and risk factors for 30-day unplanned readmissions after pediatric spinal deformity surgery. Spine (Phila Pa 1976) 2015;40:238–46.
Roddy E, Diab M. Rates and risk factors associated with unplanned hospital readmission after fusion for pediatric spinal deformity. Spine J 2017;17:369–79.
Edler A, Murray D, Forbes R. Blood loss during posterior spinal fusion surgery in patients with neuromuscular disease: is there an increased risk? Paediatr Anaesth 2003;13:818–22.
Cahill PJ, Pahys JM, Asghar J, et al. The effect of surgeon experience on outcomes of surgery for adolescent idiopathic scoliosis. J Bone Joint Surg Am 2014;96:1333–9.
Samdani AF, Ranade A, Sciubba DM, et al. Accuracy of free-hand placement of thoracic pedicle screws in adolescent idiopathic scoliosis: how much of a difference does surgeon experience make? Eur Spine J 2010;19:91–5.
Samdani AF, Belin EJ, Bennett JT, et al. Major perioperative complications after spine surgery in patients with cerebral palsy: assessment of risk factors. Eur Spine J 2016;25:795–800.
Dhawale AA, Shah SA, Sponseller PD, et al. Are antifibrinolytics helpful in decreasing blood loss and transfusions during spinal fusion surgery in children with cerebral palsy scoliosis? Spine (Phila Pa 1976) 2012;37:E549–55.
Seehausen DA, Skaggs DL, Andras LM, Javidan Y. Safety and efficacy of power-assisted pedicle tract preparation and screw placement. Spine Deform 2015;3:159–65.
Verma K, Errico T, Diefenbach C, et al. The relative efficacy of antifibrinolytics in adolescent idiopathic scoliosis: a prospective randomized trial. J Bone Joint Surg Am 2014;96:e80.
Verma K, Lonner B, Dean L, et al. Reduction of mean arterial pressure at incision reduces operative blood loss in adolescent idiopathic scoliosis. Spine Deform 2013;1:115–22.
Fuhrhop SK, Keeler KA, Oto M, et al. Surgical treatment of scoliosis in non-ambulatory spastic quadriplegic cerebral palsy patients: a matched cohort comparison of unit rod technique and all-pedicle screw constructs. Spine Deform 2013;1:389–94.
Rappaport DI, Adelizzi-Delany J, Rogers KJ, et al. Outcomes and costs associated with hospitalist comanagement of medically complex children undergoing spinal fusion surgery. Hosp Pediatr 2013;3:233–41.
Hod-Feins R, Anekstein Y, Mirovsky Y, et al. Pediatric scoliosis surgery—the association between preoperative risk factors and postoperative complications with emphasis on cerebral palsy children. Neuropediatrics 2007;38:239–43.
Lipton G, Miller F, Dabney K, et al. Factors predicting postoperative complications following spinal fusions in children with cerebral palsy. J Spinal Disord 1999;12:197–205.
Klein J, Garfin S. Nutritional status in the patient with spinal infection. Orthop Clin North Am 1996;27:33–6.
Carlon S, Shields N, Yong K, et al. A systematic review of the psychometric properties of Quality of Life measures for school aged children with cerebral palsy. BMC Pediatr 2010;10:1–11.
Comstock C, Leach J, Wenger D. Scoliosis in total body-involvement cerebral palsy: analysis of surgical treatment and patient and caregiver satisfaction. Spine 1998;23:1412–25.
Ersberg A, Gerdhem P. Pre- and postoperative quality of life in patients treated for scoliosis. Acta Orthop 2013;84:537–43.
Sarwark J, Sarwahi V. New strategies and decision making in the management of neuromuscular scoliosis. Orthop Clin North Am 2007;38:485–96.
Stanitski C, Micheli L, Hall J, Rosenthal R. Surgical correction of spinal deformity in cerebral palsy. Spine (Phila Pa 1976) 1982;7: 563–9.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures: LLB (none), RWB (grants from Susan and Luther Harrison Foundation, outside the submitted work; consultant for Medtronic; Speaker’s Bureau for Orthopaediatrics and Zimmer Biomet), LAW (none), CAB (none), NDF (personal fees from Orthopaediatrics, personal fees from Medtronic, personal fees from Biomet Spine, outside the submitted work).
IRB approval: IRB approval was received for this study.
Rights and permissions
About this article
Cite this article
Bellaire, L.L., Bruce, R.W., Ward, L.A. et al. Use of an Accelerated Discharge Pathway in Patients With Severe Cerebral Palsy Undergoing Posterior Spinal Fusion for Neuromuscular Scoliosis. Spine Deform 7, 804–811 (2019). https://doi.org/10.1016/j.jspd.2019.02.002
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2019.02.002