Abstract
Study Design
A biomechanical spine model was used to evaluate the impact of screw design on screw-vertebra interface loading during simulated surgical corrections of adult scoliosis.
Objectives
To evaluate differences in screw-vertebra interface forces during adult scoliosis correction between favored angle (FA) screws with extension tabs and standard polyaxial screws while varying deformity severity and curve rigidity.
Summary of Background Data
Pedicle screws enable surgeons to safely and effectively realign spinal deformities. The risk of perioperative screw pullout increases when presented with adult deformities that have less flexible spines and lower bone mineral density. An FA screw with reduction tabs is believed to enable surgical techniques permitting load distribution on multiple screws, thereby reducing screw pullout potential.
Methods
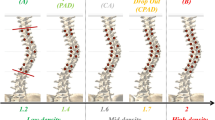
The researchers constructed 3 finite element spine models from adult scoliosis patients. Mechanical properties of intervertebral discs were modeled to reflect less flexible adult spines and their stiffness was varied to evaluate impact on screw-vertebra forces. Models simulated scoliosis surgery according to clinical data using FA or polyaxial screws. Forces measured at the screw-vertebra interface were monitored and compared for each patient with FA and then polyaxial screws.
Results
Simulations using FA screws reduced screw-vertebra interface forces significantly compared with polyaxial screws. Favored angle screws caused 18%, 14%, and 16% reductions in peak forces and 29%, 35%, and 22% reductions in average forces compared with polyaxial screws for patients 1, 2, and 3, respectively. Favored angle screws also provided consistent relative reduction in average forces by 28% when varying properties of intervertebral discs among 8, 10, and 12 MPa.
Conclusions
Using a virtual finite element platform, FA screws reduced screw-vertebra interface forces encountered during simulated correction of less flexible adult scoliosis compared with standard polyaxial screws. These results show a potential benefit of using this modified screw design to reduce screw-vertebra forces and potential intraoperative pullout failures.
Similar content being viewed by others
References
Hsu CC, Cao CK, Wang JL, et al. Increase of pullout strength of spinal pedicle screws with conical core: biomechanical tests and finite element analyses. J Orthop Res 2005;23:788–94.
Jacob A, Ingalhalikar A, Morgan J, et al. Biomechanical comparison of single- and dual-lead pedicle screws in cadaveric spine. J Neurosurg Spine 2008;8:52–7.
Ruland C, McAfee P, Warden K, et al. Triangulation of pedicular instrumentation: a biomechanical analysis. Spine (Phila Pa 1976) 1991;(6 Suppl):S270–6.
Ono A, Brown MD, Latta LL, et al. Triangulated pedicle screw construct technique and pull-out strength of conical and cylindrical screws. J Spinal Disord 2001;14:323–9.
Santoni BG, Hynes RA, McGilvray KC, et al. Cortical bone trajectory for lumbar pedicle screws. Spine J 2009;9:366–73.
Youssef JA, Mckinley TO, Yerby SA, et al. Characteristics of pedicle screw loading: effect of sagittal insertion angle on intrapedicular bending moments. Spine (Phila Pa 1976) 1999;24:1077–81.
McKinley TO, McLain RF, Yerby SA, et al. Characteristics of pedicle screw loading: effect of surgical technique on intravertebral and intrapedicular bending moments. Spine (Phila Pa 1976) 1999;24:18–24; discussion 25.
Paxinos O, Tsitsopoulos P, Zindrick M, et al. Evaluation of pullout strength and failure mechanism of posterior instrumentation in normal and osteopenic thoracic vertebrae. J Neurosurg Spine 2010;13:469–76.
Halvorson TL, Kelley LA, Thomas KA, et al. Effects of bone mineral density on pedicle screw fixation. Spine (Phila Pa 1976) 1994;19:2415–20.
Driscoll M, Mac-Thiong JM, Labelle H, et al. Biomechanical assessment of reduction forces measured during scoliotic instrumentation using two different screw designs. Spine Deformity 2013;1:94–101.
Li S, Patwardhan AG, Amirouche FM, et al. Limitations of the standard linear solid model of intervertebral discs subject to prolonged loading and low-frequency vibration in axial compression. J Biomech 1995;28:779–90.
Yerramalli CS, Chou AI, Miller GJ, et al. The effect of nucleus pulposus crosslinking and glycosaminoglycan degradation on disc mechanical function. Biomech Model Mechanobiol 2007;6:13–20.
Pintar F. Biomechanics of spinal element. Milwaukee, WI: Marquette University; 1986.
Driscoll M, Mac-Thiong JM, Labelle H, et al. Development of a detailed volumetric finite element model of the spine to simulate surgical correction of spinal deformities. Biomed Res Int 2013;2013:931741.
Chen SH, Lin SC, Tsai WC, et al. Biomechanical comparison of unilateral and bilateral pedicle screws fixation for transforaminal lumbar interbody fusion after decompressive surgery-a finite element analysis. BMC Musculoskelet Disord 2012;13:13–72.
Aubin CE, Petit Y, Stokes IA, et al. Biomechanical modeling of posterior instrumentation of the scoliotic spine. Comput Methods Biomech Biomed Eng 2003;6:27–32.
Wang X, Aubin CE, Crandall D, et al. Biomechanical comparison of force levels in spinal instrumentation using monoaxial versus multi degree of freedom postloading pedicle screws. Spine (Phila Pa 1976) 2011;36:E95–104.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures: MD (none); JMT (none); HL (none); SS (none); HS (none); SP (none).
A research grant for this study was provided by DePuy Synthes Spine, Inc. Funding was also provided by an industrial research and development grant from Natural Sciences and Engineering Research Council of Canada.
Rights and permissions
About this article
Cite this article
Driscoll, M., Mac-Thiong, JM., Labelle, H. et al. Biomechanical Comparison of 2 Different Pedicle Screw Systems During the Surgical Correction of Adult Spinal Deformities. Spine Deform 3, 114–121 (2015). https://doi.org/10.1016/j.jspd.2014.07.004
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2014.07.004