Abstract
Objective
We present 2 patients with Stuve-Wiedemann syndrome (SWS) who suffered delayed tetraparesis following posterior spinal surgery for scoliosis.
Background Summary
Delayed tetraparesis after a syndromic thoracic scoliosis correction has never been reported. A cord injury distant from the surgical site is rare, and intraoperative neuromonitoring should be used to detect and prevent neurologic impairment.
Methods
Review of medical charts.
Results
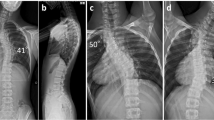
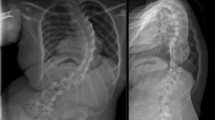
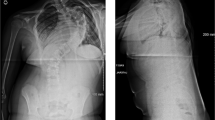
Two patients with SWS suffered delayed tetraparesis 20 and 40 hours respectively after thoracolumbar posterior surgery. In one patient distal motor evoked potentials fell and recovered partially during surgery. In both patients, early postoperative neurologic examination was normal (in one of them except for the extensor hallucis 2/5). CT scan showed correct instrumentation placement and no compressive haematoma. MRI ruled out cord anomalies, but revealed in both patients identical cervical edema that was most likely secondary to ischemia. Angiogram revealed an absence of anterior cord vascular supply.
Conclusions
Correction of severe deformities in syndromic patients may lead to stretch injuries of the spinal cord and its vascular supply. This in turn may lead to a neurological deficit extending beyond the limits of the spinal instrumentation. Abrupt postoperative neck pain may be an alert to this impending development. Close surveillance in the early postoperative period should be maintained in patients with SWS because a delayed neurological deficit can be present even hours afterwards and may be cranial to the surgical level.
Similar content being viewed by others
References
Stuve A, Wiedeman HR. Congenital bowing of the long bones in two sisters. Lancet 1971;2:495.
Akawi NA, Ali BR, Al-Gazali L. Stuve-Wiedemann syndrome and related bent bone dysplasias. Clin Genet 2012;82(1):12–21:Epub ahead of print.
Bonthuis D, Morava E, Booij LHDJ, et al. Stuve Wiedemann syndrome and related syndromes: case report and possible anesthetic complications. Pediatric Anesthesia 2009;19:212–7.
Al-Gazali LI, Ravenscroft A, Feng A, et al. Stuve-Wiedemann syndrome in children surviving infancy: clinical and radiological features. Clin Dysorphol 2003;12:1–8.
Gaspar IM, Saldanha T, Cabral P, et al. Long-term follow-up in Stuve-Wiedemann syndrome: a clinical report. Am J Med Genet 2008;146A:1748–53.
Hassan A, Whately C, Letts M. The orthopaedic manifestations and management of children with Stuve-Wiedemann syndrome. J Bone Joint Surg 2010;92:880–4.
Diab M, Smith A, Kuklo TR, et al. Neural complications in the surgical treatment of adolescent idiopathic scoliosis. Spine 2007;32:2759–63.
Girardi FP, Boachie-Adjei O, Rawlins BA. Safety of sublaminar wires with Isola instrumentation for the treatment of idiopathic scoliosis. Spine 2000;15:691–5.
Kamerlimk JR, Errico T, Xavier S, et al. Major intraoperative neurologic monitoring deficits in consecutive pediatric and adult spinal deformity. Patients at one institution. Spine 2010;35:240–5.
Hicks JM, Singla A, Shen FH, et al. Complications of pedicle screw fixation in scoliosis surgery. Spine 2010;35:E465–70.
Dapunt UA, Mok JM, Sharkey MS, et al. Delayed presentation of tetraparesis following posterior thoracolumbar spinal fusion and instrumentation for adolescent idiopathic scoliosis. Spine 2009;34: E936–41.
Thuet ED, Winscher J, Padberg AM, et al. Validity and reliability of intraoperative monitoring in pediatric spinal deformity surgery: a 23-year experience of 3436 surgical cases. Spine 2010;35:1880–6.
Malhotra NR, Shaffrey C. Intraoperative electrophysiological monitoring in spine surgery. Spine 2010;35:2167–79.
MacEwen GD, Bunnell WP, Siriam K. Acute neurological complications in the treatment of scoliosis. A report of the Scoliosis Research Society. J Bone Joint Surg Am 1975;57:404–8.
Coe JD, Arlet V, Donaldson W, et al. Complications in spinal fusion for adolescent idiopathic scoliosis in the new millennium. A report of the Scoliosis Research Society morbidity and mortality committee. Spine 2006;31:345–9.
Schulte TL, Lerner T, Berendes E, et al. Transient hemiplegia in posterior instrumentation of scoliosis. Spine 2004;29:E394–8.
Wilber RG, Thompson GH, Shaffer JW, et al. Postoperative neurological deficits in segmental spinal instrumentation: A study using spinal cord monitoring. J Bone Joint Surg Am 1984;66:1178–87.
Letts RM, Hollenberg C. Delayed paresis following spinal fusion with Harrington instrumentation. Clin Orthop Relat Res 1977;125:45–8.
Author information
Authors and Affiliations
Corresponding author
Additional information
FDA device/drug status: The devices/drugs are FDA-approved or approved by corresponding national agency for this indication.
Author disclosures: JP (none); PDS (Consulting for DePuy Spine; royalties from DePuy Spine, Globus; conference accommodations from Children’s Specialist Foundation); EI (none); ES (none); FSM (none); PA (none); LZ (none).
No funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
The study has IRB approval.
All authors give permission to reproduce copyrighted material.
Rights and permissions
About this article
Cite this article
Pizones, J., Sponseller, P.D., Izquierdo, E. et al. Delayed Tetraplegia After Thoracolumbar Scoliosis Surgery in Stuve-Wiedemann Syndrome. Spine Deform 1, 72–78 (2013). https://doi.org/10.1016/j.jspd.2012.08.001
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2012.08.001