Abstract
Objective
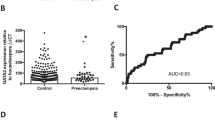
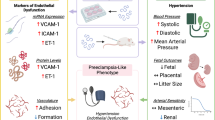
Systemic endothelial dysfunction is a central feature in the pathophysiology of preeclampsia. Its cell biologic and molecular basis is poorly understood. One leading hypothesis argues that endothelial dysfunction is caused by (at present largely unknown) circulating factors released from the ischemic placenta. This study investigated the effects of plasma factors of severe, early-onset preeclamptic women versus healthy pregnant women on endothelial gene expression in vitro.
Methods
Plasma samples were taken from eight severe early-onset preeclamptic women and eight matched pregnant control women. Primary human umbilical vein endothelial cell (HUVEC) and human glomerular microvascular endothelial cell (hGMEC) cultures were incubated with 20% (vol/vol) plasma for 4, 12, and 24 hours. Identical amounts of RNA isolated from HUVEC from three preeclamptic and three control samples were pooled for each time point, and subsequently hybridized on human 60-mer oligonucleotide microarrays containing 17,000 genes. Gene expression levels of vascular cell adhesion molecule-1 (VCAM-1,), intercellular adhesion molecule-1 (ICAM-1,), interleukin-8 (IL-8), and interleukin-6 (IL-6) in HUVEC and hGMEC were quantified using real-time reverse transcription polymerase chain reaction (RT-PCR).
Results
Microarray analyses of individual genes identified no genes that were up- or down-regulated more than 2.7-fold, and analyses of gene ontologies showed no gene ontology significantly up- or down-regulated in HUVEC by preeclamptic plasma. IL-8 gene expression was modestly induced by preeclamptic plasma after 4, 12, and 24 hours of HUVEC and hGMEC incubation, as identified by real-time RT-PCR. The other genes analyzed did not show altered regulation by preeclamptic plasma factors.
Conclusions
In vitro, plasma from preeclamptic patients does not substantially alter endothelial gene expression profile. Only modest induction of IL-8 gene expression was observed. These results indicate that mechanisms other than soluble plasma constituents are likely involved in systemic endothelial cell activation in preeclampsia.
Similar content being viewed by others
References
Roberts JM. Pregnancy related hypertension. In: Creasy RK, Reyes A, eds. Maternal fetal medicine. Philadelphia: Saunders, 1998:835–72.
Roberts JM, Lain KY. Recent insights into the pathogenesis of pre-eclampsia. Placenta 2002;23:359–72.
Aardema MW, Saro MC, Lander M, De Wolf BT, Oosterhof H, Aarnoudse JG. Second trimester Doppler ultrasound screening of the uterine arteries differentiates between subsequent normal and poor outcomes of hypertensive pregnancy; two different pathophysiological entities? Clin Sci (Lond) 2003;106:377–82.
Strevens H, Wide-Swensson D, Hansen A, et al. Glomerular endotheliosis in normal pregnancy and pre-eclampsia. BJOG 2003;110:831–6.
Mastrogiannis DS, O’Brien WF, Krammer J, Benoit R. Potential role of endothelin-1 in normal and hypertensive pregnancies. Am J Obstet Gynecol 1991;165:1711–6.
Chavarria ME, Lara-Gonzalez L, Gonzalez-Gleason A, Garcia-Paleta Y, Vital VS, Reyes A. Prostacyclin/thromboxane early changes in pregnancies that are complicated by preeclampsia. Am J Obstet Gynecol 2003;188:986–92.
Campbell DM, Campbell AJ. Evans Blue disappearance rate in normal and pre-eclamptic pregnancy. Clin Exp Hypertens B 1983;2:163–9.
Kenny L, Baker PN. Maternal pathophysiology in pre-eclampsia. Baillieres Best Pract Res Clin Obstet Gynaecol 1999;13:59–75.
Friedman SA, Schiff E, Emeis JJ, Dekker GA, Sibai BM. Biochemical corroboration of endothelial involvement in severe preeclampsia. Am J Obstet Gynecol 1995;172:202–3.
Deng L, Bremme K, Hansson LO, Blomback M. Plasma levels of von Willebrand factor and fibronectin as markers of persisting endothelial damage in preeclampsia. Obstet Gynecol 1994;84:941–5.
Hsu CD, Copel JA, Hong SF, Chan DW. Thrombomodulin levels in preeclampsia, gestational hypertension, and chronic hypertension. Obstet Gynecol 1995;86:897–9.
Rebelo I, Carvalho-Guerra F, Pereira-Leite L, Quintanilha A. Comparative study of lactoferrin and other blood markers of inflammatory stress between preeclamptic and normal pregnancies. Eur J Obstet Gynecol Reprod Biol 1996;64:167–73.
Madazli R, Aydin S, Uludag S, Vildan O, Tolun N. Maternal plasma levels of cytokines in normal and preeclamptic pregnancies and their relationship with diastolic blood pressure and fibronectin levels. Acta Obstet Gynecol Scand 2003;82:797–802.
Takacs P, Green KL, Nikaeo A, Kauma SW. Increased vascular endothelial cell production of interleukin-6 in severe preeclampsia. Am J Obstet Gynecol 2003;188:740–4.
Velzing-Aarts FV, Muskiet FA, van der Dijs FP, Duits AJ. High serum interleukin-8 levels in Afro-Caribbean women with preeclampsia. Relations with tumor necrosis factor-alpha, duffy negative phenotype and von Willebrand factor. Am J Reprod Immunol 2002;48:319–22.
Kauma S, Takacs P, Scordalakes C, Walsh S, Green K, Peng T. Increased endothelial monocyte chemoattractant protein-1 and interleukin-8 in preeclampsia. Obstet Gyencol 2002;100:706–14.
Redman CW, Sacks GP, Sargent IL. Preeclampsia: An excessive maternal inflammatory response to pregnancy. Am J Obstet Gyencol 1999;180:499–506.
Faas MM, Schuiling GA. Pre-eclampsia and the inflammatory response. Eur J Obstet Gyencol Reprod Biol 2001;95:213–7.
Austgulen R, Lien E, Vince G, Redman CW. Increased maternal plasma levels of soluble adhesion molecules (ICAM-1, VCAM-1, E-selectin) in preeclampsia. Eur J Obstet Gyencol Reprod Biol 1997;71:53–8.
Chaiworapongsa T, Romero R, Yoshimatsu J, et al. Soluble adhesion molecule profile in normal pregnancy and pre-eclampsia. J Matern Fetal Neonatal Med 2002;12:19–27.
Phocas I, Rizos D, Papoulias J, Xyni K, Sarandakou A, Salamalekis E. A comparative study of serum soluble vascular cell adhesion molecule-1 and soluble intercellular adhesion molecule-1 in preeclampsia. J Perinatol 2000;20:114–9.
VanWijk MJ, Kublickiene K, Boer K, Van Bavel E. Vascular function in preeclampsia. Cardiovasc Res 2000;47:38–48.
Baker PN, Davidge ST, Barankiewicz J, Roberts JM. Plasma of preeclamptic women stimulates and then inhibits endothelial prostacyclin. Hypertension 1996;27:56–61.
Taylor RN, Musci TJ, Rodgers GM, Roberts JM. Preeclamptic sera stimulate increased platelet-derived growth factor mRNA and protein expression by cultured human endothelial cells. Am J Reprod Immunol 1991;25:105–8.
Endresen MJ, Morris JM, Nobrega AC, Buckley D, Linton EA, Redman CW. Serum from preeclamptic women induces vascular cell adhesion molecule-1 expression on human endothelial cells in vitro: A possible role of increased circulating levels of free fatty acids. Am J Obstet Gyencol 1998;179:665–70.
Hayman R, Brockelsby J, Kenny L, Baker P. Preeclampsia: The endothelium, circulating factor(s) and vascular endothelial growth factor. J Soc Gynecol Investig 1999;6:3–10.
Takacs P, Kauma SW, Sholley MM, Walsh SW, Dinsmoor MJ, Green K. Increased circulating lipid peroxides in severe preeclampsia activate NF-kappaB and upregulate ICAM-1 in vascular endothelial cells. FASEB J 2001;15:279–81.
Brown MA, Lindheimer MD, de Swiet M, Van Assche A, Moutquin JM. The classification and diagnosis of the hypertensive disorders of pregnancy: Statement from the International Society for the Study of Hypertension in Pregnancy (ISSHP). Hypertens Pregnancy 2001;20:IX–XIV.
von Dadelszen P, Magee LA, Roberts JM. Subclassification of preeclampsia. Hypertens Pregnancy 2003;22:143–8.
Audibert F, Friedman SA, Frangieh AY, Sibai BM. Clinical utility of strict diagnostic criteria for the HELLP (hemolysis, elevated liver enzymes, and low platelets) syndrome. Am J Obstet Gyencol 1996;175:460–4.
Janssen S, Limburg PC, Bijzet J, et al. SAA versus CRP in chronic inflammatory diseases. In: Peeters H, ed. Protides of the biological fluids. Oxford, UK: Pergamon Press, 1986:347–50.
Xiang CC, Kozhich OA, Chen M, et al. Amine-modified random primers to label probes for DNA microarrays. Nat Biotechnol 2002;20:738–42.
Trentani A, Kuipers SD, te Meerman GJ, Beekman J, ter Horst GJ, den Boer JA. Immunohistochemical changes induced by repeated footshock stress: Revelations of gender-based differences. Neurobiol Dis 2003;14:602–18.
Mutin M, Dignat-George F, Sampol J. Immunologic phenotype of cultured endothelial cells: Quantitative analysis of cell surface molecules. Tissue Antigens 1997;50:449–58.
Asgeirsdottir SA, Kok RJ, Everts M, Meijer DK, Molema G. Delivery of pharmacologically active dexamethasone into activated endothelial cells by dexamethasone-anti-E-selectin immunoconjugate. Biochem Pharmacol 2003;65:1729–39.
McCormick SM, Eskin SG, McIntire LV, et al. DNA microarray reveals changes in gene expression of shear stressed human umbilical vein endothelial cells. Proc Natl Acad Sci USA 2001;98:8955–60.
Murakami T, Mataki C, Nagao C, et al. The gene expression profile of human umbilical vein endothelial cells stimulated by tumor necrosis factor alpha using DNA microarray analysis. J Atheroscler Thromb 2000;7:39–44.
Vince GS, Starkey PM, Austgulen R, Kwiatkowski D, Redman CW. Interleukin-6, tumour necrosis factor and soluble tumour necrosis factor receptors in women with pre-eclampsia. Br J Obstet Gynaecol 1995;102:20–5.
Kupferminc MJ, Peaceman AM, Wigton TR, Rehnberg KA, Socol ML. Tumor necrosis factor-alpha is elevated in plasma and amniotic fluid of patients with severe preeclampsia. Am J Obstet Gyencol 1994;170:1752–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was financially supported by the Jan Kornelis de Cock Foundation and the Jan Dekker & Dr. Ludgardine Bouwman Foundation. The authors thank Henk Moorlag and Naomi Werner, Department of Pathology and Laboratory Medicine, for their expert technical assistance, and Robert M. W. Hofstra, PhD, Department of Medical Genetics, Piet C. Limburg, PhD, Department of Clinical Immunology, Anke van den Berg, PhD, and Marijke M. Faas, PhD, Department of Pathology and Laboratory Medicine, for their participation in discussing study design and results.
Rights and permissions
About this article
Cite this article
Donker, R.B., Ásgeirsdóttir, S.A., Gerbens, F. et al. Plasma Factors in Severe Early-Onset Preeclampsia Do Not Substantially Alter Endothelial Gene Expression In Vitro. Reprod. Sci. 12, 98–106 (2005). https://doi.org/10.1016/j.jsgi.2004.10.014
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jsgi.2004.10.014