Abstract
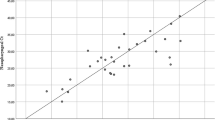
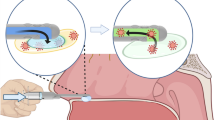
Appropriate collection of respiratory samples is essential for diagnostic testing of respiratory pathogens such as, SARS-CoV-2. During the early pandemic period, there was a shortage of imports such as, nasopharyngeal (NP) swabs in Pakistan, which led to difficulties in sampling for COVID-19 tests. At the Aga Khan University, we developed a 3D-printed anterior nares nasal swab kit paired with in-house viral transport medium (VTM) to address this gap. We conducted a prospective observational study to compare sampling with 3D-printed swab kit and standard NP commercial swab and VTM kits, in 200 individuals presenting for diagnostic testing for SARS-CoV-2 between August and September 2020. The effectiveness of the standard NP and 3D swabs were assessed using RT-PCR results of tested specimens. Results were evaluated based on cut offs of ≤ CT 35 (high to medium viral loads) or, ≤ CT 37 (low viral loads). For the former, 3D swab-based testing had a sensitivity of 93%, specificity of 99%, positive predictive value (PPV) of 98.5%, and negative predictive value (NPV) of 96.2%, respectively. For the latter, sensitivity was 88%, with specificity of 99%, with PPV of 98.5%, and NPV of 93.2%.%. In conclusion, 3D swab-based sampling of anterior nares was comparable with NP sampling using standard swabs, providing a reliable and convenient local solution for respiratory sample collection. Our work highlights the value of using 3D printing for diagnostic tools for convenient and effective sampling when items are scarce. 3D printing also provides new opportunities for rapid assay development as prototypes prior to scale up.





Similar content being viewed by others
Data availability
All data associated with work is provided with the manuscript.
References
World Health Organization, Report of the WHO-China Joint Mission on Coronavirus Disease 2019 (COVID-2019) (2020)
A. Nasir, U.B. Aamir, A. Kanji, A.R. Bukhari, Z. Ansar, N.K. Ghanchi, K.I. Masood, A. Samreen, N. Islam, S. Ghani et al., Tracking SARS-CoV-2 variants through pandemic waves using RT-PCR testing in low-resource settings. PLOS Glob. Public Health 3(6), e0001896 (2023)
S. Tamim, N.S. Trovao, P. Thielen, T. Mehoke, B. Merritt, A. Ikram, M. Salman, M.M. Alam, M. Umair, N. Badar et al., Genetic and evolutionary analysis of SARS-CoV-2 circulating in the region surrounding Islamabad. Pakistan. Infect Genet Evol 94, 105003 (2021)
N.K. Ghanchi, A. Nasir, K.I. Masood, S.H. Abidi, S.F. Mahmood, A. Kanji, S.A. Razzak, W. Khan, S. Shahid, M. Yameen et al., Higher entropy observed in SAR-CoV-2 genomes from the first COVID-19 wave in Pakistan. PLoS ONE 16(8), e0256451 (2021). https://doi.org/10.1371/journal.pone.0256451
N. Tyagi, V. Bhardwaj, D. Sharma, R. Tomar, V. Chaudhary, M. Khanuja, M.K. Singh, G. Sharma, 3D printing technology in the pharmaceutical and biomedical applications: a critical review. Biomed. Mater. Dev. (2023). https://doi.org/10.1007/s44174-023-00105-9
Formlabs: 3D printed COVID-19 test swabs (2020). https://formlabs.com/covid-19-response/covid-test-swabs/
Formlabs: 3D printing materials for healthcare (2020). https://formlabs.com/industries/medical/materials/
Formlabs: Professional 3D printing materials for digital dentistry (2020). https://dental.formlabs.com/materials/
Formlabs: Form 3: Industrial-quality desktop SLA 3D printer (2020). https://formlabs.com/3d-printers/form-3/
Formlabs: Form wash and form cure: Automated post-processing (2020). https://formlabs.com/asia/wash-cure/
FDA US: Establishment registration & device listing (2020). https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfRL/rl.cfm?lid=656158&lpcd=KXF
C.J. Callahan, R. Lee, K.E. Zulauf, L. Tamburello, K.P. Smith, J. Previtera, A. Cheng, A. Green, A. Abdul Azim, A. Yano et al., Open development and clinical validation of multiple 3D-printed nasopharyngeal collection swabs: rapid resolution of a critical COVID-19 testing bottleneck. J. Clin. Microbiol. (2020). https://doi.org/10.1128/JCM.00876-20
S. Grandjean Lapierre, S. Bedwani, F. DeBlois, A. Fortin, N. Zamorano Cuervo, K. Zerouali, E. Caron, P. Morency-Potvin, S. Gagnon, N. Nguissan et al., Clinical evaluation of in-house-produced 3D-printed nasopharyngeal swabs for COVID-19 testing. Viruses 13(9), 1752 (2021)
J.K. Tay, G.B. Cross, S.T. Toh, C.K. Lee, J. Loh, Z.Y. Lim, N. Ngiam, J. Chee, S.W. Gan, A. Saraf et al., Design and multicenter clinical validation of a 3-dimensionally printed nasopharyngeal swab for SARS-CoV-2 testing. JAMA Otolaryngol Head Neck Surg. 147(5), 418–425 (2021)
G. Oland, O. Garner, M.A. de St, Prospective clinical validation of 3D printed nasopharyngeal swabs for diagnosis of COVID-19. Diagn. Microbiol. Infect. Dis. 99(3), 115257 (2021)
S.J. Decker, T.A. Goldstein, J.M. Ford, M.N. Teng, R.S. Pugliese, G.J. Berry, M. Pettengill, S. Silbert, T.R. Hazelton, J.W. Wilson et al., 3-Dimensional printed alternative to the standard synthetic flocked nasopharyngeal swabs used for coronavirus disease 2019 testing. Clin. Infect. Dis. 73(9), e3027–e3032 (2021)
A.S. Walker, E. Pritchard, T. House, J.V. Robotham, P.J. Birrell, I. Bell, J.I. Bell, J.N. Newton, J. Farrar, I. Diamond et al., Ct threshold values, a proxy for viral load in community SARS-CoV-2 cases, demonstrate wide variation across populations and over time. Elife (2021). https://doi.org/10.7554/eLife.64683
C. Callahan, R.A. Lee, G.R. Lee, K. Zulauf, J.E. Kirby, R. Arnaout, Nasal swab performance by collection timing, procedure, and method of transport for patients with SARS-CoV-2. J. Clin. Microbiol. 59(9), e0056921 (2021)
A. Manoj, M. Bhuyan, S. Raj Banik, M. Ravi Sankar, 3D printing of nasopharyngeal swabs for COVID-19 diagnose: past and current trends. Mater. Today Proc. 44, 1361–1368 (2021)
J. Song, J. Korunes-Miller, R. Banerji, Y. Wu, S. Fazeli, H. Zheng, B. Orr, E. Morgan, C. Andry, J. Henderson et al., On-site, on-demand 3D-printed nasopharyngeal swabs to improve the access of coronavirus disease-19 testing. Glob. Chall. 5(11), 2100039 (2021)
D.J. McCulloch, A.E. Kim, N.C. Wilcox, J.K. Logue, A.L. Greninger, J.A. Englund, H.Y. Chu, Comparison of unsupervised home self-collected midnasal swabs with clinician-collected nasopharyngeal swabs for detection of SARS-CoV-2 infection. JAMA Netw. Open 3(7), e2016382 (2020)
R.M. Kagan, A.A. Rogers, G.A. Borillo, N.J. Clarke, E.M. Marlowe, Performance of unobserved self-collected nasal swabs for detection of SARS-CoV-2 by RT-PCR utilizing a remote specimen collection strategy. Open Forum. Infect. Dis. 8(4), ofab039 (2021)
M. Zeraati, R. Pourmohamad, B. Baghchi, N.P. Singh Chauhan, G. Sargazi, Optimization and predictive modelling for the diameter of nylon-6,6 nanofibers via electrospinning for coronavirus face masks. J. Saudi Chem. Soc. 25(11), 101348 (2021)
W.W. Leung, Q. Sun, Charged PVDF multilayer nanofiber filter in filtering simulated airborne novel coronavirus (COVID-19) using ambient nano-aerosols. Sep Purif Technol 245, 116887 (2020)
M. Zeraati, R. Arshadizadeh, N.P.S. Chauhan, G. Sargazi, Genetic algorithm optimization of magnetic properties of Fe-Co-Ni nanostructure alloys prepared by the mechanical alloying by using multi-objective artificial neural networks for the core of transformer. Mater. Today Commun. 28, 102653 (2021)
Acknowledgements
We thank the Aga Khan University Hospital Clinical Laboratories and Department of Pathology and Laboratory Medicine, teams of phlebotomists and Technologists for their contributions.
Funding
This work was supported by Aga Khan Development Network through the Technology Innovation Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest with regard to this study.
Ethical approval
This work received approval from the Ethical Review Committee, Aga Khan University, Pakistan.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hasan, Z., Iqbal, A., Ahmed, I. et al. Value of 3-D-Printed Swabs for Respiratory Sampling and Testing. Biomedical Materials & Devices 2, 521–528 (2024). https://doi.org/10.1007/s44174-023-00120-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44174-023-00120-w