Abstract
Background
Little evidence exists studying the benefits of pre-hospital trauma team activation. Our study measured the impact of pre-hospital trauma team activation on 24-h survival. Our secondary objectives assessed the effects of pre-hospital trauma team activation on time to emergency procedure, computed tomography, blood transfusion, and critical administration threshold, as well as emergency department length of stay.
Methods
We conducted a 40-month health records review on all trauma team activations at The Ottawa Hospital, a Level 1 Trauma Center. Outcomes were compared between pre-hospital and in-hospital trauma team activations. We used logistic and linear regression models to assess outcomes, while controlling for injury severity score, age, systolic blood pressure, and anti-coagulation use. A P value < 0.05 was considered statistically significant. A sensitivity analysis was also used to validate the primary outcome results.
Results
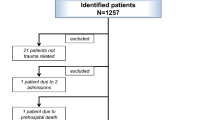
Of the 1013 trauma team activations occurring during the study period, 762 patients were included. The mean age (41.3 vs. 43.8) and percentage of males (79.4% vs. 77.5%) for pre-hospital activations were similar to their counterparts. Pre-hospital activations did not have a statistically significant effect on 24-h mortality (14.4% vs. 4.5%; P = 0.30). However, pre-hospital activations did demonstrate a statistically significant reduction in time (minutes) to emergency procedure (18.0 vs. 27.0; P < 0.001), computed tomography (37.0 vs 42.0; P = 0.009), and blood transfusion (14.0 vs. 28.0; P < 0.001), as well as emergency department length of stay (101.0 vs. 171.0; P < 0.001).
Conclusion
When controlling for key covariates, pre-hospital trauma team activation did not have a significant effect on 24-h mortality, but did result in a significant reduction in time to emergency procedure, computed tomography, and blood transfusion, as well as emergency department length of stay. Our study demonstrates that pre-hospital trauma team activation can expedite patient intervention and disposition.
Résumé
Contexte
Il existe peu de données sur les avantages de l’activation de l’équipe de traumatologie préhospitalière. Notre étude a mesuré l’impact de l’activation de l’équipe de traumatologie pré-hospitalière sur la survie à 24 heures. Nos objectifs secondaires ont évalué les effets de l’activation de l’équipe de traumatologie préhospitalière sur le délai de la procédure d’urgence, de la tomodensitométrie, de la transfusion sanguine et du seuil d’administration critique, ainsi que sur la durée du séjour dans les services d’urgence.
Méthodes
Nous avons procédé à un examen des dossiers médicaux sur 40 mois pour toutes les activations de l’équipe de traumatologie à l’Hôpital d’Ottawa, un centre de traumatologie de niveau 1. Les résultats ont été comparés entre les activations des équipes de traumatologie pré-hospitalières et intra-hospitalières. Nous avons utilisé des modèles de régression logistique et linéaire pour évaluer les résultats, tout en contrôlant le score de gravité des blessures, l’âge, la pression artérielle systolique et l’utilisation d’anticoagulants. Une valeur P < 0.05 a été considérée comme statistiquement significative. Une analyse de sensibilité a également été utilisée pour valider les résultats primaires.
Résultats
Sur les 1013 activations d’équipes de traumatologie survenues pendant la période de l’étude, 762 patients ont été inclus. L’âge moyen (41.3 contre 43.8) et le pourcentage d’hommes (79.4% contre 77.5%) pour les activations préhospitalières étaient similaires à ceux de leurs homologues. Les activations préhospitalières n’ont pas eu d’effet statistiquement significatif sur la mortalité à 24 heures (14.4% contre 4.5%; P = 0.30). Cependant, les activations préhospitalières ont démontré une réduction statistiquement significative du temps (minutes) nécessaire à la procédure d’urgence (18.0 contre 27.0; P < 0.001), à la tomodensitométrie (37.0 contre 42.0; P = 0.009) et à la transfusion sanguine (14.0 contre 0.009). 28.0; P < 0.001), ainsi que la durée du séjour aux urgences (101.0 contre 171.0; P < 0.001).
Conclusion
En tenant compte des principales covariables, l’activation de l’équipe de traumatologie préhospitalière n’a pas eu d’effet significatif sur la mortalité à 24 heures, mais a entraîné une réduction significative du temps nécessaire à l’intervention d’urgence, à la tomodensitométrie et à la transfusion sanguine, ainsi que de la durée de séjour dans les services d’urgence.

Similar content being viewed by others
References
Statistics Canada. (March 5th, 2020). Retrieved from https://www150.statcan.gc.ca/t1/tbl1/en/tv.action?pid=1310039401&pickMembers%5B0%5D=2.23&pickMembers%5B1%5D=3.1. Accessed 5 Mar 2020.
Heron M, Hoyert DL, Murphy SL. National vital statistics reports. National vital statistics reports. 2021;70(4):9.
American College of Surgeons. Resources for the optimal care of the injured patient: 2006. Chicago, IL: American College of Surgeons; 2006.
Emergency Health Regulatory and Accountability Branch. Basic Life Support Patient Care Standards: 2018. Toronto, ON: Ministry of Health and Long-Term Care, 2018
Larsen KT, Uleberg O, Skogvoll E. Differences in trauma team activation criteria among Norwegian hospitals. Scand J Trauma Resusc Emerg Med. 2010;18(1):1.
Kann SH, Hougaard K, Christensen EF. Evaluation of pre-hospital trauma triage criteria: a prospective study at a Danish level I trauma centre. Acta Anaesthesiol Scand. 2007;51(9):1172–7.
Gerardo CJ, Glickman SW, Vaslef SN, et al. The rapid impact on mortality rates of a dedicated care team including trauma and emergency physicians at an academic medical center. J Emerg Med. 2011;40(5):586–91.
Ryb GE, Cooper C, Waak SM. Delayed trauma team activation: patient characteristics and outcomes. J Trauma Acute Care Surg. 2012;73(3):695–8.
Falcone RA Jr, Haas L, King E, et al. A multicenter prospective analysis of pediatric trauma activation criteria routinely used in addition to the six criteria of the American college of surgeons. J Trauma Acute Care Surg. 2012;73(2):377–84.
Hoyt DB, Hollingsworth-Fridlund P, Winchell RJ, et al. Analysis of recurrent process errors leading to provider-related complications on an organized trauma service: directions for care improvement. J Trauma. 1994;36(3):377–84.
Dehli T, Fredriksen K, Osbakk SA, et al. Evaluation of a university hospital trauma team activation protocol. Scand J Trauma Resusc Emerg Med. 2011;19(1):1–7.
Savage SA, Sumislawski JJ, Zarzaur BL, et al. The new metric to define large-volume hemorrhage: results of a prospective study of the critical administration threshold. J Trauma Acute Care Surg. 2015;78(2):224–30.
Rotondo MF, Cribari C, Smith RS (2014) American College of Surgeons Committee on Trauma. Resources for optimal care of the injured patient, vol 6. Chicago: American College of Surgeons; 2014. p. 16–22.
Huang YT, Huang YH, Hsieh CH, et al. Comparison of injury severity score, glasgow coma scale, and revised trauma score in predicting the mortality and prolonged ICU stay of traumatic young children: a cross-sectional retrospective study. Emerg Med Int. 2019;1:2019.
Wilson MS, Konda SR, Seymour RB, et al. Early predictors of mortality in geriatric patients with trauma. J Orthop Trauma. 2016;30(9):e299-304.
Meshcheryakov SV, Semenova ZB, Lukianov VI, et al. Prognosis of severe traumatic brain injury outcomes in children. In: Intracranial Pressure & Neuromonitoring XVI. Cham: Springer; 2018. p. 11–6.
Franklin GA, Boaz PW, Spain DA, et al. Prehospital hypotension as a valid indicator of trauma team activation. J Trauma Acute Care Surg. 2000;48(6):1034–9.
Pieracci FM, Eachempati SR, Shou J, et al. Degree of anticoagulation, but not warfarin use itself, predicts adverse outcomes after traumatic brain injury in elderly trauma patients. J Trauma Acute Care Surg. 2007;63(3):525–30.
Demetriades D, Karaiskakis M, Velmahos G, et al. Effect on outcome of early intensive management of geriatric trauma patients. Br J Surg. 2002;89(10):1319–22.
Yoo Y, Mun S. The advantages of early trauma team activation in the management of major trauma patients who underwent exploratory laparotomy. Ann Surg Treat Res. 2014;87(6):319–24.
de la Mar AC, Lokerman RD, Waalwijk JF, et al. In-house versus on-call trauma surgeon coverage: a systematic review and meta-analysis. J Trauma Acute Care Surg. 2021;91(2):435–44.
Gianola S, Castellini G, Biffi A, et al. Accuracy of pre-hospital triage tools for major trauma: a systematic review with meta-analysis and net clinical benefit. World J Emerg Surg. 2021;16(1):1–1.
Lillebo B, Seim A, Vinjevoll OP, et al. What is optimal timing for trauma team alerts? A retrospective observational study of alert timing effects on the initial management of trauma patients. J Multidiscip Healthc. 2012;5:207.
Driscoll PA, Vincent CA. Organizing an efficient trauma team. Injury. 1992;23(2):107–10.
Acknowledgements
The authors would like to acknowledge Heather Knight and Angela Marcantonio for their contributions to the project.
Funding
None to declare.
Author information
Authors and Affiliations
Contributions
KD: conceptualization, investigation, writing—original draft; MH: conceptualization, supervision, writing—reviewing and editing; ML: conceptualization, writing—reviewing and editing; DG: conceptualization, writing—reviewing and editing; M-JN: methodology, formal analysis, writing—reviewing and editing; JP: conceptualization, methodology, supervision, writing—reviewing and editing.
Corresponding author
Ethics declarations
Conflicts of interest
None to declare.
Additional information
Communicated by Ian Stiell.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Durr, K., Ho, M., Lebreton, M. et al. Evaluating the impact of pre-hospital trauma team activation criteria. Can J Emerg Med 25, 976–983 (2023). https://doi.org/10.1007/s43678-023-00604-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43678-023-00604-0