Abstract
Background
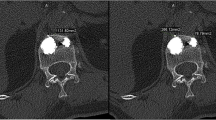
To analyze and evaluate the clinical outcomes of using high-viscosity bone cement compared to low-viscosity bone cement in percutaneous vertebroplasty (PVP) for treatment of Kummell’s disease.
Methods
From July 2017 to July 2019, 68 Kummell’s disease patients who underwent PVP were chosen and separated into 2 groups: H group (n = 34), were treated with high-viscosity bone cement and L group (n = 34), treated with low-viscosity bone cement during treatment. The operation time, number of fluoroscopy tests done, and amount of bone cement perfusion were recorded for both groups. Clinical outcomes were compared, by measuring their Visual Analog Scale (VAS), Oswestry Disability Index (ODI), Kyphosis Cobb’s angle, vertebral height compression rate, and other complications.
Results
High-viscosity group showed less operation time and reduced number of fluoroscopy tests than the low-viscosity group (P < 0.05). When compared to preoperative period, both groups’ VAS and ODI scores were significantly reduced at 1 day and 1 year postoperatively (P < 0.05). The vertebral height compression rate and Cobb’s angle were significantly lower (P < 0.05) in both groups after surgery compared with those before surgery (P < 0.05). The cement leakage rate in group H was 26.5%, which was significantly lower than that in group L, which was 61.8% (P < 0.05).
Conclusions
High-viscosity and low-viscosity bone cement in PVP have similar clinical efficacy in reducing pain in patients during the treatment, but in contrast, high-viscosity bone cement shortens the operative time, reduces number of fluoroscopy views and vertebral cement leakage and improves surgical safety.







Similar content being viewed by others
Data Availability
All information included in this review is documented by relevant references.
References
Pappou, I. P., Papadopoulos, E. C., Swanson, A. N., Cammisa, F. P., Jr., & Girardi, F. P. (2008). Osteoporotic vertebral fractures and collapse with intravertebral vacuum sign (Kümmel’s disease). Orthopedics, 31(1), 61–66.
Kümmell, H. (1895). Die rarefizierende ostitis der Wirbelkorper. Deutsche Med, 21(1), 180–181.
Lim, J., Choi, S. W., Youm, J. Y., Kwon, H. J., Kim, S. H., & Koh, H. S. (2018). Posttraumatic delayed vertebral collapse: Kummell’s disease. Journal of Korean Neurosurgical Association, 61(1), 1–9.
Formica, M., Basso, M., Cavagnaro, L., Formica, C., Zanirato, A., & Felli, L. (2016). Kümmell disease: Illustrative case for definition criteria. The Spine Journal, 16(10), e707–e708.
Xia, Y. H., Chen, F., Zhang, L., Li, G., Tang, Z. Y., Feng, B., et al. (2018). Percutaneous kyphoplasty treatment evaluation for patients with Kümmell disease based on a two-year follow-up. Experimental and Therapeutic Medicine, 16(4), 3617–3622.
Wang, W., Liu, Q., Liu, W. J., Li, Q. B., Cai, L., & Wang, Z. K. (2020). Different performance of intravertebral vacuum clefts in Kümmell’s disease and relevant treatment strategies. Orthopaedic Surgery, 12(1), 199–209.
Wu, A. M., Chi, Y. L., & Ni, W. F. (2013). Vertebral compression fracture with intravertebral vacuum cleft sign: Pathogenesis, image, and surgical intervention. Asian Spine Journal, 7(2), 148–155.
Siemionow, K., & Lieberman, I. H. (2007). Vertebral augmentation in osteoporosis and bone metastasis. Current Opinion in Supportive and Palliative Care, 1(4), 323–327.
Park, J. W., Park, J. H., Jeon, H. J., Lee, J. Y., Cho, B. M., & Park, S. H. (2017). Kümmell’s disease treated with percutaneous vertebroplasty: Minimum 1 year follow-up. Korean Journal of Neurotrauma, 13(2), 119–123.
Ha, K. Y., Lee, J. S., Kim, K. W., & Chon, J. S. (2006). Percutaneous vertebroplasty for vertebral compression fractures with and without intravertebral clefts. Journal of Bone and Joint Surgery, British Volume, 88(5), 629–633.
Baroud, G., Crookshank, M., & Bohner, M. (2006). High-viscosity cement significantly enhances uniformity of cement filling in vertebroplasty: An experimental model and study on cement leakage. Spine (Phila Pa 1976), 31(22), 2562–2568.
Luo, A. J., Liao, J. C., Chen, L. H., & Lai, P. L. (2022). High viscosity bone cement vertebroplasty versus low viscosity bone cement vertebroplasty in the treatment of mid-high thoracic vertebral compression fractures. The Spine Journal, 22(4), 524–534.
Wang, Q., Sun, C., Zhang, L., Wang, L., Ji, Q., Min, N., & Yin, Z. (2022). High- versus low-viscosity cement vertebroplasty and kyphoplasty for osteoporotic vertebral compression fracture: A meta-analysis. European Spine Journal, 31(5), 1122–1130.
Wang, W., Liu, H., Wu, Z., Teng, Y., Huang, Y., Liu, T., & Yang, H. (2022). A comparison of percutaneous kyphoplasty with high-viscosity and low-viscosity bone cement for treatment of osteoporotic vertebral compression fractures: A retrospective study. Geriatr Orthop Surg Rehabil, 13, 21514593221119624.
Georgy, B. A. (2013). Comparison between radiofrequency targeted vertebral augmentation and balloon kyphoplasty in the treatment of vertebral compression fractures: Addressing factors that affect cement extravasation and distribution. Pain Physician, 16(5), E513–E518.
Swartz, K., & Fee, D. (2008). Kümmell’s disease: A case report and literature review. Spine (Phila Pa 1976), 33(5), E152–E155.
Li, K. C., Li, A. F., Hsieh, C. H., Liao, T. H., & Chen, C. H. (2007). Another option to treat Kümmell’s disease with cord compression. European Spine Journal, 16(9), 1479–1487.
Liu, F., Chen, Z., Lou, C., Yu, W., Zheng, L., He, D., et al. (2018). Anterior reconstruction versus posterior osteotomy in treating Kümmell’s disease with neurological deficits: A systematic review. Acta Orthopaedica et Traumatologica Turcica, 52(4), 283–288.
Huang, Y., Peng, M., He, S., Tang, X., Dai, M., & Tang, C. (2016). Clinical efficacy of percutaneous kyphoplasty at the hyperextension position for the treatment of osteoporotic Kümmell disease. Clinical Spine Surgery, 29(4), 161–166.
Zhang, G. Q., Gao, Y. Z., Chen, S. L., Ding, S., Gao, K., & Wang, H. Q. (2015). Comparison of percutaneous vertebroplasty and percutaneous kyphoplasty for the management of Kümmell’s disease: A retrospective study. Indian Journal of Orthopaedics, 49(6), 577–582.
Elnoamany, H. (2015). Percutaneous vertebroplasty: A first line treatment in traumatic non-osteoporotic vertebral compression fractures. Asian Spine Journal, 9(2), 178–184.
Ploeg, W. T., Veldhuizen, A. G., The, B., & Sietsma, M. S. (2006). Percutaneous vertebroplasty as a treatment for osteoporotic vertebral compression fractures: A systematic review. European Spine Journal, 15(12), 1749–1758.
Nieuwenhuijse, M. J., Van Erkel, A. R., & Dijkstra, P. D. (2011). Cement leakage in percutaneous vertebroplasty for osteoporotic vertebral compression fractures: Identification of risk factors. The Spine Journal, 11(9), 839–848.
Peh, W. C., Gelbart, M. S., Gilula, L. A., & Peck, D. D. (2003). Percutaneous vertebroplasty: Treatment of painful vertebral compression fractures with intraosseous vacuum phenomena. AJR, American Journal of Roentgenology, 180(5), 1411–1417.
Ding, J., Zhang, Q., Zhu, J., Tao, W., Wu, Q., Chen, L., et al. (2016). Risk factors for predicting cement leakage following percutaneous vertebroplasty for osteoporotic vertebral compression fractures. European Spine Journal, 25(11), 3411–3417.
Chen, B., Li, Y., Xie, D., Yang, X., & Zheng, Z. (2011). Comparison of unipedicular and bipedicular kyphoplasty on the stiffness and biomechanical balance of compression fractured vertebrae. European Spine Journal, 20(8), 1272–1280.
Tang, S., Fu, W., Zhang, H., Zhang, H., & Liang, B. (2019). efficacy and safety of high-viscosity bone cement vertebroplasty in treatment of osteoporotic vertebral compression fractures with intravertebral cleft. World Neurosurg, 132, e739–e745.
Zhang, Z. F., Huang, H., Chen, S., Liu, D. H., Feng, Y. H., Xie, C. L., et al. (2018). Comparison of high- and low-viscosity cement in the treatment of vertebral compression fractures: A systematic review and meta-analysis. Medicine (Baltimore), 97(12), e0184.
Tanigawa, N., Kariya, S., Komemushi, A., Tokuda, T., Nakatani, M., Yagi, R., et al. (2009). Cement leakage in percutaneous vertebroplasty for osteoporotic compression fractures with or without intravertebral clefts. AJR, American Journal of Roentgenology, 193(5), W442–W445.
Lee, H. J., Park, J., Lee, I. W., Yi, J. S., & Kim, T. (2019). Clinical, radiographic, and morphometric risk factors for adjacent and remote vertebral compression fractures over a minimum follow-up of 4 years after percutaneous vertebroplasty for osteoporotic vertebral compression fractures: Novel three-dimensional voxel-based morphometric analysis. World Neurosurgery, 125, e146–e157.
Funding
This research received no external funding.
Author information
Authors and Affiliations
Contributions
Conceptualization, D-JK; Methodology, D-PH; Software, D-PH; Formal analysis, J-HW and L-FW; Investigation, J-HW; Resources, L-FW; Writing—original draft, D-JK; Writing—review and editing, YS; Supervision, YS.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical Standard Statement
This article does not contain any studies with human or animal subjects performed by the any of the authors.
Informed Consent Statement
Written informed consent has been obtained from the patient(s) to publish this paper.
Institutional Review Board Statement
The study was conducted according to the guidelines of the Declaration of Helsinki and approved by the Institutional Review Board (or Ethics Committee) of Affiliated Hospital of Hebei University of Engineering (2022[K]038 and 2022-6-16).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kan, DJ., Han, DP., Wang, JH. et al. Efficacy and Safety of High-Viscosity Bone Cement in Percutaneous Vertebroplasty for Kummell’s Disease. JOIO 58, 575–586 (2024). https://doi.org/10.1007/s43465-024-01133-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-024-01133-3