Abstract
Background
Femoral shaft fracture in patients of post-polio syndrome (PPS) represents an uncommon yet complex injury pattern. Poorly developed soft-tissue envelope, decreased muscle bulk, reduced vascularity, regional osteopenia, joint contractures, and altered bony anatomy impose significant surgical challenges. Thorough pre-operative planning is imperative as each case requires individualized approach and method of fixation. The aim of the study was to analyze the clinical outcomes in such patients following fracture fixation and to assess the surgical challenges encountered and provide solutions.
Materials and Methods
A retrospective case series of 33 patients with femoral shaft fracture in PPS limbs was undertaken. Mode of injury, method of fixation, surgical time, intra-operative blood loss, union time, and complications were recorded.
Results
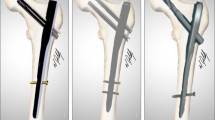
Low-energy fall was the most common mechanism of injury (73%). Thirty-three patients underwent fixation with intramedullary nailing being the most common mode (79%). Femoral canal diameter, femoral bow, fracture location and morphology and clinical deformities of the patients are key governing factors that determine the choice of implant. Locking plates, pre-contoured anatomical plates, and titanium elastic nailing system offer an alternative in patients unsuitable for nailing. With no difference between various implants, average time for bone healing was 13.8 ± 4.4 weeks. All patients resumed full weight-bearing mobilization and returned to pre-injury activity status at the end of 6 months post-surgery.
Conclusion
With detailed pre-operative work-up, contemplating intra-operative difficulties, individualized surgical plan, careful handling of soft tissues, and availability of back-up implants, good clinical outcomes can be achieved in femur fractures in PPS patients.





Similar content being viewed by others
Change history
29 November 2022
A Correction to this paper has been published: https://doi.org/10.1007/s43465-022-00764-8
References
Trojan, D. A., & Cashman, N. R. (2005). Post-poliomyelitis syndrome. Muscle and Nerve, 31(1), 6–19.
Poliomyelitis (polio) [Internet]. [cited 2021 Jun 26]. https://www.who.int/westernpacific/health-topics/poliomyelitis. Accessed 26 June 2021
Tiffreau, V., Rapin, A., Serafi, R., Percebois-Macadré, L., Supper, C., Jolly, D., & Boyer, F. C. (2010). Post-polio syndrome and rehabilitation. Annals of Physical and Rehabilitation Medicine, 53(1), 42–50. https://doi.org/10.1016/j.rehab.2009.11.007.
Haziza, M., Kremer, R., Benedetti, A., & Trojan, D. A. (2007). Osteoporosis in a postpolio clinic population. Archives of Physical Medicine and Rehabilitation, 88(8), 1030–1035.
Silver, J. K., & Aiello, D. D. (2002). Polio survivors: Falls and subsequent injuries. American Journal of Physical Medicine and Rehabilitation, 81(8), 567–570.
Mohammad, A. F., Khan, K. A., Galvin, L., Hardiman, O., & O’Connell, P. G. (2009). High incidence of osteoporosis and fractures in an aging post-polio population. European Neurology, 62(6), 369–374.
Goerss, J. B., Atkinson, E. J., Windebank, A. J., O’Fallon, W. M., & Melton, L. J. (1994). Fractures in an aging population of poliomyelitis survivors: A community-based study in Olmsted County. Minnesota. Mayo Clin Proc., 69(4), 333–339.
Mingo-Robinet, J., Alonso, J. A., Moreno-Barrero, M., González-García, L., Garcia-Virto, V., & Aguado, H. J. (2018). Aspectos técnicos y complicaciones en el tratamiento de las fracturas de los miembros inferiores con secuelas de poliomielitis. Rev Esp Cir Ortopédica Traumatol., 62(4), 257–266.
Wang, W., Shi, H., Chen, D., Chen, Y., Wang, J., Wang, S., et al. (2013). Distal femoral fractures in post-poliomyelitis patients treated with locking compression plates. Orthopaedic Surgery, 5(2), 118–123.
Mehndiratta, M. M., Mehndiratta, P., & Pande, R. (2014). Poliomyelitis. The Neurohospitalist., 4(4), 223–229.
Gonzalez, H., Khademi, M., Borg, K., & Olsson, T. (2012). Intravenous immunoglobulin treatment of the post-polio syndrome: Sustained effects on quality of life variables and cytokine expression after one year follow up. Journal of Neuroinflammation, 9(9), 167.
Gellman, Y. N., Khoury, A., Liebergall, M., Mosheiff, R., & Weil, Y. A. (2019). Outcome of femoral fractures in poliomyelitis patients. International Orthopaedics, 43(11), 2607–2612.
Hill, K. D., & Stinson, A. T. (2004). A pilot study of falls, fear of falling, activity levels and fall prevention actions in older people with polio. Aging Clinical and Experimental Research, 16(2), 126–131.
Bickerstaffe, A., Beelen, A., & Nollet, F. (2010). Circumstances and consequences of falls in polio survivors. Journal of Rehabilitation Medicine, 42(10), 908–915.
Brogårdh, C., & Lexell, J. (2014). Falls, fear of falling, self-reported impairments, and walking limitations in persons with late effects of polio. PM & R: The Journal of Injury, Function, and Rehabilitation, 6(10), 900–907.
Khallaf, F. G. M., Al-Rowaih, A., & Abdul-Hamid, H. F. (1998). Results of subtrochanteric fractures treated with dynamic hip screw and dynamic condylar screw. Medical Principles and Practice, 7(4), 283–291.
Çevik HB. Management of femoral fractures in aging adult polio population: A retrospective review of 13 cases. South Clin Istanb Eurasia [Internet]. 2020 [cited 2021 Jul 6]. http://www.scie.online/jvi.aspx?un=SCIE-95967. Accessed 21 Aug 2019
Park, H., & Kim, H. W. (2012). Treatment of femoral shaft fracture with an interlocking humeral nail in older children and adolescents. Yonsei Medical Journal, 53(2), 408–415.
Lee, K.J., Min, B.W., Jung, J.H., Kang, M.K., Kim, M.J. (2015) Expert tibia nail for subtrochanteric femoral fracture to prevent thermal injury. International Journal of Surgery Case Reports, 10, 158–61.
El-Sayed, K. A. (2010). Locked plating for femoral fractures in polio patients. Archives of Orthopaedic and Trauma Surgery, 130(10), 1299–1304.
Gupta, M., Jain, V. K., Upadhyaya, G. K., & Arya, R. K. (2016). Comprehensive review of challenges associated with management of lower limb fractures in poliomyelitis patients. Journal of Clinical Orthopaedics and Trauma, 7(4), 276–281.
Krupp, R. J., Malkani, A. L., Goodin, R. A., & Voor, M. J. (2003). Optimal entry point for retrograde femoral nailing. Journal of Orthopaedic Trauma, 17(2), 100–105.
Pettett, B. J., Avery, M. C., & Ostrum, R. F. (2017). Retrograde femoral nailing using percutaneous reduction techniques. Journal of Orthopaedic Trauma, 31, S6.
Assessment of bone geometry and its considerations in implant selection for polio affected femoral fractures: An outcome analysis [Internet]. ResearchGate. [cited 2019 Jan 19]. https://www.researchgate.net/publication/316019975_Assessment_of_bone_geometry_and_its_considerations_in_implant_selection_for_polio_affected_femoral_fractures_An_outcome_analysis. Accessed 6 Dec 2016
Alvarez, A., Kremer, R., Weiss, D. R., Benedetti, A., Haziza, M., & Trojan, D. A. (2010). Response of postpoliomyelitis patients to bisphosphonate treatment. PM&R., 2(12), 1094–1103.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors (Suman Saurabh, Anupam Gupta, Tanya Trikha, Aashraya Karpe, and Samarth Mittal) declare that they have no conflict of interests. Authors also declare that no funding has been received from any source.
Ethical approval
All procedures performed in study were in accordance with the ethical standards of the institutional guidelines and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants involved in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: It was erroneously stated in the Introduction that “Poliovirus predominantly affects the dorsal root ganglion …”.
The correct statement is: “Poliovirus predominantly affects the anterior horn cells …” [3].
References
3. Tiffreau V, Rapin A, Serafi R, Percebois-Macadré L, Supper C, Jolly D, Boyer FC. Post-polio syndrome and rehabilitation. Ann Phys Rehabil Med. 2010 Feb;53(1):42-50. doi: https://doi.org/10.1016/j.rehab.2009.11.007. Epub 2009 Dec 30. PMID: 20044320.
The original article has been corrected.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gupta, A., Saurabh, S., Trikha, T. et al. Femoral Shaft Fracture in Post-polio Syndrome Patients: Case Series from a Level-I Trauma Center and Review of Literature. JOIO 56, 1339–1346 (2022). https://doi.org/10.1007/s43465-022-00683-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-022-00683-8